Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail.
Imported Human Rabies in a U.S. Army Soldier — New York, 2011
On August 19, 2011, a male U.S. Army soldier with progressive right arm and shoulder pain, nausea, vomiting, ataxia, anxiety, and dysphagia was admitted to an emergency department (ED) in New York for suspected rabies. Rabies virus antigens were detected in a nuchal skin biopsy, rabies virus antibodies in serum and cerebrospinal fluid (CSF), and rabies viral RNA in saliva and CSF specimens by state and CDC rabies laboratories. An Afghanistan canine rabies virus variant was identified. The patient underwent an experimental treatment protocol (1) but died on August 31. The patient had described a dog bite while in Afghanistan. However, he had not received effective rabies postexposure prophylaxis (PEP). In total, 29 close contacts and health-care personnel (HCP) received PEP after contact with the patient. This case highlights the continued risks for rabies virus exposure during travel or deployment to rabies-enzootic countries, the need for global canine rabies elimination through vaccination, and the importance of following effective PEP protocols and ensuring global PEP availability.
Case Report
On August 14, 2011, a previously healthy soldier, aged 24 years, traveled from Grafenwöhr, Germany, to Fort Drum, New York, to begin a new military assignment (Figure). In transit, he experienced neck and shoulder pain and right arm and hand paresthesias. During the days following, he experienced fever, nausea, vomiting, and on August 18, difficulty swallowing. He visited the ED at hospital A on August 15 and 17 and was discharged with diagnoses of neck tendinitis and gastritis, respectively. He twice visited a chiropractor for his pain during August 15–16.
On August 19, the patient experienced ataxia and syncope, was evaluated at Fort Drum's medical facility, and was transferred to the ED at hospital A. Upon arrival, he was dehydrated and markedly hydrophobic. He was lucid and described having received a dog bite on the right hand during January 2011 while deployed to Afghanistan. Rabies was suspected on the basis of symptoms and this history. The New York State Department of Health (NYSDOH) and CDC were notified. The patient was transferred to hospital B, where a nuchal skin biopsy was performed and samples of serum, saliva, and CSF obtained. On August 20–21, Wadsworth Center (NYSDOH's public health laboratory) detected rabies virus antigens in hair follicles of nuchal skin biopsy specimens by direct immunofluorescence, and rabies viral RNA in saliva and CSF by reverse transcriptase–polymerase chain reaction. CDC corroborated these findings and detected rabies virus antibodies in serum and CSF. The viral RNA sequence was compatible with a canine rabies virus variant associated with dogs in Afghanistan.
Before the patient's admission to hospital B, staff members were notified, and isolation precautions (including goggles, gowns, gloves, and face masks for all HCP who had contact with the patient) were instituted. Upon admission, the patient exhibited severe aerophobia and hydrophobia, became combative and agitated, and was intubated for airway protection. Dysautonomia and fixed dilated pupils were noted. Computed tomography scan of the brain revealed no abnormalities. Complete heart block required temporary pacemaker placement. Ketamine, fentanyl, and midazolam were administered according to an experimental treatment protocol (1). On hospitalization day 2, an external ventricular drain was placed to monitor intracranial pressure. On day 3, the patient experienced severe neurogenic diabetes insipidus. On day 4, severe brain edema caused erratic intracranial pressure measurements. The patient experienced severe acute respiratory distress syndrome. Extracorporeal membrane oxygenation, anticoagulation, and a hypothermia protocol were started. Chest radiographs indicated worsening confluent parenchymal opacities. These findings, in addition to leukocytosis, prompted intravenous vancomycin and ceftazidime administration beginning on day 6.
On days 10–11, computed tomography revealed two small intracerebral hemorrhages. On day 11, extracorporeal membrane oxygenation and anticoagulation were discontinued, fresh frozen plasma and factor VII were administered, and mechanical ventilation maintained oxygen saturation. On day 12, severe intracerebral hemorrhage was evident, and recovery was deemed unlikely. With the family's agreement, life support was withdrawn on day 13 (August 31), and the patient died.
Wadsworth Center and CDC tested specimens daily for clinical monitoring (1). Rabies virus–specific immunoglobulin M and immunoglobulin G antibodies were present and increased in serum and CSF throughout hospitalization. Virus neutralizing antibodies (VNA) were first detected in serum at 0.07 IU/mL on August 28 and increased to 0.50 IU/mL on August 31, the day the patient died. No VNA were detected in CSF through August 29, the last day a sample was submitted.
On autopsy, all central nervous system specimens demonstrated edema and mononuclear inflammation. Neurons contained eosinophilic intracytoplasmic inclusions. Immunohistochemical and immunofluorescent staining revealed abundant rabies virus antigens distributed diffusely.
Public Health Investigation
Beginning on August 19, public health officials from multiple jurisdictions were notified about the case. Local health departments and the U.S. Army, with assistance from NYSDOH and CDC, interviewed the patient's close contacts, including friends, family members, fellow travelers, HCP, hotel staff members, and members of his new and former military units to provide risk assessments and PEP recommendations. Interviewees were counseled regarding rabies virus exposure risks and types of contact that constitute exposures. The patient was considered potentially infectious during the 14 days before illness onset, per CDC recommendations (Charles E. Rupprecht, CDC, personal communication, 2012).
The investigation identified approximately 190 persons who had interacted with the patient during his travel or while in New York. Thirteen persons met exposure criteria (defined as wound or mucous membrane exposure to the patient's saliva, CSF, neural tissue, or tears) and received PEP consistent with Advisory Committee on Immunization Practices guidelines (2). All exposures occurred before rabies was suspected. Nine HCP contacts without confirmed exposures also received PEP. No seatmates on flights from Germany to New York had exposures requiring PEP. Among 50 assessed members of the patient's previous Army unit in Germany, seven met exposure criteria and received PEP. The patient had no known contact with additional persons in Germany, except a taxi driver, who did not require PEP.
In January 2011, while in Afghanistan, the patient reported to family members and close friends that he had been bitten by a feral dog and had sought medical treatment, which he described as wound cleansing and injections. However, an Army investigation revealed no documentation of a reported bite wound or treatment. A May 2011 banked serum specimen, tested at CDC in August 2011, did not contain rabies virus–specific antibodies or VNA, further indicating that the patient had not received PEP. No record of submission of the dog for rabies diagnosis was obtained.
Reported by
Waleed Javaid, MD, Ioana G. Amzuta, MD, Amritpal Nat, MD, Upstate Univ Hospital, State Univ of New York; Troy Johnson, MD, Carthage Area Hospital, Carthage; Donna Grant, Jefferson County Public Health Svcs, Watertown; Robert J. Rudd, MS, Wadsworth Center Rabies Laboratory; Bryan Cherry, VMD, PhD, Alexandra Newman, DVM, Bur of Communicable Disease Control; Debra Blog, MD, Div of Epidemiology, New York State Dept of Health. Rodney Willoughby, MD, Medical College of Wisconsin. Charlene Fix, Fort Drum; Steven Baty, DVM, Michael Cooper, PhD, Kathryn Ellis, MD, US Army Public Health Command Region-Europe; Derron A. Alves, DVM, Veterinary Corps; Steven Cersovsky, MD, Institute of Public Health, US Army, US Dept of Defense. Charles E. Rupprecht, VMD, PhD, Div of High-Consequence Pathogens and Pathology, National Center for Emerging and Zoonotic Infectious Diseases; Angela M. Maxted, DVM, PhD, Emily W. Lankau, DVM, PhD, EIS officers, CDC. Corresponding contributor: Angela M. Maxted, amaxted@cdc.gov, 518-473-4436.
Editorial Note
This report is the first since 1974 of a U.S. service member dying from rabies after an overseas dog exposure (3). This case highlights the importance of rabies risk awareness for all travelers, including service members, and the need for prompt medical care, including PEP, for potential exposures. Although canine rabies virus transmission is considered eliminated in the continental United States (4), dog exposures remain a concern for all residents and travelers abroad in canine rabies–enzootic areas. During 1996–August 2011, a total of 10 of 45 reported U.S. human rabies cases were associated with canine variant viruses, and all resulted from dog exposures occurring overseas (5). Canine rabies variants acquired as the result of dog bites in Africa and Asia account for >95% of all human rabies deaths worldwide (6). Travel-associated rabies virus exposure rates have not been calculated with accuracy (6).
Clinical human rabies infections are nearly always fatal, even when treated using an experimental protocol (1). In this case, after-clinical-onset treatment efforts failed. Prompt PEP administration remains the only consistent method for preventing death after rabies virus exposure (2).
With the exception of transmission through transplantation, human-to-human rabies transmission has not been laboratory-documented but is possible theoretically (7) because rabies virus can be present in saliva, CSF, neural tissue, and tears. Infection control practices can decrease the risk for virus transmission to caregivers of patients with suspected or confirmed rabies. Once rabies is suspected, HCP should wear goggles, gowns, gloves, and face masks, particularly during activities with risk for saliva contact (e.g., intubation and suctioning) (2). Rapid institution of these precautions at hospital B demonstrated these measures' value for reducing exposures in the health-care setting: none of approximately 150 HCP who had patient contact required PEP. If rabies is confirmed, a standardized risk assessment of patient contacts should be conducted, with strict application of the exposure definitions detailed by ACIP (2). A rabies patient's autopsy can be conducted safely in facilities equipped to handle postmortem evaluations of infectious disease patients, using standard barrier precautions (i.e., an N95 or higher-grade respirator, full face shield, goggles, heavy gloves, and complete body coverage by protective wear) (8).
The patient's travel while potentially infectious added a unique public health concern. Local, state, federal, and international parties collaborated to ensure that all persons who potentially had contact with the patient's infectious secretions during his travel were reached for timely risk assessment. None required PEP.
Travelers should be informed of rabies risks when traveling to rabies-enzootic countries and should be encouraged to keep a safe distance from wild and feral animals. Travelers receiving bites or scratches from such animals should wash the wound thoroughly with soap and water and promptly seek medical attention. Persons who are at increased risk for exposure because of professional or tourist activities in enzootic areas or who might have limited access to medical resources should consult a physician about preexposure vaccination before departure and consider purchasing travel insurance that includes a provision for medical evacuation (6,9). Additional recommendations for travelers are available in the CDC Yellow Book: Health Information for International Travel 2012 (6) and at http://wwwnc.cdc.gov/travel. The case described in this report underscores the need for global partnerships for the prevention, control, and future elimination of canine rabies virus transmission (10).
Acknowledgments
Desirée Beaujean, PhD, Centre for Infectious Disease Control, National Institute for Public Health and the Environment, Netherlands. Dana Savici, MD, Birenda P. Sah, MD, Julius Gene S. Latorre, MD, Timothy P. Endy, MD, Upstate Univ Hospital, State Univ of New York; Cynthia Morrow, MD, Laura Knight, MD, Onondaga County Health Department, Syracuse; Jodie Jarvis, Michelle Dupuis, April Davis, DVM, PhD, Jill Taylor, PhD, Susan Wong, PhD, Wadsworth Center; Daniel Kuhles, MD, Bur of Communicable Disease Control, New York State Dept of Health. James H. Wright, DVM, Tom J. Sidwa, DVM, Texas Dept of Health. Rena Trumbull, Evelyn Barraza, MD, James Barker, Victorio Vaz, LVM, PhD, Europe Regional Medical Command; Jerry R. Cowart, DVM, Veterinary Pathology Div, Laboratory Science, US Army Public Health Command Region-Europe, US Army, US Dept of Defense. Elizabeth Bryan, Clare Dykewicz, MD, Gale Galland, DVM, Thomas George, MPH, Peter Houck, MD, Robynne Jungerman, MPH, Curi Kim, MD, Karen Marienau, MD, Nina Marano, DVM, Chris Schembri, MPH, Don Spatz, Julie Sinclair, DVM, Div of Global Migration and Quarantine; Clifton Drew, DVM, PhD, Sherif R. Zaki, MD, PhD, Christopher D. Paddock, MD, Jesse Blanton, MPH, Richard Franka, DVM, PhD, Xiaoyue Ma, MS, Lillian Orciari, MS, Sergio Recuenco, MD, PhD, Andres Velasco, PhD, Pamela Yager, James Ellison, Natalia Kuzmina, PhD, Div of High-Consequence Pathogens and Pathology, National Center for Emerging and Zoonotic Infectious Diseases; Julie Magri, MD, Scientific Education and Professional Development Program Office; Danielle Tack, DVM, EIS Officer, CDC.
References
- Medical College of Wisconsin. Care of rabies. Version 3.1. Milwaukee, WI: Medical College of Wisconsin; 2009. Available at http://www.mcw.edu/filelibrary/groups/pediatrics/infectiousdiseases/milwaukee_rabies_protocol_v3_1.pdf. Accessed April 25, 2012.
- CDC. Human rabies prevention—United States, 2008: recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR 2008;57(No. RR-3).
- Fester JM. Public health aspects of rabies. Aviat Space Enviro Med 1975;46:1194–5.
- Blanton JD, Hanlon CA, Rupprecht CE. Rabies surveillance in the United States during 2006. J Am Vet Med Assoc 2007;231:540–56.
- CDC. Human rabies. Atlanta, GA: US Department of Health and Human Services, CDC; 2012. Available at http://www.cdc.gov/rabies/location/usa/surveillance/human_rabies.html. Accessed April 25, 2012.
- CDC. CDC health information for international travel 2012. New York, NY: Oxford University Press; 2012.
- Fekadu M, Endeshaw T, Alemu W, Bogale Y, Teshager T, Olson JG. Possible human-to-human transmission of rabies in Ethiopia. Ethiop Med J 1996;34:123–7.
- CDC. Human rabies—Kentucky/Indiana, 2009. MMWR 2010;59:393–6.
- Blanton JD, Rupprecht CE. Travel vaccination for rabies. Expert Rev Vaccines 2008;7:613–20.
- Lembo T, Attlan M, Bourhy H, et al. Renewed global partnerships and redesigned roadmaps for rabies prevention and control. Vet Med Int 2011;2011:923149.
What is already known on this topic?
If not prevented by postexposure prophylaxis, rabies virus infection causes an acute progressive encephalitis that is nearly always fatal. Although considered eliminated from the United States, canine rabies is responsible for the majority of rabies deaths worldwide.
What is added by this report?
In August 2011, a recently returned U.S. Army soldier died of rabies after being bitten by a dog in Afghanistan; he did not receive correct postexposure prophylaxis. This is the first rabies death among U.S. service members since 1974.
What are the implications for public health practice?
This case demonstrates the need to avoid animal contact while in rabies-enzootic regions and to seek prompt medical evaluation after any animal bite. Early clinical suspicion of rabies and infection control measures can help reduce the need for postexposure prophylaxis among health-care personnel. Prompt suspicion and confirmation of rabies can inform experimental treatment decisions. Canine rabies is and will remain a risk to residents and visitors of many countries around the globe until it is eliminated through vaccination of animals.
FIGURE. Timeline of events surrounding an imported case of human rabies in a U.S. Army soldier — Afghanistan, Germany, and New York, 2011
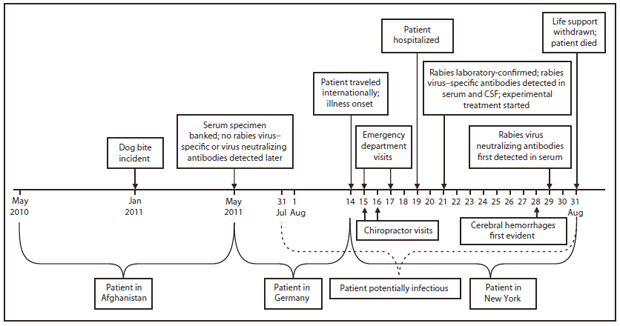
Alternate Text: The figure above shows the timeline of events surrounding an imported case of human rabies in a U.S. Army soldier from the locations of Afghanistan, Germany, and New York during 2011.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All MMWR HTML versions of articles are electronic conversions from typeset documents.
This conversion might result in character translation or format errors in the HTML version.
Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr)
and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S.
Government Printing Office (GPO), Washington, DC 20402-9371;
telephone: (202) 512-1800. Contact GPO for current prices.
**Questions or messages regarding errors in formatting should be addressed to
mmwrq@cdc.gov.


