SARS-CoV-2–Associated Deaths Among Persons Aged <21 Years — United States, February 12–July 31, 2020
Weekly / September 18, 2020 / 69(37);1324–1329
On September 15, 2020, this report was posted online as an MMWR Early Release.
Danae Bixler, MD1; Allison D. Miller, MPH1; Claire P. Mattison, MPH1; Burnestine Taylor, MD2; Kenneth Komatsu, MPH3; Xandy Peterson Pompa, MPH3; Steve Moon4; Ellora Karmarkar, MD5; Caterina Y. Liu, MD5; John J. Openshaw, MD5; Rosalyn E. Plotzker, MD5; Hilary E. Rosen, MPH5; Nisha Alden, MPH6; Breanna Kawasaki, MPH6; Alan Siniscalchi, MPH, MS7; Andrea Leapley, MPH8; Cherie Drenzek, DVM9; Melissa Tobin-D’Angelo, MD9; Judy Kauerauf, MPH10; Heather Reid10; Eric Hawkins, MS11; Kelly White, MPH11; Farah Ahmed, PhD12; Julie Hand, MSPH13; Gillian Richardson, MPH13; Theresa Sokol, MPH13; Seth Eckel, MPH14; Jim Collins, MPH14; Stacy Holzbauer, DVM15; Leslie Kollmann15; Linnea Larson, MPH15; Elizabeth Schiffman, MPH15; Theresa S. Kittle, MPH16; Kimberly Hertin, MPH17; Vit Kraushaar, MD17; Devin Raman, MPH17; Victoria LeGarde, MPH18; Lindsey Kinsinger, MPH18; Melissa Peek-Bullock, MPH18; Jenna Lifshitz19; Mojisola Ojo, MPH19; Robert J Arciuolo, MPH20; Alexander Davidson, MPH20; Mary Huynh, PhD20; Maura K. Lash, MPH20; Julia Latash, MPH20; Ellen H. Lee, MD20; Lan Li, MPH20; Emily McGibbon, MPH20; Natasha McIntosh-Beckles20; Renee Pouchet, MHA20; Jyotsna S. Ramachandran, MPH20; Kathleen H. Reilly, PhD20; Elizabeth Dufort, MD21; Wendy Pulver, MS21; Ariela Zamcheck, DO21; Erica Wilson, MD22; Sietske de Fijter, MS23; Ozair Naqvi, MS24; Kumar Nalluswami, MD25; Kirsten Waller, MD25; Linda J. Bell, MD26; Anna-Kathryn Burch, MD26; Rachel Radcliffe, DVM26; Michelle D. Fiscus, MD27; Adele Lewis, MD27; Jonathan Kolsin, MPH28; Stephen Pont, MD28; Andrea Salinas, MPH28; Kelsey Sanders, MPH28; Bree Barbeau, MPH29; Sandy Althomsons, MHS1; Sukhshant Atti, MD30; Jessica S. Brown, PhD1; Arthur Chang, MD1; Kevin R. Clarke, MD1; S. Deblina Datta, MD1; John Iskander, MD1; Brooke Leitgeb, MS1; Talia Pindyck, MD1; Lalita Priyamvada, PhD1; Sarah Reagan-Steiner, MD1; Nigel A. Scott, MS1; Laura J. Viens, MD1; Jonathan Zhong, MPH1; Emilia H. Koumans, MD1; Pediatric Mortality Investigation Team (View author affiliations)
View suggested citationSummary
What is already known about this topic?
Symptoms associated with SARS-CoV-2 infection are milder in children compared with adults.
What is added by this report?
Among 121 SARS-CoV-2–associated deaths among persons aged <21 years reported to CDC by July 31, 2020, 12 (10%) were infants and 85 (70%) were aged 10–20 years. Hispanic, non-Hispanic Black and non-Hispanic American Indian/Alaskan Native persons accounted for 94 (78%) of these deaths; 33% of deaths occurred outside of a hospital.
What are the implications for public health practice?
Persons aged <21 years exposed to SARS-CoV-2 should be monitored for complications. Ongoing surveillance for SARS-CoV-2–associated infection, hospitalization, and death among persons aged <21 years should be continued as schools reopen in the United States.
Since February 12, 2020, approximately 6.5 million cases of SARS-CoV-2 infection, the cause of coronavirus disease 2019 (COVID-19), and 190,000 SARS-CoV-2–associated deaths have been reported in the United States (1,2). Symptoms associated with SARS-CoV-2 infection are milder in children compared with adults (3). Persons aged <21 years constitute 26% of the U.S. population (4), and this report describes characteristics of U.S. persons in that population who died in association with SARS-CoV-2 infection, as reported by public health jurisdictions. Among 121 SARS-CoV-2–associated deaths reported to CDC among persons aged <21 years in the United States during February 12–July 31, 2020, 63% occurred in males, 10% of decedents were aged <1 year, 20% were aged 1–9 years, 70% were aged 10–20 years, 45% were Hispanic persons, 29% were non-Hispanic Black (Black) persons, and 4% were non-Hispanic American Indian or Alaska Native (AI/AN) persons. Among these 121 decedents, 91 (75%) had an underlying medical condition,* 79 (65%) died after admission to a hospital, and 39 (32%) died at home or in the emergency department (ED).† These data show that nearly three quarters of SARS-CoV-2–associated deaths among infants, children, adolescents, and young adults have occurred in persons aged 10–20 years, with a disproportionate percentage among young adults aged 18–20 years and among Hispanics, Blacks, AI/ANs, and persons with underlying medical conditions. Careful monitoring of SARS-CoV-2 infections, deaths, and other severe outcomes among persons aged <21 years remains particularly important as schools reopen in the United States. Ongoing evaluation of effectiveness of prevention and control strategies will also be important to inform public health guidance for schools and parents and other caregivers.
Public health jurisdictions in the United States use standard definitions to identify cases of COVID-19§ and multisystem inflammatory syndrome in children (MIS-C),¶ a severe illness characterized by fever, multiorgan system involvement, laboratory evidence of inflammation, and laboratory or epidemiologic evidence of SARS-CoV-2 infection or exposure. SARS-CoV-2–associated deaths were defined as deaths associated with COVID-19 or MIS-C per the determination of the jurisdiction. Persons aged <21 years who met the definition for a SARS-CoV-2–associated death and died during February 12–July 31, 2020, were included in this study. Fifty states, New York City, the District of Columbia, Puerto Rico, Guam, and the U.S. Virgin Islands were asked to submit information on SARS-CoV-2–associated deaths among persons aged <21 years, including COVID-19 or MIS-C case status (as determined by each jurisdiction), demographics, dates of illness onset and hospitalization, underlying medical conditions, and location of death. Number of days from illness onset to hospitalization, days from hospitalization until date of death, and days from onset to date of death were calculated for decedents with available data.
Cases of SARS-CoV-2 infection among persons aged <21 years in the United States were first reported in March 2020 (Figure 1); the first SARS-CoV-2–associated fatality among persons in that age group also occurred in March. During February 12–July 31, a total of 391,814 cases of confirmed or probable COVID-19 or MIS-C in persons aged <21 years were reported through case-based surveillance in the United States.
Among the 55 health jurisdictions invited to submit information on SARS-CoV-2–associated deaths among persons aged <21 years, 47 responded; 20 reported no deaths,** and 27 identified 121 deaths†† that met inclusion criteria. Overall, 120 (99%) decedents met the confirmed or probable COVID-19 case definition, and 15 (12%) met the MIS-C case definition, including 14 (12%) who met both case definitions. Twelve (10%) deaths were in infants aged <1 year, 24 (20%) in children aged 1–9 years, and 85 (70%) in persons aged 10–20 years; the median age at death was 16 years (interquartile range [IQR] = 7–19 years) (Figure 2) (Table). Among the 121 decedents, 76 (63%) were male, 54 (45%) were Hispanic, 35 (29%) were Black, and five (4%) were AI/AN.
Among the 121 decedents, 30 (25%) were previously healthy (no reported underlying medical condition), 91 (75%) had at least one underlying medical condition, and 54 (45%) had two or more underlying medical conditions. The most frequently reported medical conditions were chronic lung disease, including asthma (34 [28%]), obesity (33 [27%]), neurologic and developmental conditions (26 [22%]), and cardiovascular conditions (22 [18%]).
Overall, 79 (65%) deaths occurred after hospital admission. Among the remaining 42 decedents, 16 (38%) died at home, 23 (55%) were critically ill and died in the ED, one (2%) died in hospice care, and the location of death was unknown for two (5%). Out-of-hospital deaths occurred in all age groups; however, the highest proportions of deaths at home or in the ED occurred in infants (33%) and adolescents and young adults aged 14–20 years (37%)§§ (Supplementary figure, https://stacks.cdc.gov/view/cdc/93381). Among the 79 decedents who died in the hospital, the median interval from onset of symptoms until admission was 3 days (IQR = 1–7 days),¶¶ and the median interval from hospital admission until death was 8 days (IQR = 4–21.5 days).*** Among 94 decedents with known illness onset date, median interval from onset of symptoms until death was 11 days (IQR = 6–24 days).
Discussion
During February 12–July 31, 2020, a total of 391,814 cases of COVID-19 and MIS-C (representing approximately 8% of all reported cases) (1,2) and 121 deaths (approximately 0.08% of all deaths) (1,2) were identified among persons aged <21 years in the United States. Four important findings were identified. First, although Hispanic, Black, and AI/AN persons represent 41% of the U.S. population aged <21 years (4), these groups accounted for approximately 75% of deaths in persons aged <21 years. Second, deaths were more prevalent among males and among persons aged 10–20 years; young adults aged 18–20 years accounted for nearly half of all deaths in this population. Third, 75% of decedents had at least one underlying condition, and 45% had two or more underlying conditions. Fourth, a substantial proportion of out-of-hospital deaths in association with SARS-CoV-2 infection occurred among all age groups in this analysis.
Among infants, children, and adolescents hospitalized with laboratory-confirmed COVID-19 (5) and cases of MIS-C (6), persons from racial and ethnic minority groups are overrepresented. These racial/ethnic groups are also disproportionately represented among essential workers unable to work from their homes (7), resulting in higher risk for exposure to SARS-CoV-2 with potential secondary transmission among household members, including infants, children, adolescents, and young adults. In addition, disparities in social determinants of health, such as crowded living conditions, food and housing insecurity, wealth and educational gaps, and racial discrimination, likely contribute to racial and ethnic disparities in COVID-19 and MIS-C incidence and outcomes (7). Finally, higher rates of adverse outcomes among racial and ethnic minorities are likely related to challenges in seeking care for various reasons, including difficulty and delays in accessing health care services because of lack of insurance, child care, transportation, or paid sick leave, and social determinants of health that contribute to higher prevalence of medical conditions (7).
Thirty-nine out-of-hospital SARS-CoV-2–associated deaths occurred at home or in the ED among persons aged <21 years. In the United States, significant reductions in ED visits (8) and childhood immunizations (9) occurred during March–April 2020, suggesting that necessary care might be delayed or deferred during the pandemic. Although infants, children, and adolescents are more likely to have milder COVID-19 illness than are adults (3), complications, including MIS-C (6) and respiratory failure (5,6), do occur in these populations. Persons infected with or exposed to SARS-CoV-2 should be followed closely so that clinical deterioration can be detected early. In this analysis, the number of deaths was highest in persons aged 14–20 years. Adolescents especially need patient-centered follow-up services that are developmentally appropriate (10).
The findings in this report are subject to at least five limitations. First, case-based surveillance data††† underestimate cases of COVID-19 compared with aggregate case reports§§§ from states, and data for some variables in case-based surveillance (e.g., demographic variables) are missing. Therefore, data on cases and deaths by race/ethnicity are not comparable and case fatality rates by race/ethnicity cannot be calculated. Second, the possibility exists that all deaths were not recognized or reported, in part because of incomplete testing, failure to update vital status after death of a previously reported case of COVID-19 or MIS-C, or delays in reporting SARS-CoV-2–associated deaths because of the lengthy process for cause of death ascertainment. Third, autopsy findings and death certificates were not available to verify cause of death for this report. More detailed review of available medical and death records is currently underway in collaboration with public health jurisdictions. Fourth, although guidance for death certificate coding for COVID-19 is available,¶¶¶ a standard surveillance case definition for SARS-CoV-2–associated death is not in use in the United States; case ascertainment and data collection procedures were nonuniform among jurisdictions. Finally, during most of the time between February 12 and July 31, 2020, the majority of U.S. early child care providers, schools, and other educational institutions were closed, gatherings of children and adolescents were reduced, and testing and treatment protocols changed.**** As early child care providers, schools, and other educational institutions reopen for in-person learning and treatment protocols continue to evolve, the incidence of pediatric SARS-CoV-2–associated deaths might change, and pediatric case and death surveillance should continue.
Adolescents and young adults, Hispanic, Black, and AI/AN persons, and persons with underlying medical conditions are disproportionately represented among deaths associated with SARS-CoV-2 in persons aged <21 years reported to CDC. Infants, children, adolescents, and young adults, particularly those from racial and ethnic minority groups at higher risk, those with underlying medical conditions, and their caregivers, need clear, consistent, and developmentally, linguistically, and culturally appropriate COVID-19 prevention messages (e.g., related to mask wearing, physical distancing, hand hygiene). To ensure accurate surveillance, it is important that health care providers and health departments assure follow-up for infants, children, adolescents, and young adults infected with or exposed to SARS-CoV-2 and document and report underlying medical conditions and cause of death related to COVID-19. Health departments, in collaboration with school districts and the communities they serve, can evaluate and improve health promotion, health access, and health equity for all infants, children, adolescents, and young adults. Ultimately, health departments, health providers, and community partners can mobilize to remove systemic barriers that contribute to health disparities.††††
Acknowledgments
Jasmine Abdelnabi, Judy Chen, Marie S. Dorsinville, Meredith Eddy, Michele English, Kevin Guerra, Fabiana Jeanty, Lucretia Jones, Kenya Murray, Marc Paladini, John Paul Quinn, Gloria E. Rivera, Brian Toro, New York City Department of Health and Mental Hygiene; Kimberly D. Machesky, Ohio Department of Health; Courtney Dewart, Ohio Department of Health and Epidemic Intelligence Service, CDC.
Pediatric Mortality Investigation Team
David Blythe, Maryland Department of Health; Laurel Harduar Morano, Pennsylvania Department of Health; Carla Black, CDC COVID-19 Response Team; Carter McCabe, CDC COVID-19 Response Team; Xia Lin, CDC COVID-19 Response Team.
Corresponding author: Danae Bixler, nqd0@cdc.gov.
1CDC COVID-19 Response Team; 2Alabama Department of Public Health; 3Arizona Department of Health Services; 4Los Angeles County Department of Public Health; 5California Department of Public Health; 6Colorado Department of Public Health and Environment; 7Connecticut Department of Public Health; 8Florida Department of Health; 9Georgia Department of Public Health; 10Illinois Department of Public Health; 11Indiana State Department of Health; 12Kansas Department of Health and Environment; 13Louisiana Department of Health; 14Michigan Department of Health and Human Services; 15Minnesota Department of Health; 16Mississippi State Department of Health; 17Southern Nevada Health District, Las Vegas, Nevada; 18Nevada Department of Health and Human Services; 19New Jersey Department of Health; 20New York City Department of Health and Mental Hygiene; 21New York State Department of Health; 22North Carolina Department of Health and Human Services; 23Ohio Department of Health; 24Oklahoma State Department of Health; 25Pennsylvania Department of Health; 26South Carolina Department of Health and Environmental Control; 27Tennessee Department of Health; 28Texas Department of State Health Services; 29Utah Department of Health; 30University of Alabama School of Medicine, Birmingham, Alabama.
All authors have completed and submitted the International Committee of Medical Journal Editors form for disclosure of potential conflicts of interest. No potential conflicts of interest were disclosed.
* https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/people-with-medical-conditions.html.
† Location of death for all cases (121): hospital (79 [65.3%]), home (16 [13.2%]), ED (23 [19.0%]), hospice (one [0.8%]), and unknown (2 [1.7%])
§ https://wwwn.cdc.gov/nndss/conditions/coronavirus-disease-2019-covid-19/case-definition/2020/.
¶ https://www.cdc.gov/mis-c/hcp/.
** Jurisdictions reporting no deaths included Alaska, Delaware, District of Columbia, Guam, Hawaii, Idaho, Kentucky, Massachusetts, Missouri, Montana, New Mexico, Oregon, South Dakota, Vermont, Virginia, U.S. Virgin Islands, Washington, West Virginia, Wisconsin, and Wyoming.
†† Jurisdictions reporting one or more deaths included: Alabama, Arizona, California, Colorado, Connecticut, Florida, Georgia, Illinois, Indiana, Kansas, Louisiana, Maryland, Michigan, Minnesota, Mississippi, Nevada, New Jersey, New York City, New York State, North Carolina, Ohio, Oklahoma, Pennsylvania, South Carolina, Tennessee, Texas, and Utah.
§§ By age group the following decedents died at home or in the ED: infants (four of 12 [33%]), age 1–4 years (three of 11 [27%], age 5–9 years (two of 13 [15%]), 10–13 years (three of 12 [25%]), 14–17 years (nine of 23 [39%]), and 18–20 years (18 of 50 [36%]); overall, 39 (32%) of 121 decedents died at home or in the ED.
¶¶ Calculation is based on data from 72 decedents for whom information on onset date and hospital admission date were available.
*** Calculation is based on data from 60 decedents for whom information on hospital admission date and death date were available.
††† https://covid.cdc.gov/covid-data-tracker/#demographics.
§§§ https://covid.cdc.gov/covid-data-tracker/#cases_totalcases.
†††† https://www.cdc.gov/coronavirus/2019-ncov/community/health-equity/what-we-can-do.html.
References
- CDC. Coronavirus disease 2019 (COVID-19): CDC COVID data tracker. United States COVID-19 cases and deaths by states. Atlanta, GA: US Department of Health and Human Services, CDC; 2020. https://www.cdc.gov/coronavirus/2019-ncov/cases-updates/cases-in-us.html
- CDC. Multisystem inflammatory syndrome (MIS-C): health department-reported cases of multisystem inflammatory syndrome in children (MIS-C) in the United States. Atlanta, GA: US Department of Health and Human Services, CDC; 2020. https://www.cdc.gov/mis-c/cases/index.html
- Zimmermann P, Curtis N. COVID-19 in children, pregnancy and neonates: a review of epidemiologic and clinical features. Pediatr Infect Dis J 2020;39:469–77. CrossRef PubMed
- CDC. CDC Wonder: national population projections 2014–2060 request. Atlanta, GA: US Department of Health and Human Services, CDC; 2020. https://wonder.cdc.gov/population-projections-2014-2060.html
- Kim L, Whitaker M, O’Halloran A, et al.; COVID-NET Surveillance Team. Hospitalization rates and characteristics of children aged <18 years hospitalized with laboratory-confirmed COVID-19—COVID-NET, 14 States, March 1–July 25, 2020. MMWR Morb Mortal Wkly Rep 2020;69:1081–8. CrossRef PubMed
- Godfred-Cato S, Bryant B, Leung J, et al.; California MIS-C Response Team. COVID-19–associated multisystem inflammatory syndrome in children—United States, March–July 2020. MMWR Morb Mortal Wkly Rep 2020;69:1074–80. CrossRef PubMed
- CDC. Coronavirus disease 2019 (COVID-19): health equity considerations and racial and ethnic minority groups. US Department of Health and Human Services, CDC; 2020. https://www.cdc.gov/coronavirus/2019-ncov/community/health-equity/race-ethnicity.html
- Lange SJ, Ritchey MD, Goodman AB, et al. Potential indirect effects of the COVID-19 pandemic on use of emergency departments for acute life-threatening conditions—United States, January–May 2020. MMWR Morb Mortal Wkly Rep 2020;69:795–800. CrossRef PubMed
- Bramer CA, Kimmins LM, Swanson R, et al. Decline in child vaccination coverage during the COVID-19 pandemic—Michigan Care Improvement Registry, May 2016–May 2020. MMWR Morb Mortal Wkly Rep 2020;69:630–1. CrossRef PubMed
- Alderman EM, Breuner CC. Unique needs of the adolescent. Pediatrics 2019;144(6): e20193150.
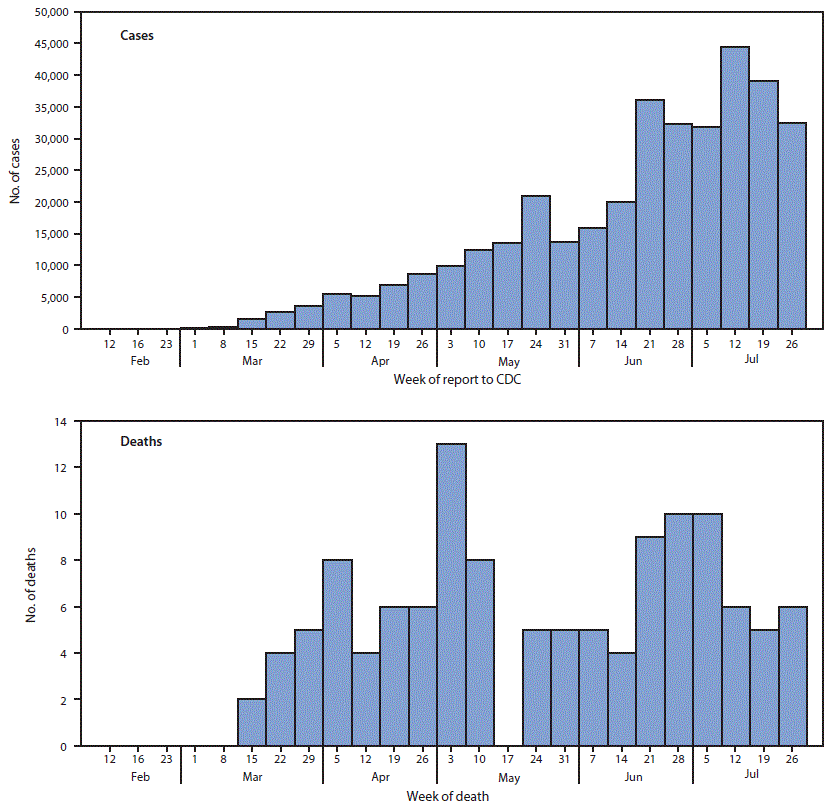
 FIGURE 1. SARS-CoV-2–associated cases,*,† by week of case report to CDC, and deaths,§,¶ by week of death,** among persons aged <21 years — United States, February 12–July 31, 2020
FIGURE 1. SARS-CoV-2–associated cases,*,† by week of case report to CDC, and deaths,§,¶ by week of death,** among persons aged <21 years — United States, February 12–July 31, 2020
* https://wwwn.cdc.gov/nndss/conditions/coronavirus-disease-2019-covid-19/case-definition/2020/.
† During February 12–July 31, 2020, 391,814 cases of coronavirus disease 2019 (COVID-19) in persons age <21 years were reported to CDC. Among these, date of report to CDC was missing for 34,538 cases not shown here. Weeks beginning February 12 and July 26 represent partial weeks, February 12–15 and July 26–31, respectively.
§ The first SARS-CoV-2–associated death in a person aged < 21 years in the United States occurred during the week beginning March 15, 2020.
¶ Includes 121 total decedents, 120 persons who met the case definition for COVID-19, 15 persons who met the case definition for multisystem inflammatory syndrome in children, and 14 persons who met both case definitions.
** Among 121 decedents, 94 had a recorded symptom onset date; median interval from symptom onset to death was 11 days (interquartile range = 6–24 days).
 FIGURE 2. Age at death among persons aged <21 years with SARS-CoV-2–associated deaths*,† — United States, February 12–July 31, 2020)§
FIGURE 2. Age at death among persons aged <21 years with SARS-CoV-2–associated deaths*,† — United States, February 12–July 31, 2020)§
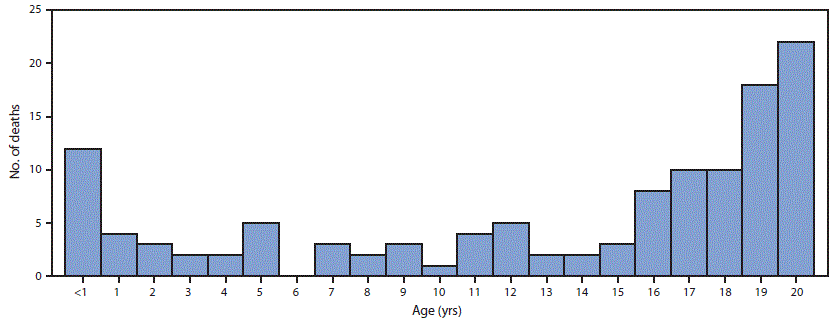
* https://wwwn.cdc.gov/nndss/conditions/coronavirus-disease-2019-covid-19/case-definition/2020/.
† https://www.cdc.gov/mis-c/hcp/.
§ Includes 121 total decedents, 120 persons who met the case definition for coronavirus disease 2019, 15 who met the case definition for multisystem inflammatory syndrome in children, and 14 persons who met both case definitions.
Abbreviations: COVID-19 = coronavirus disease 2019; IQR = interquartile range; MIS-C = multisystem inflammatory syndrome in children.
* Persons aged <21 years were included if they were reported by state and local health departments as meeting case definitions for COVID-19 (https://wwwn.cdc.gov/nndss/conditions/coronavirus-disease-2019-covid-19/case-definition/2020/) or MIS-C (https://www.cdc.gov/mis-c/hcp/) with a fatal outcome that occurred before August 1, 2020. Denominator for calculation of all percentages was total decedents with COVID-19 or MIS-C (121).
† Includes persons reported as multiracial and persons reported as being of another race without further specification.
§ Individual decedents could meet both definitions. Both confirmed (114) and probable (six) cases of COVID-19 are included in totals.
¶ Decedents could have more than one underlying condition. Categories include only decedents for whom the condition within the specified category was present at the time of illness onset as reported from state and local health departments.
** Among 34 decedents with chronic lung disease, 21 had additional information, including 19 with asthma and three with other lung disease. Decedents could have more than one chronic lung condition.
†† Decedents with body mass index ≥30 kg/m2 at or above the 95th percentile for age and sex.
§§ Among 26 decedents with neurologic or developmental disorders, 26 had additional information, including 10 with seizure disorders, 11 with neuromuscular disorders, and 20 with other neurologic and developmental conditions. Decedents could have more than one neurologic or developmental condition.
¶¶ Among 22 decedents with cardiovascular disease, 14 had additional information, including five with hypertension, three with lipid disorders, three with congenital heart disease, and six with other cardiovascular diseases. Decedents could have more than one cardiovascular condition.
*** Among 17 decedents with cancer and immunosuppressive conditions, 14 had additional information, including 10 with any history of cancer, two with immunosuppressive therapy, one with solid organ transplantation and three with other conditions. Decedents could have more than one condition in this category.
††† Includes decedents with type 1 and type 2 diabetes mellitus.
¶¶¶ Includes decedents with history of hematologic disorders (three), rheumatologic disorders (four), metabolic disorders (five), gastrointestinal disorders (five), endocrine disorders (six), dermatologic conditions (three), congenital disorders (14), psychiatric conditions (five), substance use disorder (three), smoking or vaping (two), pregnancy (one), and other medical conditions (nine). Decedents could have more than one condition in this category.
**** Calculation is based on decedents for whom information on symptom onset date and hospital admission date were available (72).
†††† Calculation is based on decedents for whom information on hospital admission date and date of death were available (60).
§§§§ Calculation is based on decedents for whom information on symptom onset date and date of death were available (94).
Suggested citation for this article: Bixler D, Miller AD, Mattison CP, et al. SARS-CoV-2–Associated Deaths Among Persons Aged <21 Years — United States, February 12–July 31, 2020. MMWR Morb Mortal Wkly Rep 2020;69:1324–1329. DOI: http://dx.doi.org/10.15585/mmwr.mm6937e4.
MMWR and Morbidity and Mortality Weekly Report are service marks of the U.S. Department of Health and Human Services.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All HTML versions of MMWR articles are generated from final proofs through an automated process. This conversion might result in character translation or format errors in the HTML version. Users are referred to the electronic PDF version (https://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.