Meet People Where They Are
CDC’s National Preparedness Month campaign materials are available to assist partners in communicating about the importance of emergency preparedness and response.
This CDC Digital Media Toolkit includes sample social media and graphics. This material is downloadable and shareable. Some of the material is customizable.
The theme of this year’s toolkit is #MeetPeopleWhereTheyAre in their capabilities to prepare and respond to emergencies. Specifically, this toolkit includes messaging that
- looks at ways social determinants of health can impact personal health preparedness and response.
- suggests ways the whole community can create opportunities and conditions for everyone to prepare for and respond to emergencies to their full potential.
This emphasis builds on previous #PrepYourHealth social media content to bring additional focus to the needs of all populations affected by disasters.
What Does It Mean to Meet People Where They Are?
In the context of emergency preparedness and response, “meeting people where they are” means creating opportunities for everyone to prepare and respond to emergencies to their full potential.
It also means acknowledging that preparedness recommendations and protective actions, such as evacuation, have limitations. They may not account for conditions in which people are born, grow, work, live, and age or how those conditions can affect a person’s opportunities to prepare and respond to their full potential.
For example, the recommendation to “set aside enough food, water, supplies, and personal needs to last at least 72 hours” may not consider the effect of poverty on a person’s access to food beyond daily use. Poverty is an example of a social determinant of health.
Protective actions are research-based actions and advice that anyone can take to prepare for, keep safe during, and recover from a disaster.
The three most common and recognizable protective actions are evacuate, shelter in place, and secure in place.
Source: https://bit.ly/3sI4tvB
What are Social Determinants of Health?
Social determinants of health (SDOH) are non-medical factors that influence health outcomes. They are the conditions in which people are born, grow, work, live, and age, and the wider set of forces and systems shaping the conditions of daily life. They include transportation, discrimination, income, polluted air and water, poverty, and language and literacy skills.
SDOH contribute to health disparities and inequities in living, working, health, and social conditions. Inequities can limit access to resources, supplies, and services. Limitations such as these can make it difficult or impossible for some people to prepare for and respond to emergencies.
This toolkit highlights resources and promising practices that the whole community (i.e., individuals, businesses, community organizations, schools, nonprofit groups, and all levels of government) is taking to make preparedness possible for everybody.
Disparities are not personal failings. They are the preventable differences in
- the burden of disease, injury, impacts of emergencies, etc. and
- opportunities to prepare and respond to emergencies.
Recommendations to make healthy choices, such as prepare for emergencies, won’t eliminate disparities. Public health organizations and others in the whole community can take action to address SDOH.
The examples in this toolkit of the effects of SDOH on emergency preparedness and response are not exhaustive. Neither they nor the examples of interventions undertaken by the whole community address all dimensions of the issue. Examples and evidence of SDOH impacts and interventions are likely to evolve with additional research and experience.
The content of this toolkit is organized into Healthy People 2030’s five SDOH domains:
Economic Stability
This key area includes topics such as poverty, employment, food security, and housing stability.
People’s access to steady employment and reliable income can affect their opportunities to prepare for and respond to emergencies:
- Many people, including those living in poverty, may not have the means to evacuate before an emergency, such as a hurricane.
- Families that spend more than 30% of their income on housing may not have enough money to buy earthquake or flood insurance.
- People with lower or fixed incomes may find it difficult to build an emergency fund.
- People experiencing homelessness may find it difficult to stay healthy during emergencies.
Learn more about the impacts of economic stability on risks and outcomes.
Education access and quality
This key area includes topics such as graduating from high school, enrolling in higher education, and understanding language and literacy.
People’s access to quality educational opportunities and resources can affect their opportunities to prepare for and respond to emergencies.
- People with limited English proficiency may not receive, understand, and take protective actions.
- People who aren’t taught media and online-search literacy skills can have difficulty identifying reputable sources of information.
- People who live in rural and lower-income communities may have fewer opportunities to get involved in organizations and activities that build resilience.
Learn more about the impacts of education access and quality on risks and outcomes.
Health care access and quality
This key area includes topics such as access to health care, access to primary care, health insurance coverage, and health literacy.
People’s access to health care and understanding of their own health can affect their opportunities to prepare for and respond to emergencies.
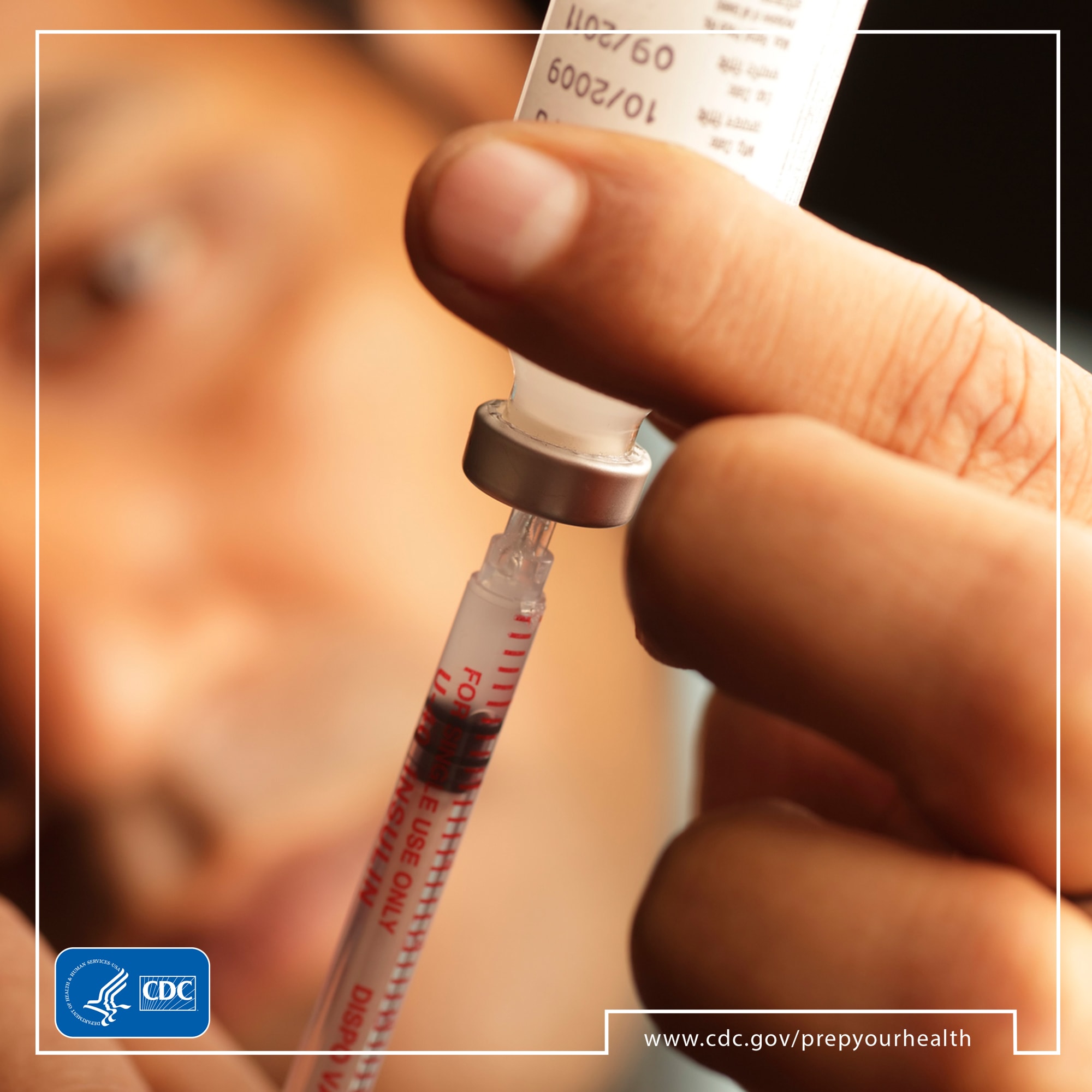
- People who don’t have a primary care provider may find it difficult to create an emergency supply of prescription medicines.
- People who don’t have health insurance may find it difficult to stay up to date on vaccines.
- People with low health literacy may find it difficult to understand and use health information to make good emergency preparedness decisions.
Learn more about the impacts of health care access and quality on risks and outcomes.
Personal health literacy is the degree to which individuals have the ability to find, understand, and use information and services to inform health-related decisions and actions for themselves and others.
Organizational health literacy is the degree to which organizations equitably enable individuals to find, understand, and use information and services to inform health-related decisions and actions for themselves and others.
Source: https://bit.ly/3wElyrv
Neighborhood and built environment
This key area includes topics such as quality of housing, access to transportation, availability of healthy foods, air and water quality, and access to high-speed internet.
The physical environment people live in (e.g., the air they breathe, water they drink, houses and neighborhoods they live in, and transportation they take to work) can affect their opportunities to prepare for and respond to emergencies.
- People who do not have a reliable personal vehicle or access to public transportation may find it difficult to evacuate.
- People who live in low-income, minority, and rural communities may have limited access to emergency medical (or ambulatory) transportation.
- People who live in low-income, minority, and rural communities may be at greater risk for health impacts from power outages and planned blackouts.
Learn more about the impacts of neighborhood and built environment on risks and outcomes.
Social and community context
This area includes key issues such as cohesion within a community, civic participation, discrimination, conditions in the workplace, and incarceration.
People’s interactions with and connectedness to family, friends, co-workers, and community members can affect their health, well-being, and opportunities to prepare for emergencies.
- People experiencing social isolation may find it difficult to build a personal support network.
- People who have experienced discrimination or racism are less likely to follow the instructions of government officials.
- People who have fewer opportunities for civic participation in emergency response organizations, such as Community Emergency Response Team, may find it difficult to build resilience to emergencies.
Learn more about the impacts of social and community context on risks and outcomes.