At a glance
- Craniosynostosis (crane-eo-sin-ost-O-sis) is a birth defect in which the bones in a baby’s skull join too early.
- This happens before the brain forms fully and can slow the baby's brain growth.
- Researchers estimate that about 1 in every 2,500 babies has craniosynostosis in the United States.
What it is
Craniosynostosis is a condition where the bones in a baby's skull join together too early, before the brain forms fully. As the baby's brain grows, the skull can become misshapen.
The spaces between a baby's skull bones are filled with flexible material. These spaces, called sutures, allow the skull to grow as the baby's brain grows. Typically, around two years of age, the skull bones begin to join together as the sutures "close" and become bone.
When a suture closes, the baby’s head will stop growing in only that part of the skull. In other areas where sutures have not joined together, the baby's head will continue to grow. When that happens, the skull will have an abnormal shape, though the brain inside can grow to its usual size.
Sometimes more than one suture closes early. In these instances, the brain might not have enough room to grow. This can lead to a build-up of pressure inside the skull.
The severity of the craniosynostosis can cause additional problems, depending on:
- Which sutures closed early
- When the sutures closed (was it before or after birth and at what age)
- Whether or not the brain has room to grow
Sometimes, if the condition is not treated, the pressure in the baby's skull can lead to blindness, seizures, or brain damage.
Types
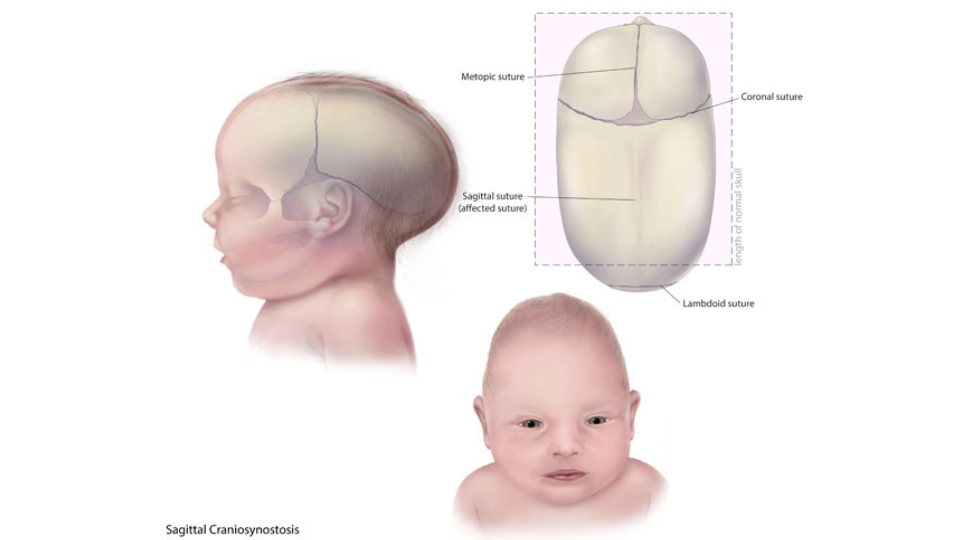
Sagittal synostosis
The sagittal suture runs along the top of the head, from front to back. When this suture closes too early, the baby’s head will grow long and narrow (scaphocephaly). It is the most common type of craniosynostosis.
Coronal synostosis
The right and left coronal sutures run from each ear to the sagittal suture at the top of the head. Early closure of these sutures may cause a flattened forehead on the side of the skull that closed early (anterior plagiocephaly). The baby's eye socket on that side might also be raised up and the nose could be pulled toward that side. This is the second most common type of craniosynostosis.
Bicoronal synostosis
This type of craniosynostosis occurs when the coronal sutures on both sides of the baby's head close too early. In this case, the baby's head will grow broad and short (brachycephaly).
Lambdoid synostosis
The lambdoid suture runs along the back of the head. If this suture closes too early, the baby’s head may be flattened on the back (posterior plagiocephaly).
Metopic synostosis
The metopic suture runs from the baby’s nose to the sagittal suture at the top of the head. If this suture closes too early, the top of the baby’s head may appear narrow in the front and broad in the back (trigonocephaly).
Risk factors
The causes of craniosynostosis in most infants are unknown. In some cases, craniosynostosis occurs because of an abnormality in a single gene. However, in most cases, craniosynostosis is thought to be caused by a combination of genes and other factors.
Research studies have also found some factors, like certain medications before or early in pregnancy1, might increase the risk of having a baby with craniosynostosis.
Diagnosis
Craniosynostosis usually is diagnosed soon after a baby is born.
Usually, the first sign of craniosynostosis is an abnormally shaped skull. Healthcare providers can identify craniosynostosis by feeling the baby's head for hard edges along the sutures and unusual soft spots. Other signs may include:
- No "soft spot" on the baby's skull
- Slow growth or no growth in the baby's head size over time
The provider also will look for any problems with the shape of the baby's face.
The healthcare provider will usually request tests to help confirm the diagnosis. For example, a CT or CAT scan (special x-ray test) can show the details of the skull and brain.
Treatment
Many types of craniosynostosis require surgery. The surgical procedure is meant to relieve pressure on the brain to allow it to grow properly. It is usually performed during the first year of life.
Babies with very mild craniosynostosis might not need surgery. Special medical helmets can be used to help mold the baby's skull. As the baby gets older and grows hair, the shape of the skull can become less noticeable.
Each baby born with craniosynostosis is different, and most babies with craniosynostosis are otherwise healthy. Some children, however, have developmental delays or intellectual disabilities.
A baby with craniosynostosis will need to see a doctor regularly to check that the brain and skull are developing properly.
Children with craniosynostosis may have issues with self-esteem if they are concerned with visible differences between themselves and other children. Parent-to-parent support groups can be useful for new families of babies with craniosynostosis.
Resources
The views of these organizations are their own and do not reflect the official position of CDC.
Children's Craniofacial Association (CCA): CCA addresses the medical, financial, psychosocial, and educational concerns relating to craniofacial conditions.
The National Craniofacial Association (FACES): FACES is dedicated to assisting children and adults who have craniofacial disorders resulting from disease, accident, or birth.
American Cleft Palate Craniofacial Association (ACPA): Care for children with craniofacial conditions is often best managed when a team of specialists works with the family to develop a treatment plan. ACPA is dedicated to team care and to optimizing outcomes for patients.
- Reefhuis J, Honein MA, Schieve LA, Rasmussen SA, and the National Birth Defects Prevention Study. Use of clomiphene citrate and birth defects, National Birth Defects Prevention Study, 1997–2005. Hum Reprod. 2011;26:451–457.
- Boulet SL, Rasmussen SA, Honein MA. A population-based study of craniosynostosis in metropolitan Atlanta, 1989-2003. Am J Med Genet Part A. 2008;146A:984–991
