Streptococcal Toxic Shock Syndrome: All You Need to Know

Streptococcal toxic shock syndrome (STSS) is a rare, but serious bacterial infection. STSS can develop very quickly into low blood pressure, multiple organ failure, and even death.
Group A strep bacteria cause STSS
Bacteria called group A Streptococcus (group A strep) can cause STSS when they spread into deep tissues and the bloodstream.
How you get STSS
For nearly half of people who get STSS, experts do not know how the bacteria got into the body. Sometimes the bacteria get into the body through openings in the skin, like an injury or surgical wound. The bacteria can also get into the body through mucus membranes, like the skin inside the nose and throat.
STSS is rarely contagious
It is very rare for someone with STSS to spread the infection to other people. However, any group A strep infection can turn into STSS and it is very easy to spread group A strep bacteria.
Illness gets worse soon after symptoms appear
STSS often begins with the following symptoms:
- Fever and chills
- Muscle aches
- Nausea and vomiting
After the first symptoms start, it usually only takes about 24 to 48 hours for low blood pressure to develop. Once this happens, STSS quickly gets much more serious:
- Hypotension (low blood pressure)
- Tachycardia (faster than normal heart rate)
- Tachypnea (rapid breathing)
- Organ failure (other signs that organs are not working)
- Examples: Someone with kidney failure may not make urine. Someone with liver failure may bleed or bruise a lot or their skin and eyes may turn yellow.
Seek medical attention immediately if you have signs or symptoms of STSS.
Some people are at increased risk
Anyone can get STSS, but there are some factors that can increase your risk of getting this infection.
Age
STSS is most common in adults 65 years old or older.
Infections or injuries that break the skin
People with an open wound are at increased risk for STSS. This can include people who recently had
- Surgery
- A viral infection that caused open sores (such as varicella that causes chickenpox and shingles)
Other health factors
People with diabetes or alcohol use disorder, previously known as alcohol dependence or alcoholism, are at increased risk for STSS.
Many tests, considerations help doctors diagnose STSS
There is no single test used to diagnose STSS. Instead, doctors may:
- Collect blood or other samples to test for group A strep infection
- Order tests to see how well different organs are working
Doctors diagnose STSS when they find group A strep bacteria in a patient who also has:
- Low blood pressure
- Problems with two or more of the following organs:
- Kidney
- Liver
- Lung
- Blood
- Skin
- Soft tissue (tissue beneath the skin and muscles)
STSS needs treatment in a hospital
Doctors treat STSS with antibiotics. People with STSS need care in a hospital. They often need fluids given through a vein and other treatments to help treat shock and organ failure. Many people with STSS also need surgery to remove infected tissue.
Serious complications are common
STSS often results in complications from organs shutting down and the body going into shock, including:
- Limbs removed through surgery
- Severe scarring from having infected tissues removed through surgery
Even with treatment, STSS can be deadly. Out of 10 people with STSS, as many as 3 people will die from the infection.
Prevent STSS
There are no vaccines to prevent group A strep infections, but there are things you can do to help protect yourself and others.
To help prevent group A step infections, you should:
- Clean and care for wounds
- Wash your hands often
- Take antibiotics, if prescribed
Clean and care for wounds

Wash hands often
Wash hands often with soap and water or use an alcohol-based hand rub if washing is not possible.
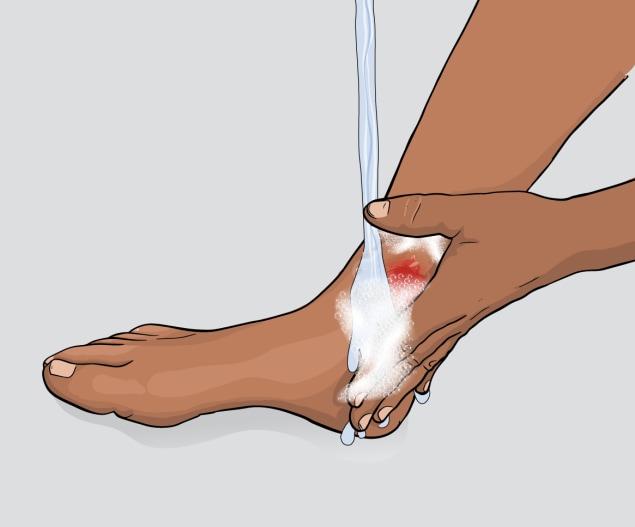
Clean wounds
Clean all minor cuts and injuries that break the skin (like blisters and scrapes) with soap and water.
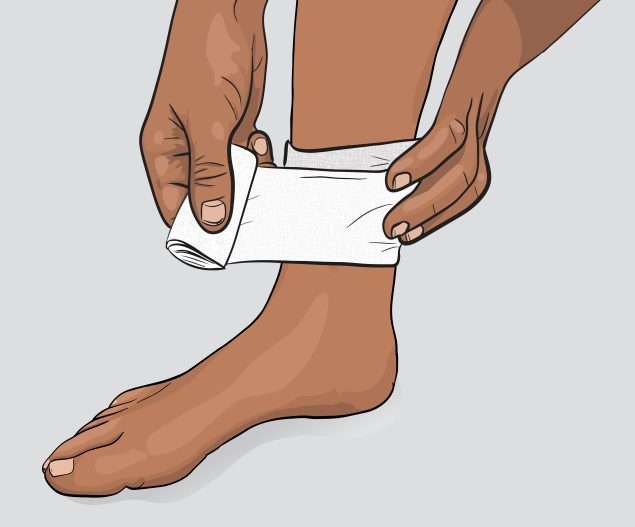
Bandage wounds
Clean and cover draining or open wounds with clean, dry bandages until they heal.
See a doctor
See a doctor for puncture and other deep or serious wounds.
If you have an open wound or skin infection, avoid spending time in:
- Hot tubs
- Swimming pools
- Natural bodies of water (e.g., lakes, rivers, oceans)
Wash hands often
The best way to keep from getting or spreading group A strep bacteria is to wash your hands often. This is especially important after coughing or sneezing and before preparing foods or eating.
You should also wash glasses, utensils, and plates after someone who is sick uses them. After they have been washed, these items are safe for others to use.
Take antibiotics, if prescribed
It is very rare for someone with STSS to spread the infection to other people. For this reason, doctors usually do not give preventive antibiotics to people who are under the age of 65 years and in close contact with someone with STSS. People who live together would be an example of close contacts. However, doctors may consider giving antibiotics to close contacts who are 65 years old or older and at higher risk of getting STSS.