Information for Infection Preventionists
Candida auris: A drug-resistant fungus that spreads in healthcare facilities

Download and print this fact sheet [PDF - 2 pages].
A CDC message to infection preventionists
Candida auris is a fungus that causes serious infections and spreads in healthcare facilities. Infection preventionists, healthcare personnel, and laboratory staff can all help prevent it from spreading.
Why is Candida auris a problem?
- It causes serious infections. C. auris can cause bloodstream and other types of invasive infections, particularly in patients in hospitals and nursing homes who have many medical problems. More than 1 in 3 patients die within a month of being diagnosed with an invasive C. auris infection.
- It is often multidrug-resistant. Antifungal medications commonly used to treat other Candida infections often don’t work for C. auris. Some C. auris isolates are resistant to all three major classes of antifungal medications.
- It is becoming more common. Although C. auris was just discovered in 2009, the number of cases has grown quickly. Since 2009, it has been reported in dozens of countries, including the United States.
- It is difficult to identify. C. auris can be misidentified as other types of fungus unless specialized laboratory methods are used. Correctly identifying C. auris is critical for starting measures to stop its spread and prevent outbreaks.
- It can spread and cause outbreaks in healthcare facilities. Just like other multidrug-resistant organisms such as carbapenem-resistant Enterobacteriaceae (CRE) and methicillin-resistant Staphylococcus aureus (MRSA), C. auris can be transmitted in healthcare settings and cause outbreaks. It can colonize patients for many months, persist in the environment, and withstand some commonly used healthcare facility disinfectants.
Early detection and infection control can limit the spread of C. auris.
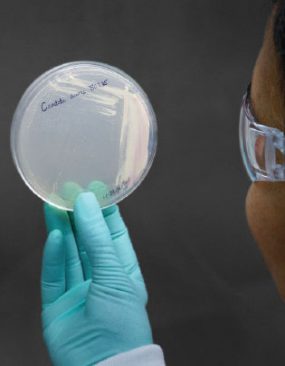
Prepare for C. auris in your facility
- Work with your laboratory to ensure the fungus identification method used in your facility can identify C. auris. If it cannot, know when to suspect C. auris and send suspected isolates to your state or local public health department for further identification.
- Begin surveillance. Establish a protocol with your laboratory so that your department is promptly informed when C. auris is suspected.
- If your laboratory is not equipped to identify C. auris, begin surveillance for the organisms that commonly represent a C. auris misidentification. See https://www.cdc.gov/fungal/candida-auris/identification.html for common misidentifications by different yeast identification methods.
- Know which patients are at higher risk for C. auris infection or asymptomatic colonization. These include:
- Patients who have received healthcare in post-acute care facilities (e.g., nursing homes), especially those with ventilator units.
- Patients recently hospitalized outside the United States, especially in countries with known C. auris cases (visit www.cdc.gov/fungal/candida-auris for a map of countries), and patients infected or colonized with carbapenemase-producing bacteria.
- Have a response plan. Discuss recommendations for infection prevention and control of C. auris with healthcare personnel, including environmental services.
What should I do if there is C. auris in my facility?
- Check the CDC website for the most up-to-date guidance on identifying and managing C. auris: www.cdc.gov/fungal/candida-auris.
- Report possible or confirmed C. auris test results immediately to your public health department.
- Ensure adherence to CDC recommendations for infection control, including
- Placing patients infected or colonized with C. auris on Transmission-Based Precautions and, whenever possible, in a single room.
- Making sure gown and gloves are accessible and used appropriately.
- Reinforcing hand hygiene.
- Coordinate with environmental services to monitor and ensure the patient care environment is cleaned using a disinfectant with an Environmental Protection Agency claim for C. auris or, if not available, for Clostridioides difficile. These products can be found at www.cdc.gov/fungal/candida-auris/c-auris-infection-control.html. Some disinfectants used in healthcare facilities (e.g., quaternary ammonium compounds [QACs]) may not be effective against C. auris, despite claims about effectiveness against C. albicans or other fungi. Work with the environmental services team to monitor the cleaning process.
- After consulting with public health personnel, screen contacts of case-patients to identify patients with C. auris colonization. Use the same infection control measures for patients found to be colonized.
- When a patient is being transferred from your facility (e.g., to a nursing home or other hospital), clearly communicate the patient’s C. auris status to receiving healthcare providers.
For more information, please contact the Centers for Disease Control and Prevention (CDC), National Center for Emerging and Zoonotic Infectious Diseases, Division of Foodborne, Waterborne, and Environmental Diseases
1600 Clifton Road, NE, Mail Stop H24-9, Atlanta, GA 30329-4018
Telephone: 800-CDC-INFO (232-4636) E-mail: cdcinfo@cdc.gov Web: https://www.cdc.gov/fungal/