Key points
- Mental health is an important part of overall health and refers to a person’s emotional, psychological, and social well-being. Mental health involves how we think, feel, act, and make choices.

Overview
Mental health disorders can be short- or long-term and can interfere with a person's mood, behavior, thinking, and ability to relate to others. Various studies have shown the impact of trauma, depression, anxiety, and stress on the body, including stress on the heart.123
What mental health disorders are related to heart disease?
Some of the most commonly studied mental health disorders associated with heart disease or related risk factors include the following:
Mood Disorders: People living with mood disorders, such as major depression or bipolar disorder, find that their mood affects both psychological and mental well-being nearly every day for most of the day.
Anxiety Disorders: People respond to certain objects or situations with fear, dread, or terror. Anxiety disorders include generalized anxiety, social anxiety, panic disorders, and phobias.
Post-Traumatic Stress Disorder (PTSD): People can experience PTSD after undergoing a traumatic life experience, such as war, natural disaster, or any other serious incident.
Chronic Stress: People are in a state of uncomfortable emotional stress—accompanied by predictable biochemical, physiological, and behavioral changes—that is constant and persists over an extended period of time.
There may be other behavioral health disorders, such as substance use disorders, that are connected to heart disease.
How it affects your health
What is the connection between mental health disorders and heart disease?
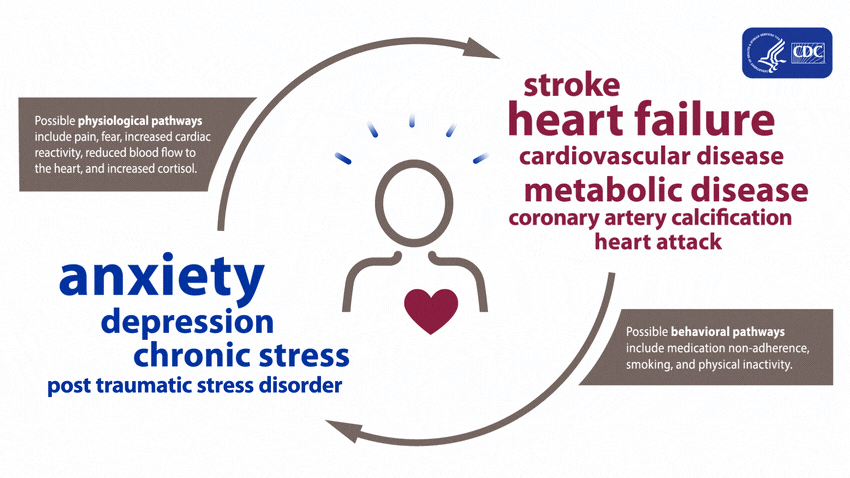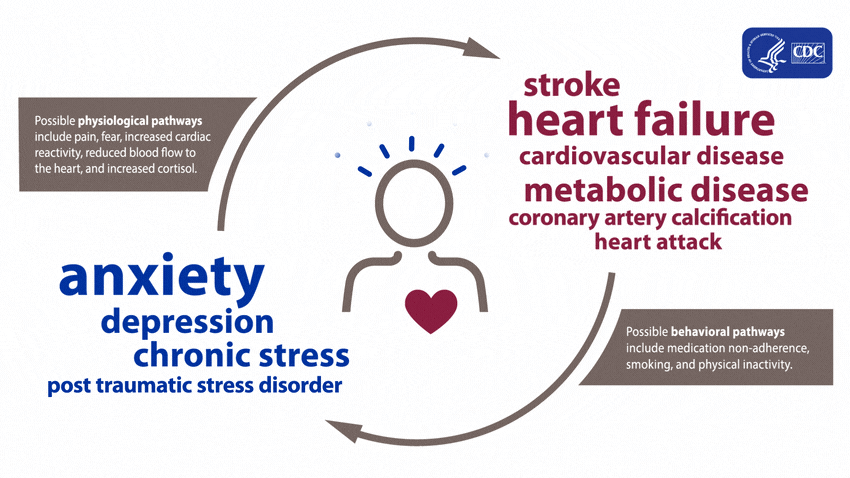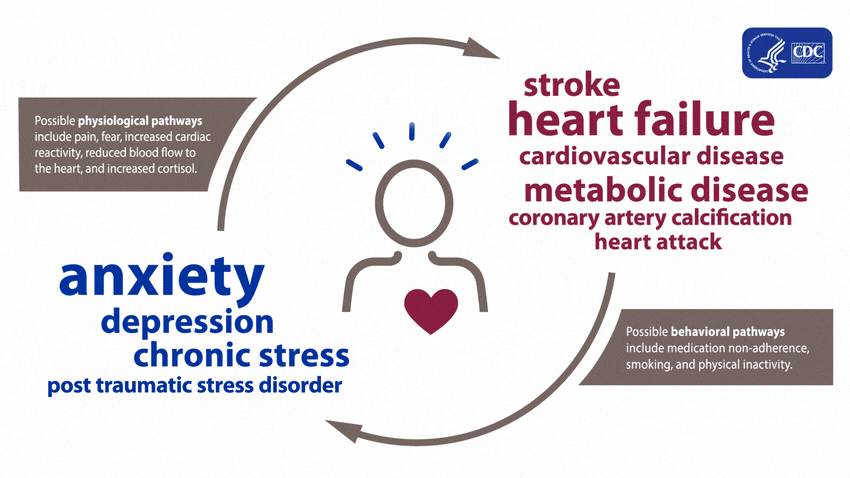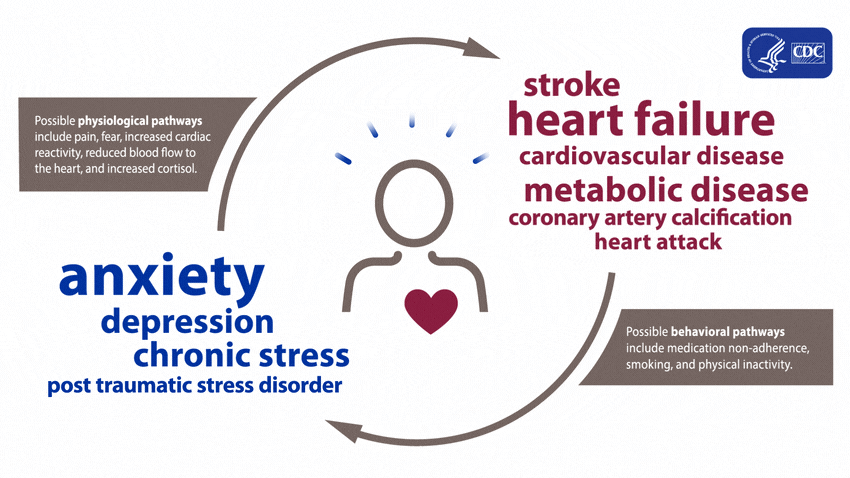
A large and growing body of research shows that mental health is associated with risk factors for heart disease before a diagnosis of a mental health disorder and during treatment. These effects can arise both directly, through biological pathways, and indirectly, through risky health behaviors.4
People experiencing depression, anxiety, stress, and even PTSD over a long period of time may experience certain physiologic effects on the body, such as increased cardiac reactivity (e.g., increased heart rate and blood pressure), reduced blood flow to the heart, and heightened levels of cortisol. Over time, these physiologic effects can lead to calcium buildup in the arteries, metabolic disease, and heart disease.15678910
Evidence shows that mental health disorders—such as depression, anxiety, and PTSD—can develop after cardiac events, including heart failure, stroke, and heart attack.4111213141516171819 These disorders can be brought on after an acute heart disease event from factors including pain, fear of death or disability, and financial problems associated with the event.415
Some literature notes the impact of medicines used to treat mental health disorders on cardiometabolic disease risk. The use of some antipsychotic medications has been associated with obesity, insulin resistance, diabetes, heart attacks, atrial fibrillation, stroke, and death.20
Mental health disorders such as anxiety and depression may increase the chance of adopting behaviors such as smoking, inactive lifestyle, or failure to take prescribed medications.4 This is because people experiencing a mental health disorder may have fewer healthy coping strategies for stressful situations, making it difficult for them to make healthy lifestyle choices to reduce their risk for heart disease.4
Who is at risk
Specific populations, such as the following, show higher rates of heart disease as a result of pre-existing mental health disorders:
Veterans. Studies found that veterans are at a higher risk for heart disease, mainly due to PTSD as a result of combat.2122232425
Women. Studies exclusively focused on women found that PTSD and depression may have damaging effects on physical health, particularly with increased risk for coronary heart disease (CHD)–related morbidity and mortality.2627
Couples with someone who has PTSD. Comparative studies found that couples where one or both partners had PTSD experienced more severe conflict, greater anger, and increased cardiovascular reactivity to conflict discussions than couples where neither partner had PTSD. Anger and physiological stress responses to couple discord might contribute to CHD and heart disease risk within these relationships.2829
Racial and ethnic minorities. Lastly, studies focused on racial or ethnic minority groups found that depression, stress, and anxiety due to disparities in social determinants of health,30 adverse childhood experiences,31 and racism/discrimination323334 could place certain subpopulations at a higher risk for hypertension,31323435 cardiovascular reactivity,34 heart disease,3033 and poor heart health outcomes.36
Reducing risk
Addressing mental health disorders early by providing access to appropriate services and support to increase healthy behaviors (e.g., increased physical activity, improved diet quality, and reduced smoking) can reduce someone's risk of experiencing a heart disease event.1214161827373839
Below are some actions that health care systems, health care professionals, individuals, and researchers can take to promote heart disease prevention and support mental health.
Actions for health care systems
- Set up multidisciplinary teams that include both mental health and heart disease professionals.40414243
- Employ clinical decision support or electronic health record systems to coordinate care among the multidisciplinary teams.4142
Actions for health care professionals
- Learn more about the link between mental health and heart disease18 with the following resources:
- Talk to your patients about the relationship between mental health and heart disease.127384445
- Incorporate mental health screening and treatment into care surrounding a major heart disease event and chronic disease.25716202431394446
- Involve individuals and their family members in communication and decision making regarding treatment following a heart disease event.14
- For patients with severe mental health disorders and pre-existing heart disease or its risk factors:20
Actions for individuals
- Recognize the signs and symptoms of mental health disorders and heart disease.
- Talk with your health care professionals about potential heart conditions in relation to your mental health disorder and treatment options.47
- Know that your family history and genetic factors likely play some role in your risk for heart disease.
- Know which conditions increase the risk of heart disease.
- Maintain a healthy lifestyle.
Actions for researchers
- Address the role of social determinants of health and health disparities in improving the intersection between mental health and heart health outcomes.4849
- Understand the link and impact of mental health on the prevention and treatment of heart disease and its risk factors.43
- Describe the biological pathway between mental health disorders and heart disease to understand the intermediate and long-term outcomes (e.g., chronic inflammation, cardiac reactivity, heart rate variability, and coronary artery calcification).2843465051525354
- Analyze the impact of emotional well-being (i.e., a state in which people understand and manage their emotions through achievable goals, positive relationships, and responsible decision making) on mental health and physical health.5556
- Expand traditional heart disease risk assessments, such as the Atherosclerotic Cardiovascular Disease Risk Estimator or Framingham 10-Year Risk of General Cardiovascular Disease 57to include mental health disorders.
- Develop valid and reliable screening instruments to help identify vulnerable populations.11
Resources
For more information about the link between mental health and heart disease, see the following resources:
- CDC: Interactive Atlas of Heart Disease and Stroke
- CDC: Mental Health
- Cleveland Clinic: Depression & Heart Disease
- National Institute of Mental Health: Chronic Illness & Mental Health
- Substance Abuse and Mental Health Services Administration (SAMHSA)–Health Resources and Services Administration (HRSA): Center for Integrated Health Solutions
- World Health Organization: Mental Health
- Bremner JD, Campanella C, Khan Z, Shah M, Hammadah M, Wilmot K, et al. Brain correlates of mental stress-induced myocardial ischemia. Psychosom Med. 2018;80(6):515–525.
- Del Gaizo AL, Elhai JD, Weaver TL. Posttraumatic stress disorder, poor physical health and substance use behaviors in a national trauma-exposed sample. Psychiatry Res. 2011;188(3):390–395.
- Sowden GL, Huffman JC. The impact of mental illness on cardiac outcomes: a review for the cardiologist. Int J Cardiol. 2009;132(1):30–37.
- Abed MA, Kloub MI, Moser DK. Anxiety and adverse health outcomes among cardiac patients: a biobehavioral model. J Cardiovasc Nurs. 2014;29(4):354–363.
- Hopkinson NS, Baxter N. Breathing SPACE—a practical approach to the breathless patient. NPJ Prim Care Respir Med. 2017;27(1):5.
- Jacob L, Haro JM, Koyanagi A. Post-traumatic stress symptoms are associated with physical multimorbidity: findings from the Adult Psychiatric Morbidity Survey 2007. J Affect Disord. 2018;232:385–392.
- Jurek B, Neumann ID. The oxytocin receptor: from intracellular signaling to behavior. Physiol Rev. 2018;98(3):1805–1908.
- Ning L, Guan S, Liu J. An investigation into psychological stress and its determinants in Xinjiang desert oil workers. Medicine (Baltimore). 2018;97(15):e0323.
- Quensell ML, Taira DA, Seto TB, Braun KL, Sentell TL. "I need my own place to get better": patient perspectives on the role of housing in potentially preventable hospitalizations. J Health Care Poor Underserved. 2017;28(2):784–797.
- Sambamoorthi U, Mitra S, Findley PA, Pogach LM. Decomposing sex differences in low-density lipoprotein cholesterol among veterans with or at risk for cardiovascular illness. Womens Health Issues. 2012;22(2):e201–208.
- Alosaimi F, Hawa R. Broken heart: broken mind. J Psychosom Res. 2009;67(4):285–287.
- Copeland LA, Sako EY, Zeber JE, et al. Mortality after cardiac or vascular operations by preexisting serious mental illness status in the Veterans Health Administration. Gen Hosp Psychiatry. 2014;36(5):502–508.
- Edmondson D, von Känel R. Post-traumatic stress disorder and cardiovascular disease. Lancet Psychiatry. 2017;4(4):320–329.
- Hwang B, Moser DK, Dracup K. Knowledge is insufficient for self-care among heart failure patients with psychological distress. Health Psychol. 2014;33(7):588–596.
- Lett HS, Blumenthal JA, Babyak MA, et al. Social support and prognosis in patients at increased psychosocial risk recovering from myocardial infarction. Health Psychol. 2007;26(4):418–427.
- Morin RT, Galatzer-Levy IR, Maccallum F, Bonanno GA. Do multiple health events reduce resilience when compared with single events? Health Psychol. 2017;36(8):721–728.
- Pino EC, Zuo Y, Borba CP, Henderson DC, Kalesan B. Clinical depression and anxiety among ST-elevation myocardial infarction hospitalizations: results from Nationwide Inpatient Sample 2004–2013. Psychiatry Res. 2018;266:291–300.
- Spitznagel MB, Potter V, Miller LA, et al. Ability to regulate emotion is predicted by depressive symptoms and cognitive function in a cardiac sample. J Cardiovasc Nurs. 2013;28(5):453–459.
- Violanti JM, Andrew ME, Burchfiel CM, Dorn J, Hartley T, Miller DB. Posttraumatic stress symptoms and subclinical cardiovascular disease in police officers. Int J Stress Manag. 2006;13(4):541–554.
- World Health Organization. WHO Guidelines: Management of Physical Health Conditions in Adults With Severe Mental Disorders. World Health Organization; 2018.
- Davis MB, Maddox TM, Langner P, Plomondon ME, Rumsfeld JS, Duvernoy CS. Characteristics and outcomes of women veterans undergoing cardiac catheterization in the Veterans Affairs Healthcare System: insights from the VA CART Program. Circ Cardiovasc Qual Outcomes. 2015;8(2 Suppl 1):S39–47.
- Dedert EA, Calhoun PS, Watkins LL, Sherwood A, Beckham JC. Posttraumatic stress disorder, cardiovascular, and metabolic disease: a review of the evidence. Ann Behav Med. 2010;39(1):61–78.
- Khazaie H, Saidi MR, Sepehry AA, et al. Abnormal ECG patterns in chronic post-war PTSD patients: a pilot study. Int J Behav Med. 2013;20(1):1–6.
- Oddone AE, Dennis PA, Calhoun PS, et al. Orthostatic hypotension in young adults with and without posttraumatic stress disorder. Psychol Trauma. 2015;7(3):229–233.
- Olff M, Meewisse ML, Kleber RJ, et al. Tobacco usage interacts with postdisaster psychopathology on circadian salivary cortisol. Int J Psychophysiol. 2006;59(3):251–258.
- Kubzansky LD, Koenen KC, Jones C, Eaton WW. A prospective study of posttraumatic stress disorder symptoms and coronary heart disease in women. Health Psychol. 2009;28(1):125–130.
- Schwartzman JB, Glaus KD. Depression and coronary heart disease in women: implications for clinical practice and research. Prof Psychol Res Pract. 2000;31(1):48–57.
- Caska CM, Smith TW, Renshaw KD, et al. Posttraumatic stress disorder and responses to couple conflict: implications for cardiovascular risk. Health Psychol. 2014;33(11):1273–1280.
- Troxel WM, DeSantis A, Germain A, Buysse DJ, Matthews KA. Marital conflict and nocturnal blood pressure dipping in military couples. Health Psychol. 2017;36(1):31–34.
- Belgrave FZ, Abrams JA. Reducing disparities and achieving equity in African American women's health. Am Psychol. 2016;71(8):723–733.
- Lehman BJ, Taylor SE, Kiefe CI, Seeman TE. Relationship of early life stress and psychological functioning to blood pressure in the CARDIA study. Health Psychol. 2009;28(3):338–346.
- Moody DLB, Chang YF, Pantesco EJ, et al. Everyday discrimination prospectively predicts blood pressure across 10 years in racially/ethnically diverse midlife women: study of women's health across the nation. Ann Behav Med. 2019;53(7):608–620.
- Paradies Y, Ben J, Denson N, et al. Racism as a determinant of health: a systematic review and meta-analysis. PLoS One. 2015;10(9):1–48.
- Peters RM, Butler K, Gjini K, Yeragani V, Boutros NN. The role of sensory gating in the racism/blood pressure relationship: a pilot study. J Psychophysiol. 2011;25(1):40–49.
- Hunter LR, Schmidt NB. Anxiety psychopathology in African American adults: literature review and development of an empirically informed sociocultural model. Psychol Bull. 2010;136(2):211–235.
- Brewer LC, Redmond N, Slusser JP, et al. Stress and achievement of cardiovascular health metrics: the American Heart Association Life's Simple 7 in blacks of the Jackson Heart Study. J Am Heart Assoc. 2018;7(11):1–16.
- Stewart JC, Perkins AJ, Callahan CM. Effect of collaborative care for depression on risk of cardiovascular events: data from the IMPACT randomized controlled trial. Psychosom Med. 2014;76(1):29–37.
- Appleton AA, Buka SL, Loucks EB, Gilman SE, Kubzansky LD. Divergent associations of adaptive and maladaptive emotion regulation strategies with inflammation. Health Psychol. 2013;32(7):748–756.
- Van den Berk-Clark C, Secrest S, Walls J, et al. Association between posttraumatic stress disorder and lack of exercise, poor diet, obesity, and co-occuring smoking: a systematic review and meta-analysis. Health Psychol. 2018;37(5):407–416.
- Katon WJ, Lin EH, Von Korff M, et al. Collaborative care for patients with depression and chronic illnesses. N Engl J Med. 2010;363(27):2611–2620.
- Community Preventive Services Task Force. Recommendation for use of collaborative care for the management of depressive disorders. Am J Prev Med. 2012;42(5):521–524.
- Thota AB, Sipe TA, Byard GJ, et al. Collaborative care to improve the management of depressive disorders: a Community Guide systematic review and meta-analysis. Am J Prev Med. 2012;42(5):525–538.
- Gerber MR, King MW, Iverson KM, Pineles SL, Haskell SG. Association between mental health burden and coronary artery disease in U.S. women veterans over 45: a national cross-sectional study. J Womens Health. 2018;27(3):238–244.
- Hawkley LC, Masi CM, Berry JD, Cacioppo JT. Loneliness is a unique predictor of age-related differences in systolic blood pressure. Psychol Aging. 2006;21(1):152–164.
- Zen AL, Whooley MA, Zhao S, Cohen BE. Post-traumatic stress disorder is associated with poor health behaviors: findings from the Heart and Soul Study. Health Psychol. 2012;31(2):194–201.
- Kinder LS, Kamarck TW, Baum A, Orchard TJ. Depressive symptomatology and coronary heart disease in type I diabetes mellitus: a study of possible mechanisms. Health Psychol. 2002;21(6):542–552.
- Chaddha A, Robinson EA, Kline-Rogers E, Alexandris-Souphis T, Rubenfire M. Mental health and cardiovascular disease. Am J Med. 2016;129(11):1145–1148.
- Havranek EP, Mujahid MS, Barr DA, et al. Social determinants of risk and outcomes for cardiovascular disease: a scientific statement from the American Heart Association. Circulation. 2015;132(9):873–898.
- Tawakol A, Osborne MT, Wang Y, et al. Stress-associated neurobiological pathway linking socioeconomic disparities to cardiovascular disease. J Am Coll Cardiol. 2019;73(25):3243–3255.
- Agorastos A, Boel JA, Heppner PS, et al. Diminished vagal activity and blunted diurnal variation of heart rate dynamics in posttraumatic stress disorder. Stress. 2013;16(3):300–310.
- Carroll AJ, Carnethon MR, Liu K, et al. Interaction between smoking and depressive symptoms with subclinical heart disease in the Coronary Artery Risk Development in Young Adults (CARDIA) study. Health Psychol. 2017;36(2):101–111.
- Pizzi C, Manzoli L, Mancini S, Costa GM. Analysis of potential predictors of depression among coronary heart disease risk factors including heart rate variability, markers of inflammation, and endothelial function. Eur Heart J. 2008;29(9):1110–1117.
- Rohleder N. Stress system regulation of chronic low-grade inflammation. Adv Neuroimmune Biol. 2012;3(3):265–276.
- Smith TW, Uchino BN, Berg CA, et al. Associations of self-reports versus spouse ratings of negative affectivity, dominance, and affiliation with coronary artery disease: where should we look and who should we ask when studying personality and health? Health Psychol. 2008;27(6):676–684.
- Kubzansky LD, Huffman JC, Boehm JK, et al. Positive psychological well-being and cardiovascular disease: JACC Health Promotion Series. J Am Coll Cardiol. 2018;72(12):1382–1396.
- Sin NL. The protective role of positive well-being in cardiovascular disease: review of current evidence, mechanisms, and clinical implications. Curr Cardiol Rep. 2016;18(11):106.
- Jin H, Folsom D, Sasaki A, et al. Increased Framingham 10-year risk of coronary heart disease in middle-aged and older patients with psychotic symptoms. Schizophr Res. 2011;125(2-3):295–299.
