Tuberculosis (TB) in Healthcare Settings
General Information about TB
Transmission of Mycobacterium tuberculosis (M. tuberculosis [TB]) is a recognized risk to patients and healthcare personnel in healthcare settings. Transmission is most likely to occur from patients who have unrecognized pulmonary or larynx-related TB, are not on effective anti-TB therapy, and have not been placed in TB isolation. Transmission of M. tuberculosis in healthcare settings has been associated with close contact with persons who have infectious TB, particularly during the performance of cough-inducing procedures such as bronchoscopy and sputum induction. TB can spread through the air and can travel long distances. Cases of multidrug-resistant TB (MDR-TB, which includes extensively drug-resistant TB [XDR-TB]), have been recognized and are more difficult to treat.
Drug-resistant TB
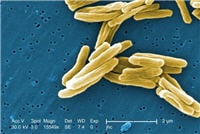
Mycobacterium tuberculosis
Drug-resistant tuberculosis is TB disease caused by M. tuberculosis organisms that are resistant to at least one first-line anti-TB drug. Multidrug-resistant TB (MDR-TB) is resistant to at least isoniazid (INH) and rifampicin (RIF). Extensively drug-resistant tuberculosis (XDR-TB) is a relatively rare type of MDR-TB. It is resistant to almost all drugs used to treat TB, including the two best first-line drugs: isoniazid and rifampin. XDR-TB is also resistant to the best second-line medications: fluoroquinolones and at least one of three injectable drugs (i.e., amikacin, kanamycin, or capreomycin). Treating and curing drug-resistant TB is complicated. Drug-resistant TB should be managed by, or in close consultation with, an expert in the disease.
- Infection Control in Health-Care Settings (Fact sheet) pdf icon[PDF 295 KB]
- Multidrug-Resistant TB (Fact sheet)
For more information visit CDC’s Tuberculosis (TB) web site
Diagnosis and Treatment
- Guidelines for Using the QuantiFERON®-TB Gold Test for Detecting Mycobacterium Tuberculosis Infection, U.S. 2005. MMWR 2005;54(RR15);49-55
- Guidelines for the Investigation of Contacts of Persons with Infectious Tuberculosis 2005 pdf icon[PDF 544 KB] MMWR 2005;54(RR-15):1-47.
- Treatment of Tuberculosis American Thoracic Society, CDC, and Infectious Diseases Society of America MMWR 2003;52 (.RR-11);1-77
- Diagnostic Standards and Classification of Tuberculosis in Adults and Children pdf icon[PDF 151 KB] Am. J. Respir. Crit. Care Med., Volume 161, Number 4, April 2000, 1376-1395
- Update: Fatal and Severe Liver Injuries Associated With Rifampin and Pyrazinamide for Latent Tuberculosis Infection, and Revisions in American Thoracic Society/CDC Recommendations — US, 2001 MMWR 2001; 50(34);733-5
Guidelines and Recommendations
- Guidelines for Preventing the Transmission of Mycobacterium tuberculosis in Healthcare Settings, 2005 MMWR 2005; 54 (No. RR-17, 1-141)
- Guidelines for Investigation Contacts of Persons with TB, 2005 MMWR 2005; 54(No.RR-15, 1-37)
- Prevention and Control of Tuberculosis in Correctional and Detention Facilities: Recommendations from CDC 2006 pdf icon[PDF 588 KB] MMWR 2006; 55( No.RR-9)
- Tuberculosis in the Workplaceexternal icon IOM preliminary report (National Academy Press)
- International Standards for Tuberculosis Care pdf icon[PDF 1.89 MB]external icon WHO 2006
- Tuberculosis Infection Control in the Era of Expanding HIV Care and Treatment pdf icon[PDF 360 KB]external icon