Rocky Mountain Spotted Fever (RMSF)
- Home
- Tick ID
- Overview of Tickborne Diseases
- Lyme Disease
- Tickborne Relapsing Fever (TBRF)
- Hard Tick Relapsing Fever
- Anaplasmosis
- Ehrlichiosis
- Rocky Mountain Spotted Fever
- Rickettsia parkeri Rickettsiosis
- Tularemia
- Babesiosis
- Heartland and Bourbon Virus Diseases
- Colorado Tick Fever
- Powassan Virus Disease
- Tickborne Diseases Abroad
- Tick Bites/Prevention
- Lyme Disease Prophylaxis After Tick Bite
Agent
Rickettsia rickettsii
RMSF is most often transmitted by the American dog tick in the Eastern, Central and Western United States; by the Rocky Mountain wood tick in the Rocky Mountain states; and by the brown dog tick in the Southwestern United States, along the U.S.-Mexico border. RMSF can be rapidly fatal if not treated within the first 5 days of symptoms. Before tetracycline antibiotics were available, case fatality rates ranged from 20–80%.
Where Found
Since 2010, cases of RMSF are reported as spotted fever rickettsiosis along with other spotted fevers like Rickettsia parkeri rickettsiosis in national surveillance. RMSF has become increasingly common in certain areas of Arizona over the last several years; between 2002-2021 more than 500 cases and 28 fatalities occurred.
Incubation Period
3–12 days
Signs and Symptoms
Early (1–4 Days)
- High fever
- Severe headache
- Malaise
- Myalgia
- Edema around eyes and on the back of hands
- Gastrointestinal symptoms (nausea, vomiting, anorexia)
Late (5 Days and Beyond)
- Altered mental status, coma, cerebral edema
- Respiratory compromise (pulmonary edema, ARDS)
- Necrosis, requiring amputation
- Multiorgan system damage (CNS, renal failure)
Rash
- Typically appears 2–5 days after onset of symptoms; approximately 10% of RMSF patients never develop a rash.
- Decision to treat should not be based on presence of rash.
Early Rash
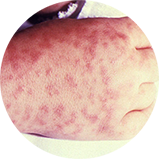
- Maculopapular: Small, flat, pink, non-itchy spots (macules) initially appear on the wrists, forearms, and ankles then spread to the trunk and sometimes palms and soles.
Late Rash
- Petechial: Red to purple spots (petechiae) are usually not seen until day 6 or later after onset of symptoms.
- Petechial rash is considered a sign of progression to severe disease. Every attempt should be made to begin treatment before petechiae develop.

Confirmation of the diagnosis is based on laboratory testing, but antibiotic therapy should not be delayed in a patient with a suggestive clinical presentation. Antibiotics are more likely to prevent fatal outcome from RMSF if started within the first 5 days of symptoms.
General Laboratory Findings
- Thrombocytopenia
- Elevated hepatic transaminases
- Hyponatremia
NOTE: Laboratory values are often within normal limits in early illness.
Laboratory Diagnosis
- Demonstration of a four-fold rise in IgG-specific antibody titer by indirect immunofluorescence antibody (IFA) assay in paired serum samples. The first sample should be taken within the first 2 weeks of illness and the second should be taken 2 to 4 weeks later.
- Detection of DNA in a skin biopsy specimen of a rash lesion by PCR assay or in an acute phase whole blood specimen. Additionally, new pan-Rickettsia and R. rickettsii-specific PCR assays are available at some local and state health departments.
- Immunohistochemical (IHC) staining of organism from skin or tissue biopsy specimen.
NOTE: Antibody titers are frequently negative in the first 7–10 days of illness. Acute antibody results cannot be independently relied upon for confirmation
NOTE: IgM antibodies are less specific than IgG antibodies and are more likely to generate false positives. IgM results alone should not be used for laboratory diagnosis.
Treatment
Anaplasmosis, ehrlichiosis, and spotted fever group rickettsioses are treated with doxycycline. Clinical suspicion of any of these diseases is sufficient to begin treatment. Delay in treatment may result in severe illness and even death. These regimens may need to be adjusted depending on a person’s age, medical history, underlying health conditions, pregnancy status, or allergies. Consult an infectious disease specialist in cases of pregnancy or life-threatening allergy to doxycycline.
| Age Category | Drug | Dosage | Maximum | Duration (Days) |
|---|---|---|---|---|
| Adults | Doxycycline | 100 mg twice per day, orally or IV | 100 mg/dose | Patients should be treated for at least 3 days after the fever subsides and until there is evidence of clinical improvement. Minimum course of treatment is 5-7 days. |
| Children weighing <100 lbs. (45.4 kg) | Doxycycline | 2.2 mg/kg per dose twice per day, orally or IV | 100 mg/dose |
NOTE: Use doxycycline as the first-line treatment for suspected RMSF in patients of all ages. The use of doxycycline to treat suspected RMSF in children is recommended by both the CDC and the American Academy of Pediatrics Committee on Infectious Diseases. Use of antibiotics other than doxycycline increases the risk of patient death. At the recommended dose and duration needed to treat RMSF, no evidence has been shown to cause staining of permanent teeth, even when multiple courses are given before the age of eight.
References
Centers for Disease Control and Prevention. Diagnosis and management of tickborne rickettsial diseases: Rocky Mountain spotted fever and other spotted fever group rickettsioses, ehrlichioses, and anaplasmosis—United States: a practical guide for health care and public health professionals. MMWR 2016;65 (No.RR-2).
Demma LJ, Traeger MS, Nicholson WL, et al. Rocky Mountain spotted fever from an unexpected tick vector in Arizona. N Engl J Med 2005;353:587–94.
Elghetany MT, Walker DH. Hemostatic changes in Rocky Mountain spotted fever and Mediterranean spotted fever. Am J Clin Pathol 1999;112:159–68.
Holman RC, Paddock CD, Curns AT, et al. Analysis of risk factors for fatal Rocky Mountain spotted fever: evidence for superiority of tetracyclines for therapy. J Infect Dis 2001;184:1437–44.
Jay R, Armstrong PA. Clinical characteristics of Rocky Mountain spotted fever in the United States: A literature review. J Vector Borne Dis. 2020 Apr-Jun;57(2):114-120.
Kirkland KB, Wilkinson WE, Sexton DJ. Therapeutic delay and mortality in cases of Rocky Mountain spotted fever. Clin Infect Dis 1995;20:1118–21.
Massey EW, Thames T, Coffey CE, et al. Neurologic complications of Rocky Mountain spotted fever. South Med J 1985;78:1288–90, 1303.
McQuiston JH, Wiedeman C, Singleton J, et al. Inadequacy of IgM antibody tests for diagnosis of Rocky Mountain Spotted Fever. Am J Trop Med Hyg. 2014 Oct;91(4):767-70.
Paddock CD, Alvarez-Herandez G. Rickettsia rickettsii (Rocky Mountain spotted fever). In: Principles and Practice of Pediatric Infectious Diseases. 5th ed. Philadelphia, PA: Elsevier; 2017. p. 952-957.
Regan JJ, Traeger MS, Humpherys D, et al. Risk factors for fatal outcome from Rocky Mountain spotted fever in a highly endemic area—Arizona, 2002–2011. Clin Infect Dis 2015;60:1659–66.
Smithee L, et al. Public health reporting and national notification for spotted fever rickettsiosis (including Rocky Mountain spotted fever). Council of State and Territorial Epidemiologists, Infectious Diseases Committee, 2009 Position Statement. [PDF – 11 pages]
Todd SR, Dahlgren FS, et al. No visible dental staining in children treated with doxycycline for suspected Rocky Mountain spotted fever. J Pediatr 2015;166(5):1246-51
Traeger MS, Regan JJ, Humpherys D, et al. Rocky Mountain spotted fever characterization and comparison to similar illnesses in a highly endemic area—Arizona, 2002–2011. Clin Infect Dis 2015;60:1650–8.