Key points
- Schistosomiasis incubates for 14 – 84 days for people with acute infection.
- Chronic schistosomiasis results from the hosts' immune response to the schistosome eggs.
- There are multiple ways to test for schistosomiasis.
- Praziquantel can treat infections from all major Schistosoma species.
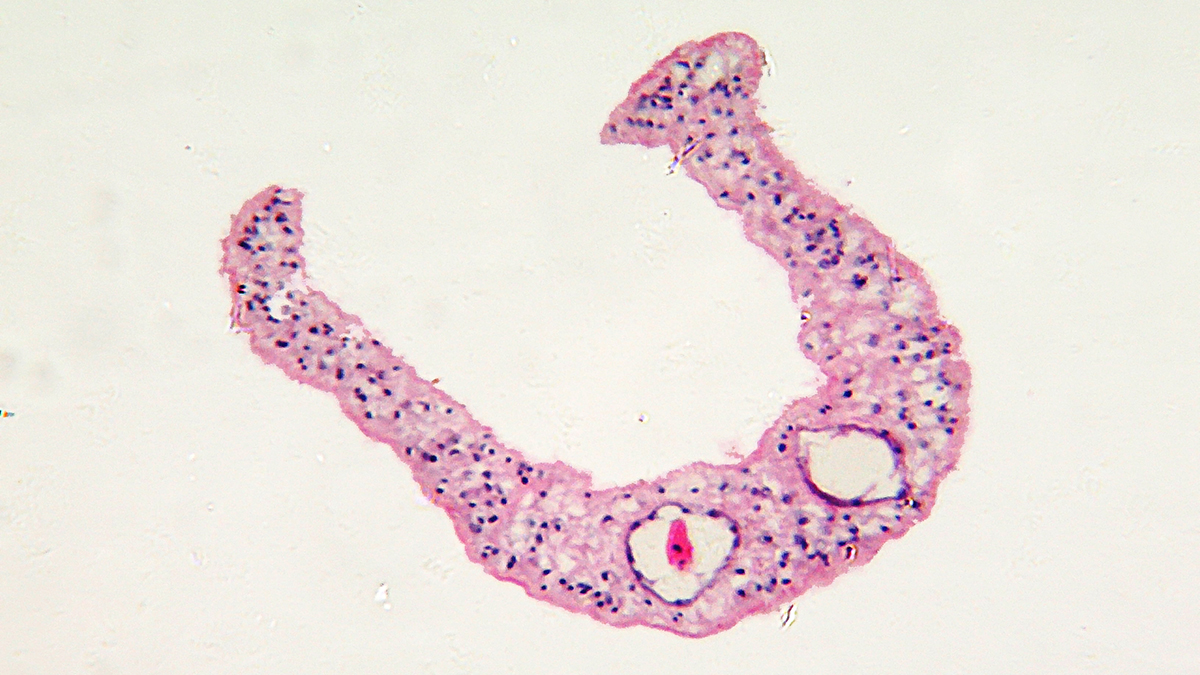
Incubation
The incubation period for patients with acute schistosomiasis is usually 14 – 84 days. However, many people are asymptomatic and have subclinical disease during both acute and chronic stages of infection.
People with acute infection (also known as Katayama syndrome) may present with:
- Rash
- Fever
- Headache
- Myalgia
- Respiratory symptoms
Often eosinophilia is present with hepato- and/or splenomegaly.
Clinical features
Clinical manifestations of chronic disease result from host immune responses to schistosome eggs.
Abdominal symptoms
S. mansoni and S. japonicum eggs most commonly lodge in the blood vessels of the liver or intestine and can cause:
- Diarrhea
- Constipation
- Blood in the stool
Chronic inflammation can lead to:
- Bowel wall ulceration
- Hyperplasia
- Polyposis
Heavy infections can lead to liver fibrosis and portal hypertension.
S. haematobium eggs tend to lodge in the urinary tract causing damage that can lead to dysuria and hematuria. Chronic infections may increase the risk of bladder cancer, bladder fibrosis, and kidney damage. These eggs have also been associated with damage to the female genital tract. This damage can cause female genital schistosomiasis, which can affect the cervix, Fallopian tubes, and vagina. Female genital schistosomiasis can also lead to increased susceptibility to other infections.
Central nervous system symptoms
Central nervous system lesions have been reported but are rare. Disease is the result of ectopic deposition of eggs in the spinal cord (S. mansoni or S. haematobium) or brain (S. japonicum) and inflammatory reactions, typically the formation of granulomas that act as space occupying lesions.
Testing and diagnosis
Examination of stool and/or urine for ova is the primary method of diagnosis for suspected schistosome infections. Because symptom presentation can vary due to species, it is important to gather a full travel or former residence history. Testing recommendations can also vary depending on light versus heavy infections and recent travel status versus former residents of schistosomiasis-endemic country or region.
Treatment and recovery
Praziquantel is effective at treating infections with all major Schistosoma species. The timing of treatment is important since praziquantel is most effective against the adult worm and requires the presence of a mature antibody response to the parasite. The immune response in lightly infected patients may be less robust from the response in heavily infected patients. Lightly infected patients may need repeat treatments. Limited evidence of parasite resistance to praziquantel has been reported based on low cure rates in recently exposed or heavily infected populations. See full treatment guidelines.
