Prevalence of Diagnosed Arthritis — United States, 2019–2021
Weekly / October 13, 2023 / 72(41);1101–1107
Elizabeth A. Fallon, PhD1; Michael A. Boring, MS2; Anika L. Foster, DrPH1; Ellen W. Stowe, PhD1; Tyler D. Lites, MPH1,3; Erica L. Odom, DrPH1; Puja Seth, PhD1 (View author affiliations)
View suggested citationSummary
What is already known about this topic?
Arthritis is a leading cause of activity limitations, disability, and chronic pain, and is associated with dispensed opioid prescriptions, substantially contributing to health care costs.
What is added by this report?
During 2019–2021, 21.2% of U.S. adults (53.2 million) reported diagnosed arthritis. Approximately one half (52.2%–62.4%) of adults aged ≥65 years with self-reported diagnosed dementia, chronic obstructive pulmonary disease, stroke, heart disease, diabetes, or cancer also had a reported diagnosis of arthritis.
What are the implications for public health practice?
These prevalence estimates can be used to guide public health policies and activities to increase equitable access to physical activity opportunities within the built environment and other community-based, arthritis-appropriate, evidence-based interventions.
Altmetric:
Abstract
Arthritis includes approximately 100 conditions that affect the joints and surrounding tissues. It is a leading cause of activity limitations, disability, and chronic pain, and is associated with dispensed opioid prescriptions, substantially contributing to health care costs. Combined 2019–2021 National Health Interview Survey data were analyzed to update national prevalence estimates of self-reported diagnosed arthritis. An estimated 21.2% (18.7% age-standardized) of U.S. adults aged ≥18 years (53.2 million) had diagnosed arthritis during this time frame. Age-standardized arthritis prevalences were higher among women (20.9%) than men (16.3%), among veterans (24.2%) than nonveterans (18.5%), and among non-Hispanic White (20.1%) than among Hispanic or Latino (14.7%) or non-Hispanic Asian adults (10.3%). Adults aged ≥45 years represent 88.3% of all U.S. adults with arthritis. Unadjusted arthritis prevalence was high among adults with chronic obstructive pulmonary disease (COPD) (57.6%), dementia (55.9%), a disability (54.8%), stroke (52.6%), heart disease (51.5%), diabetes (43.1%), or cancer (43.1%). Approximately one half of adults aged ≥65 years with COPD, dementia, stroke, heart disease, diabetes, or cancer also had a diagnosis of arthritis. These prevalence estimates can be used to guide public health policies and activities to increase equitable access to physical activity opportunities within the built environment and other arthritis-appropriate, evidence-based interventions.
Introduction
Arthritis includes approximately 100 conditions that affect the joints and surrounding tissues. If not managed properly, arthritis can result in severe pain, activity limitations, and disability (1–3). Adults with arthritis have disproportionate rates of anxiety and depression and received 55.3% of all-cause prescription opioids dispensed in the United States in 2015 (4,5). Thus, arthritis is a significant driver of lost wages, disability, and medical costs (3,6). Updated arthritis prevalence estimates can help identify disproportionately affected groups, monitor arthritis prevalence over time, and guide resource allocation.
Methods
The National Health Interview Survey (NHIS) is an annual, nationally representative household survey of the noninstitutionalized U.S. civilian population.* One adult in a household is randomly selected to complete the in-home interview. When necessary, telephone follow-up is permitted to complete the interview.† If the selected person is physically or mentally unable to answer the survey, a knowledgeable proxy can answer on behalf of the selected person. During April–June 2020, the COVID-19 pandemic necessitated a change to telephone-only data collection. During July 2020–April 2021, interviews were attempted by telephone first, with in-home follow-up to complete data collection. In May 2021, data collection returned to prepandemic procedures.§
NHIS sample sizes and response rates for 2019, 2020, and 2021 were 31,997 (59.1%), 21,153 (48.9%), and 29,482 (50.9%), respectively.¶ A person was identified as having arthritis if he or she responded “yes” to the question, “Have you ever been told by a doctor or other health care professional that you have arthritis, rheumatoid arthritis, gout, lupus, or fibromyalgia?” Survey respondents answering “yes” or “no” to this item were included in the analytic sample (82,503; 99.8% of survey respondents). Data were weighted to account for complex survey design, selection probability, and nonresponse. Unadjusted and age-standardized** arthritis prevalence estimates for adults aged ≥18 years were calculated overall and by selected self-reported demographic and health characteristics. Subgroup prevalences were compared with a reference group using t-tests; all differences are significant at α = 0.05. Analyses were conducted in SAS (version 9.4; SAS Institute) and SUDAAN (version 11.0; RTI International). This activity was reviewed by CDC, deemed not research, and was conducted consistent with applicable federal law and CDC policy.††
Results
Approximately 53.2 million (95% CI = 52.1–54.4) or 21.2% (18.7% age-standardized) of U.S. adults aged ≥18 years had diagnosed arthritis (Table 1). Age-standardized prevalence was higher among women (20.9%) than men (16.3%) and among veterans (24.2%) than nonveterans (18.5%). Age-standardized prevalence was higher among non-Hispanic White (20.1%) than among Hispanic or Latino (14.7%) or non-Hispanic Asian adults (10.3%). There was no difference between non-Hispanic White and non-Hispanic Black or African American adults (19.7%), or non-Hispanic American Indian or Alaska Native adults (21.0%). The unadjusted prevalence of arthritis among U.S. adults with a disability was 54.8% (12.3 million); after adjusting for age, prevalence was higher among adults with a disability (40.5%) than among those without a disability (16.6%).
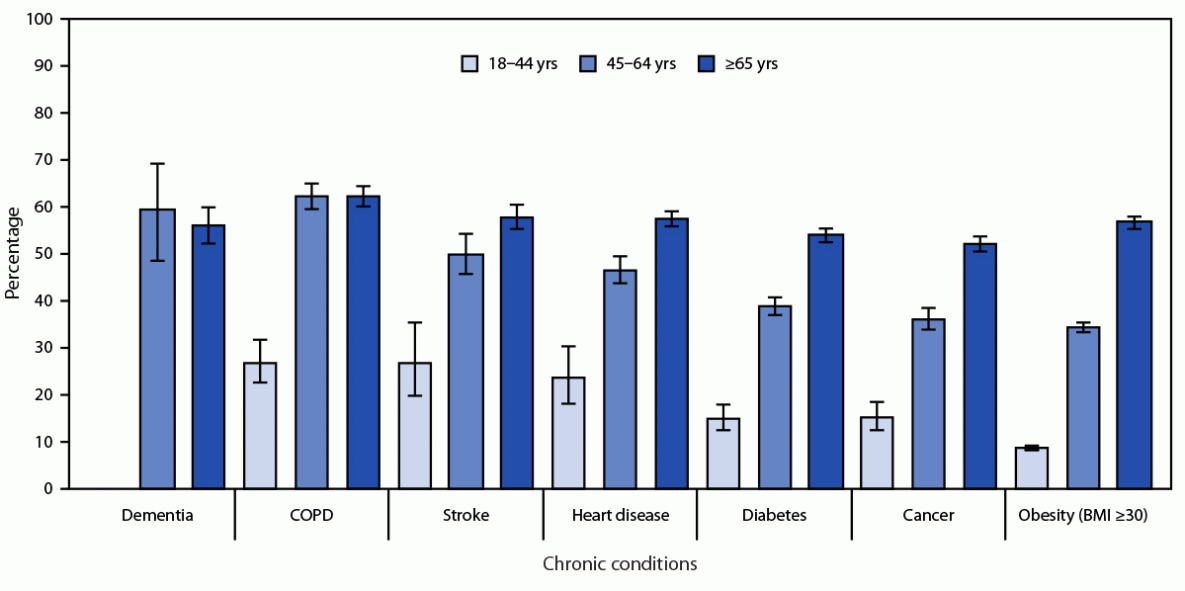
Adults aged ≥45 years represent 88.3% of all U.S. adults with arthritis. Nearly one half of adults with arthritis (48.3%; 25.7 million) were aged ≥65 years, and 40.0% (21.3 million) were aged 45–64 years. Age-standardized prevalence of arthritis was higher among adults with dementia (47.8%),§§ chronic obstructive pulmonary disease (COPD) (43.5%), stroke (39.0%), heart disease (36.3%), diabetes (28.8%), or cancer (27.7%), than among adults without these chronic conditions (Table 1). The U.S. arthritis prevalence was substantial among adults with COPD (57.6%; 6.8 million), dementia (55.9%; 1.4 million), stroke (52.6%; 3.7 million), heart disease (51.5%; 8.2 million), diabetes (43.1%; 10.2 million), or cancer (43.1%; 8.3 million). Among adults aged ≥65 years, approximately one half of those with COPD (62.4%), stroke (57.9%), heart disease (57.4%), obesity (body mass index ≥30 kg/m2; 56.8%), dementia (56.1%), diabetes (54.0%), or cancer (52.2%) also had diagnosed arthritis (Table 2) (Figure).
Discussion
During 2019–2021, 53.2 million (21.2%) U.S. adults aged ≥18 years had diagnosed arthritis. Approximately one half of adults aged ≥65 years with a chronic disease also reported diagnosed arthritis. Consistent with previous NHIS (1) and Behavioral Risk Factor Surveillance System data (7), arthritis prevalence was higher among women than men, among adults aged 45–64 and ≥65 years than among those aged 18–44 years, among veterans than among nonveterans, among persons with a disability than among those without a disability, and among persons reporting a comorbid chronic condition than among those without such a condition.
The 2019–2021 NHIS prevalence estimate is lower than the 2016–2018 NHIS prevalence estimate (58.5 million; 23.7%) (1). The NHIS survey was redesigned in 2019 (8), resulting in reordering and eliminating some arthritis-relevant questions, which might have led to differences in respondents’ ability to recall an arthritis diagnosis. Therefore, estimates produced by NHIS before 2019 should not be statistically compared with NHIS estimates after 2019, but instead interpreted as independent estimates obtained from different survey methodologies. This study establishes a new baseline for monitoring NHIS arthritis prevalence estimates, beginning with the combined 2019–2021 data. These estimates can be used to guide public health activities, policies, and resource allocation for improving arthritis-attributable health outcomes and associated health care costs.
Limitations
The findings in this report are subject to at least five limitations. First, because of the cross-sectional nature of NHIS, causality among selected characteristics and arthritis diagnosis cannot be inferred. Second, arthritis diagnosis was self-reported and was not validated by medical record review. Third, social desirability, recall, and proxy response biases might lead to over- or underestimation of arthritis prevalence. Fourth, the single survey item assessing diagnosed arthritis does not capture undiagnosed arthritis or allow prevalence estimates to be calculated for arthritis subtypes. Finally, although annual prevalence estimates of arthritis were similar during 2019–2021, the COVID-19 pandemic necessitated changes in data collection methods and might have altered U.S. adult health care use and potentially affected estimates of diagnosed arthritis.
Implications for Public Health Practice
Physical activity is important for managing arthritis-attributable pain and improving physical function (9). Many adults, including those with arthritis, do not meet the 2018 Physical Guidelines for Americans recommendations for physical activity despite its known benefits¶¶; these recommendations include engaging in 150–300 minutes of moderate-intensity or 75–150 minutes of vigorous-intensity activity per week or an equivalent combination, as well as ≥2 days of strength training per week. The guidelines also recommend that adults aged ≥65 years do multicomponent physical activity that includes balance training and aerobic and muscle strengthening activities. When an older adult or adult with arthritis cannot meet these recommendations because of health conditions, they need to be as physically active as their health and abilities allow.***
Maintaining a healthy weight, engaging in sufficient physical activity, and avoiding joint injury are important for prevention. The CDC Arthritis Management and Wellbeing Program recognizes community-based, arthritis-appropriate, evidence-based interventions (AAEBIs)††† to increase physical activity and chronic disease self-management among adults with arthritis. A recommendation from a health care provider can increase the likelihood that adults with arthritis attend education programs and engage in physical activity (10). CDC funds national and state organizations§§§ to increase the availability of AAEBIs in the community, as well as to increase awareness among health care providers and health systems about the need to screen adults with arthritis for physical activity and facilitate the use of appropriate tools for physical activity screening, counseling, and referral to AAEBIs, with emphasis on reaching populations and communities with high prevalences of arthritis. Increasing equitable access to physical activity opportunities within the built environment and across settings (e.g., worksites, community organizations, and home), implementing AAEBIs as independent interventions or in combination with other chronic disease management programs (e.g., Diabetes Prevention Program), and adopting health care systems policies and actions facilitating health care provider screening, counseling, and referrals or linkages, are public health priorities to address arthritis and arthritis-attributable health outcomes.
Corresponding author: Elizabeth A. Fallon, EFallon@cdc.gov.
1Division of Population Health, National Center for Chronic Disease Prevention and Health Promotion, CDC; 2American Society of Radiologic Technologists, Smyrna, Georgia; 3Oak Ridge Institute for Science and Education, Oak Ridge, Tennessee.
All authors have completed and submitted the International Committee of Medical Journal Editors form for disclosure of potential conflicts of interest. No potential conflicts of interest were disclosed.
* https://www.cdc.gov/nchs/nhis/index.htm
† https://www.cdc.gov/nchs/nhis/data-questionnaires-documentation.htm
§ https://ftp.cdc.gov/pub/Health_Statistics/NCHS/Dataset_Documentation/NHIS/2019/srvydesc-508.pdf; https://ftp.cdc.gov/pub/Health_Statistics/NCHS/Dataset_Documentation/NHIS/2020/srvydesc-508.pdf; https://ftp.cdc.gov/pub/Health_Statistics/NCHS/Dataset_Documentation/NHIS/2021/srvydesc-508.pdf
¶ Per NHIS instructions, the “sample adult partial” data file from 2020 was combined with the 2019 and 2021 data for this analysis. https://www.cdc.gov/nchs/nhis/2020nhis.htm
** Age-standardized to the 2000 projected U.S. adult population with three age groups (18–44, 45–64, and ≥65 years). https://www.cdc.gov/nchs/data/statnt/statnt20.pdf
†† 45 C.F.R. part 46.102(l)(2), 21 C.F.R. part 56; 42 U.S.C. Sect. 241(d); 5 U.S.C. Sect. 552a; 44 U.S.C. Sect. 3501 et seq.
§§ A total of 45.9% of respondents with dementia used a survey proxy, compared with 2.0% of survey respondents without dementia, indicating greater potential for proxy response bias among adults with dementia.
¶¶ Part C. https://health.gov/sites/default/files/2019-09/PAG_Advisory_Committee_Report.pdf
*** https://health.gov/sites/default/files/2019-09/Physical_Activity_Guidelines_2nd_edition.pdf
References
- Theis KA, Murphy LB, Guglielmo D, et al. Prevalence of arthritis and arthritis–attributable activity limitation—United States, 2016–2018. MMWR Morb Mortal Wkly Rep 2021;70:1401–7 https://doi.org/10.15585/mmwr.mm7040a2 PMID:34618800
- Barbour KE, Boring M, Helmick CG, Murphy LB, Qin J. Prevalence of severe joint pain among adults with doctor-diagnosed arthritis—United States, 2002–2014. MMWR Morb Mortal Wkly Rep 2016;65:1052–6 https://doi.org/10.15585/mmwr.mm6539a2 PMID:27711038
- Theis KA, Steinweg A, Helmick CG, Courtney-Long E, Bolen JA, Lee R. Which one? What kind? How many? Types, causes, and prevalence of disability among U.S. adults. Disabil Health J 2019;12:411–21 https://doi.org/10.1016/j.dhjo.2019.03.001 PMID:31000498
- Murphy LB, Cisternas MG, Theis KA, et al. All-cause opioid prescriptions dispensed: the outsized role of adults with arthritis. Am J Prev Med 2020;59:355–66 https://doi.org/10.1016/j.amepre.2020.03.028 PMID:32763134
- Guglielmo D, Hootman JM, Boring MA, et al. Symptoms of anxiety and depression among adults with arthritis—United States, 2015–2017. MMWR Morb Mortal Wkly Rep 2018;67:1081–7 https://doi.org/10.15585/mmwr.mm6739a2 PMID:30286053
- Murphy LB, Cisternas MG, Pasta DJ, Helmick CG, Yelin EH. Medical expenditures and earnings losses among US adults with arthritis in 2013. Arthritis Care Res (Hoboken) 2018;70:869–76 https://doi.org/10.1002/acr.23425 PMID:28950426
- Zablotsky B, Lessem SE, Gindi RM, Maitland AK, Dahlhamer JM, Blumberg SJ. Overview of the 2019 National Health Interview Survey questionnaire redesign. Am J Public Health 2023;113:408–15 https://doi.org/10.2105/AJPH.2022.307197 PMID:36758202
- Murphy LB, Helmick CG, Allen KD, et al.; CDC. Arthritis among veterans—United States, 2011–2013. MMWR Morb Mortal Wkly Rep 2014;63:999–1003. PMID:25375071
- Kolasinski SL, Neogi T, Hochberg MC, et al. 2019 American College of Rheumatology/Arthritis Foundation guideline for the management of osteoarthritis of the hand, hip, and knee. Arthritis Rheumatol 2020;72:220–33. https://doi.org/10.1002/art.41142 PMID:31908163
- Murphy LB, Theis KA, Brady TJ, Sacks JJ. Supporting self-management education for arthritis: evidence from the Arthritis Conditions and Health Effects Survey on the influential role of health care providers. Chronic Illn 2021;17:217–31. https://doi.org/10.1177/1742395319869431 PMID:31475576
Abbreviations: BMI = body mass index; COPD = chronic obstructive pulmonary disease; NA = not applicable; NH = non-Hispanic; Ref = referent group.
* Unadjusted and age-standardized estimates are calculated using sampling weights to produce nationally representative prevalences. Age-standardized estimates were calculated using 82,290 (99.6%) respondents, with complete data for both arthritis and age questions. Estimates are age-standardized to the 2000 U.S. projected adult population, using three age groups: 18–44, 45–64, and ≥65 years. https://www.cdc.gov/nchs/data/statnt/statnt20.pdf
† Responded “yes” to the question, “Have you ever been told by a doctor or other health professional that you had some form of arthritis, rheumatoid arthritis, gout, lupus, or fibromyalgia?”
§ Might not sum to column total for some categories because of item-specific missing data.
¶ Might not sum to 100% because of rounding.
** During the COVID-19 pandemic (April 2020–May 2021), data collection procedures changed from in-home to telephone-based and back to in-home. This analysis combined the 2020 partial adult sample data file with 2019 and 2021 data to obtain arthritis prevalence for 2019–2021. Therefore, the 2020 estimate displayed is only used to explore the potential effects of COVID-19 and should not be used as a single year estimate of diagnosed arthritis for 2020. https://ftp.cdc.gov/pub/Health_Statistics/NCHS/Dataset_Documentation/NHIS/2020/srvydesc-508.pdf
†† T-tests were used to determine statistically significant differences in arthritis prevalence by survey year; differences with p≤0.05 were considered statistically significant. Despite statistically significant differences by year for age-adjusted arthritis prevalence, crude prevalence and weighted population estimates were not substantively different across years.
§§ T-tests were used to determine statistically significant differences in arthritis prevalence for subgroups defined by selected characteristics; differences with p≤0.05 were considered statistically significant.
¶¶ Identified as “male” or “female” in response to the question, “are you male or female?”
*** Racial and ethnic categories from the sample adult file codebook were used. Persons identifying as “other single and multiple race,” or “NH American Indian or Alaska Native and any other group” were combined into “Other, multiple races, NH.”
††† The sample adult file codebook sexual orientation categories were used. Survey responses coded as “refused,” “don’t know,” “not ascertained,” or missing responses were excluded.
§§§ Responses to the question, “What is the highest level of school you completed…?” were combined into the following groups: 1) less than high school graduate: never attended/attended only kindergarten, grades 1–11, or attended 12th grade but did not get a diploma, 2) high school graduate or equivalent: graduated high school, or earned a general education development certificate, 3) at least some college: some college or associate degree, and 4) college degree or greater: bachelor’s, master’s, professional school, or doctoral degree.
¶¶¶ Persons responding “yes” to the question, “Do you usually work 35 hours or more per week in total at all jobs or businesses?” were considered “employed/self-employed.” Persons responding “no” were asked “What is the MAIN reason you were not working for pay…?” with responses categorized as 1) unemployed: “unemployed, laid off, seasonal/contract work, looking for work,” 2) retired: “retired,” 3) unable to work/disabled: “unable to work for health reasons/disabled,” and 4) other: all remaining valid options.
**** Income-to-poverty ratio values for the income-to-poverty ratio variable were calculated using National Health Interview Survey imputed income files. https://ftp.cdc.gov/pub/Health_Statistics/NCHS/Dataset_Documentation/NHIS/2021/NHIS2021-imputation-techdoc-508.pdf; https://ftp.cdc.gov/pub/Health_Statistics/NCHS/Dataset_Documentation/NHIS/2020/NHIS2020-imputation-techdoc-508.pdf; https://ftp.cdc.gov/pub/Health_Statistics/NCHS/Dataset_Documentation/NHIS/2019/NHIS2019-imputation-techdoc-508.pdf
†††† Veterans were defined as respondents who answered “yes” to “Did you ever serve on active duty in the U.S. Armed Forces, military Reserves, or National Guard?”
§§§§ Self-reported height and weight were used to calculate BMI [weight (kg)/(height [m])2].
¶¶¶¶ A respondent who reported a lot of difficulty or being unable to do an activity in any of the six Washington Group Short Set on Functioning items (vision, hearing, mobility, self-care, cognitive, or communication) was considered to have a disability.
***** Respondents were considered as having the following chronic diseases if they answered “yes” to “Have you ever been told by a doctor or other health professional that you have/had…” 1) heart disease: coronary heart disease, angina (angina pectoris), or heart attack (myocardial infarction); 2) cancer: cancer or a malignancy of any kind (excluding skin cancer); 3) dementia: dementia, including Alzheimer disease; 4) COPD, emphysema, or chronic bronchitis, 5) stroke, or 6) diabetes.
Abbreviations: BMI = body mass index; COPD = chronic obstructive pulmonary disease.
* Calculated using sampling weights to produce nationally representative prevalence estimates.
† Responded “yes” to the question, “Have you ever been told by a doctor or other health professional that you had some form of arthritis, rheumatoid arthritis, gout, lupus, or fibromyalgia?”
§ Self-reported height and weight were used to calculate BMI [weight (kg)/(height [m])2].
¶ Respondents were considered as having the following chronic diseases if they answered “yes” to “Have you ever been told by a doctor or other health professional that you have/had…” 1) heart disease: coronary heart disease, angina (angina pectoris), or heart attack (myocardial infarction); 2) cancer: cancer or a malignancy of any kind (excluding skin cancer); 3) dementia: dementia, including Alzheimer disease; 4) COPD, emphysema, or chronic bronchitis, 5) stroke, or 6) diabetes.
** The estimate is suppressed on the basis of the data presentation standards for proportions. https://www.cdc.gov/nchs/data/series/sr_02/sr02_175.pdf
†† Respondents answered “no” to “Have you ever been told by a doctor or other health professional that you have/had…” for all of the following: 1) heart disease: coronary heart disease, angina (angina pectoris), or heart attack (myocardial infarction); 2) cancer: cancer or a malignancy of any kind (excluding skin cancer); 3) dementia: dementia, including Alzheimer disease; 4) COPD, emphysema, or chronic bronchitis, 5) stroke, or 6) diabetes.
 FIGURE. Prevalence*,† of diagnosed arthritis§ among adults aged ≥18 years with selected chronic conditions,¶,** by age group — National Health Interview Survey, United States, 2019–2021
FIGURE. Prevalence*,† of diagnosed arthritis§ among adults aged ≥18 years with selected chronic conditions,¶,** by age group — National Health Interview Survey, United States, 2019–2021
Abbreviations: BMI = body mass index; COPD = chronic obstructive pulmonary disease.
* Calculated using sampling weights to produce nationally representative prevalence estimates. 95% CIs indicated by error bars.
† The estimate for dementia (18–44 years) is suppressed based on the data presentation standards for proportions. https://www.cdc.gov/nchs/data/series/sr_02/sr02_175.pdf
§ Responded “yes” to the question, “Have you ever been told by a doctor or other health professional that you had some form of arthritis, rheumatoid arthritis, gout, lupus, or fibromyalgia?”
¶ Respondents were considered as having the following chronic diseases if they answered “yes” to “Have you ever been told by a doctor or other health professional that you have or had…” 1) heart disease: coronary heart disease, angina (angina pectoris), or heart attack (myocardial infarction); 2) cancer: cancer or a malignancy of any kind (excluding skin cancer); 3) dementia: dementia, including Alzheimer disease; 4) COPD, emphysema, or chronic bronchitis, 5) stroke, or 6) diabetes.
** Self-reported height and weight were used to calculate BMI [weight (kg)/(height [m])2].
Suggested citation for this article: Fallon EA, Boring MA, Foster AL, et al. Prevalence of Diagnosed Arthritis — United States, 2019–2021. MMWR Morb Mortal Wkly Rep 2023;72:1101–1107. DOI: http://dx.doi.org/10.15585/mmwr.mm7241a1.
MMWR and Morbidity and Mortality Weekly Report are service marks of the U.S. Department of Health and Human Services.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All HTML versions of MMWR articles are generated from final proofs through an automated process. This conversion might result in character translation or format errors in the HTML version. Users are referred to the electronic PDF version (https://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.