Uganda FETP Fellows Address COVID-19 Challenges with Timely Research
November 8, 2022
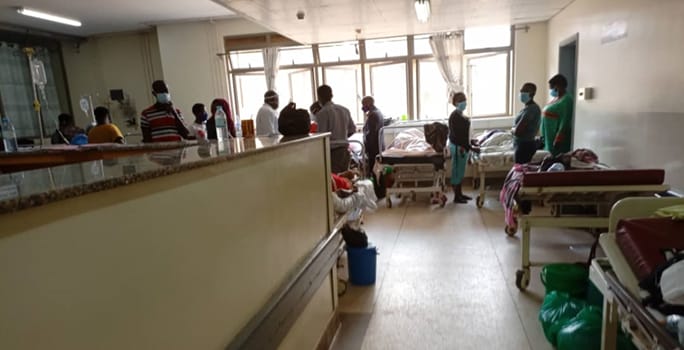
An Advanced FETP fellow took this photo of a hospital that mixed COVID-19 and non-COVID-19 patients due to limited space. Photo: Dr. Patience Mwine
In early 2020, when COVID-19 was becoming a global threat, the Ugandan Ministry of Health (MOH) sprang into action to protect the health of its citizens and stall the spread of COVID-19 in Uganda for as long as possible. The MOH relied on a workforce of disease detectives trained through the Uganda Field Epidemiology Training Program (FETP) and supported by U.S. Center for Disease Control & Prevention (CDC). The presence of a ready, trained workforce integrated into the MOH to be responsive to emergent needs and provide critical data on demand greatly contributed to the successful COVID-19 response in Uganda.
FETP and Contributions to the COVID-19 Response
CDC’s FETP trains epidemiologists in more than 80 countries, including Uganda. The program has three dedicated levels: 1) FETP-Advanced, which trains fellows who work with the Uganda MOH and other national-level government agencies; 2) FETP-Intermediate, which trains public health workers at the regional level or district level; and 3) FETP-Frontline, which trains public health workers at the local and community level. Together, epidemiologists at different levels work to prevent diseases from spreading and communicate rapidly as part of coordinated efforts at the national, regional and local levels.
Uganda’s FETP fellows and graduates responded quickly to the crisis. They coordinated early airport screening activities, traced contacts, and managed a call center to address public concerns. Fellows also conducted studies to provide crucial data to inform and improve the MOH’s response. Between March 2020 and September 2021, they conducted more than 70 major COVID-19-focused projects. These activities included assessing facilities’ readiness to manage patient increases and protect healthcare workers, using data to address rumors about vaccines and COVID-19, and studying how community leader engagement could improve vaccination coverage.
Fellows Use Evidence-Based Approach to Assess Gaps in the Health System

Advanced FETP fellow Sarah Elayeete searches for COVID-19 patients records at a Kampala Hospital in June 2021. Photo: Dr. Rose Nampeera, Advanced FETP fellow, Cohort 2021
To respond to COVID-19 effectively, health centers needed various measures in place to prevent the spread of infection. This included isolating COVID-19 patients in health facilities, providing personal protective equipment for health workers, recording, and reporting positive patients to the government.
As cases of COVID-19 increased throughout Uganda’s second wave in 2021, FETP fellows conducted a national study to find out if health facilities across all levels of the health system were ready to receive and treat COVID-19 patients. This study identified several gaps. Some facilities combined COVID-19 and non-COVID-19 patients due to a lack of space to treat patients. Many facilities did not have enough personal protective equipment for healthcare workers, and some had broken oxygen generators. Lower-level facilities, where many patients presented first, were the most unprepared. They lacked triage systems or ways to isolate suspected patients while they waited for referrals. In addition, although most of the country had shifted to using rapid test kits, no mechanism existed to allow facilities to report results to the national tracking system. This resulted in the undercounting of thousands of cases over several weeks.
Key Findings Strengthen the Response to COVID-19
In May 2021, FETP fellows presented their study to the MOH. As a result, the MOH made changes such as reporting rapid test results, expanding available space to accommodate COVID-19 patients, and assigning additional staff to an understaffed referral hospital. The inclusion of rapid tests in reporting added thousands of backlogged case identifications that had not been reported previously, provided a more accurate picture of the pandemic, and enabled better decision-making within the healthcare system.
The team also examined the COVID-19 vaccination rates of frontline healthcare workers. “The results of their evaluation were alarming,” says Dr. Julie Harris, CDC Uganda FETP Resident Advisor. “By May 2021, only 13% of facilities had fully vaccinated healthcare workers for COVID-19. Many districts tested patients using rapid tests but didn’t know how to report their positive results. In some districts, hundreds of cases had been diagnosed with rapid tests, but they were not recognized at the national level. From the findings of the various studies, FETP fellows made recommendations to help address the gaps identified.”
Using Research to Address Misconceptions and Promote the COVID-19 Vaccine

Bob Amodan, an Advanced FETP fellow, interviews community members regarding their feelings about the COVID-19 vaccine. Photo: Julius Asiimwe, Assistant DHO, Rwampara District
FETP fellows also investigated rumors from the community about COVID-19 and vaccines. The vaccine became available in Uganda in early 2021, just months before the second wave. Almost immediately after the start of the second wave, the community shared concerns that many fully-vaccinated Ugandans were dying from COVID-19 in hospitals. In addition, rumors were circulating that hospitalized patients were much younger during the second wave than the first. To investigate these rumors, FETP fellows collected and compared data on both COVID-19 patients who were hospitalized and those who were not hospitalized during both waves. Although the team found that patients were dying in hospitals in both waves because vaccine distribution was fairly new in Uganda, the investigators found that no COVID-19 patients were fully vaccinated, regardless of whether or not they were hospitalized.
In addition, the investigators found that patients hospitalized during the second wave were older, rather than younger when compared to those who were hospitalized during the first wave.
MOH shared these findings in a widely disseminated social media message campaign which aimed to reassure the public that their concerns were being addressed by providing evidence to counter the rumors.
Even after the COVID-19 vaccines became available in Uganda, uptake was slow among the public. Studies suggested that community members would be more willing to take the vaccine if community leaders took it first. When the vaccine became available in March 2021, fellows met with district leaders to identify ways to promote the vaccine among the leaders themselves. With the support of Baylor-Uganda, fellows conducted ‘dialogue meetings’ between study staff and district leaders in which they provided information about vaccine effectiveness and safety and allowed leaders to discuss the topic amongst themselves. Each meeting lasted several hours and addressed the concerns of the participants. After the meetings, leaders expressed less fear of the vaccine and more willingness to get vaccinated. As a result, the MOH supported the roll-out of additional dialogue meetings to promote the vaccine.
An Award-Winning Program of Excellence
Overall, Uganda’s FETP fellows were engaged in nearly every aspect of the COVID-19 response. The efforts of this trained, devoted workforce helped keep Uganda’s case counts and deaths low. The fellows’ successes were apparent not only in Uganda but also within CDC and the global public health community.
Fellows have won many awards at the FETP International Nights, an event during which fellows from all FETP countries present their work. In 2016 and 2018, fellows won awards for their scientific oral and poster presentations. In addition, in 2017 and 2021, FETP Uganda won the Director’s Award for Excellence in Epidemiology and Public Health Response.
This recognition highlights the importance and impact of having a well-developed, integrated program that trains health professionals on all levels to respond to a country’s needs. Uganda FETP’s significant contribution resulted in a successful response to COVID-19 in Uganda and many lives saved.

