Acute Flaccid Myelitis (AFM)




On average, CDC received reports of suspected AFM cases 18 days after patient’s limb weakness began.
Overview
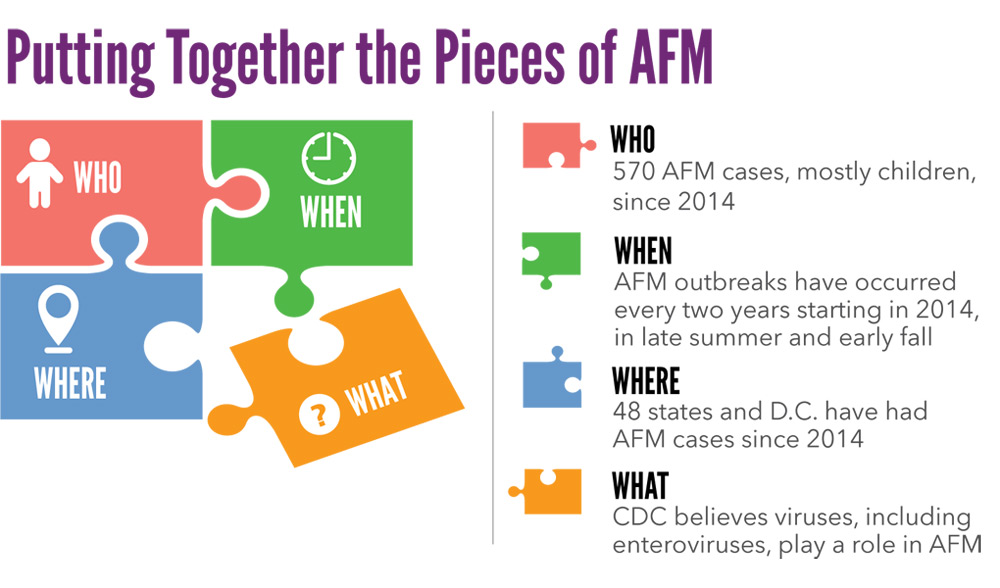
Acute flaccid myelitis (AFM) is a rare but serious syndrome (a pattern of symptoms) that causes limb weakness, mostly in children. Three national outbreaks have occurred starting in 2014, when CDC began surveillance for AFM.
- Most patients developed AFM in late summer or early fall.
- Most patients had respiratory symptoms or fever consistent with a viral infection less than a week before onset of limb weakness.
- CDC believes viruses, including enteroviruses, play a role in AFM.
- Currently, there are no proven ways to treat or prevent AFM.
- Prompt symptom recognition, specimen collection, and reporting to CDC are all critical to improve understanding of this complex syndrome, including its risk factors, outcomes, possible treatments, and ways to prevent it.
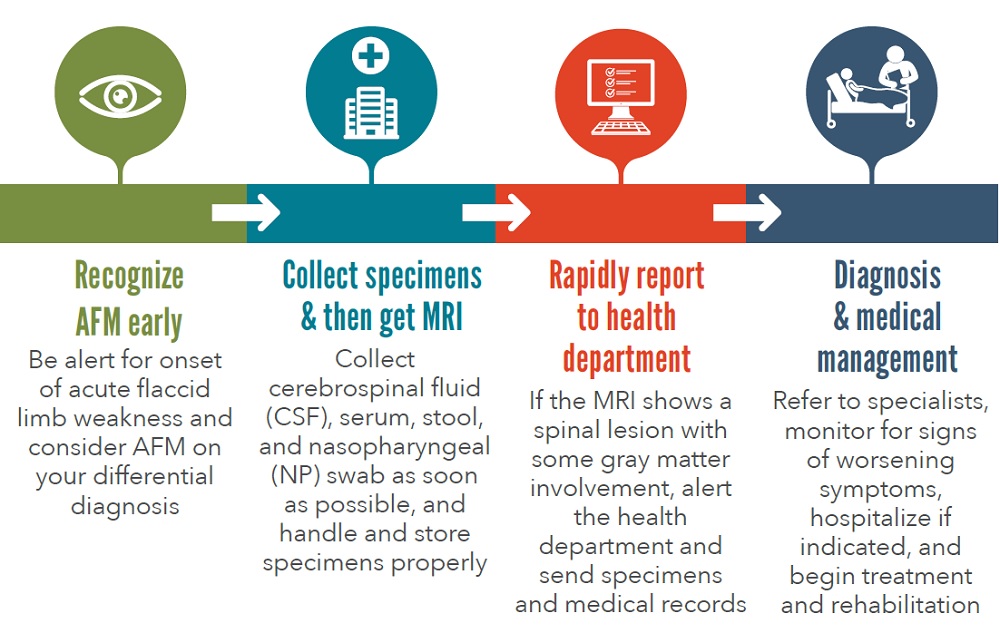
Clinicians: Timing is Key for AFM
Putting Together the Pieces of AFM
Recognizing AFM is challenging.
- AFM is rare, and there is no lab test available yet to diagnose patients.
- When clinicians recognize AFM early, they can quickly:
- Get patients the best care, including treatment and rehabilitation.
- Collect lab specimens like blood or urine to better understand AFM and its causes.
- Report suspected cases for prompt investigation and outbreak detection.
CDC Is:
- Monitoring AFM trends and the clinical presentation.
- Researching possible risk factors.
- Conducting advanced lab testing and research to understand how viral infections may lead to AFM.
- Tracking long-term patient outcomes.
Clinicians Can:
- Contact neurologists specializing in AFM through the AFM Physician Consult and Support Portal for help with patient diagnosis and medical management. https://wearesrna.org/living-with-myelitis/resources/afm-physician-support-portal/
- Contact CDC with any questions about AFM, including how to report cases and collect appropriate specimens.
Health Departments Can:
- Work with CDC to collect medical information, MRI images, and specimens, and classify cases.
- Communicate information about AFM to clinicians and the public.
Parents Can:
- Immediately seek medical care if their child develops sudden arm or leg weakness.

Clinicians should:
- Strongly suspect AFM in patients with acute flaccid limb weakness, especially after respiratory illness or fever, and between August and October.
- Hospitalize patients immediately, collect lab specimens, diagnose, and begin medical management.
- Don’t wait for CDC’s case classification for diagnosis.
- Alert the health department and send lab specimens and medical records.
Related Pages and Resources
- Vital Signs: Press Release — Los CDC instan a los médicos a reconocer y notificar rápidamente los casos de mielitis flácida aguda [Spanish]
- Vital Signs: Surveillance for Acute Flaccid Myelitis — United States, 2018
- AFM Cases and Outbreaks
- For Clinicians and Health Departments
- Specimens to collect and send to CDC
- Job aid on how to send information to the health department about a patient under investigation (PUI) for AFM [444 KB, 2 pages]
Science Behind the Issue
For More Information
1-800-CDC-INFO (232-4636)
TTY: 1-888-232-6348
Web: www.cdc.gov
Centers for Disease Control and Prevention
1600 Clifton Road NE
Atlanta, GA 30333
Publication date: July 9, 2019