Sickle Cell Disease Clinical Guidelines
Managing Sickle Cell Disease in the Emergency Department
The American College of Emergency Physicians recruited field experts and thought leaders to develop a point-of-care tool for SCD. Providers can deploy the evidence-based, clinical content to deliver quality care to patients with SCD in the emergency department.
Understanding the Complications of Sickle Cell Disease
From the American Journal of Nursing, 2019.
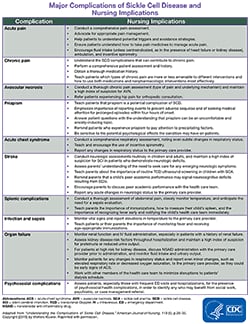
This publications provides an overview of major sickle cell disease (SCD)-related health complications, as well as the nursing implications for each. CNE credits are available for reading the article. Read the full article.
Available as a free resource, download and print a reference table

ASH Clinical Practice Guidelines on Sickle Cell Disease
In 2016, the American Society of Hematology (ASH) initiated an effort to develop clinical practice guidelines on Sickle Cell Disease (SCD). ASH formed a committee of medical experts, researchers and patients to review evidence and form recommendations on SCD. The recommendations address treatment of both adult and pediatric SCD.
Available Guidelines
- Cardiopulmonary and Kidney Disease
- Transfusion Support
- Cerebrovascular Disease
- Management of Acute and Chronic Pain
- Stem Cell Transplantation
Health Supervision for Children with Sickle Cell Disease
From the American Academy of Pediatrics (AAP), 2011
This statement provides pediatricians in primary care and subspecialty practice with an overview of the genetics, diagnosis, clinical manifestations, and treatment of SCD. Specialized comprehensive medical care decreases morbidity and mortality during childhood. The provision of comprehensive care is a time-intensive endeavor that includes ongoing patient and family education, periodic comprehensive evaluations and other disease-specific health maintenance services, psychosocial care, and genetic counseling. Timely and appropriate treatment of acute illness is critical, because life-threatening complications develop rapidly. It is essential that every child with SCD receive comprehensive care that is coordinated through a medical home with appropriate expertise.
The Management of Sickle Cell Disease
From the National Heart Lung and Blood Institute (NHLBI), 2014
The practice guidelines best supported by scientific evidence are:
- Penicillin prophylaxis prevents pneumococcal sepsis in children
- Pneumococcal vaccine prevents pneumococcal infection in children
- In surgical settings, simple transfusions to increase hemoglobin (Hb) levels to 10 g/dL are as good as or safer than aggressive transfusions to reduce sickle hemoglobin (Hb S) levels to below 30 percent
- Transfusions to maintain a hematocrit of more than 36 percent do not reduce complications of pregnancy
- Transfusions to reduce Hb S levels to below 30 percent prevent strokes in children with high central nervous system blood flow
- Hydroxyurea decreases crises in patients with severe sickle cell disease
Read more about these practice guidelines »
Problem Oriented Clinical Guidelines
From the Sickle Cell Information Center, 1991
These protocols are guidelines in use at the Sickle Cell Center at Grady Health System, and they are intended for use by heath care providers treating patients with sickle cell syndromes. These guidelines supplement to current texts in general medicine, surgery and pediatrics.
These guidelines address more than 40 specific issues, such as abdominal pain, congestive heart failure, and infections.