FIGURE 2. Percentage of children sleeping under an insecticide-treated net in countries with more than one survey, 1999--2009
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail.
Grand Rounds: The Opportunity for and Challenges to Malaria Eradication
This is another in a series of occasional MMWR reports titled CDC Grand Rounds. These reports are based on grand rounds presentations at CDC on high-profile issues in public health science, practice, and policy. Information about CDC Grand Rounds is available at http://www.cdc.gov/about/grand-rounds.
The Problem
In 2009, malaria, a disease transmitted by the bite of an infective Anopheles mosquito, caused an estimated 225 million clinical cases and 781,000 deaths worldwide, of which more than 90% occurred in children aged <5 years in Africa (1). Approximately half of the world's population, or 3 billion persons, are at risk for acquiring the illness. Malaria is transmitted most intensely in central and western Africa, where in some areas >40% of children aged <10 years are infected and residents can be bitten by more than one infective mosquito every day of the year (2).
Malaria in humans is caused mainly by four species of the intra-erythrocytic parasite Plasmodium, of which Plasmodium falciparum and P. vivax account for most morbidity worldwide. P. falciparum malaria is the most dangerous and can be fatal in 15%−20% of cases, even when appropriately treated. Death results from severe anemia, seizures and coma, acute respiratory distress syndrome, and other organ failures. P. falciparum also is the species in which resistance to multiple antimalarials has appeared over the past 50 years. The burden of P. falciparum includes placental infection that increases the risk for low birth weight and subsequent infant mortality or disability. In countries with a high incidence of malaria, economic growth during 1965--1990 was lower by 1.3% per year, compared with countries without high malaria incidence, even after adjusting for other factors (3).
Efforts to combat malaria encompass a continuum from control (reduction of malaria morbidity and mortality) to elimination (cessation of transmission in a defined geographic area) and eradication (global reduction of malaria incidence to zero). The global malaria eradication campaign of the mid-20th century eliminated malaria in 37 of 143 countries where malaria was endemic in 1950, and many other countries substantially decreased malaria incidence and deaths. However, the campaign did not eradicate malaria. Technical setbacks, implementation difficulties, and a paucity of research to find solutions limited success. In 1969, the 22nd World Health Assembly acknowledged the failure of the global eradication campaign, suspended it indefinitely, and consequently placed new emphasis on improving malaria control to minimize the burden of disease. In the late 1980s and early 1990s, efforts to control malaria were hampered as a result of decreased funding and support and the spread of parasites resistant to antimalarial drugs.
Today, malaria control in areas with high incidence is based on strategic implementation and scale-up of proven, cost-effective interventions. The aim is first to rapidly reduce malaria morbidity and mortality, particularly among high-risk groups such as children and pregnant women, followed by progressive reduction of transmission and elimination from malaria-endemic areas (Figure 1). Global eradication remains the ultimate long-term goal, although it is now approached with perhaps a greater appreciation of its challenges.
Currently Recommended Interventions for Malaria Control
Four proven interventions currently are being scaled up across sub-Saharan Africa: 1) long-lasting insecticide-treated mosquito nets (ITNs), 2) indoor residual spraying (IRS), 3) diagnosis and treatment of infected persons with artemisinin-based combination therapy (ACT), and 4) protection of women with intermittent preventive treatment during pregnancy (IPTp).
ITNs, evaluated through field trials, have demonstrated a protective efficacy of 17% against all-cause childhood mortality in sub-Saharan Africa and could save up to 5.5 lives each year for every 1,000 children protected (4). Follow-up field trial data show that the child survival benefit from ITNs can last for up to 6 years (5). Additionally, expanding the availability of nets from target groups (pregnant women and children aged <5 years) to cover at least 65% of older children and adults provides some protection even for those without nets (e.g., by reducing mosquito survival and decreasing community parasitemia) (6). These findings, and the availability of funding, led to a policy aimed at achieving universal coverage rather than a focus on vulnerable groups (7).
IRS is the application of insecticide to the interior walls of houses. Ideally, the insecticide will repel mosquitoes from entering houses and kill them when they rest on treated walls, thus reducing transmission from mosquitoes that bite and rest indoors. Field studies and program experience since the 1950s have demonstrated the effectiveness of IRS in reducing malaria in both stable and unstable (epidemic-prone) malaria transmission settings (8). Like ITNs, IRS is most effective when applied communitywide with high coverage rates. IRS and ITN effectiveness is threatened by the emergence of insecticide resistance (9). Novel applications of IRS using rotational (alternating insecticides over time) or mosaic (multiple insecticides in different areas) strategies might preserve the effectiveness of this intervention.
Diagnosis and management of patients with malaria is a cornerstone of malaria control because this can cure clinical disease and blunt transmission. During a period of poor malaria control in the 1990s, P. falciparum infection accounted for an estimated 30% of childhood deaths in sub-Saharan Africa (10); a large proportion of these malaria-related deaths could be attributed to the high prevalence of parasites resistant to chloroquine, the first-line treatment during this period. In the last decade, a potent new class of drug made from derivatives of artemisinin has been introduced. To forestall the development of resistance to artemisinin derivatives, the World Health Organization (WHO) recommends that the derivatives not be used alone, but rather as artemisinin-based combination therapy (ACT) (using an artemisinin in combination with another antimalarial with a different mode of action); ACT regimens have been adopted as first-line treatment globally (11). Rapid and accurate diagnosis enhances malaria case management by directing ACTs to patients with a confirmed diagnosis of malaria. Recently, malaria rapid diagnostic tests based on lateral-flow immunochromatography have been introduced. They can detect malaria parasite antigens from finger-prick blood specimens in 10--15 minutes, and their availability has begun to increase the ability of health-care workers to diagnose cases, especially in rural areas without laboratory capacity.
In sub-Saharan Africa, an estimated 28% of women are infected with P. falciparum during pregnancy. Because of pregnancy-altered changes in immunity, women living in moderate- to high-transmission areas who are pregnant for the first or second time are at greater risk for adverse events from malaria than women who have had three or more pregnancies (12). In these transmission contexts, IPTp, the preventive treatment of all pregnant women with curative regimens of sulfadoxine pyrimethamine (SP) during the second and third trimesters, can decrease both placental malaria parasitemia and maternal anemia (13). In many areas where SP is used for IPTp, a high prevalence of parasites with SP resistance genes and concomitant failures of SP monotherapy for clinical malaria treatment in children have been observed. Whether SP resistance might alter the effectiveness of SP for IPTp is unclear and underscores the need to continue monitoring its efficacy in curing P. falciparum infection in pregnant women and the need for support for research into new medications for IPTp.
Progress and Strategies Toward Malaria Eradication
Developments at the turn of the millennium gave rise to renewed optimism for malaria control. Global partnerships to coordinate work were established, notably the Roll Back Malaria (RBM) partnership (information available at http://www.rollbackmalaria.org). Unprecedented funding for program scale-up became available through donor mechanisms such as the Global Fund to Fight AIDS, Tuberculosis, and Malaria; the World Bank; and the U.S. President's Malaria Initiative. Leaders in malaria-endemic countries committed to malaria control as a national priority through assent to RBM's Abuja Declaration and adoption of UN Millennium Development Goals.
In many countries, more money, applied science, and enhanced global partnerships are beginning to result in decreased malaria. Coverage of key interventions, such as ITNs, is increasing, although most countries have yet to achieve their targets; recent household surveys from African countries such as Rwanda and the Gambia show that approximately 50% or more of children aged <5 years sleep under ITNs. However, coverage is low for other countries, including Nigeria and Democratic Republic of the Congo (Figure 2). Reductions in malaria resulting from scale-up of control efforts have been best seen, so far, in certain areas, such as the islands of Zanzibar, where the National Malaria Control Program accelerated its scale-up efforts beginning in 2003. ACTs were provided free of charge in public health facilities in late 2003, ownership of ITNs reached 72% by 2007, and four rounds of IRS were conducted during 2006−2008. These efforts, combined with improved diagnostic practices, resulted in 70% fewer malaria inpatient cases and deaths in a combined sample of six of the seven hospitals on the islands of Zanzibar during 2006−2008, compared with 2001--2002 (Figure 3) (14). In other countries, the effect of malaria control efforts on a national scale are only beginning to be seen; for example, in seven countries (Ghana, Kenya, Madagascar, Rwanda, Senegal, Tanzania, and Zambia), reductions in all-cause mortality in children aged <5 years ranged from 19%--36% in paired nationwide household surveys following the scale-up of malaria control (15). While a variety of factors might be influencing the decline in mortality rates of children, strong and growing evidence indicates that malaria prevention and treatment efforts have played a major role (16). Thorough impact assessments are under way in several countries to examine this relationship.
Although current malaria control efforts are showing promising results in some countries, many others have yet to achieve targets (14). One reason is the relatively short period that increased resources have been available. Also, even though the funds put toward malaria control have increased substantially since 2003, the total resources available globally to scale-up malaria control interventions fall far short of what is needed. To ensure the maximal effect from implemented interventions, barriers to scale-up should be identified and eliminated, and these efforts should cover all aspects of current interventions, from determining optimal approaches to ITN distribution and IRS implementation to diagnostic and treatment protocols for case management and IPTp policies.
Even when targets for scale-up of recommended interventions are achieved, most experts agree that because of the very high transmission rate in sub-Saharan Africa, additional investments in research and development of new control and elimination tools will be required before malaria can be eradicated. Recently published research recommendations emphasize that the long-term vision for malaria interventions should include new antimalarial medications, evaluation of treatment strategies such as mass drug administration, and novel vector-control approaches (17). In regions with less malaria endemicity, elimination might rest on novel molecular assays capable of detecting low numbers of parasites among persons in remote, rural areas; novel diagnostic technology such as real-time fluorescence loop-mediated amplification might make parasite detection possible in the absence of reference laboratory personnel and equipment (18).
The availability of vaccines has been critical in targeting diseases for global eradication. Unfortunately, a highly effective vaccine for malaria control has not been found, although several promising candidates are in development. Currently the first Phase III, individually randomized, clinical trial of a malaria vaccine is being conducted, advancing earlier work that demonstrated that the candidate vaccine was associated with a 35% reduction in clinical illness from malaria and a 49% reduction of severe malaria in children for up to 6 months (19).
Conclusion
Malaria is an enormous global disease burden, and its eradication is an ambitious goal. Although the tools for malaria control are much improved, to ensure continued progress, national programs, local communities, global health partners, and donors will have to build on initial successes, maintain a prolonged commitment, and invest in strategies for the future. This will require leadership, perseverance, flexibility, and financial support. Research into new medications, insecticides, and vaccines will be required to achieve the eventual goal of eradication. Organizations working toward malaria eradication should be pleased with the progress so far, cautioned by the challenges ahead, and heartened with confidence that the implementing foundation is solid and science is guiding the way.
Reported by
KE Mace, PhD,* MF Lynch, MD, JR MacArthur, MD, SP Kachur, MD, L Slutsker, MD, Div of Parasitic Diseases and Malaria, Center for Global Health, CDC. RW Steketee, MD, Malaria Control and Evaluation Partnership in Africa, PATH, Seattle, Washington. T Popovic, MD, PhD, Office of the Director, CDC. *Corresponding contributor: Kimberly E. Mace, Div of Parasitic Diseases and Malaria, Center for Global Health, CDC, 770-488-7118, kmace@cdc.gov.
References
- World Health Organization. World malaria report 2010. Geneva, Switzerland: World Health Organization; 2010. Available at http://www.who.int/malaria/world_malaria_report_2010/en/index.html. Accessed April 18, 2011.
- Hay SI, Guerra CA, Gething PW, et al. A world malaria map: Plasmodium falciparum endemicity in 2007. PLoS Med 2009;6(3):e1000048.
- Gallup JL, Sachs JD. The economic burden of malaria. Am J Trop Med Hyg 2001;64(1--2 Suppl):85--96.
- Lengeler C. Insecticide-treated bed nets and curtains for preventing malaria. Cochrane Database Syst Rev 2004;(2):CD000363.
- Lindblade KA, Eisele TP, Gimnig JE, et al. Sustainability of reductions in malaria transmission and infant mortality in western Kenya with use of insecticide-treated bednets: 4 to 6 years of follow-up. JAMA 2004;291:2571--80.
- Killeen GF, Smith TA, Ferguson HM, et al. Preventing childhood malaria in Africa by protecting adults from mosquitoes with insecticide-treated nets. PLoS Med 2007;4:e229.
- World Health Organization. Insecticide-treated mosquito nets: a WHO position statement. Geneva, Switzerland: World Health Organization, Global Malaria Programme; 2007. Available at http://www.who.int/entity/malaria/publications/atoz/itnspospaperfinal.pdf. Accessed April 18, 2011.
- Pluess B, Tanser FC, Lengeler C, Sharp BL. Indoor residual spraying for preventing malaria. Cochrane Database Syst Rev 2010;(4):CD006657.
- Ranson H, N'Guessan R, Lines J, Moiroux N, Nkuni Z, Corbel V. Pyrethroid resistance in African anopheline mosquitoes: what are the implications for malaria control? Trends Parasitol 2011;27:91--8.
- Snow RW, Trape JF, Marsh K. The past, present and future of childhood malaria mortality in Africa. Trends Parasitol 2001;17:593--7.
- World Health Organization. Guidelines for the treatment of malaria. 2nd ed. Geneva, Switzerland: World Health Organization; 2010. Available at http://www.who.int/malaria/publications/atoz/9789241547925/en/index.html. Accessed April 18, 2011.
- Steketee RW, Breman JG, Paluku KM, Moore M, Roy J, Ma-Disu M. Malaria infection in pregnant women in Zaire: the effects and the potential for intervention. Ann Trop Med Parasitol 1988;82:113--20.
- ter Kuile FO, van Eijk AM, Filler SJ. Effect of sulfadoxine-pyrimethamine resistance on the efficacy of intermittent preventive therapy for malaria control during pregnancy: a systematic review. JAMA 2007;297:2603--16.
- World Health Organization. World malaria report 2009. Geneva, Switzerland: World Health Organization; 2009. Available at http://www.who.int/malaria/world_malaria_report_2009/en/index.html. Accessed April 18, 2011.
- United States Agency for International Development. President's Malaria Initiative. Sustaining momentum against malaria: saving lives in Africa. Fourth annual report. Washington, DC: US Agency for International Development; 2010. Available at http://www.fightingmalaria.gov/resources/reports/index.html. Accessed April 18, 2011.
- Steketee RW, Campbell CC. Impact of national malaria control scale-up programmes in Africa: magnitude and attribution of effects. Malar J 2010;9:299.
- Alonso PL, Brown G, Arevalo-Herrera M, et al. A research agenda to underpin malaria eradication. PLoS Med 2011;8:e1000406.
- Lucchi NW, Demas A, Narayanan J, et al. Real-time fluorescence loop mediated isothermal amplification for the diagnosis of malaria. PLoS One 2010;5:e13733.
- Alonso PL, Sacarlal J, Aponte JJ, et al. Efficacy of the RTS,S/AS02A vaccine against Plasmodium falciparum infection and disease in young African children: randomised controlled trial. Lancet 2004;364:1411--20.
FIGURE 1. Malaria-free countries and malaria-endemic countries in phases of control,* preelimination, elimination, and prevention of reintroduction --- worldwide, 2008
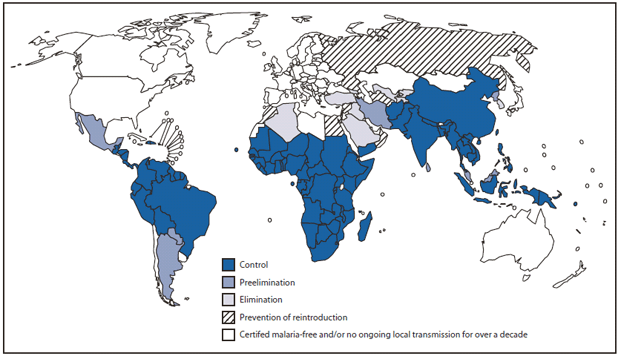
Source: World Health Organization. World malaria report 2009. Available at http://www.who.int/malaria/world_malaria_report_2009/en/index.html.
* China, Philippines, Solomon Islands, Sudan, Vanuatu, and Yemen have localized malaria-free projects.
Alternate Text: The figure above is a world map showing malaria-free countries and malaria-endemic countries in different phases of malaria control, preelimination, elimination, and prevention of reintroduction in 2008.
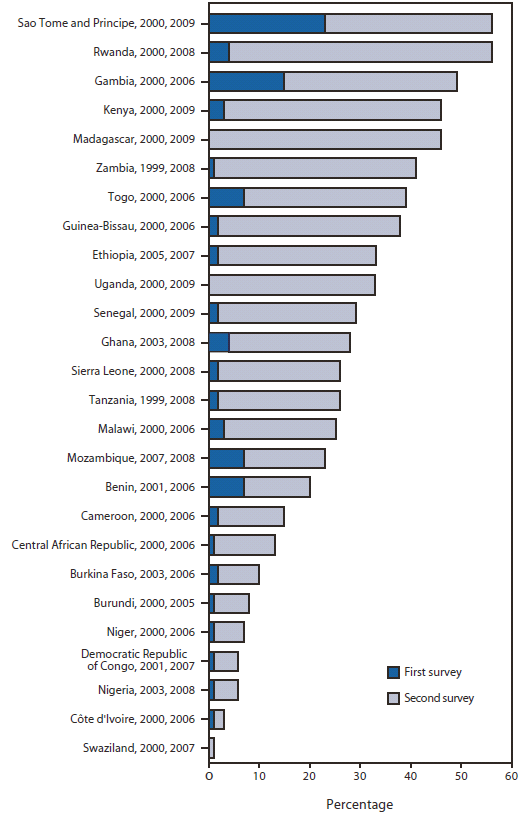
Source: World Health Organization. World malaria report 2010. Available at http://www.who.int/malaria/world_malaria_report_2010/en/index.html
Alternate Text: The figure above shows the percentage of children sleeping under an insecticide-treated net in countries with more than one survey, during 1999-2009. The figure shows that coverage was highest in Sao Tome and Principe and lowest in Swaziland.
FIGURE 3. Number of malaria inpatient cases and deaths --- six hospitals, Zanzibar, Tanzania, 1999--2008
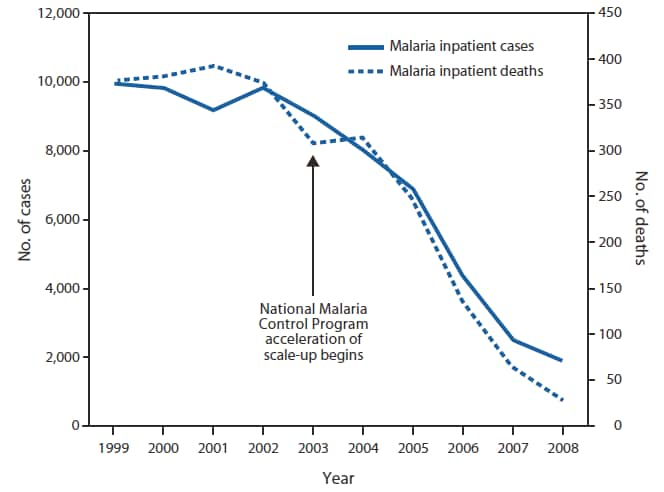
Sources: Ministry of Health routine surveillance data.
World Health Organization. World malaria report 2009. Available at http://www.who.int/malaria/world_malaria_report_2009/en/index.html.
Alternate Text: The figure above shows the number of malaria inpatient cases and deaths at six hospitals in Zanzibar, Tanzania, during 1999-2008. Eradication efforts combined with improved diagnostic practices resulted in 70% fewer malaria inpatient cases and deaths during 2006−2008, compared with 2001-2002.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All MMWR HTML versions of articles are electronic conversions from typeset documents.
This conversion might result in character translation or format errors in the HTML version.
Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr)
and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S.
Government Printing Office (GPO), Washington, DC 20402-9371;
telephone: (202) 512-1800. Contact GPO for current prices.
**Questions or messages regarding errors in formatting should be addressed to
mmwrq@cdc.gov.


