Key points
- Antiretroviral therapy (ART) is recommended for all people with HIV, regardless of CD4 cell count.
- Assess your patients' readiness to begin ART.
- Help your patients adhere to ART by engaging in regular conversations at every office visit.
- Monitor your patients' viral load to confirm initial and sustained response to ART.

Treatment options
ART should be started as soon as possible after diagnosis and should be accompanied by patient education regarding the benefits and risks of ART and the importance of adhering to ART. People with HIV who are aware of their status should be prescribed ART and, by achieving and maintaining an undetectable (<200 copies/mL) viral load, can remain healthy for many years.1
ART reduces HIV-related morbidity and mortality at all stages of HIV infection and reduces HIV transmission.23456789 ART is known to reduce levels of multiple markers of immune activation and inflammation. Mortality associated with uncontrolled HIV replication at higher CD4 counts is believed to be due to immune activation and an inflammatory milieu that promotes progression of end-organ disease.
In the large, multinational Strategic Timing of Antiretroviral Treatment (START) study,3 asymptomatic patients with HIV infection who started ART immediately after diagnosis had a >50% reduction in morbidity and mortality compared with patients who deferred treatment until they had a CD4 count ≤350 cells/mm.10
ART reduces the chances of transmitting HIV to others. Three landmark studies have shown that treatment prevents sexual transmission of HIV.3411 Evidence shows that taking ART as prescribed can help achieve an undetectable viral load. When maintained, an undetectable viral load prevents transmission of HIV through sex.12 This is known as treatment as prevention.
| Transmission category | Chances of transmission with an undetectable viral load |
|---|---|
| Sex (oral, anal, or vaginal) 13, 14 | Studies have shown no chance of sexual transmission |
| Pregnancy, labor, and delivery 15 | 1% or less* |
| Sharing syringes or other drug injection equipment 16 | Unknown, but likely reduced |
| Breastfeeding 17 | Substantially reduces, but does not eliminate** |
* HIV transmission during pregnancy can be 1% or less if HIV medicine is taken daily as prescribed throughout pregnancy, labor, and delivery, and if the baby receives HIV medicine for 4–6 weeks after birth.
**People who have questions about breastfeeding or who desire to breastfeed should receive patient-centered, evidence-based counseling on infant-feeding options.
Patients starting ART should commit to treatment and understand the benefits and risks of therapy and the importance of adherence.
When assessing a patient's readiness to begin ART, stay objective and nonjudgmental. Make it clear that even if you do not share patients' views, you respect them. This helps to strengthen relationships with patients. It also encourages patients to be open with you and to adhere to treatment.

Connecting your patients diagnosed with HIV to medical care, including ART and other services, is essential.
The goal of HIV treatment is to achieve viral suppression. For someone who is virally suppressed, the amount of HIV in their body is very low or undetectable. This is important for people with HIV to stay healthy, live longer, and reduce their chances of transmitting HIV. People with HIV who take HIV medicines as prescribed and achieve and maintain an undetectable viral load (or stay virally suppressed) won't transmit HIV to a sexual partner.13 This is sometimes referred to as Undetectable=Untransmittable (U=U).

Use the following resources to find an HIV care provider when a referral is needed:
- American Academy of HIV Medicine
- HIV Medicine Association (by telephone: 703-299-1215)
- Ryan White HIV/AIDS Program (by telephone: 877-646-4772)
- HIV.gov
Long-term adherence to ART can be challenging, but talking to patients with HIV can help. Engage in regular conversations at every office visit to identify ART adherence barriers, offer adherence support services and provide information on other interventions to improve patient adherence.14

Once the conversation has started, you may find that patients are encountering barriers to adherence. Below are some common barriers and ways you can address them through routine conversations during patient visits.
Patient beliefs and behaviors, such as not taking their medications when they "feel well."
Explain the importance of consistent ART adherence even when they feel well or when their viral load is already undetectable and emphasize the decrease in chances of transmission when viral suppression is achieved.
Cognitive or organizational barriers, such as lack of logistic skills or low comprehension level.
- Offer advice about and tools for adherence, such as weekly pill boxes, dose reminder alarms, and linking dosing to daily events/activities.
- Use a feedback strategy (such as "tell me what you just heard") to help patients avoid confusion about new medicines, the dosing schedule, and/or a changed regimen.
Psychosocial barriers, such as mental health issues (e.g., depression, perceived low quality of life), drug or alcohol use, negative attitudes or beliefs about HIV, and lack of social support.
- When possible, refer patients to designated staff members, often called "patient navigators," for help in receiving essential support services related to mental health, substance use, and other support (e.g., psychologists, addiction specialists, support groups, adherence counselors, case managers).
- Remind patients not to share their ART with anyone.
- Encourage patients to recruit friends and/or family members to help with adherence.
Comorbid conditions such as diabetes, dyslipidemia, hypertension, and viral hepatitis may complicate the treatment and the patient's ability to adhere to the plan.
Regularly review the treatment plan and simplify the regimen if possible, considering patients' lifestyles and comorbidities. Anticipate (and plan to manage) possible drug interactions.
Structural barriers such as lack of transportation, housing, childcare, or insurance covering ART and long-term HIV care.
When possible, refer patients to patient navigators for help with issues such as lack of transportation, housing, childcare, and access to insurance.
Treatment competence or the ability to adhere to a potentially complicated and long-term regimen.
- Involve patients in decision making, when possible.
- Ensure that patients understand their treatment plan.
- Prepare patients for situations or changes in routine that could trigger nonadherence or short-term interruption.
- Encourage patients to keep 1-2 days' worth of medication on hand.
- Encourage patients to recruit friends and/or family members to help with adherence.
Short-term side effects that can occur when patients start or change ART regimens, such as nausea, fatigue, disturbed sleep, or dreaming can be concerning to patients.
- Alert patients that side effects, if they occur, are usually mild and short-lived and can be managed.
- Explain which side effects may occur with the ART they are taking.
- Anticipate and plan to manage any side effects.
- Instruct patients that if they experience side effects, they should seek help before stopping their ART regimen.
Regimen-related barriers, including fear of treatment and related side effects, as well as confusion about doses.
- Offer ART regimens that are highly effective and simple to take (e.g., once daily single-tablet dosing, few if any dietary restrictions).
- Explain that treatment has improved and is easier to take and better tolerated today than ever before.
- Encourage patients to recruit friends and/or family members to help with adherence.
Ask patients open-ended questions to assess adherence to medication. Engaging patients in brief conversations at every office visit can help build trust with patients by becoming more familiar with them, including challenges with adherence to their medication and barriers they face to staying in care.
In addition to supporting ART adherence, monitoring patients' viral loads is important. A patient's plasma HIV RNA viral load should be measured regularly to confirm initial and sustained response to ART. Most patients taking ART achieve viral suppression within 6 months.
Note: Patients may experience temporary increases or "blips" in their viral load, defined as viral loads transiently detectable at low levels. These blips usually go back down by the next viral load test. Patients using viral suppression as their primary prevention method who experience a blip should use other prevention strategies until their viral load is undetectable again. These prevention strategies could include condoms and PrEP for partners without HIV.
The frequency of viral load testing depends on several factors. Current guidelines recommend viral load monitoring as follows:10
- Initiation. With initiation of ART (before initiation and within 2-4 weeks after treatment initiation, followed by 4- to 8-week intervals until the levels become undetectable).
- Modification. After ART modification because of suboptimal response (within 2-4 weeks after treatment modification, followed by 4- to 8-week intervals until the levels become undetectable).
- Regimen Change. After ART modification because of toxicity or need for regimen simplification (within 4-8 weeks after changing therapy).
- Stable Regimen. In patients on a stable, suppressive ART regimen (every 3-4 months, or every 6 months if virally suppressed for more than 2 years, to confirm durable viral suppression).
- Suboptimal Response. In patients with suboptimal response (frequency depends on clinical circumstances).
Treatment recommendations
Three landmark studies have shown that treatment prevents sexual transmission of HIV.151617 Across these studies, no linked HIV transmissions were observed between mixed-HIV-status partners when the partner with HIV was virally suppressed (defined in these studies as having a plasma HIV RNA viral load less than either 200 or 400 copies/mL).
These data provide conclusive evidence of the power of viral suppression in preventing HIV transmission. Although statistically, a non-zero risk estimate cannot be completely ruled out, the data show that the best estimate for the chances of transmission is zero. Therefore, future HIV transmissions are not expected when people with HIV remain virally suppressed.

Taken as prescribed, antiretroviral therapy (ART) reduces the amount of HIV in the body to a very low level. This is known as viral suppression, and it keeps the immune system working and prevents illness. Viral suppression is defined as having less than 200 copies of HIV per milliliter of blood. ART can make the viral load so low that a test can't detect it. This is called an undetectable viral load.
Getting and keeping an undetectable viral load is the best way for people with HIV to stay healthy and prevent transmission of HIV through sex. This is sometimes referred to as treatment as prevention (TasP).
Patients may also refer to treatment as prevention as Undetectable = Untransmittable or U=U. The U=U campaign was developed by members of the HIV community to increase awareness about the relationship between viral suppression and the prevention of sexual transmission of HIV.
There is strong evidence about treatment as prevention for preventing HIV transmission through sex, but more research is needed for other ways, including breastfeeding and injection drug use.
Talking to patients with HIV about treatment as prevention is one of the best things you can do for their overall health and to stop HIV transmission. Speak to each patient at every visit to discuss the prevention steps they are taking and whether treatment as prevention is right for them.
These conversations can help you become familiar with each patient, including their adherence and likelihood of transmitting HIV. In addition, these conversations can help normalize discussions about topics like sex, substance use, and mental health.
Here are some tips and conversation starters to support patients with HIV:
- Share information with patients about the research on treatment as prevention and ask open-ended questions to start the conversation.
- Talk about the benefits of achieving and maintaining an undetectable viral load, including not being able to sexually transmit HIV to others.
- Emphasize that while treatment as prevention is effective, its success depends on achieving and maintaining an undetectable viral load. Note that if a patient's viral load increases, so does their chance of transmitting HIV to their partners through sex.
- Discuss the prevention steps patients are taking to help them adhere to their treatment regimen and maintain an undetectable viral load.
- Use the information patients share with you to identify barriers they may have to adhering to ART and ongoing care that may make it difficult for them to achieve and maintain viral suppression.

Using multiple HIV prevention methods is especially important if the person with HIV has trouble adhering to ART, has taken ART for less than 6 months, or has not yet achieved or maintained viral suppression.
To help people with HIV and their partners fully benefit from treatment as prevention, they should understand the benefits of and challenges with achieving and maintaining viral suppression. Some challenges include:
- Time to viral suppression. Most people will achieve an undetectable viral load within 6 months of starting ART. Many will become undetectable quickly, but it could take longer.
- Importance of regular viral load testing. Regular testing is critical to confirm that an individual has achieved and is maintaining an undetectable viral load. Data show a discordance between some people's self-report of their viral load status and laboratory measurements. This suggests that people may not know or be able to accurately report their viral load level.18
- Protection against other STIs. Taking HIV medicine and achieving and maintaining an undetectable viral load do not protect against STI transmission.
- Lack of awareness about the benefits of viral suppression. Knowledge of the prevention benefits of viral suppression may help motivate people with HIV and their partners to adopt this strategy. Studies have shown that many people do not know or do not believe that viral suppression works for prevention. For example, a survey among over 12,000 men who have sex with men showed that most participants without HIV and nearly one-third of participants with HIV thought that a message about the prevention benefits of having an undetectable viral load was inaccurate.19 Even when individuals understand that having an undetectable viral load protects against HIV transmission, they still tend to over-estimate the chances of transmission.20
Keeping patients in care
HIV care among people with diagnosed HIV in 47 states and the District of Columbia, 2021*
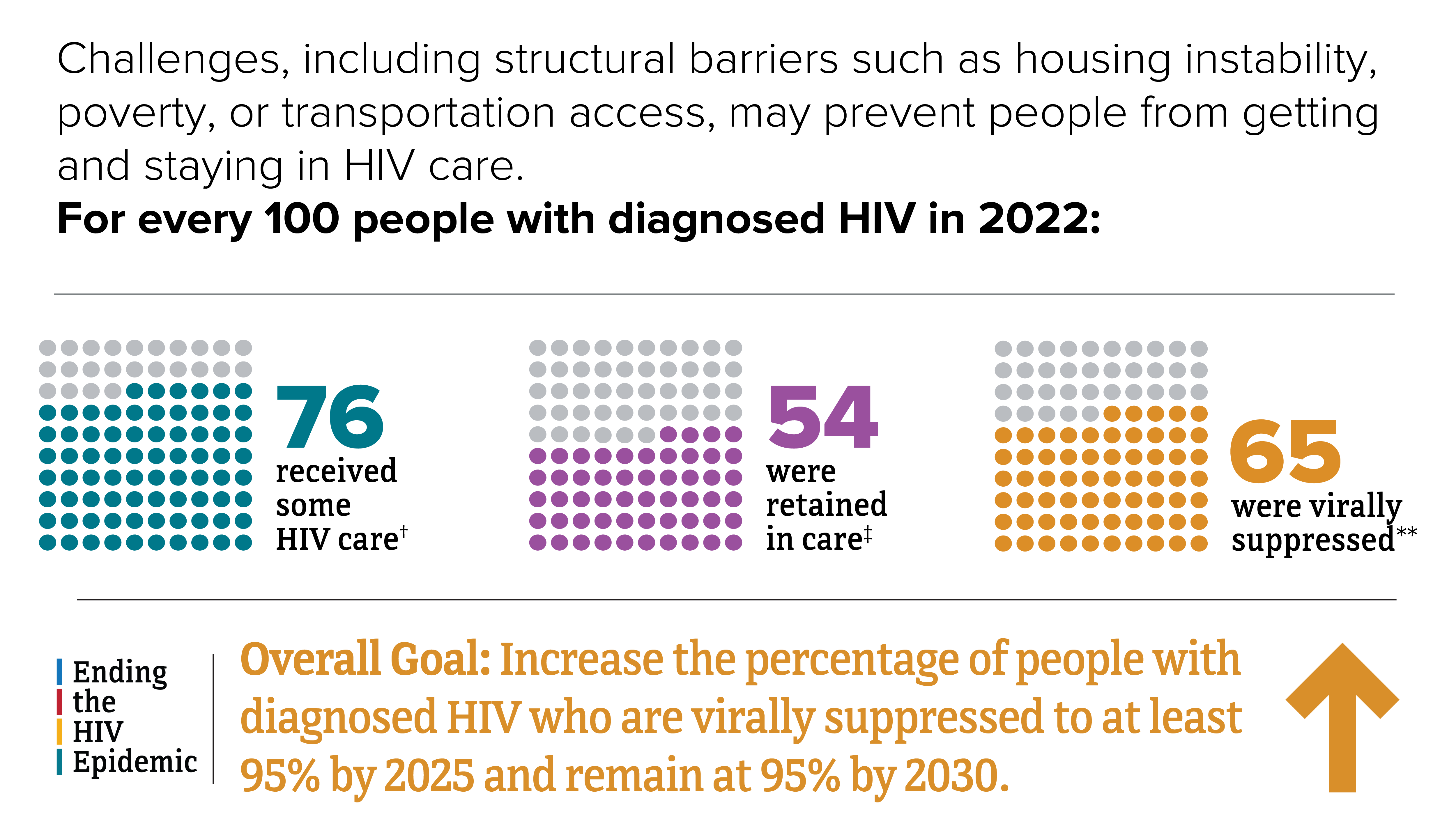
*Among people aged 13 and older.
† At least 1 viral load or CD4 test during 2022.
‡ Had 2 viral load or CD4 tests at least 3 months apart during 2022.
** Based on most recent viral load test during 2022.
Source: CDC. Monitoring selected national HIV prevention and care objectives by using HIV surveillance data—United States and 6 dependent areas, 2021. HIV Surveillance Supplemental Report 2023;28(4).
Regularly scheduled care can help support ART adherence, maintain decreased viral load and increased CD4 count, lower rates of progression to the most advanced stage of HIV, decrease rates of hospitalization, and improve overall health.212223
Poor retention in HIV care is more common in people who have substance use disorders; serious mental health problems; unmet needs such as housing, food, or transportation; limited financial resources or health insurance; or schedules that complicate adherence to HIV medication.
There are several ways you can help patients stay in HIV care, improve their medication adherence, achieve viral suppression, and improve their health outcomes:
- Clinic-wide marketing, (such as posters and brochures) and support (such as customer service training for patient-facing staff) to promote attending scheduled visits and provide patients with a welcoming experience.2425
- "Data to Care" approaches that use clinic and public health data to identify patients in need of retention, reengagement, or adherence support services to improve their health outcomes, including achieving viral suppression.262728
- Retention and re-engagement support for out-of-care people or patients at risk of falling out of care (such as patients who missed a care visit or are experiencing barriers to care engagement).
- A patient navigator to focus on retention, adherence, and reengagement efforts. The patient navigator can help with appointments, referrals, system navigation, service coordination, and transportation.25
- Medication adherence support for patients in care. Encourage your patients to download apps that help with appointment and medication reminders.
- Local or state health departments or local community-based organizations can help providers and HIV medical clinics by integrating their existing prevention services within the HIV care clinic to provide the support services your patients need to improve engagement in and adherence to HIV care.
Establishing patient trust is key to retention in care. Studies have found that low trust in health care providers and poor provider–patient relationships are associated with lower retention in HIV care and lower satisfaction with the clinic experience.293031 These findings underscore the need for providers to build supportive relationships with patients to help improve health outcomes.
Help patients modify behaviors that lead to poor retention in HIV care
- Communicate with patients nonjudgmentally to learn what they know about the importance of retention.
- Identify additional skills that patients might need to remain in care, such as problem-solving.
- Guide patients to identify possible changes to eliminate or reduce the barriers they face; congratulate patients when they can lessen these barriers.
- Strategize with patients to identify new goals and healthy behaviors.
- Actively refer patients to relevant clinic support services to provide additional support for retention.
Foster patient trust
- Be direct, nonjudgmental, and supportive.
- Use open-ended questions to involve patients in decision making regarding their HIV treatment and overall care.
- Include simple actions during patient encounters to foster communication, such as asking how patients prefer to be addressed.
Allow open communication and collaborative decision making
- Educate patients about their options and ask what questions come to mind.
- Encourage discussions on subjects about substance use, sexual behavior, and mental health.
- Provide referrals as appropriate and assess patients' willingness to complete the referral.*
Demonstrate interest in addressing barriers to care, including structural barriers, from the first interaction
- When possible, extend office hours or offer more flexible appointment times (e.g., offer some walk-in or same-day appointments).
- Maintain accurate patient contact information, updating it at every visit.
- Use patient-tracking systems to determine whether a patient has dropped out of care; contact patients promptly to reschedule missed appointments.
- Help patients find resources to address unmet needs and barriers to care. When possible, connect patients with childcare, transportation, or other services and offer co-location of primary care and social services.*
- When needed, encourage patients to access substance use or mental health services.
- Encourage patients to identify friends and family who can help with encouragement and support and attend medical appointments with them.
*Patient navigators, case managers, peer counselors, social workers, and treatment advocates can also assist with referrals and resources.
Talking with patients at each office visit allows you to reinforce positive behaviors, uncover barriers to successful long-term treatment, and facilitate access to services and resources as their needs change over time.

ART is a powerful tool to prevent HIV transmission. Health care providers who treat patients with HIV have an important role in supporting HIV prevention. Educating patients about the value of treatment as prevention can help them manage their HIV. Engaging patients in routine, brief conversations about treatment as prevention can also help you become more familiar with each of patients, including their adherence and chances of transmission.
Patients' health status, relationship status, and personal needs change over time. Therefore, conversations about risk reduction should continue and evolve for as long as the patient remains in care. Topics of these conversations can include, but are not limited to:
- Adherence to ART and ongoing medical care, even if the patient's viral load is undetectable.
- Communication of HIV status with others.
- Correct and consistent use of condoms with appropriate non-oil-based lubricants to prevent sexually transmitted infections (STIs), even when negotiations about condom use occur in the heat of the moment.
- How alcohol and/or drug use can impair judgment.
- The use of PrEP by partners without HIV, including people planning to become pregnant.
- The use of PEP by HIV-negative or unknown status partners in emergencies (e.g., when a condom breaks or is not used, and the patient is not virally suppressed).
Here are some conversation starters you can use to initiate brief conversations about reducing the chances of HIV transmission with patients:
- Disclosing HIV status to others. "Some of my patients have shared that it can be hard to decide who to tell about their HIV status or to know the best way to tell someone. Are you comfortable disclosing your HIV status to your sexual partners?"
- Couples where one partner has HIV and the other does not. "You mentioned your spouse [or partner] does not have HIV. Have they talked with their doctor about additional ways to protect themselves, such as PrEP?" or "I know you always use condoms, and that's terrific. But what do you do if your condom breaks while you're having sex with a partner who does not have HIV?"
Once you've started the conversation, you can identify teachable moments where you can help patients understand how to best protect their overall health and prevent transmission to partners.
Resources
Materials for you and your practice
Materials for your patients
- Panel on Antiretroviral Guidelines for Adults and Adolescents. Guidelines for the use of antiretroviral agents in adults and adolescents with HIV. Department of Health and Human Services. Accessed November 17, 2020. https://clinicalinfo.hiv.gov/sites/default/files/guidelines/documents/adult-adolescent-arv/guidelines-adult-adolescent-arv.pdf
- Bavinton B, Grinsztejn B, Phanuphak N, et al, for the Opposites Attract Study Group. HIV treatment prevents HIV transmission in male serodiscordant couples in Australia, Thailand and Brazil. Presented at the 9th IAS Conference on HIV Science; July 25, 2017; Paris, France.
- Garcia F, de Lazzari E, Plana M, et al. Long-term CD4+ T-cell response to highly active antiretroviral therapy according to baseline CD4+ T-cell count. J Acquir Immune Defic Syndr. 2004;36(2):702-713. https://journals.lww.com/jaids/fulltext/2004/06010/long_term_cd4__t_cell_response_to_highly_active.7.aspx
- INSIGHT START Study Group. Initiation of antiretroviral therapy in early asymptomatic HIV infection. N Engl J Med. 2015;373(9):795-807. https://www.nejm.org/doi/full/10.1056/NEJMoa1506816
- TEMPRANO ANRS Study Group, Danel C, Moh R, et al. A trial of early antiretrovirals and isoniazid preventive therapy in Africa. N Engl J Med. 2015;373(9):808-822. https://www.nejm.org/doi/full/10.1056/NEJMoa1507198
- Kitahata MM, Gange SJ, Abraham AG, et al. Effect of early versus deferred antiretroviral therapy for HIV on survival. N Engl J Med. 2009;360(18):1815-1826. https://www.nejm.org/doi/full/10.1056/NEJMoa0807252
- Mofenson LM, Lambert JS, Stiehm ER, et al. Risk factors for perinatal transmission of human immunodeficiency virus type 1 in women treated with zidovudine. Pediatric AIDS Clinical Trials Group Study 185 Team. N Engl J Med. 1999;341(6):385-393. https://www.nejm.org/doi/full/10.1056/NEJM199908053410601
- Wood E, Kerr T, Marshall BD, et al. Longitudinal community plasma HIV-1 RNA concentrations and incidence of HIV-1 among injecting drug users: prospective cohort study. BMJ. 2009;338:b1649. https://www.bmj.com/content/338/bmj.b1649
- Cohen MS, Chen YQ, McCauley M, et al. Prevention of HIV-1 infection with early antiretroviral therapy. N Engl J Med. 2011;365(6):493-505. https://www.nejm.org/doi/full/10.1056/NEJMoa1105243
- O'Brien WA, Hartigan PM, Martin D, et al. Changes in plasma HIV-1 RNA and CD4+ lymphocyte counts and the risk of progression to AIDS. Veterans Affairs Cooperative Study Group on AIDS. N Engl J Med. 1996;334(7):426-431. https://www.nejm.org/doi/full/10.1056/NEJM199602153340703
- Reynolds SJ, Makumbi F, Nakigozi G, et al. HIV-1 transmission among HIV-1 discordant couples before and after the introduction of antiretroviral therapy. AIDS. 2011;25(4):473-477. https://journals.lww.com/aidsonline/Fulltext/2011/02200/HIV_1_transmission_among_HIV_1_discordant_couples.9.aspx
- Hardy, WD. The art of ART adherence: a common-sense approach to helping patients adhere to life-saving drug therapy. HIV Specialist. 2012;4(3):30-32. https://aahivm.org/wp-content/uploads/2017/03/HIVspecialist_Oct_2012_FINAL.pdf
- Centers for Disease Control and Prevention. Evidence of HIV treatment and viral suppression in preventing the sexual transmission of HIV. Accessed August 27, 2021. https://www.cdc.gov/hiv/risk/art/evidence-of-hiv-treatment.html
- Bogart LM, Mutchler MG, McDavitt B, et al. A randomized controlled trial of Rise, a community-based culturally congruent adherence intervention for black Americans living with HIV. Ann Behav Med. 2017;51(6):868-878. https://academic.oup.com/abm/article/51/6/868/4648599
- Rodger AJ, Cambiano V, Bruun T, et al., for the PARTNER Study Group. Sexual activity without condoms and risk of HIV transmission in serodifferent couples when the HIV-positive partner is using suppressive antiretroviral therapy. JAMA. 2016;316:171-1811. https://jamanetwork.com/journals/jama/article-abstract/2533066?casa_token=C7mS84STqxYAAAAA:fpCmVNevXAccZf7JU-L9PDh3IjvENqfE17bqM1oed6CPP7BA4sxhlL3WmejJI2qaucFMCxs2Rw
- Bavinton BR, Pinto AN, Phanuphak N, et al. Viral suppression and HIV transmission in serodiscordant male couples: an international, prospective, observational, cohort study. Lancet HIV. 2018;5(8):e438-e447. https://www.sciencedirect.com/science/article/abs/pii/S2352301818301322
- Rodger AJ, Cambiano V, Bruun T, et al. Risk of HIV transmission through condomless sex in serodifferent gay couples with the HIV-positive partner taking suppressive antiretroviral therapy (PARTNER): final results of a multicentre, prospective, observational study. Lancet. 2019;393(10189):2428-2438. https://www.sciencedirect.com/science/article/pii/S0140673619304180
- Mustanski B, Ryan DT, Remble TA, D'Aquila RT, Newcomb ME, Morgan E. Discordance of self-report and laboratory measures of HIV viral load among young men who have sex with men and transgender women in Chicago: implications for epidemiology, care, and prevention. AIDS Behav. 2018;22(7):2360-2367. https://link.springer.com/article/10.1007/s10461-018-2112-7
- Rendina HJ, Parsons JT. Factors associated with perceived accuracy of the Undetectable = Untransmittable slogan among men who have sex with men: implications for messaging scale-up and implementation. J Int AIDS Soc. 2018;21(1):e25055. https://onlinelibrary.wiley.com/doi/full/10.1002/jia2.25055
- Rendina HJ, Cienfuegos-Szalay J, Talan A, Jones SS, Jimenez RH. Growing acceptability of Undetectable = Untransmittable but widespread misunderstandings of transmission risk: findings from a very large sample of sexual minority men in the United States. J Acquir Immune Defic Syndr. 2020;83(3):215-222. https://journals.lww.com/jaids/Fulltext/2020/03010/Growing_Acceptability_of_Undetectable__.4.aspx
- Tripathi A, Youmans E, Gibson JJ, Duffus WA. The impact of retention in early HIV medical care on viro-immunological parameters and survival: a statewide study. AIDS Res Hum Retroviruses. 2011;27(7):751-758. https://www.liebertpub.com/doi/abs/10.1089/aid.2010.0268
- Giordano TP. Retention in HIV care: what the clinician needs to know. Top Antivir Med. 2011;19(1):12-16. https://www.iasusa.org/tam/february-march-2011/
- Mizuno Y, Zhu J, Crepaz N, et al. Receipt of HIV/STD prevention counseling by HIV-infected adults receiving medical care in the United States. AIDS. 2014;28(3):407-415. https://journals.lww.com/aidsonline/fulltext/2014/01280/receipt_of_hiv_std_prevention_counseling_by.13.aspx
- Gardner LI, Marks G, Craw JA, et al. A low-effort, clinic-wide intervention improves attendance for HIV primary care. Clin Infect Dis. 2012;55(8):1124-1134. https://academic.oup.com/cid/article/55/8/1124/341728?login=true
- Higa DH, Crepaz N, Mullins MM; Prevention Research Synthesis Project. Identifying best practices for increasing linkage to, retention, and re-engagement in HIV medical care: findings from a systematic review, 1996-2014. AIDS Behav. 2016;20(5):951-966. https://link.springer.com/article/10.1007/s10461-015-1204-x
- Bove JM, Golden MR, Dhanireddy S, Harrington RD, Dombrowski JC. Outcomes of a clinic-based surveillance-informed intervention to relink patients to HIV care. J Acquir Immune Defic Syndr. 2015;70(3):262-268. https://journals.lww.com/jaids/fulltext/2015/11010/Outcomes_of_a_Clinic_Based_Surveillance_Informed.7.aspx
- Seña AC, Donovan J, Swygard H, et al. The North Carolina HIV Bridge Counselor Program: outcomes from a statewide level intervention to link and reengage HIV- infected persons in care in the South. J Acquir Immune Defic Syndr. 2017;76(1):e7-e14. https://journals.lww.com/jaids/fulltext/2017/09010/The_North_Carolina_HIV_Bridge_Counselor_Program_.17.aspx
- Udeagu CC, Webster TR, Bocour A, Michel P, Shepard CW. Lost or just not following up: public health effort to re-engage HIV-infected persons lost to follow-up into HIV medical care. AIDS. 2013;27(14):2271-2279. https://journals.lww.com/aidsonline/Fulltext/2013/09100/Lost_or_just_not_following_up__public_health.14.aspx
- Flickinger TE, Saha S, Moore RD, Beach MC. Higher quality communication and relationships are associated with improved patient engagement in HIV care. J Acquir Immune Defic Syndr. 2013;63(3):362-366. https://journals.lww.com/jaids/fulltext/2013/07010/Higher_Quality_Communication_and_Relationships_Are.15.aspx
- Dang BN, Westbrook RA, Hartman CM, Giordano TP. Retaining HIV patients in care: the role of initial patient care experiences. AIDS Behav. 2016;20(10):2477-2487. https://link.springer.com/article/10.1007/s10461-016-1340-y
- Magnus M, Herwehe J, Murtaza-Rossini M, et al. Linking and retaining HIV patients in care: the importance of provider attitudes and behaviors. AIDS Patient Care STDs. 2013;27(5):297-303. https://www.liebertpub.com/doi/abs/10.1089/apc.2012.0423
- Panel on Treatment of HIV in Pregnancy and Prevention of Perinatal Transmission. Recommendations for the use of antiretroviral drugs during pregnancy and interventions to reduce perinatal HIV transmission in the United States. Accessed February 3, 2023 https://clinicalinfo.hiv.gov/en/guidelines/perinatal/whats-new
- Wood E, Milloy MJ, Montaner JS. HIV treatment as prevention among injection drug users. Curr Opin HIV AIDS. 2012;7:151-156. https://journals.lww.com/co-hivandaids/Abstract/2012/03000/HIV_treatment_as_prevention_among_injection_drug.10.aspx
- Townsend CL, Cortina-Borja M, Peckham CS, de Ruiter A, Lyall H, Tookey PA. Low rates of mother-to-child transmission of HIV following effective pregnancy interventions in the United Kingdom and Ireland, 2000–2006. AIDS. 2008;22(8):973-981. https://journals.lww.com/aidsonline/Fulltext/2008/05110/HIV_infected_pregnant_women_and_vertical.00008.aspx