EHDI Guidance Manual – Chapter 1: The EHDI Information System: Overview and Key Considerations
Chapters
- ›Chapter 1: The EHDI Information System: Overview and Key Considerations
- Chapter 2: The EHDI Information System: Data Collection and Reporting
- Chapter 3: Updating and Using Your EHDI-IS for Tracking, Surveillance and Program Improvement
- Chapter 4: EHDI Information System: Data Use and Dissemination
- Chapter 5: Privacy, Confidentiality and Security of the EHDI-IS
- Chapter 6: Monitoring and Evaluation
Chapter Objectives:
This chapter will help you to
- Understand the purpose of having a complete EHDI Information System (EHDI-IS);
- Define what a basic and complete EHDI-IS looks like with regard to its data and functional requirements;
- Understand the importance of the link between planning and evaluation;
- Think about the role of program stakeholders; and
- Consider the critical elements important to your system’s sustainability.
What constitutes a basic EHDI-IS?
The EHDI-IS is an important tool that supports EHDI programs in their work to ensure that all deaf and hard of hearing (D/HH) infants and young children are identified early and receive intervention services. These systems can also provide a variety of relevant data reports that aid in surveillance and program performance assessments. Given those advantages, every state and territory could benefit by having at least a basic EHDI-IS in place.
A basic EHDI-IS is described by the following characteristics:
- It is purchased from a vendor or developed by the jurisdiction.
- Data may be entered online by users, sent electronically in batch files and then uploaded by a program, and/or submitted on paper and then entered manually.
- The system allows access to EHDI information by state EHDI program staff, providing no or limited ability to obtain and provide other relevant information, such as patient demographics, and no access to EHDI information by other stakeholders, such as primary care providers.
- The system gathers individual level information about infants and young children who do not pass the hearing screening, but may not include individual level information about infants and young children who do pass the hearing screening.
- The system gathers individual level information about infants/young children who receive audiology diagnostic follow-up services, but may offer only limited or no information about referral and enrollment into early intervention.
- The system has a limited ability to generate reports and support data analysis activities.
- The system does not enable programs to review and analyze data using different data definitions or criteria.
What constitutes a complete EHDI-IS?
The attributes of a “complete” EHDI-IS have been enumerated in CDC’s Functional Standards.
A complete EHDI-IS exceeds the capabilities of a basic system by
- Meeting all functional criteria as defined by the SHALL statements in the EHDI-IS Functional Standards;
- Collecting and storing all minimum data items as specified in the EHDI-IS Functional Standards; and
- Providing the functional ability to obtain and report on all minimum and core data items as specified in the EHDI-IS Functional Standards.
Functional Standards
What are the Functional Standards of a complete EHDI-IS?
A set of Functional Standards and programmatic goals for a complete EHDI-IS was developed by the EHDI-IS Functional Standard Working Group (FSWG), which consisted of members of the CDC EHDI team and program managers/data system experts from nine jurisdictions. These standards were based on three general considerations:
- These Functional Standards are intended to identify the operational, programmatic, and technical criteria that all jurisdictional EHDI programs can implement during the processes of developing, using, and evaluating the EHDI-IS.
- The Functional Standards are NOT intended to provide specifications on how those functions are to be implemented.
- However, in some cases, current laws or policies may preempt the implementation of some or all of the Functional Standards (e.g., a law does not allow for a certain data item to be collected).
What are the goals of a complete EHDI-IS?
The goals of the CDC EHDI-IS Functional Standards are as follows:
- Document unduplicated, individually identifiable data on the delivery of newborn hearing screening services for all infants and young children born in the jurisdiction.
- Support tracking and documentation of the delivery of follow-up services for every infant/child who did not receive, complete, or pass newborn hearing screening.
- Document all cases of hearing loss, including congenital, late-onset, progressive, and acquired cases for infants/children < 3 years old.
- Document the enrollment status, delivery, and outcome of early intervention services for infants and young children < 3 years old with hearing loss.
- Maintain data quality (accurate, complete, timely data) of individual newborn hearing screening, follow-up screening and diagnosis, early intervention, and demographic information in the EHDI-IS.
- Preserve the integrity, security, availability and privacy of all personally-identifiable health and demographic data in the EHDI-IS.
- Enable evaluation and data analysis activities.
- Support dissemination of EHDI information to authorized stakeholders.
What are the system functional requirements to achieve each of the above goals?
For each goal listed above, the CDC EHDI-IS Functional Standards define a set of functional requirements and their conformance criteria for the collection, management, and use of EHDI data. These Standards articulate the functional requirements needed to support EHDI tracking and surveillance in jurisdictional public health programs.
Collection of Individual Level and Aggregate Data
By routinely capturing comprehensive data, your EHDI-IS can quickly provide accurate and precise information at both the individual and population levels. This allows programs to ensure that infants and young children are receiving services, as well as to assess progress and answer questions from leadership and other stakeholders.
Why Collect Individual Level Data?
Individual level data provide the ability to ensure that all infants and young children are screened and receive recommended follow-up diagnostic testing and early intervention services. This level of detail is frequently not possible using aggregate information.
Individual level data also provide the ability to understand and answer critical epidemiological questions in EHDI that cannot be answered using aggregated level data (e.g., average age of diagnosis and factors related to not receiving services). For example, individual level data about the receipt of diagnostic testing can be used to document the infants and young children who were identified early as D/HH. When analyzed with demographic data, it is possible to determine if a certain factor (e.g., maternal education or age) is associated with infants and young children becoming lost to follow-up. Individual level data can also be combined with data from other public health databases, such as birth defects registries or education records, which makes it possible to conduct additional analyses to assess the delivery of services and outcomes among D/HH children.
The collection of individual-level data facilitates
- An evaluation based on health outcomes;
- A rapid and more precise monitoring of coverage, which can help with operational planning and local intervention;
- Scientifically rigorous studies of the effectiveness of the EHDI program;
- Tracking and notification upon loss to follow-up;
- Appropriate scheduling of outpatient visits;
- The potential to assess outcomes in D/HH infants and young children identified early through an EHDI program; and
- Transmission of reminders to patients when a follow-up visit is required.
This last action is particularly important because the effectiveness of an EHDI program is reduced when those who do not pass the initial screening do not receive necessary diagnostic and/or intervention services in a timely manner.
Why Collect Aggregate Data?
Aggregate data are used for the generation of routine reports and indicators, and allow estimates of coverage for large areas (e.g., state, city). Most importantly, these data are crucial for program planning and guidance, as aggregate data can allow multiple comparisons (e.g., percent screened in each birthing facility in a state). The downside to aggregate data is its inflexibility to examine relationships among variables, answer specific questions, identify data quality issues, and to re-aggregate data if reporting needs change.
Growing Your EHDI-IS
How do I develop a project plan to enhance and maintain the EHDI-IS?
Planning is critical to the successful development, implementation and maintenance of an EHDI-IS that is flexible enough to adapt to a changing environment. Project planning is an ongoing process in a dynamic system. It generally begins with reviewing the program context and existing stage of EHDI-IS development, determining clear goals and measures of success, and developing an evaluation plan. Planning and evaluation are interrelated ─a thorough evaluation begins with proper planning. While this section describes important considerations for program staff during the planning process, it is not intended to be an exhaustive technical guide to developing a new EHDI-IS.
Program Context
Program context refers to the environment in which your program exists. Because external factors can influence your EHDI-IS, you should be aware of and understand them. These include rules and regulations, current and available funding, stakeholders, interagency support, social and environmental conditions, and history of leadership (of the program, agency, and past collaborations).
What are my jurisdiction’s rules and regulations with regard to the collection, use and/or dissemination of EHDI related data?
In this process, it is important to identify and review all applicable laws and regulations in your jurisdiction. The relevant federal rules and regulations are outlined in Chapter 3. The NCHAM eBook also provides an overview of state legislation and specific guides to legislation by state, which can be found here. [1]
Example: It is decided that it may be more economical for some hospitals to outsource newborn hearing screening service to a privately owned company. This economic decision will affect your tracking and surveillance plan. Does the legislation requiring all hospital-based providers to report a screening result to the EHDI program apply to a privately owned company? If no, how should you modify your surveillance and tracking plan?
Stakeholders and Interagency Support
Stakeholders and interagency support are essential components for the successful implementation of the EHDI-IS. Persons and organizations that have an interest and/or involvement with EHDI programs are classified as stakeholders; consider involving them in the planning, implementation, and evaluation of the EHDI-IS. These are also the key groups of people to target for dissemination of surveillance and evaluation findings. By sharing this information, such as the number of D/HH infants and young children identified early, the program can help stakeholders better understand the actual impact that the EHDI program is making in the community.
Building Your Sustainable EHDI Program
Program sustainability is the ability to maintain program services and the system’s functions over time.[2] Maintaining the services and capacity of a complete EHDI-IS will help ensure that all D/HH infants and young children are consistently identified early. This requires a strategic approach to planning, collaborating, and sharing.[3]
Building a sustainable EHDI program and EHDI-IS will require multiple strategies and extensive collaboration. When developing information systems, people often focus only on the costs related to initial development and implementation, without considering the funding needs to sustain the system over time. As political and financial environments change, it is critical to plan for sustainability to ensure that programs and services continue and thrive over time.
Understanding all the factors that contribute to program sustainability, such as strategic planning, organizational capacity, strategic partnerships, and program visibility ─and importantly, funding stability ─can help build program capacity for sustainability. This also will position your current and future efforts for long-term success, even when a particular funding period is over.
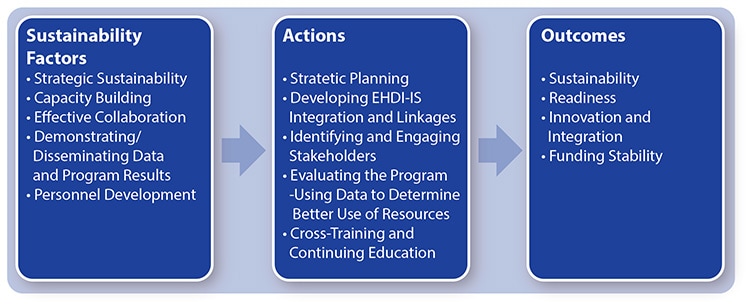
Primary Dimensions of Sustainability for EHDI Programs
- Strategic Planning
Strategic planning is critical to the successful development, implementation and maintenance of the EHDI-IS. Without a strategic direction and long-term goals, programs and systems find themselves only reacting to day-to-day demands. A strategic plan can be either goals-based or issues-based.
- Goals-based: Beginning with your mission and vision, create goals towards that mission through action planning (who will do what and when). The use of a logic model and a work plan can be very helpful in strategic planning [PDF – 519 KB].
A logic model provides a visual representation of the program and the intended outcomes. It illustrates the relationship between program activities and their expected outcomes. The work plan allows programs to clearly define the objectives and activities they will incorporate to meet those objectives, as well as the measures used to determine progress.
- Issues-based: Begin by examining issues, then develop strategies and action plans to address those issues.
- Capacity Building Organizational capacity and strong leadership at the jurisdictional level will be a key factor in program sustainability.Leaders at the jurisdictional level who ensure that the EHDI program is integrated into statewide strategic planning are likely to have stronger, more sustainable programs. According to the PHAB’s Standards and Measures [PDF – 1.44MB][4] document (a guidance specifically for public health departments preparing for accreditation Standard 11.1), public health departments must “develop and maintain an operational infrastructure to support the performance of public health functions.” EHDI program leaders benefit from ensuring that the program is well integrated into the operations of the organization, which can be done by creating formal linkages. Brainstorm and select a list of opportunities that may allow the program to expand the EHDI-IS’s capability, such as integration with Vital Records. Ensure that personnel are fully trained. If one individual needs additional training or assistance, consider ways to provide this in a timely manner. Consider cross-training so that job responsibilities are not isolated to one individual.
- Effective Partnerships Effective partnerships can help programs achieve sustainability.[5] By leveraging partnerships and collaborations, jurisdictions may be able to increase program and services capacity, become more efficient, and decrease the likelihood of duplicated efforts. It is important for programs to identify their needs and opportunities for building lasting and effective partnerships, and to establish a clear purpose for collaborative efforts. Doing so will help secure partners who are committed to sharing the responsibility of sustaining program and service efforts, and the benefits they generate. EHDI champions and advisory boards are key to the success and sustainability of EHDI programs.
- Demonstrating/Disseminating Program Data Program Visibility and Communication Ensuring that people are aware of the program is important. Being able to demonstrate the impact and benefits of the EHDI program and the EHDI-IS is a key aspect of sustainability. Agency leaders at the jurisdictional level will not be successful in sustaining EHDI programs unless they are able to promote the program and effectively communicate and demonstrate past and current success through data and results. Evaluate program process and outcomes, and inform stakeholders of results. Adaptable programs are better able to meet the needed changes identified by evaluation. Explain how the program will use the evaluation results to make better use of resources.
- Funding Stability Nothing better demonstrates the need for a program’s continuation and support than data showing its successes and impact. Programs might consider whether they can create a diverse base for program funding and support. A 2012 study of program longevity factors found that diversity of funding was the most significant financial factor in predicting sustainability.[6] Understanding the current funding environment helps programs ensure adequate sustainability planning is part of their organizational strategy. Some ideas include
- Look at possible funding from the state health department to support EHDI efforts. According to the Standards and Measures document, public health departments “…are required to manage resources wisely, to analyze present and future needs, to sustain operations, and demonstrate accountability”; that is, they must establish effective financial management systems and seek resources to enhance programs and interventions.
- Seek financial support from other sources or in-kind resources (e.g., personnel time, supplies; recruit partners with needed skills, etc.).
- Estimate the maintenance cost of the EHDI-IS by identifying the individual major cost categories and the variables that drive those costs (e.g., human resources, software and hardware maintenance fees, hardware replacement, internet connectivity, and ongoing training needs), and identify ways to reduce those costs.
- Take every opportunity to promote the value of the program, such as by disseminating success stories of identified D/HH infants and young children.
- Evaluation and Action Plan Evaluation data that document the effectiveness of your Information System in achieving outcomes are vital to the pursuit of new funding sources. This can be more easily attained if program evaluation is integrated into your strategic planning.
As part of planning for sustainability, it is important for EHDI programs to assess their current operating environment to determine their sustainability capacity. A best practice includes reviewing areas of weakness within your assessment results and deciding which ones are most urgent to address. The Center for Public Health Systems Science, at Washington University in St. Louis, developed the Sustainability Framework and the Program Sustainability Assessment Tool. This tool can be used to assess a program’s sustainability capacity, and is discussed in more detail here.[7]
Programs might consider developing a sustainability action plan that is reviewed and updated on a routine basis. Considering the results of your sustainability assessment profile helps determine priorities and areas needing attention. The following template may be helpful in developing your sustainability action plan:
EHDI Sustainability Action Plan
Consider the results of your program sustainability assessment to identify your priority domains.For each of the priority domains, consider the following:
- Action Steps: What are the next 3 steps to address this domain?
- Identify who is responsible for each step and a timeframe
- Resources:
- What agencies, organizations, or individuals need to be involved?
- What resources will be needed and how could you obtain those resources?
- Monitoring Progress:
- How will you track progress and know you have succeeded?
EHDI Sustainability Action Plan Primary Dimension Action Steps
Resources
Monitoring Progress
Responsibility Timeframe Strategic planning Funding stability Organizational capacity Effective partnerships Strategic communication EHDI-IS evaluation - Action Steps: What are the next 3 steps to address this domain?
Summary
Ideally, an EHDI-IS is not just a data repository; it is an integral, dynamic tool that ensures the program’s success. And, important to sustainability, it demonstrates the impact of the program’s work to all interested stakeholders. To achieve an EHDI-IS that best fulfills its role, thoughtful planning, development, and evaluation are needed. The concepts introduced in this chapter and discussed in greater detail in subsequent chapters can help you optimize your EHDI-IS and support the program’s work to its ultimate goal: to ensure the early identification and success of all D/HH infants and young children.
[2] Schell SF, Luke DA, Schooley MW, Elliott MB, Herbers SH, Mueller NB, et al. (2013). Public health program capacity for sustainability: a new framework. Implementation Science 8:15; http://www.ncbi.nlm.nih.gov/pubmed/23375082
[3] https://opa.hhs.gov/sites/default/files/2021-02/framework-for-program-sustainability.pdf [PDF – 624KB]
[5] Hanson HM, Salmoni AW. (2011). Stakeholders’ perceptions of programme sustainability: Findings from a community-based fall prevention programme. The Journal of Public Health 125:525-532.
[6] Savaya R, Spiro S, Elran-Barak R. (2008). Sustainability of social programs: A comparative case study analysis. American Journal of Evaluation 29(4):478-493.
