Cellulitis: All You Need to Know
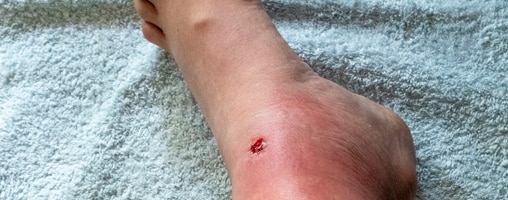
Cellulitis is a common bacterial skin infection that causes redness, swelling, and pain in the infected area of the skin. If untreated, it can spread and cause serious health problems.
Good wound care and hygiene are important for preventing cellulitis.
Many bacteria can cause cellulitis
Different types of bacteria can cause cellulitis, which is an infection of the deeper layers of the skin. This page focuses on one of the most common causes of cellulitis: group A Streptococcus (group A strep).
How you get cellulitis
For many people who get cellulitis, experts do not know how the bacteria get into the body. Sometimes the bacteria get into the body through openings in the skin, like an injury or surgical wound. In general, people cannot catch cellulitis from someone else; it is not contagious.
Symptoms often affect feet and legs
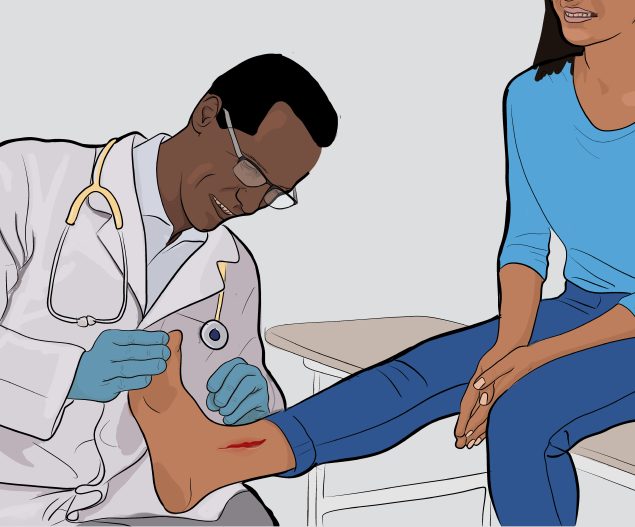
In general, cellulitis appears as a red, swollen, and painful area of skin that is warm and tender to the touch. The skin may look pitted, like the peel of an orange, or blisters may appear on the affected skin. Some people may also develop fever and chills. Cellulitis can appear anywhere on the body, but it is most common on the feet and legs.
Seek medical attention immediately if the red area of the skin spreads quickly or you develop a fever or chills.
Some people are at increased risk
Anyone can get cellulitis, but some factors can increase the risk of getting this infection.
Infections or injuries that break skin
The following are risk factors because they allow bacteria to get through the skin:
- Injuries that cause a break in the skin (like cuts, ulcers, bites, puncture wounds, tattoos, piercings)
- Chronic skin conditions (like athlete’s foot and eczema)
- Chickenpox and shingles
- Injection drug use
People who have had multiple cellulitis infections below the knee should be checked for fungal infections, such as athlete’s foot. These infections should be treated since they can cause breaks in the skin that can lead to cellulitis.
Other health factors
Other factors that increase someone’s risk for cellulitis include:
- Being overweight
- Having limbs (feet, legs, hands, and arms) that stay swollen (chronic edema), including swelling due to
- Lymphedema (problems with the lymphatic system so it does not drain the way it should); the lymphatic system is a part of the body’s immune system that helps move fluid that contains infection-fighting cells throughout the body
- Coronary artery bypass grafting (having a healthy vein removed from the leg and connected to the coronary artery to improve blood flow to the heart)
Doctors diagnose cellulitis by how it looks
Doctors typically diagnose cellulitis by looking at the affected skin during a physical examination. Blood or other lab tests are usually not needed.
Antibiotics are needed for treatment
Doctors treat cellulitis with antibiotics.
- Oral antibiotics (medicine taken by mouth) — Used to treat most cellulitis infections
- Intravenous (IV) antibiotics (medicine given directly into a vein) — Used to treat more serious infections
If the infection is in the arm or leg, then keeping that limb elevated can help decrease swelling and speed up recovery.
Complications are uncommon
Complications from cellulitis are uncommon but can include serious infections:
- Bacteremia (blood infection)
- Suppurative arthritis (bacterial infection in a joint)
- Osteomyelitis (bone infection)
- Endocarditis (swelling of the inner lining of the chambers of the heart and heart valves)
Cellulitis can cause thrombophlebitis (swelling in a vein due to a blood clot).
Prevent cellulitis
People can get cellulitis more than once. Having cellulitis does not protect someone from getting it again in the future. There are no vaccines to prevent group A strep infections, but there are things you can do to help protect yourself and others.
To help prevent group A strep infections, you should:
- Wash your hands often
- Clean and care for wounds
Wash hands often
The best way to keep from getting or spreading group A strep bacteria is to wash your hands often. This is especially important after coughing or sneezing and before preparing foods or eating.
Clean and care for wounds

Wash hands often
Wash hands often with soap and water or use an alcohol-based hand rub if washing is not possible.
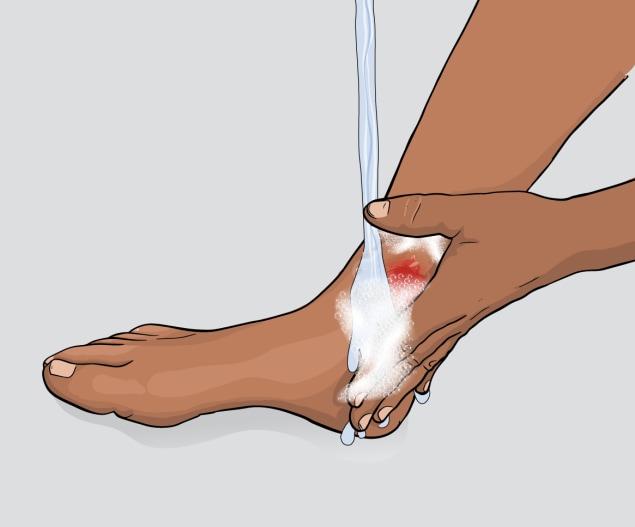
Clean wounds
Clean all minor cuts and injuries that break the skin (like blisters and scrapes) with soap and water.
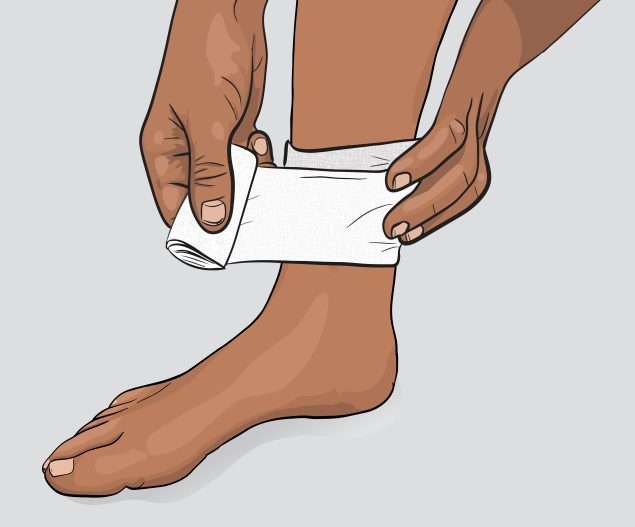
Bandage wounds
Clean and cover draining or open wounds with clean, dry bandages until they heal.
See a doctor
See a doctor for puncture and other deep or serious wounds.
If you have an open wound or skin infection, avoid spending time in:
- Hot tubs
- Swimming pools
- Natural bodies of water (e.g., lakes, rivers, oceans)
People with diabetes should check their feet daily, looking for injuries or signs of infection.