Streptococcal Toxic Shock Syndrome
Streptococcal toxic shock syndrome (STSS) is a disease defined as an infection with Streptococcus pyogenes accompanied by sudden onset of shock, organ failure, and frequently death.
Etiology
STSS is caused by S. pyogenes, which are also called group A Streptococcus (group A strep). When production of bacterial exotoxins and virulence factors occur in the deep tissues and bloodstream, this can lead to the induction of the cytokine cascade. Massive cytokine cascades contribute to the development of shock or organ failure.
S. pyogenes are gram-positive cocci that grow in chains (see Figure 1). They exhibit β-hemolysis (complete hemolysis) when grown on blood agar plates. They belong to group A in the Lancefield classification system for β-hemolytic Streptococcus, and thus are also called group A streptococci.
Clinical features
STSS often begins with influenza-like symptoms, including:
- Fever
- Chills
- Myalgia
- Nausea
- Vomiting
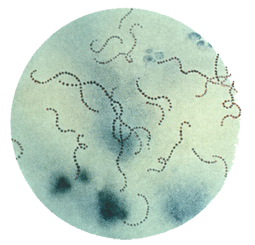
Figure 1. Streptococcus pyogenes (group A Streptococcus) on Gram stain. Source: Public Health Image Library, CDC
These symptoms often quickly progress to sepsis with hypotension, tachycardia, tachypnea, and signs and symptoms suggestive of specific organ failure, including of the following organ systems:
- Kidney
- Liver
- Lung
- Blood
Transmission
Any group A strep infection may progress to STSS. Disease occurs with entry of the bacterium through a compromised barrier (such as a skin injury) or through mucus membranes. The bacteria then spread to deep tissues and eventually to the bloodstream. The main sites of entry for streptococci leading to toxic shock syndrome include:
- Vagina
- Pharynx
- Mucosa
- Skin/soft tissue
Any skin injury or breakdown, including surgical wounds, may provide a site of entry for the bacteria. Unfortunately, route of entry remains unknown for up to 50% of cases.
Secondary cases among close contacts or healthcare workers are rare, although have been known to occur.
Incubation period
The incubation period for STSS varies depending on site of entry. Once initial symptoms occur, hypotension generally develops within 24 to 48 hours.
Risk factors
STSS can occur in anyone, but risk factors can include:
Age: STSS is more common in adults 65 years of age or older.
Skin injury or breakdown: Recently having surgery, a viral infection that causes open sores (like varicella), or other skin injury increases risk for developing STSS.
Chronic illnesses: Having alcohol use disorder or diabetes can also increase risk for developing STSS.
Additionally, strains of group A strep that produce certain virulence factors and exotoxins, particularly streptococcal pyrogenic exotoxins, are more likely to cause STSS and other severe infections.1
Use of non-steroidal anti-inflammatory drugs (NSAIDs) may also increase risk, although evidence for this is limited.
Diagnosis and testing
The differential diagnosis of patients in the early stages of STSS is broad, including other viral or bacterial infections (such as staphylococcal toxic shock); therefore, patients are often misdiagnosed.
Diagnosis of STSS is made based on the Nationally Notifiable Diseases Surveillance System 2010 case definition.
STSS clinical case definition
An illness associated with invasive or noninvasive group A strep infection with the following clinical manifestations:
- Hypotension defined by a systolic blood pressure less than or equal to 90 mm Hg for adults or less than the fifth percentile by age for children aged less than 16 years.
- Multi-organ involvement characterized by two or more of the following:
- Renal impairment: Creatinine greater than or equal to 2 mg/dL (greater than or equal to 177 µmol/L) for adults or greater than or equal to twice the upper limit of normal for age. In patients with preexisting renal disease, a greater than twofold elevation over the baseline level.
- Coagulopathy: Platelets less than or equal to 100,000/mm3 (less than or equal to 100 x 106/L) or disseminated intravascular coagulation, defined by prolonged clotting times, low fibrinogen level, and the presence of fibrin degradation products.
- Liver involvement: Alanine aminotransferase, aspartate aminotransferase, or total bilirubin levels greater than or equal to twice the upper limit of normal for the patient’s age. In patients with preexisting liver disease, a greater than twofold increase over the baseline level.
- Acute respiratory distress syndrome: Defined by acute onset of diffuse pulmonary infiltrates and hypoxemia in the absence of cardiac failure or by evidence of diffuse capillary leak manifested by acute onset of generalized edema, or pleural or peritoneal effusions with hypoalbuminemia.
- A generalized erythematous macular rash that may desquamate.
- Soft-tissue necrosis, including necrotizing fasciitis or myositis, or gangrene.
Laboratory criteria for diagnosis: Isolation of group A Streptococcus.
Case classification:
- Probable: A case that meets the clinical case definition in the absence of another identified etiology for the illness and with isolation of group A Streptococcus from a nonsterile site.
- Confirmed: A case that meets the clinical case definition and with isolation of group A Streptococcus from a normally sterile site (e.g., blood or cerebrospinal fluid or, less commonly, joint, pleural, or pericardial fluid).
Treatment
Hospitalization is required. Standard treatment of shock and organ failure, such as fluid resuscitation, is imperative as the first step in treatment.
Antibiotic therapy is critical. Know your facility’s existing guidance for diagnosing and managing sepsis. If you suspect sepsis, start antibiotics as soon as possible, in addition to other therapies appropriate for the patient. Check patient progress frequently. Reassess antibiotic therapy within 24-48 hours to stop or change therapy as needed. Once STSS is confirmed, antibiotics can be tailored. Penicillin and clindamycin are used in conjunction as first-line antibiotic choices for STSS. For more specific recommendations on antibiotic therapy for STSS, please refer to Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases (7th ed.) and the Red Book.2,3
Removal of the source of infection, if possible, is important in the management of STSS, and surgical debridement of deep tissue infection may be necessary. The use of intravenous immunoglobulin has been used for severely ill patients early in the clinical course; however, more evidence is needed to determine the potential efficacy of this therapy.2,3
For recommendations on the diagnosis and management of sepsis, please refer to the Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock.4
Prognosis and complications
Despite aggressive treatment, the mortality rate for STSS ranges from 30% to 70%.5 Mortality from STSS is substantially lower in children than adults. Known complications of shock and organ failure can occur, including tissue necrosis and loss of extremities.
Prevention
Screening and antibiotic prophylaxis for household contacts of STSS patients is not recommended for household members under age 65 years, as the risk of secondary cases in these individuals is low.6 However, the risk of a secondary case in the 30 days following exposure to the index case is highest among household contacts who are 65 years of age or older, and thus, antibiotic chemoprophylaxis should be considered for household contacts aged ≥65 years old.7
View the latest CDC data on group A strep transmission in households.
The spread of group A strep can be reduced by standard infection control practices, including good hand hygiene and respiratory etiquette (e.g., covering your cough or sneeze).
Epidemiology
Streptococci have been implicated as a long-standing cause of invasive infection in immunocompromised individuals. However, in the 1980s, STSS was discovered to be affecting young, otherwise healthy individuals as well. The majority of cases are sporadic. CDC tracks invasive group A strep infections through the Active Bacterial Core surveillance (ABCs) program.
View ABCs data using Bact Facts Interactive.
- Stevens DL, Bryant AE. Severe group A streptococcoal infections. In Ferretti JJ, Stevens DL, Fischetti VA, editors. Streptococcus pyogenes: Basic biology to clinical manifestations. Oklahoma City (OK). University of Oklahoma Health Sciences Center. 2022.
- Bryant AE, Stevens DL. Streptococcus pyogenes. In Bennett J, Dolin R, Blaser M, editors. 8th Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases. Philadelphia (PA): Elsevier. 2015;2:2285–300.
- Committee on Infectious Diseases. Group A streptococcal infections. In Kimberlin DW, Barnett ED, Lynfield R, Sawyer MH, editors. 32nd ed. Red Book: 2021 Report of the Committee on Infectious Diseases. Elk Grove Village (IL). American Academy of Pediatrics. 2021:633–46.
- Rhodes A, Evans LE, Alhazzani W, et al. Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock: 2016. Crit Care Med. 2017;45(3):486–552.
- Nelson GE, Pondo T, Toews KA, et al. Epidemiology of invasive group A streptococcal infections in the United States, 2005–2012. Clin Infect Dis. 2016;63(4):478–86.
- Adebanjo T, Apostol M, Alden N, et al. Evaluating household transmission of invasive group A Streptococcus disease in the United States using population-based surveillance data, 2013–2016. Clin Infect Dis. 2020;70(7):1478–81.
- Prevention of Invasive Group A Streptococcal Infections Workshop Participants. Prevention of invasive group A streptococcal disease among household contacts of case patients and among postpartum and postsurgical patients: Recommendations from the Centers for Disease Control and Prevention. Clin Infect Dis. 2002;35(8):950–9. Erratum in: Clin Infect Dis. 2003;36(2):243.