Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail.
Clinical and Behavioral Characteristics of Adults Receiving Medical Care for HIV Infection — Medical Monitoring Project, United States, 2007
Corresponding author: Janet M. Blair, National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention, CDC. Telephone: 404-639-6298; E-mail: JBlair@cdc.gov.
MMWR in Brief summarizes key points from "Clinical and Behavioral Characteristics of Adults Receiving Medical Care for HIV Infection — Medical Monitoring Project, United States, 2007." MMWR 2011; 60(No. SS-11). Available at: http://www.cdc.gov/mmwr/preview/mmwrhtml/ss6011a1.htm.Certain text might not have appeared in the original publication.
New Information
This is the first large scale, nationally representative study of HIV-infected adults receiving medical care since the HIV Cost and Services Utilization Study. The Medical Monitoring Project (MMP) was created in response to an Institute of Medicine report(1).
Analysis
To describe the clinical and behavioral characteristics of adults receiving medical care for human immunodeficiency virus (HIV) infection at participating surveillance sites (26 project areas in 19 states and Puerto Rico). Clinical and behavioral characteristics of participants included: 1) delays in seeking medical care and use of health-care services; 2) antiretroviral medications and adherence, CD4 T-lymphocyte and HIV viral load testing, and vaccinations; 3) unmet need for services; 4) alcohol and drug use; 5) sexual behavior; and 6) prevention activities.
Data Source
MMP is an ongoing, supplemental surveillance project that collects interview data on health-related behaviors, clinical outcomes, and quality of care of HIV-infected adults aged ≥18 years who are receiving medical care.
Summary Findings
The results from the 2007 MMP cycle indicated that among 3,643 participants, 3,040 (84%) had some form of health insurance or coverage during the 12 months preceding the interview. Of these, 45% reported having Medicaid, 37% reported having private health insurance or coverage through a health maintenance organization, and 30% reported having Medicare.
A total of 3,091 (85%) of the participants were taking antiretroviral medications (ART). Of 3,592 participants who reported having a CD4 T-lymphocyte test, 36% had a CD4 count of ≥500 cells/mm3 (Figure 1). Among 3,546 participants who reported having an HIV viral load test, the most recent viral load was undetectable for 58% (Figure 2). Approximately 83% reported having three or more CD4 and/or viral load tests during the preceding year.
Among 3,643 participants, 45% needed HIV case management, 33% needed mental health counseling, and 32% needed assistance finding dental services during the 12 months preceding the interview. Of these participants, 8%, 13%, and 25% respectively, had not received these services by the time of the interview.
Excessive drinking (five or more drinks per day for men, four or more for women) during the preceding 30 days was reported by 500 (14%) participants. Overall, 1,117 (31%) participants reported using noninjection drugs during the preceding year. The most frequently used drugs were marijuana (23%), amyl nitrate (7%), cocaine that is smoked or snorted (7%), and crack cocaine (6%). Three percent of participants injected drugs for nonmedical purposes during the preceding year.
The proportion of MMP participants who had unprotected anal or vaginal intercourse with at least one partner during the preceding 12 months varied by the sex of the participants and their partners: 32% (176 of 553) of males with a female sex partner, 42% (216 of 516) of females with a male sex partner, and 54% (527 of 970) of males with a male sex partner. However, the proportion of males and females who reported that they knew the HIV status of their most recent sex partner was similar for the three groups (range: 78%-83%).
Limitations
Because of the low participation rate (40%) for 2007, the results might not be nationally or locally representative and are not generalizable to all HIV-infected persons receiving care in the United States. Clinical information for this report (CD4+ T-lymphocyte count and HIV viral load) was obtained through patient interview. Because medical record abstraction data were not available for inclusion in this document, information reported by participants and medical record abstraction could not be compared. CDC plans to release future MMP data that will provide representative estimates.
Public Health Implications
Public health recommendations from CDC and others note the importance of linkage to support services and retention in medical care. Missed opportunities to link patients to critical support services can adversely impact access to care, ART adherence, retention in medical care, and quality of life. Integration of substance abuse treatment services into clinical-care settings can address these gaps. Clinicians can incorporate nonjudgmental counseling regarding unprotected sex to encourage safer behaviors.
MMP data can be used to monitor the National HIV/AIDS Strategy goal of increasing access to care and optimizing health outcomes among persons living with HIV. Prevention planning groups, state and local health departments, policy leaders, health-care providers, and persons living with HIV can use the data to focus HIV prevention activities and highlight disparities in care and services, identify unmet support service needs, guide policy and funding decisions, and allocate resources where they are most needed.
Reference
- Institute of Medicine. Measuring what matters: allocation, planning and quality assessment for the Ryan White CARE Act. Washington, DC: National Academies Press; 2004:1-302.
FIGURE 1. Most recent self-reported CD4 T-lymphocyte count* among persons with HIV infection — Medical Monitoring Project, United States, 2007
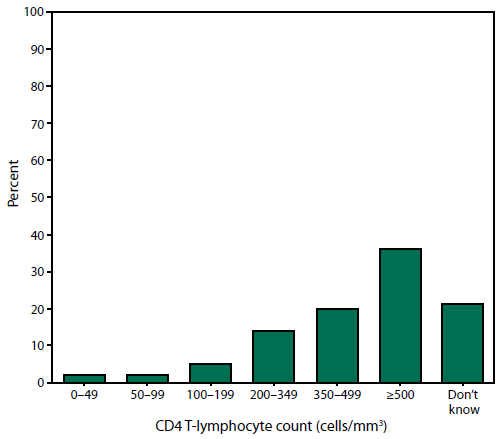
*N = 3,592. Among participants who reported having a CD4 T-lymphocyte test during the past 12 months; excludes refused, skipped, and missing responses.
Alternate Text: The figure is a bar chart that presents the most recent self-reported CD4 T-lymphocyte count among persons with HIV infection during 2007. Counts range from 0 to >500 cells/mm3 and includes a category for those who did not know their count.
FIGURE 2. Most recent self-reported HIV viral load* among persons with HIV infection — Medical Monitoring Project, United States, 2007
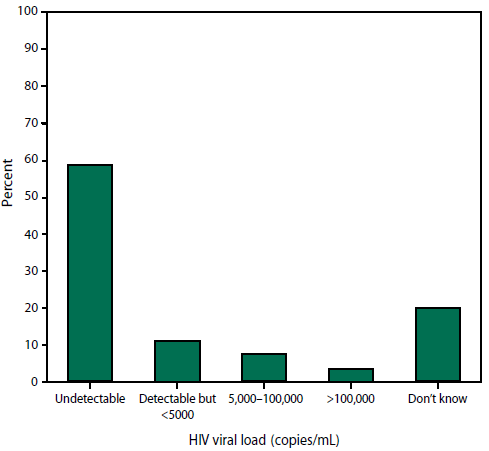
* N = 3,546. Among participants who reported having an HIV viral load test during the past 12 months; excludes refused, skipped, and missing responses.
Alternate Text: The figure is a bar chart that presents the most recent self-reported HIV viral load among persons with HIV infection during 2007. It includes categories for undetectable, detectable but <5,000, 5,000-100,000, >100,000, and don't know.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All MMWR HTML versions of articles are electronic conversions from typeset documents.
This conversion might result in character translation or format errors in the HTML version.
Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr)
and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S.
Government Printing Office (GPO), Washington, DC 20402-9371;
telephone: (202) 512-1800. Contact GPO for current prices.
**Questions or messages regarding errors in formatting should be addressed to
mmwrq@cdc.gov.


