Subjective Cognitive Decline — A Public Health Issue
Available for Download [PDF – 2 MB]
Subjective Cognitive Decline (SCD) is the self-reported experience of worsening or more frequent confusion or memory loss.1,2 It is a form of cognitive impairment and one of the earliest noticeable symptoms of Alzheimer’s disease and related dementias.2,3 SCD can have implications for living with and managing chronic disease, or performing everyday activities like cooking or cleaning.2 Because SCD is self-reported, it does not imply a diagnosis of cognitive decline by a health care professional.1,2
Cognition is a combination of processes in the brain that includes the ability to learn, remember, and make judgments.1 When cognition is impaired, it can have a profound impact on an individual’s overall health and well-being.1 Cognitive decline can range from mild cognitive impairment to dementia, a form of decline in abilities severe enough to interfere with daily life.1 Alzheimer’s disease is the most common form of dementia.1-3
Some cognitive decline can occur as adults age, but frequently forgetting how to perform routine tasks, for example, is not a normal part of aging and can affect a person’s ability to live and function independently. Some people with cognitive decline may be unable to care for themselves or perform activities of daily living, such as meal preparation, managing medical appointments, or managing their personal finances. Limitations in cognitive ability may impact a person’s ability to effectively manage medication regimens which can result in poor health outcomes of comorbid chronic diseases like heart disease or diabetes. By educating people about modifiable risk factors, encouraging early assessment and intervention, and understanding its impact on adults and their families, the health and well-being of many older adults may be improved.1,2
Subjective Cognitive Decline is self-reported confusion or memory problems that have been happening more often or getting worse in the past 12 months.4

Subjective Cognitive Decline is a Growing Public Health Issue
With the growing older adult population and the related increase in the need for health and social services, the public health community is challenged to be proactive. By acting quickly
and strategically to stimulate needed changes to systems and environments, public health professionals can work to mitigate future impacts of SCD as well as Alzheimer’s disease and related dementias on the health and wellness of the public. This is particularly important as these issues can impact not only older adults but also their family and friends who act as caregivers.
This brief examines the following questions:
- What percentage of adults live with SCD?
- What percentage of adults with SCD live alone?
- What percentage of adults with SCD have discussed their memory loss or confusion with a health care professional?
- What percentage of adults with SCD experience coronary heart disease (including angina and myocardial infarction) or strokes?
- What percentage of adults with SCD also have other chronic diseases?
- What percentage of adults with SCD also report issues with their mental health?
- What percentage of adults with SCD have difficulty with everyday activities, like cooking, cleaning, or with work or volunteering?
SCD data presented in this brief were collected from communitydwelling adults aged 45 years and older in 2015-2017 through the Behavioral Risk Factor Surveillance System (BRFSS).4
Questions related to SCD were administered as part of the BRFSS in 49 states, the District of Columbia and Puerto Rico. For states administering the module during multiple years, and the most recent data were used for this brief. Additional results for these data were previously published.5 Additional data reports can be generated and viewed at the CDC Alzheimer’s Disease and Healthy Aging Data Portal.
These data were examined in two age groups, adults 45-64 years and 65 years of age and older, as well as by sex, race, Hispanic ethnicity, chronic disease status, and other demographic characteristics.
By acting quickly and strategically to stimulate needed changes to systems and environments, public health professionals can work to mitigate future impacts of SCD as well as Alzheimer’s disease and related dementias on the health and wellness of the public.

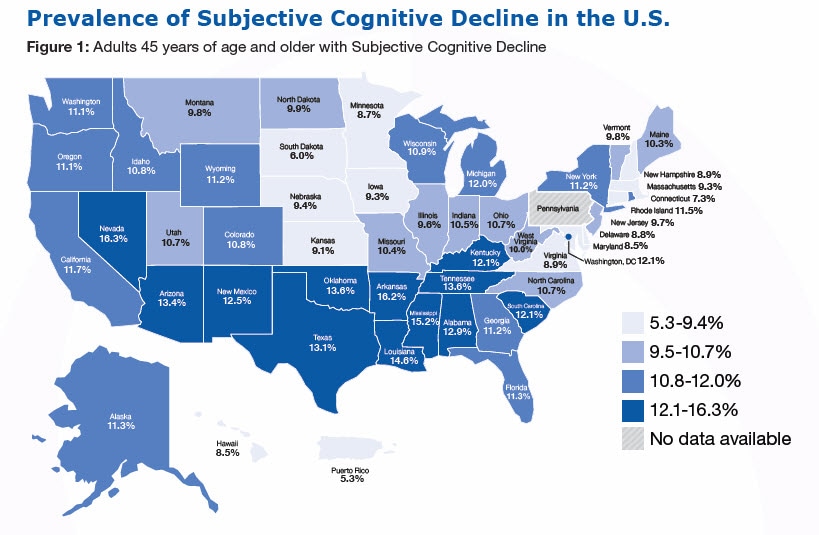
During the past 12 months, have you experienced confusion or memory loss that is happening more often or is getting worse?

- The prevalence of subjective cognitive decline (SCD) is 11.1%, or 1 in 9 adults.
- The prevalence of SCD among adults aged 65 years and older is 11.7% compared to 10.8% among adults 45-64 years of age.
- The prevalence of SCD is 11.3% among men compared to 10.6% among women.
- The prevalence of SCD differs among racial/ethnic groups, 10.9% of Whites report SCD compared to 12.8% of Blacks/African Americans, 11.0% of Hispanics, and 6.7% of Asians and Pacific Islanders.
- Lower prevalence of SCD is reported in adults with more years of formal education.
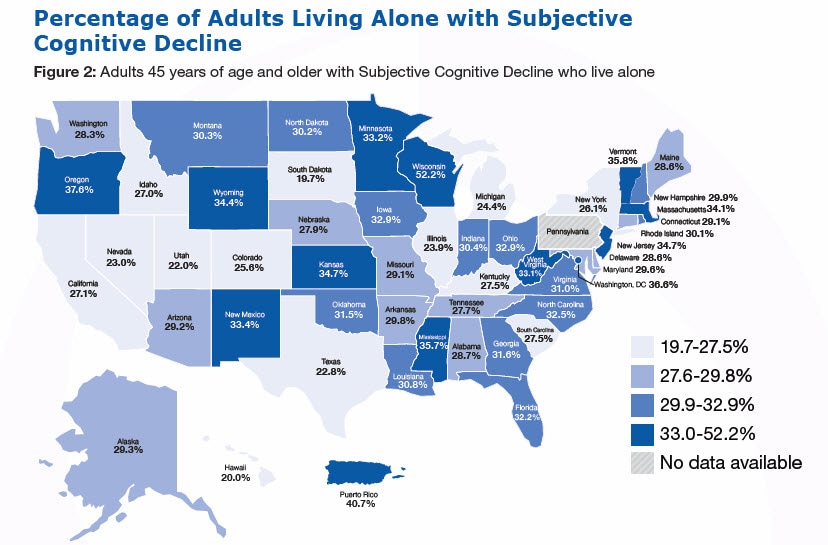
How many adults aged 18 and older live in your household? How many children less than 18 years of age live in your household?

Older adults who live alone can be at risk for poor health outcomes, are less likely to use health services, and are more vulnerable to self-neglect and fall-related injuries than those living with others.6,7 Older adults who live alone report more unmet needs such as managing money, medications, mobility, and some activities of daily living.6,7
- Of adults with SCD, 29.3% live alone.
- Among persons reporting SCD aged 45-64 years, 24.7% live alone compared to 36.2% of those aged 65 years and older.
- 30.3% of women with SCD live alone compared to 28.1% of men.
- The prevalence of living alone among adults with SCD differs among racial/ethnic groups. Of those with SCD, 30.4% of Whites live alone compared to 35.5% of Blacks/African Americans, 18.3% of Hispanics, and 15.3% of Asians and Pacific Islanders.
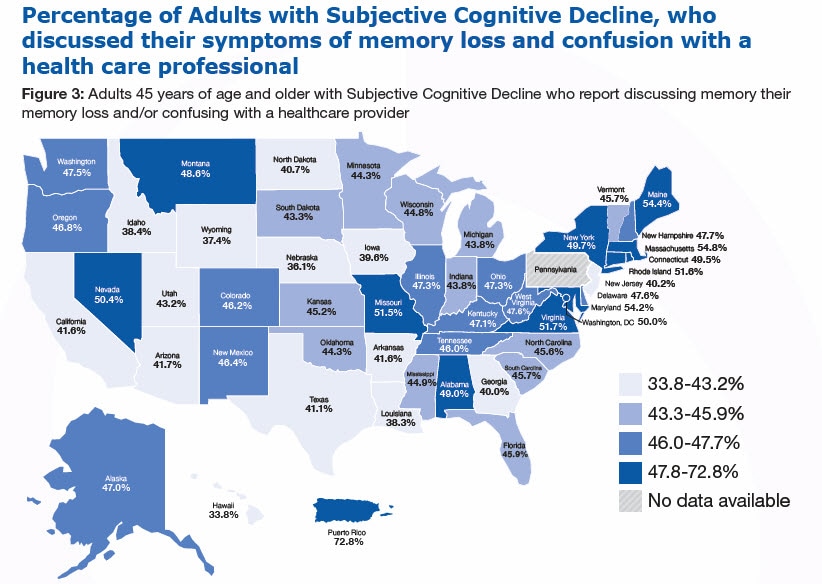
Have you or anyone else discussed your confusion or memory loss with a health care professional?
Researchers have found that few adults with SCD discussed their confusion or memory loss with a health care professional.7-9 In fact, the prevalence of cognitive decline identified in community surveys is over twice that reported in medical records of general practitioners.8,9 Opportunities for improvement exist for increased screening, diagnosis, and identification of treatable cause(s).9
- Less than half of adults with SCD (45.3% of adults aged 45 years and older) reported discussing symptoms of confusion or memory loss with a health care professional.
- Among persons reporting SCD, 48.8% of those aged 45 to 64 years reported discussing their memory loss or confusion with a health care professional compared to 39.8% of persons aged 65 years and older.
- Half (50.5%) of women reported discussing SCD with a health care professional compared to 39.2% of men.
- The percentage of those who discussed SCD with a health care professional varies by race and ethnicity. Among Whites, 46.0% reported discussing SCD with a health care professional compared to 45.3% of Blacks/African Americans, 40.2% of Hispanics and 34.1% of Asians and Pacific Islanders.
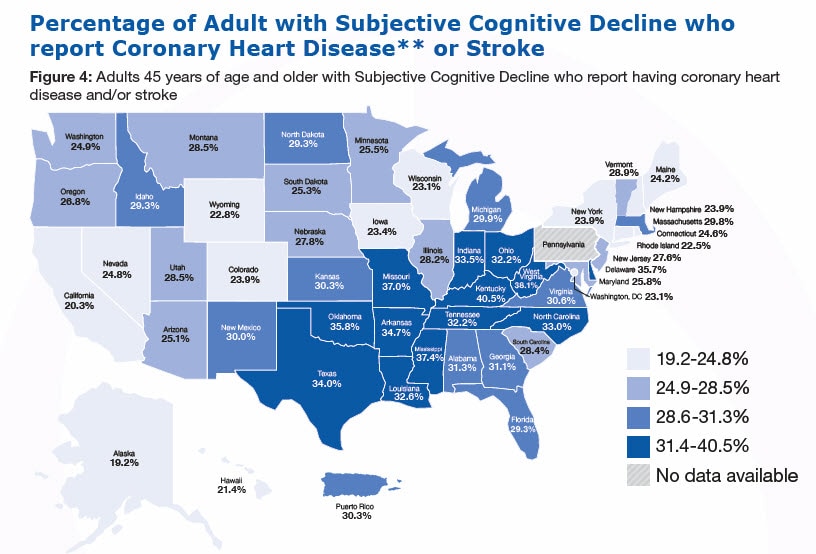
Has a doctor, nurse or other health professional ever told you that you had one of the following: Coronary heart disease (including angina and/or myocardial infarction)? Has a doctor, nurse or other health professional ever told you that you a stroke?

Coronary heart disease can lead to decreased cognitive function that can impact effective chronic disease self-management.10-13 Cognitive impairment in areas of learning, memory, and decision-making can increase the need for assistance in self-management, such as help with medication management or scheduling medical appointments.10-13
- More than 1 in 4 (28.6%) adults with SCD reported having coronary heart disease or stroke.
- Among adults with SCD, 23.9% of adults aged 45-64 years report having coronary heart disease or stroke, compared to 35.9% of adults aged 65 years and older.
- One in four (26.3%) women with SCD reported having coronary heart disease or stroke, compared to nearly one-third (31.3%) of men.
- The prevalence of CHD among adults with SCD is 25.7% in adults who completed at least some post high school education or higher compared to 31.7% among adults with a high school degree and 31.0% among adults with less than a high school degree.
** Respondents were classified as having coronary heart disease if they reported experiencing a heart attack (i.e., myocardial infarction) or angina
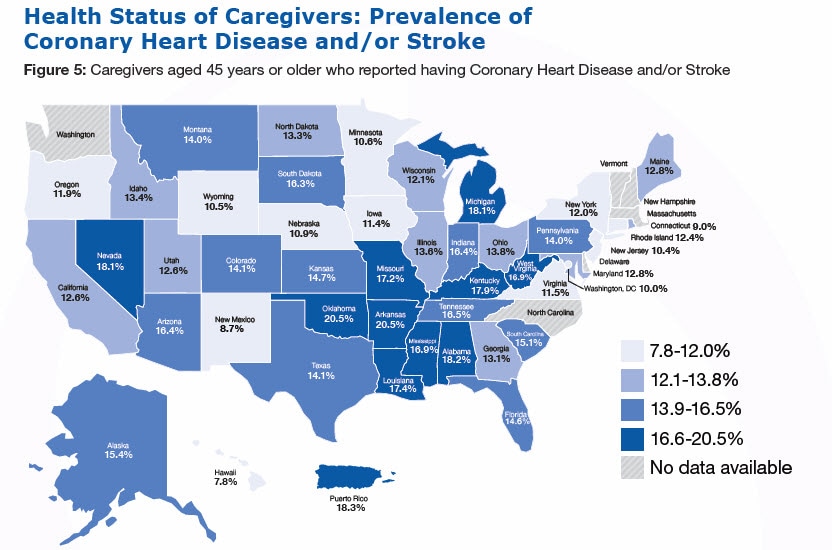
Has a doctor, nurse or other health professional ever told you that you had one of the following: Coronary heart disease (including angina and/or myocardial infarction), stroke, asthma (still have), cancer (skin, other types of cancer), COPD, arthritis, depressive disorder, kidney disease, diabetes?
Multiple chronic diseases (two or more) have been found to be associated with increased cognitive decline.12-14 As the number of chronic diseases increases, the management of these conditions becomes increasingly complex, which may lead to a greater need for assistance. The presence of chronic diseases includes the report of at least one of the following: heart attack, coronary heart disease, stroke, asthma, cancer, arthritis, or diabetes.
- More than two-thirds (66.2%) of adults with SCD and have two or more chronic diseases.
- More than two-thirds (69.1%) of adults 65 years of age and older have both SCD and two or more chronic diseases, compared to 64.3% of adults 45-64 years of age.
- With respect to sex, 70.7% of women report SCD and having 2 or more chronic diseases compared to 61.2% of men.
Subjective Cognitive Decline and Frequent Mental Distress
Mental distress includes stress, depression and problems with emotions.15 Frequent mental distress (FMD) is defined as experiencing mental distress or having mentally unhealthy days for at least 14 days in a 30 day period.15
About how many days during the past 30 days was your mental health not good? (14 or more days = frequent mental distress)
- One third (33.7%) of adults with SCD report FMD.
- One in five (20.9%) adults 65 years of age and older with SCD reported FMD compared to 42.0% of adults 45-64 years of age.
- 37.6% of women with SCD reported FMD compared to 29.4% of men.
Subjective Cognitive Decline—related Functional Difficulties
SCD can impact people’s lives in ways that extend beyond thinking and remembering. It may interfere with a person’s ability to engage in activities they typically perform, like chores, socializing, taking medications, or working outside the home. An SCD-related functional difficulty is defined as always, usually, or sometimes giving up day-to-day household activities or chores and/or experiencing interference in engaging in activities outside the home.16
During the past 12 months, as a result of confusion or memory loss, how often have you given up day-to-day household activities or chores you used to do, such as cooking, cleaning, taking medications, driving, or paying bills?
During the past 12 months, how often has confusion or memory loss interfered with your ability to work, volunteer, or engage in social activities outside the home.
- Half (50.6%) of adults with SCD experienced SCD-related functional difficulties.
- SCD-related functional difficulties were more common among middle-aged adults (45-64 years of age; 58.7%) than among older adults (age 65 and older; 38.0%).
- More than half (53.4%) of women aged 45 years and older reported SCD related functional difficulties compared to 47.3% of men.

Call to Action
Subjective Cognitive Decline (SCD) is a public health issue and public health has a role in alleviating its impact. Below are some of the actions that can be taken to improve the health and well-being of persons with SCD. For additional actions, refer to The Healthy Brain Initiative: State and Local Public Health Partnerships to Address Dementias, The 2018-2023 Road Map.17
- Educate the public and health care professionals about brain health and the burden of SCD.
- Increase awareness that dementia, such as Alzheimer’s disease, is not a normal part of aging.
- Raise awareness about the best available evidence on dementia (including detection) and dementia caregiving, including risk reduction.
- Use this report and other analyses to make informed decisions and policies and promote the role of public health in addressing SCD as a priority.
- Increase awareness about the importance of managing chronic diseases, including conditions associated with coronary heart disease or stroke, among people with SCD and at all stages of dementia.
- Encourage patients and health care professionals to discuss SCD during routine medical office visits.
Technical Information
The Behavioral Risk Factor Surveillance System (BRFSS) is the nation’s premier system of health-related telephone surveys that collect state data about U.S. residents regarding their health-related risk behaviors, chronic health conditions, and use of preventive services. Established in 1984 with 15 states, BRFSS now collects data in all 50 states as well as the District of Columbia and three U.S. territories. BRFSS completes more than 450,000 adult interviews each year, making it the largest and longest continuously conducted health survey system in the world.
CDC’s Behavioral Risk Factor Surveillance System (BRFSS) helps states survey U.S. adults regarding a wide range of health issues and behaviors that affect their health. The crucial information gathered through this state-based telephone surveillance system is used by national, state, and local public health agencies to identify populations that might be most at risk and to monitor the need for and the effectiveness of various public health interventions.
Although the BRFSS is a useful tool for assessing cognitive decline in the older adult population, it has some limitations: it excludes people who do not have telephones or are in institutions such as nursing homes; it may under-represent people who are severely impaired because of the functional capacity required to participate in the survey; and responses to BRFSS are self-reported and therefore have not been confirmed by a healthcare provider. Despite these limitations, the BRFSS is a uniquely powerful tool to provide the prevalence of cognitive decline and related health issues among older community-dwelling U.S. adults, due to its large sample size and proven reliability and validity.
The BRFSS is administered and supported by the Division of Population Health, National Center for Chronic Disease Prevention and Health Promotion, CDC. For more information, please visit https://www.cdc.gov/brfss.
Footnotes
- https://www.cdc.gov/aging/healthybrain/. Accessed 01/2017.
- Jessen F, Amarigliod RE, et.al, Subjective Cognitive Decline Initiative (SCD-I) Working Group, A conceptual framework for research on subjective cognitive decline in preclinical Alzheimer’s disease, Alzheimers Dement. 2014 November; 10(6): 844–852.
- Alzheimer’s Association. 2018 Facts and Figures. Alzheimers Dement 2018;14(3):367-429.
- Behavioral Risk Factor Surveillance System, Centers of Disease Control and Prevention 2015- 2016.
- Taylor CA, Bouldin ED, McGuire LC (2018). Subjective Cognitive Decline Among Adults Aged ≥45 Years — United States, 2015–2016. MMWR Morb Mortal Wkly Rep, 67(27): 753–757.
- Gibson AK, Richardson VE. Living Alone With Cognitive Impairment. Am J Alzheimers Dis Other Demen. 2017 Feb;32(1):56-62
- Portacolone E, Johnson JK, et.al. The Effects and Meanings of Receiving a Diagnosis of Mild Cognitive Impairment or Alzheimer’s Disease When One Lives Alone. J Alzheimer’s Disease 61 (2018) 1517–1529.
- Buckley BF, Salingab MM, et.al., Subjective Cognitive Decline from a Phenomenological Perspective: A Review of the Qualitative Literature, J Alzheimer’s Disease 48(2015) S125–S140
- Waldorff FB, et.al. If you don’t ask (about memory), they probably won’t tell. J Fam Pract. 2008 Jan;57(1):41-4.
- Haring, et.ad. Cardiovascular Disease and Cognitive Decline in Postmenopausal Women: Results From the Women’s Health Initiative Memory Study. J Am Heart Assoc. 2013 Dec; 2(6):
- Lutski M et.al. Cardiovascular Health and Cognitive Decline 2 Decades Later in Men with Preexisting Coronary Artery Disease. Am J Cardiol. 2018 Feb 15;121(4):410-415.
- Chen LY et.al. Association of Atrial Fibrillation With Cognitive Decline and Dementia Over 20 Years: The ARIC-NCS (Atherosclerosis Risk in Communities Neurocognitive Study) J Am Heart Assoc. 2018;7
- Ormel J, Kempen GI , Functioning, well-being, and health perception in late middle-aged and older people: the effects of depressive symptoms and chronic medical conditions, J Am Geriatr Soc. 1998 Jan;46(1):39-48.
- Baird C, Lovell J, et.al. The impact of cognitive impairment on self-management in chronic obstructive pulmonary disease: A systematic review, Respir Med. 2017 Aug;129:130-139.
- Self-Reported Frequent Mental Distress Among Adults — United States, 1993-1996, MMWR May 01, 1998 / 47(16);325-331.
- Anderson L, et.al. Demographic and Health Status Differences Among People Aged 45 or Older With and Without Functional Difficulties Related to Increased Confusion or Memory Loss, 2011 Behavioral Risk Factor Surveillance. Prev Chronic Dis 2015;12:140429
- https://www.cdc.gov/aging/healthybrain/roadmap.htm 2018.
Disclaimer: The mark “CDC” is owned by the U.S. Department of Health and Human Services (HHS) and is used with permission. Use of this logo is not an endorsement by HHS or the Centers for Disease Control and Prevention (CDC) or any particular product, service, or enterprise.