Inpatient Hospitalization Costs Associated with Birth Defects Among Persons Aged <65 Years — United States, 2019
Weekly / July 7, 2023 / 72(27);739–745
Justin Swanson, MPH1; Elizabeth C. Ailes, PhD2; Janet D. Cragan, MD2; Scott D. Grosse, PhD3; Jean Paul Tanner, PhD1; Russell S. Kirby, PhD1; Norman J. Waitzman, PhD4; Jennita Reefhuis, PhD2; Jason L. Salemi, PhD1 (View author affiliations)
View suggested citationSummary
What is already known about this topic?
Estimates of birth defect–associated hospitalization costs must be updated as detection, diagnosis, and treatment evolve for numerous birth defects.
What is added by this report?
During 2019, among patients aged <65 years, 4.1% of all hospitalizations and 7.7% of related inpatient medical costs were associated with birth defects. The total estimated cost of birth defect–associated hospitalizations was $22.2 billion.
What are the implications for public health practice?
These updated estimates of hospitalization costs illustrate the importance of continually determining the health care needs of persons with birth defects to ensure optimal health for all.
Altmetric:
Abstract
Changing treatments and medical costs necessitate updates to hospitalization cost estimates for birth defects. The 2019 National Inpatient Sample was used to estimate the service delivery costs of hospitalizations among patients aged <65 years for whom one or more birth defects were documented as discharge diagnoses. In 2019, the estimated cost of these birth defect–associated hospitalizations in the United States was $22.2 billion. Birth defect–associated hospitalizations bore disproportionately high costs, constituting 4.1% of all hospitalizations among persons aged <65 years and 7.7% of related inpatient medical costs. Updating estimates of hospitalization costs provides information about health care resource use associated with birth defects and the financial impact of birth defects across the life span and illustrates the need to determine the continued health care needs of persons born with birth defects to ensure optimal health for all.
Introduction
In the United States, major structural birth defects attributable to genetic, chromosomal, teratogenic, or unknown etiologies affect approximately 3% of live births (1) and are the leading cause of infant mortality, responsible for 21% of newborn and infant deaths (2). Their treatments incur significant financial costs throughout a person’s lifetime. As treatments and medical costs change, updates to hospitalization cost estimates for birth defects are needed.
Methods
Developed for the Healthcare Cost and Utilization Project (HCUP), the National Inpatient Sample (NIS) is the largest publicly available, all-payor inpatient care database in the United States.* NIS uses a 20% systematic sampling of all discharges from short-term, nonfederal community hospitals. Because NIS does not identify patients across multiple hospital visits, the unit of analysis for this study is individual hospitalization rather than individual patient. To reduce the impact of potential miscoding of age-related abnormalities as birth defects (particularly cardiovascular defects) (3), only patients aged <65 years discharged during January 1–December 31, 2019 were included. Birth hospitalizations were determined separately from other hospitalizations during the first year of life to better differentiate the costs of birth defects from routine delivery costs. Records missing values of age or billed charges were excluded. Sampling weights for the remaining hospitalizations were adjusted to retain total hospitalization frequency and cost.
Cost estimates were calculated as the product of the amount billed for a hospitalization and the corresponding hospital-level cost-to-charge ratios. HCUP-provided cost-to-charge ratios are computed on an annual basis for each hospital (total institutional service delivery costs divided by total amount charged by the hospital).† NIS records facility charges but not professional fees charged by physicians who are not hospital employees.
Birth defects were identified by scanning up to 40 available diagnosis code fields associated with each hospitalization among codes Q00–Q99 (congenital malformations, deformations, and chromosomal abnormalities) of the International Classification of Diseases, Tenth Revision, Clinical Modification (ICD-10-CM). Patent ductus arteriosus (Q25.0) and atrial septal defect (Q21.1) were not considered birth defects when occurring in neonates aged <28 days or with an associated indicator of preterm birth (P07.2 or P07.3). In addition, 23 conditions classified within the Q00–Q99 code range that are commonly considered benign or are otherwise unlikely to contribute to hospitalization costs were not considered birth defects for the purposes of this analysis (Supplementary Table, https://stacks.cdc.gov/view/cdc/130207).
Sampling weights were applied to calculate national estimates of hospitalization frequency and cost. Mean, median, and total costs were calculated by patient demographic and birth defect code characteristics. Mean hospitalization costs were stratified by age group for selected individual birth defects and birth defect categories. If a hospitalization was associated with more than one defect included in the table, the full cost of the hospitalization was included for each defect. The individual birth defects listed include those defined in the National Birth Defects Prevention Network Congenital Malformations Surveillance Report.§ Statistical analyses were performed using SAS software (version 9.4; SAS Institute) with survey procedures incorporating sampling design. This activity was reviewed by CDC and was conducted consistent with applicable federal law and CDC policy.¶
Results
During 2019, a total of 937,295 birth defect–associated hospitalizations incurred a total cost of $22,204,754,855 (Table 1), representing 4.1% of hospitalizations and 7.7% of hospitalization costs among persons in the United States aged <65 years. A birth defect code was the principal diagnosis code for 15.8% of all birth defect–associated hospitalizations that were not birth hospitalizations.
Nonbirth hospitalizations of persons aged <1 year at admission were associated with the highest mean ($61,881) and median ($15,708) costs per hospitalization among all age groups (Table 1). Among birth defect–associated hospitalizations during the first year of life, a co-occurring preterm birth diagnosis code was present in 15.3% of hospitalizations, and hospitalizations with a preterm birth diagnosis code were associated with 45.9% of hospitalization costs. The most prevalent birth defect category was cardiovascular defects (22.3%), which were associated with a total cost of $9,833,000,308 (44.3% of all birth defect–associated hospitalization costs) (Table 1). Critical cardiovascular defects alone accounted for 12.7% of birth defect–associated hospitalization costs and had the highest median cost ($29,430) per hospitalization. Among nonbirth hospitalizations of neonates and infants, defects with a mean cost >$150,000 included esophageal atresia ($214,651), interrupted aortic arch ($199,973), and diaphragmatic hernia ($195,456) (Table 2). Although mean costs per nonbirth hospitalization were highest for patients aged <1 year, this was not consistent across individual birth defects (Table 2) (Figure). Overall, nearly one third of hospitalization costs occurred among patients aged 19–64 years (Table 1).
Discussion
During 2019, the cost of hospitalizations for persons aged <65 years with a birth defect diagnosis code was estimated at $22.2 billion. These hospitalizations were associated with disproportionately high costs, constituting 4.1% of all hospitalizations among persons in the United States aged <65 years and 7.7% of total costs. Nearly one half of hospitalization costs associated with birth defects occurred among neonates and infants, and these costs disproportionately affected persons aged <1 year during nonbirth hospitalizations. Defects of the cardiovascular system were the most prevalent birth defects, were associated with disproportionately high ($9.8 billion) hospitalization costs, and included many of the costliest individual birth defects.
Using 2013 NIS data, the total cost of birth defect–associated hospitalizations was estimated to be $22.9 billion for all ages and $19.1 billion for persons aged <65 years (4). Those estimates included adjustments for professional fees, which historically added 20%–25% to facility costs (5). Applying the same adjustments to the current estimates yields a 2019 estimate of $26.6–27.8 billion in total birth defect–associated hospitalization costs for persons aged <65 years. When adjusted to 2019 hospital care prices, the 2013 cost estimate is $21.0 billion for persons aged <65 years.** The share of birth defect–associated expenditures among total hospitalization expenditures was similar among all age groups: 5.2% in 2013 and 5.5% in 2019.
Limitations
The findings in this report are subject to at least five limitations. First, determining which costs are directly attributable to birth defects is challenging because of difficulties in identifying all sequelae of birth defects and their respective codes, the coding of minor birth defects, and the possible miscoding of some acquired structural or functional abnormalities as birth defects (3). Excluding hospitalizations for persons aged ≥65 years reduces the risk for miscoding but fails to identify the contribution of birth defects among this age group. Second, the potential for two or more birth defects to be documented during the same hospitalization could lead to overestimation of costs for findings presented by individual defect or category. Third, cost-to-charge ratios calculated at the hospital level do not necessarily accurately reflect the costs of different types of hospital services (6), which could bias estimates of a person’s hospitalization costs in an unknown direction. Fourth, HCUP costs are limited to facility fees and fail to include physician or professional fees, thereby underestimating birth defect–associated hospitalization costs. Finally, it is difficult to distinguish the relationship between preterm birth and birth defects, and some of the birth defect–associated costs among preterm infants were possibly due to their prematurity rather than their birth defect.
Implications for Public Health Practice
Updated estimates of hospitalization costs for specific birth defects provide critical information about health care resource use. These data highlight the financial impact across the life span and illustrate the need to understand the continued health care needs of persons born with birth defects to ensure optimal health for all.
Corresponding author: Justin Swanson, jswanson1@usf.edu.
1Lawton and Rhea Chiles Center for Healthy Mothers and Babies, College of Public Health, University of South Florida, Tampa, Florida; 2Division of Birth Defects and Infant Disorders, National Center on Birth Defects and Developmental Disabilities, CDC; 3Office of the Director, National Center on Birth Defects and Developmental Disabilities, CDC; 4Department of Economics, University of Utah, Salt Lake City, Utah.
All authors have completed and submitted the International Committee of Medical Journal Editors form for disclosure of potential conflicts of interest. Russell S. Kirby holds the Marrell endowed chair at the University of South Florida, College of Public Health and serves on the board of directors for the National Birth Defects Prevention Network. Jason L. Salemi and Jean Paul Tanner report grant support to the Florida Department of Health, subcontracted to the University of South Florida, for Advancing Population-based Surveillance of Birth Defects. No other potential conflicts of interest were disclosed.
* https://www.hcup-us.ahrq.gov/db/nation/nis/NISIntroduction2019.pdf
† https://www.hcup-us.ahrq.gov/reports/methods/MS2021-05-CCR-Methodologies.pdf
§ https://www.nbdpn.org/docs/Birth_Defects_Data_and_Directory_2022.pdf
¶ 45 C.F.R. part 46; 21 C.F.R. part 56; 42 U.S.C. Sect. 241(d), 5 U.S.C. Sect. 552a, 44 U.S.C. Sect. 3501 et seq.
References
- CDC. Update on overall prevalence of major birth defects—Atlanta, Georgia, 1978–2005. MMWR Morb Mortal Wkly Rep 2008;57:1–5. PMID:18185492
- Ely DM, Driscoll AK. Infant mortality in the United States, 2019: data from the period linked birth/infant death file. Natl Vital Stat Rep 2021;70:1–18. https://doi.org/10.15620/cdc:111053 PMID:34878382
- Rodriguez FH 3rd, Raskind-Hood CL, Hoffman T, et al. How well do ICD-9-CM codes predict true congenital heart defects? A Centers for Disease Control and Prevention–based multisite validation project. J Am Heart Assoc 2022;11:e024911. https://doi.org/10.1161/JAHA.121.024911 PMID:35862148
- Arth AC, Tinker SC, Simeone RM, Ailes EC, Cragan JD, Grosse SD. Inpatient hospitalization costs associated with birth defects among persons of all ages—United States, 2013. MMWR Morb Mortal Wkly Rep 2017;66:41–6. https://doi.org/10.15585/mmwr.mm6602a1 PMID:28103210
- Peterson C, Xu L, Florence C, Grosse SD, Annest JL. Professional fee ratios for US hospital discharge data. Med Care 2015;53:840–9. https://doi.org/10.1097/MLR.0000000000000410 PMID:26340662
- Salemi JL, Comins MM, Chandler K, Mogos MF, Salihu HM. A practical approach for calculating reliable cost estimates from observational data: application to cost analyses in maternal and child health. Appl Health Econ Health Policy 2013;11:343–57. https://doi.org/10.1007/s40258-013-0040-2 PMID:23807539
Abbreviations: ICD-10-CM = International Classification of Diseases, Tenth Revision, Clinical Modification; USD = U.S. dollars.
* Identified by scanning up to 40 available fields for ICD-10-CM diagnosis codes Q00–Q99: congenital malformations, deformations, and chromosomal abnormalities. Patent ductus arteriosus (Q25.0) and atrial septal defect (Q21.1) were not considered birth defects when occurring in neonates aged <28 days or with an associated indicator of preterm birth (ICD-10-CM codes P07.2 or P07.3). An additional 23 conditions of lesser clinical importance classified within the Q00–Q99 code range were not considered birth defects.
† Birth defects categories correspond to blocks of ICD-10-CM diagnosis codes: cardiovascular (Q20–Q28), central nervous system (Q00–Q07), chromosomal (Q90–Q99), cleft lip/palate (Q35–Q37), ear (Q16–Q17), eye (Q10–Q15), gastrointestinal (Q38–Q45), genitourinary (Q50–Q64), integumentary (Q80–Q85), musculoskeletal (Q65–Q79), and other syndrome (Q87). “Other defect” includes birth defects of the face and neck (Q18), respiratory system (Q30–Q34), and other congenital malformations (Q86 and Q89). Critical cardiovascular defects (https://www.cdc.gov/ncbddd/heartdefects/facts.html) were operationalized using the National Birth Defects Prevention Network Congenital Malformations Surveillance Report (https://www.nbdpn.org/docs/Birth_Defects_Data_and_Directory_2022.pdf). The specific defects included are only those defined in the National Birth Defects Prevention Network Congenital Malformations Surveillance Report; birth defects not included contribute to frequencies and costs aggregated by birth defect category and overall. Because a single hospitalization might include more than one specific birth defect, individual birth defect frequencies might sum to >100% of birth defects categories or overall frequencies, and mean costs multiplied by frequencies will correspondingly sum to >100% of total costs.
Abbreviations: CNS = central nervous system; GI = gastrointestinal; ICD-10-CM = International Classification of Diseases, Tenth Revision, Clinical Modification; MS = musculoskeletal; USD = U.S. dollars.
* Identified by scanning up to 40 available diagnosis code fields for ICD-10-CM diagnosis codes Q00–Q99: congenital malformations, deformations, and chromosomal abnormalities.
† Birth defects categories correspond to blocks of ICD-10-CM diagnosis codes: cardiovascular (Q20–Q28), CNS (Q00–Q07), chromosomal (Q90–Q99), cleft lip/palate (Q35–Q37), ear (Q16–Q17), eye (Q10–Q15), GI (Q38–Q45), genitourinary (Q50–Q64), integumentary (Q80–Q85), MS (Q65–Q79), and other syndrome (Q87). “Other defect” includes birth defects of the face and neck (Q18), respiratory system (Q30–Q34), and other congenital malformations (Q86 and Q89). Critical cardiovascular defects (https://www.cdc.gov/ncbddd/heartdefects/facts.html) were operationalized using the National Birth Defects Prevention Network Congenital Malformations Surveillance Report (https://www.nbdpn.org/docs/Birth_Defects_Data_and_Directory_2022.pdf). The specific defects included are only those defined in the National Birth Defects Prevention Network Congenital Malformations Surveillance Report; birth defects not included here contribute to frequencies and costs aggregated by birth defect category and overall.
§ Because a single hospitalization might include more than one specific birth defect, individual birth defect frequencies might sum to >100% of birth defects categories or overall frequencies, and mean costs multiplied by frequencies will correspondingly sum to >100% of total costs.
¶ For hospitalizations with any birth defect, the birth hospitalization costs include the costs for routine birth hospitalization.
** Cell sizes ≤10 were suppressed. Sums across all ages exclude suppressed cells.
 FIGURE. Weighted estimates of median costs of hospitalizations, by birth defect*,† and age group at admission — National Inpatient Sample, United States, 2019
FIGURE. Weighted estimates of median costs of hospitalizations, by birth defect*,† and age group at admission — National Inpatient Sample, United States, 2019
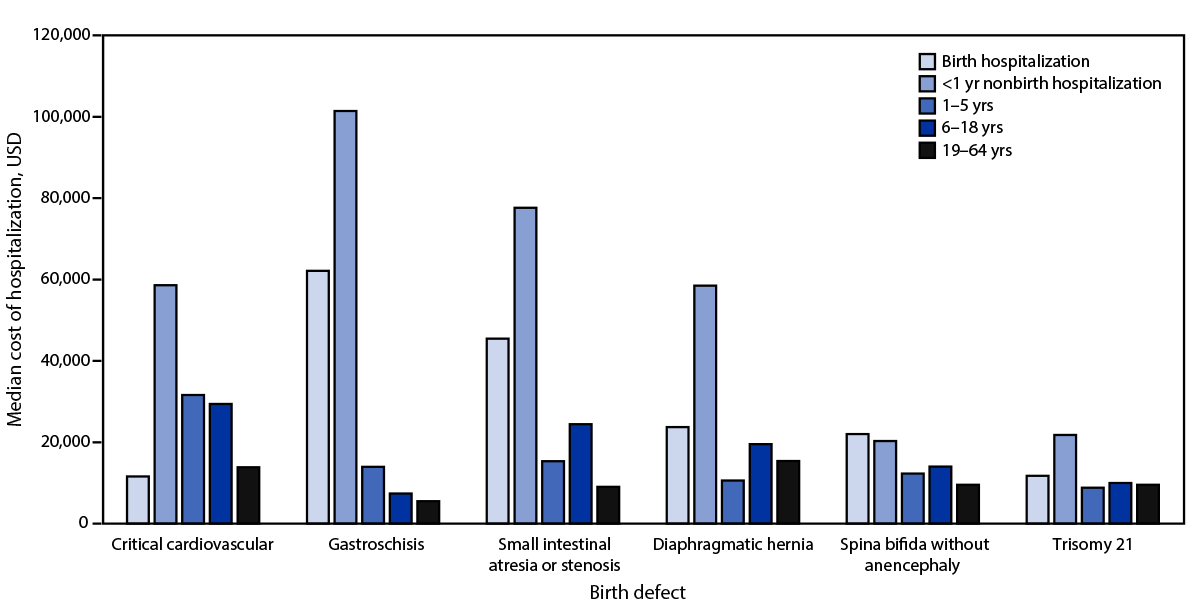
Abbreviation: USD = U.S. dollars.
* Identified by scanning up to 40 available fields of International Classification of Diseases, Tenth Revision, Clinical Modification diagnosis codes. Critical cardiovascular defects include common arterial trunk (Q20.0), double outlet right ventricle (Q20.1), transposition of the great arteries (Q20.3), single ventricle (Q20.4), tetralogy of Fallot (Q21.3), pulmonary valve atresia (Q22.0), tricuspid valve atresia (Q22.4), Ebstein anomaly (Q22.5), hypoplastic left heart syndrome (Q23.4), coarctation of aorta (Q25.1), interrupted aortic arch (Q25.21), and total anomalous pulmonary venous connection (Q26.2). Specific birth defects are identified as gastroschisis (Q79.3), small intestinal atresia or stenosis (Q41), diaphragmatic hernia (Q79.0 and Q79.1), spina bifida without anencephaly (Q05, Q07.01, and Q07.03), and trisomy 21 (Q90).
† The specific birth defects shown were selected to represent a range of body systems.
Suggested citation for this article: Swanson J, Ailes EC, Cragan JD, et al. Inpatient Hospitalization Costs Associated with Birth Defects Among Persons Aged <65 Years — United States, 2019. MMWR Morb Mortal Wkly Rep 2023;72:739–745. DOI: http://dx.doi.org/10.15585/mmwr.mm7227a1.
MMWR and Morbidity and Mortality Weekly Report are service marks of the U.S. Department of Health and Human Services.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All HTML versions of MMWR articles are generated from final proofs through an automated process. This conversion might result in character translation or format errors in the HTML version. Users are referred to the electronic PDF version (https://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.