STEPS to Care: Establishing Policies and Protocols
Clear and relevant policies and procedures ensure that staff are informed and empowered to consistently deliver high-quality care to STEPS to Care clients. The protocols below provide a base from which to develop your own agency policies. They are divided here in four areas:
- Client selection, eligibility, and referrals
- Client scheduling, missed appointment, and outreach procedures
- Confidentiality and field safety protocols
- Internal staff meeting procedures
After reviewing the information and resources below, you will know:
- The purpose of each set of policies and protocols
- How to adapt policies and protocols for your agency
- The roles and responsibilities of staff members to implement policies and protocols
Client Selection, Eligibility, and Referral Procedures
Because of the intensive nature of the strategies in STEPS to Care, not all clients with HIV will benefit in the same way from these strategies. Choosing which of your clients are best suited for STEPS to Care will result in better patient experiences and outcomes.
Client Selection Criteria
STEPS to Care is recommended for adult patients who are either:
- Newly diagnosed
- Lost to care
- Patients that have difficulty attending appointments
- Patients that have indications of antiretroviral therapy (ART) challenges
Agency staff should work with medical providers to agree on which patients would benefit most and which criteria would be best to identify those patients. Agency staff should communicate with the medical providers who are referring patients to confirm whether a patient is lost to care, as these providers often have the most accurate information about a patient’s appointment adherence behavior.
Recommended Client Selection Criteria [PDF – 121 KB]
Referral Procedures
Patients are referred to STEPS to Care by affiliated primary care or medical providers, HIV screening programs, direct outreach, or a lateral transfer from similar care programs.
Program Directors should streamline the referral process to ensure client confidentiality. It is best to provide these procedures in writing for medical providers and Care Coordinators. The general referral process involves the following steps:

If the client is being referred through any service other than a medical provider (HIV rapid testing, for example), work with the service provider or agency to make sure a primary care appointment for the client is scheduled within 48 hours of referral and no more than 2 weeks from the referral date. An affiliated primary care provider should evaluate the client first and refer the client following the procedure outlined above.
Above all, during the referral process, the Care Coordinator, primary care provider or medical provider, and client should discuss what the STEPS to Care strategies are, how they will address client needs, and any questions the client might have.
Client Scheduling, Missed Appointments, and Outreach Protocols

It’s important for your agency to have clear and consistent scheduling procedures to help your team stay organized while tracking multiple appointment types for multiple clients. Your agency’s scheduling protocols should include:
- What needs to be documented and reported
- Best practices to ensure client appointment adherence
- Communication procedures (such as reminders) with the clients before and after each appointment.
Sample Scheduling Protocol [PDF – 71 KB]
This sample protocol includes recommended procedures for agency- and team-wide scheduling policies. Tools for use by Patient Navigators and Care Coordinators to schedule client meetings can be found on the Scheduling Client Meetings topic page.
Missed Appointment Procedures
Monitoring and following up on missed appointments ensure that clients remain in care or are brought back from being lost to care.
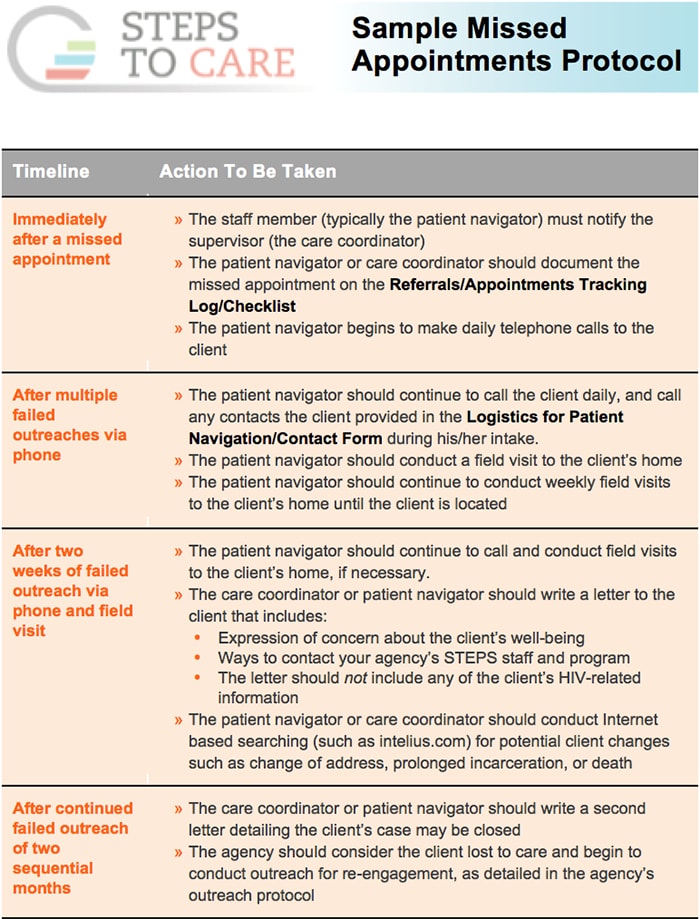
Sample Missed Appointment Protocol [PDF – 164 KB]
This sample protocol includes procedures for reaching out to clients after a missed appointment. It can be adapted to fit the needs of the agency’s client population and should take into consideration the information gathered during intake and reassessment regarding the specific client.

Outreach Procedures
STEPS to Care staff should make regular outreach attempts to find clients who have been lost to care and return them into care. This includes:
- Clients who have previously been part of your agency’s STEPS to Care
- Patients who have been lost to care (which could be defined as having at least one primary care visit within the last two years but none in the last nine months
- Patients who are part of STEPS to Care, have missed an appointment, and have been unreachable for over two months despite procedures in the Missed Appointment protocol
Sample Outreach Protocol [PDF – 39 KB]
Maintaining constant communication with the medical providers and facilities is important for successfully carrying out efficient and effective outreach. Here is a sample outreach protocol for reaching patients who may be lost to care. Typically, a Care Coordinator will conduct outreach activities.

Confidentiality and Field Safety Protocols
Confidentiality
Clients are often concerned about confidentiality. Therefore, it is very important for staff to understand confidentiality protocols and be prepared to openly discuss them with their clients. STEPS staff should implement these protocols within the agency, in the field, and through all forms of electronic communication. For more information and training on maintaining and discussing confidentiality with clients, see the Working with Clients in the Field topic page.
Sample Confidentiality Protocol [PDF – 28 KB]
Agency protocols on confidentiality should include:
- What agency and state/federal protocols exist for sharing and accessing HIV-related information
- What disclosure and HIV-related information is defined as
- Who is allowed to access HIV-related information
- Who is required to attend confidentiality trainings
- How to talk to clients about maintaining the confidentiality of their HIV status
- When disclosure without the client’s consent is justified (such as medical emergencies and the client does not have the capacity to consent)

Field Safety
Patient Navigators spend much of their time conducting field visits to client homes. Establishing concrete field safety and emergency protocols will keep staff safe, alert, and prepared to deliver field-based services.
Sample Field Safety Protocol [PDF – 29 KB]
Field safety and emergency protocols should align with what staff may face in your agency’s and client’s neighborhoods. For more information and training on staying safe in the field, see the Working with Clients in the Field topic page.
Agency protocols should cover:
- General field safety principles
- What to prepare before going out in the field
- What to bring out in the field
- Dress code
- Safety measures when traveling on foot, riding public transportation, or driving
- Techniques for handling dangerous situations
- Emergency protocols

Procedures for Internal Staff Meetings
Consistent staff meetings help Project Directors remain informed of clients, keep Care Coordinators alert to potential issues, and help Patient Navigators feel supported and prepared. The following section details common procedures for scheduling internal STEPS staff meetings. Consider the needs of your own staff when determining the frequency and structure of your meetings.
Morning Huddles
- You can use daily morning huddles to touch base before the day starts.
- Morning huddles are used to review the clients with appointments for that day, fill in gaps in coverage, and discuss potential challenges or issues.
- These daily huddles are typically attended by the Program Director, Care Coordinators, and Patient Navigators.
- They are a valuable way to start the day with all staff feeling informed and supported.
Supervision
- Supervision is a vital element of care coordination.
- Structured communication between staff members is needed to make sure staff members are equipped with the right tools and support to face complex challenges.
- Establishing a consistent schedule for supervision meetings ensures that supervision does not suffer when staff are short on time.
Learn more about best practices for conducting supervision meetings on the Staffing and Supervision topic page.
Group Training
- Program Directors and Care Coordinators can use information gained from programmatic supervision to create and lead relevant training sessions for Patient Navigators.
- These training sessions typically take place during weekly meetings, such as programmatic supervision meetings, and they can cover topics that are the most relevant and interesting to your Patient Navigators, such as mental health or communicating effectively.



