With CDC Support, Uganda Improves Emergency Medical Services During COVID-19 Pandemic
Summary
- With U.S. CDC’s technical expertise and support, Uganda’s Ministry of Health (MOH) and partners developed systems to vastly improve how patients were admitted to hospitals and clinics during COVID-19.
- Health workers were trained to quickly triage and prioritize treatment for patients.
- With CDC support, ambulances were equipped with supplies and fuel so more patients could be brought to health facilities.

Health staff - working for CDC partner organization Infectious Diseases Institute - prepare to transport a patient to a hospital in Kampala, Uganda. While caring for patients during the summer of 2021, ambulance staff were required to wear the highest level of personal protective equipment to prevent being exposed to particles in the air carrying the virus that causes COVID-19. Photo by Abubaker Kazibwe/IDI Makerere
Long before COVID-19 spread around the globe, emergency care services in many low-and middle-income countries, including Uganda, were very limited. Most hospitals in Uganda only had basic emergency services.
If someone needed emergency medical care, there wasn’t always a way to contact an ambulance, or ambulance services were not always available. If an ambulance was available, the driver usually didn’t have any medical training. The patient would often be taken to the hospital in a vehicle without any supplies or a paramedic. When the ambulance arrived at a hospital, most hospital staff were not trained to manage emergency conditions. In the few facilities that said they did triage patients, the process for doing so wasn’t always the same.
“Most public hospitals and clinics had serious emergency care staff shortages and no triage system for treating the sickest patients first,” explains CDC Uganda’s Global Health Protection Director, Amy Boore, MD. “It could happen that a person with a broken wrist would go first, even though the person next in line was critically ill or injured.”
Delayed arrival to healthcare facilities combined with a lack of a triage system to quickly identify and treat patients in critical condition often resulted in patients dying shortly after arriving at the hospital.
COVID-19 Pandemic Highlights Critical Gaps in Emergency Care
COVID-19 added more pressure on Uganda’s emergency care system. Many healthcare facilities lacked medical equipment like blood pressure cuffs or pulse oximeters, to read a patient’s oxygen levels. Without these basic tools, many seriously ill COVID-19 patients – who might have looked healthy even as their bodies were starved of oxygen – could easily be overlooked.
With these challenges, there was an urgent need to train health workers to quickly triage and prioritize treatment for patients.

An ambulance drives down a street in Kampala in July 2021. With support from CDC, health officials in Uganda improved their ambulance service during the COVID-19 pandemic. Photo by Abubaker Kazibwe/IDI Makerere
Improving Triage for Emergency Care
The Emergency Medical Services (EMS) department at the Ministry of Health (MOH) was able to identify gaps, assess needs, and work with local Ugandan partners from government facilities and the academic community (Makerere University College of Health Sciences and Mbarara University of Science and Technology),CDC, and other health partners (Infectious Diseases Institute {IDI}, Baylor Uganda, Walimu, Seed Global Health, and Emergency Care Society Uganda) to fill gaps in emergency medical services in Uganda.
As a trusted partner in Uganda, CDC sprang into action to improve triage for emergency care.
With minimal resources, a small team of staff from the MOH, CDC, and partners worked to vastly improve emergency care by supporting multiple levels of health facilities in Uganda.
“We were able to use our technical expertise, existing programs in the country, and emergency funding to support Uganda’s MOH,” says Boore.
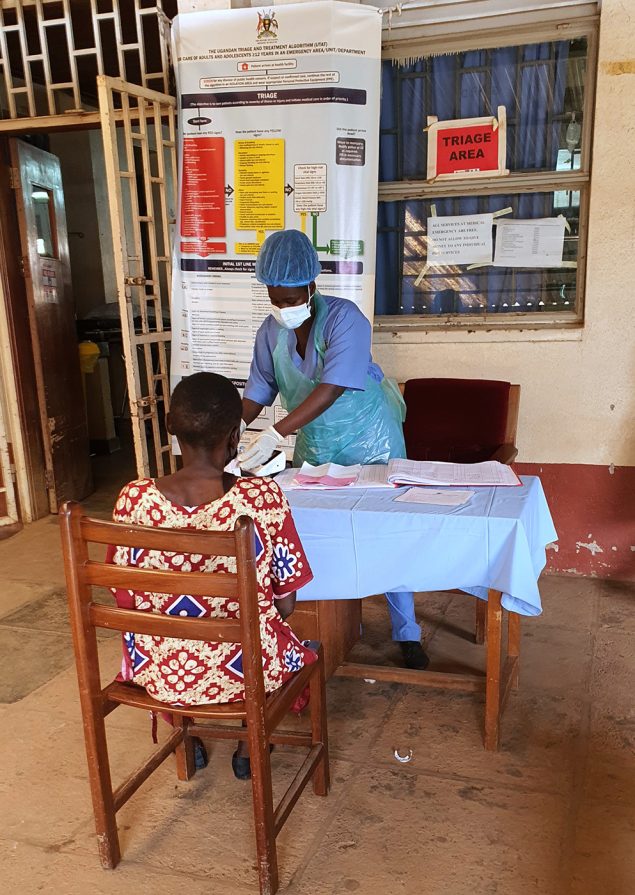
A patient is screened using the Uganda Triage and Treatment Algorithm (UTAT) at the Mulago National Referral Hospital in Kampala, Uganda. UTAT was developed by Ugandan health officials with support from the U.S. CDC office in Uganda. This triage system allows health officials to determine which patients need to be treated first based on the severity of their illness. Photo by Kambugu Carl Trevor/IDI Makerere
CDC worked with Uganda’s MOH and partners to borrow best practices from existing triage systems to create the Uganda Triage and Treatment Algorithm (UTAT) – an EMS training curriculum, with both adult and child options. CDC supported the development of the UTAT during a 3-day day meeting with educators and emergency services partners led by the MOH. The final UTAT triage process was printed on posters that could be easily displayed at health facilities.
The new triage guidelines divide patients into three categories for treatment:
- “Red” patients are treated within 10 minutes of arriving at the hospital.
- “Yellow” patients are treated within one hour.
- “Green” patients are treated after those with emergency conditions are managed.
CDC supported Uganda’s first health worker training on how to use UTAT. Working with the MOH and partners, CDC staff developed instructions for triaging and transferring patients and provided funding to six regional referral hospitals (RRH) in Uganda.
This allowed each RRH to have a dedicated regional coordinator to manage the transfer of
patients between facilities.
With CDC support, 18 phones, SIM cards, and phone call minutes were bought for the regional hospitals’ EMS departments to ensure access to communication between healthcare facilities.
This allowed lower-level facilities to contact the larger referral hospitals to confirm if they were able to accept and treat a seriously ill patient and seek clinical advice before the transfer.
Upgrading Uganda’s Ambulance Service
A well-coordinated emergency medical system needs ambulances and health facilities that can provide appropriate life-saving services during and after the transfer of patients. Uganda needed more ambulances filled with life-saving supplies so patients could get adequate care when they needed it.
In Uganda, lack of fuel, limited ambulance drivers, and emergency medical technicians were some of the barriers to proper emergency medical care. CDC’s support helped buy emergency fuel to ensure ambulances were operating where the need was greatest.
Building on Emergency Management System Successes
Uganda’s improved EMS system is a testament to CDC, MOH and other partners working so well together to address common needs.
With CDC’s technical and financial support, the MOH and partners continue to build on these EMS successes and expand training sessions and triage implementation across the country. They continue to partner to improve life-saving medical care for all Ugandans during the COVID-19 pandemic and beyond.