Notes from the Field: Outbreak of Ebola Virus Disease Caused by Sudan ebolavirus — Uganda, August–October 2022
Weekly / November 11, 2022 / 71(45);1457–1459
Thomas Kiggundu, MMed1; Alex R. Ario, PhD1; Daniel Kadobera, MSc1; Benon Kwesiga, MPH1; Richard Migisha, MPH1; Issa Makumbi, MSc2; Daniel Eurien, MPH3; Zainah Kabami, MPH1; Joshua Kayiwa, MSc2; Bernard Lubwama, MPH4; Denis Okethwangu, MSc4; Susan Nabadda, MMed5; Godfrey Bwire, PhD4; Sophia Mulei, PhD6; Julie R. Harris, PhD7; Emilio Dirlikov, PhD7; Arthur G. Fitzmaurice, PhD7; Sandra Nabatanzi, MSc7; Yonas Tegegn, MD8; Allan N. Muruta, MSc4; Daniel Kyabayinze, PhD4; Amy L. Boore, PhD7; Atek Kagirita, MPH4; Henry Kyobe-Bosa, MSc4; Henry G. Mwebesa, MPH4; Diana Atwine, MMed4; Jane R. Aceng Ocero, MMed4; Uganda Ebola Response Team (View author affiliations)
View suggested citationEbola virus disease (EVD) is a rare and often deadly viral hemorrhagic fever (VHF); four species of Ebola virus (Zaire ebolavirus, Sudan ebolavirus, Taï Forest ebolavirus, and Bundibugyo ebolavirus) cause occasional outbreaks among humans and nonhuman primates* (1). Infection is transmitted through direct contact with infectious blood, body fluids, and animal tissues. Symptoms include fever, abdominal pain, diarrhea, vomiting, generalized body weakness, and hemorrhage. Since 2000, four outbreaks of EVD caused by Sudan ebolavirus have been identified in Uganda; the largest outbreak (in 2000) resulted in 425 cases and 224 (53%) deaths (2,3). No vaccine is available to prevent Sudan ebolavirus infection, and treatment is supportive. The estimated case fatality rate is 55% (4).
On September 17, 2022, Uganda’s National Public Health Emergency Operations Centre and the Uganda Virus Research Institute VHF program were notified of a suspected VHF case in a male patient (patient A) aged 26 years who lived in Madudu subcounty, Mubende District in central Uganda. The patient had been referred to Mubende Regional Referral Hospital (MRRH) the previous day by a private health clinic. At the time of admission, patient A had high fever, abdominal pain, diarrhea, chest pain, loss of appetite, dry cough, bloody vomitus, and bleeding from the eyes. He reported no recent travel or known Ebola virus exposures. Based on public health protocols for suspected VHF, the patient was isolated at MRRH by the Mubende District health team to await laboratory test results. Despite supportive treatment, the patient died on September 18, 2022, and the Uganda Ministry of Health (MoH) was notified. A blood sample collected from patient A on September 17 was confirmed positive for Sudan ebolavirus on September 19; testing by reverse transcription–polymerase chain reaction (RT-PCR) had been conducted at the Uganda Virus Research Institute (5). On September 19, local leaders from Madudu and Butoloogo, two contiguous subcounties, reported six community deaths during August 13–September 15 among persons with probable EVD. Upon laboratory confirmation of EVD in patient A, MRRH established an Ebola treatment unit (ETU) to manage patients, and another ETU was activated at Fort Portal Regional Referral Hospital in western Uganda.
On September 21, 2022, MoH, the Mubende District health team, and other partners launched a public health emergency response to identify additional cases of EVD. The response focuses on active case finding (initiated in Madudu and Butoloogo subcounties), tracing and monitoring contacts for EVD signs and symptoms, conducting laboratory testing, and providing treatment. A probable case was defined as death in a person with suspected EVD who had a direct epidemiologic link to a confirmed case but did not have laboratory-confirmed infection. A confirmed case was a person with EVD who had received positive laboratory test results by RT-PCR or EVD immunoglobulin M serology. Patients with EVD who were discharged from ETUs with two negative RT-PCR tests 48 hours apart were considered recovered. Contact monitoring consisted of daily temperature checks and EVD symptom screening of persons who had direct (i.e., physical) or indirect contact (e.g., with used linens or utensils, or shared space) with patients with probable or confirmed EVD.
During September 18–October 31, 2022, a total of 130 confirmed and 18 probable EVD cases were identified; symptom onset in the first probable case occurred on August 8 (Figure). On October 31, a total of 1,777 contacts were monitored; among these 1,540 (87%) were successfully monitored on that day. Among probable and confirmed cases, the median patient age is 29 years (range = 1–70 years), 87 (59%) patients are men, and 81 (55%) are residents of Mubende district. Among the 130 confirmed cases, 43 (33%) deaths were reported as of October 31. Sixty-one deaths (probable and confirmed cases) were reported; the median age of decedents was 28 years (range = <1–58 years), and 31 (51%) were women. Eighteen confirmed or probable EVD cases during this period were reported among health care workers; five were linked to a surgical procedure performed on a patient with probable EVD who died on September 17. As of October 31, 45 patients had recovered, 37 patients are undergoing treatment in an ETU, and outcomes are unknown for five.
This report describes the fifth outbreak of EVD caused by Sudan ebolavirus in Uganda since 2000 (2,3). Given continued transmission, public health response to this outbreak is ongoing, including epidemiologic investigation to identify the source of the outbreak.† Persons living in or traveling to Uganda should avoid activities that could result in exposures to infected persons or animals, including direct contact with body fluids or objects contaminated with blood or body fluids. Health care workers caring for EVD patients should adhere to proper infection control practices, including appropriate use of personal protective equipment.§ Public health departments, public health laboratories, and health care workers outside Uganda, including in the United States, should be aware of recommended practices to identify, report, and prevent EVD.¶ Health care providers in the United States and elsewhere should be alert for and evaluate any patients suspected of having EVD, particularly persons who have recently been in the affected areas in Uganda.
Acknowledgments
Regional and district health teams; site staff members; partners.
Uganda Ebola Response Team
Natalie E. Brown, U.S. Department of State; Brian Agaba, Uganda National Institute of Public Health; Sherry Rita Ahirirwe, Uganda National Institute of Public Health; Rebecca Akunzirwe, Uganda National Institute of Public Health; Alice Asio, Uganda National Institute of Public Health; Immaculate Atuhaire, Uganda National Institute of Public Health; Sarah Elayeete, Uganda National Institute of Public Health; Doreen Gonahasa, Uganda National Institute of Public Health; Edirisa Juniour Nsubuga, Uganda National Institute of Public Health; Patrick King, Uganda National Institute of Public Health; Saudah Kizito, Uganda National Institute of Public Health; Allan Komackech, Uganda National Institute of Public Health; Veronica Masanja, Uganda National Institute of Public Health; Stella Martha Migamba, Uganda National Institute of Public Health; Patience Mwine, Uganda National Institute of Public Health; Hellen Nelly Naiga, Uganda National Institute of Public Health; Petranilla Nakamya, Uganda National Institute of Public Health; Rose Nampeera, Uganda National Institute of Public Health; Mackline Ninsiima, Uganda National Institute of Public Health; Alex Ndybakira, Uganda National Institute of Public Health; Lawrence Oonyu, Uganda National Institute of Public Health; Brenda Nakafeero Simbwa, Uganda National Institute of Public Health; Hildah Tendo, Uganda National Institute of Public Health; Mercy Wendy Wanyana, Uganda National Institute of Public Health; Jane Frances Zalwango, Uganda National Institute of Public Health; Maria Gorette Zalwango, Uganda National Institute of Public Health; Robert Zavuga, Uganda National Institute of Public Health; Immaculate Asiimwe, Uganda Ministry of Health; Richardson Mafigiri, Uganda Ministry of Health; Esther Muwanguzi, Uganda Ministry of Health; Stephen Balinandi, Uganda Virus Research Institute; Luke Nyakarahuka, Uganda Virus Research Institute; Jimmy Baluku, Uganda Virus Research Institute; Jackson Kyando, Uganda Virus Research Institute; Alex Tumusiime, Uganda Virus Research Institute; Caitlin Cossaboom, CDC; Carrie Eggers, CDC; John D. Klena, CDC; Lisa Nelson, CDC; Modupe Osinubi, CDC; Katrin Sadigh, CDC; Waverly Vosburgh, CDC; Mary-Claire Worrell, CDC; Philimon Kabagambe, World Health Organization Uganda; Charles Okot, World Health Organization, Uganda; Godfrey Nsereko, CDC; Olivia Namusisi, Africa Field Epidemiology Network.
Corresponding author: Thomas Kiggundu, tkiggundu@musph.ac.ug; tkiggundu@uniph.go.ug.
1Uganda Public Health Fellowship Program, Uganda National Institute of Public Health, Kampala, Uganda; 2National Public Health Emergency Operations Centre, Uganda National Institute of Public Health, Kampala, Uganda; 3Baylor College of Medicine Children’s Foundation-Uganda, Kampala, Uganda; 4Uganda Ministry of Health, Kampala, Uganda; 5National Health Laboratory Services, Uganda Ministry of Health, Kampala, Uganda; 6Uganda Virus Research Institute, Kampala, Uganda; 7CDC Uganda, Kampala, Uganda; 8World Health Organization Country Office, Kampala, Uganda.
All authors have completed and submitted the International Committee of Medical Journal Editors form for disclosure of potential conflicts of interest. No potential conflicts of interest were disclosed.
References
- Feldmann H, Geisbert TW. Ebola haemorrhagic fever. Lancet 2011;377:849–62. https://doi.org/10.1016/S0140-6736(10)60667-8 PMID:21084112
- Sanchez A, Rollin PE. Complete genome sequence of an Ebola virus (Sudan species) responsible for a 2000 outbreak of human disease in Uganda. Virus Res 2005;113:16–25. https://doi.org/10.1016/j.virusres.2005.03.028 PMID:16139097
- CDC. Outbreak of Ebola hemorrhagic fever Uganda, August 2000–January 2001. MMWR Morb Mortal Wkly Rep 2001;50:73–7. PMID:11686289
- Lefebvre A, Fiet C, Belpois-Duchamp C, Tiv M, Astruc K, Aho Glélé LS. Case fatality rates of Ebola virus diseases: a meta-analysis of World Health Organization data. Med Mal Infect 2014;44:412–6. https://doi.org/10.1016/j.medmal.2014.08.005 PMID:25193630
- Towner JS, Rollin PE, Bausch DG, et al. Rapid diagnosis of Ebola hemorrhagic fever by reverse transcription-PCR in an outbreak setting and assessment of patient viral load as a predictor of outcome. J Virol 2004;78:4330–41. https://doi.org/10.1128/JVI.78.8.4330-4341.2004 PMID:15047846
 FIGURE. Probable (n = 18) and confirmed (n = 130) cases of Ebola virus disease,* by symptom onset date† — Uganda, August 8–October 31, 2022
FIGURE. Probable (n = 18) and confirmed (n = 130) cases of Ebola virus disease,* by symptom onset date† — Uganda, August 8–October 31, 2022
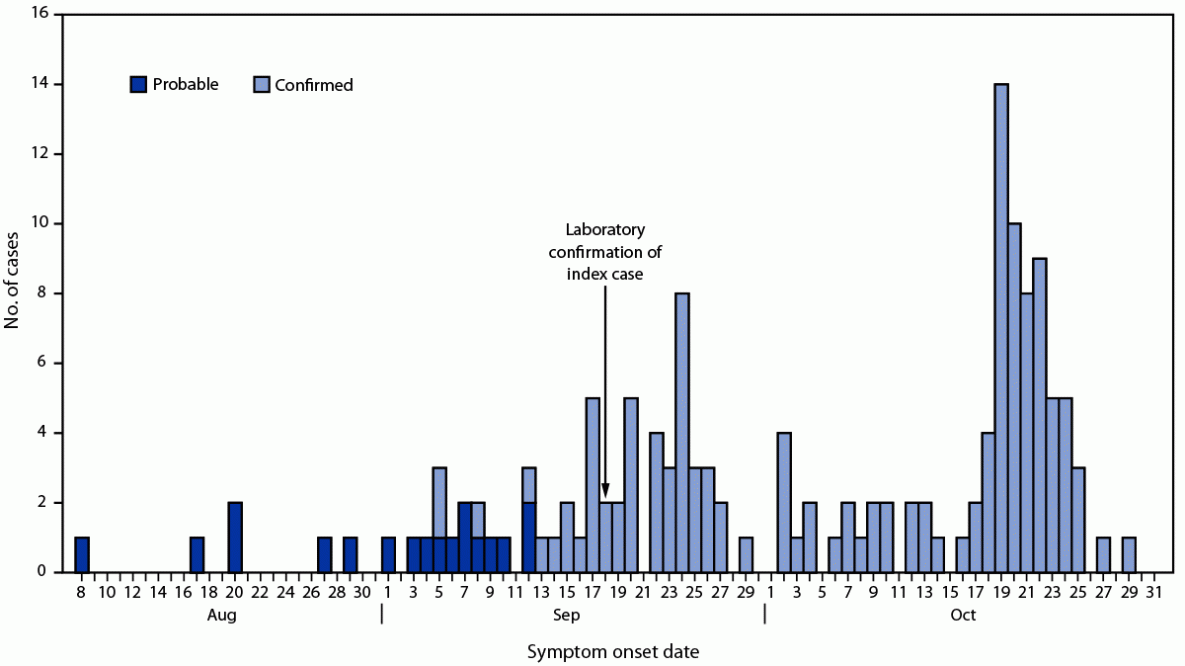
Abbreviations: EVD = Ebola virus disease; RT-PCR = reverse transcription–polymerase chain reaction.
* A probable case was defined as death in a person with suspected EVD who had a direct epidemiologic link to a confirmed case but did not have laboratory-confirmed infection. A confirmed case was a person with confirmed EVD who had received positive laboratory test results by RT-PCR or EVD immunoglobulin M serology.
† Identified cases as of October 31, 2022. Additional cases with symptom onset on or before October 31 might subsequently be identified.
Suggested citation for this article: Kiggundu T, Ario AR, Kadobera D, et al. Notes from the Field: Outbreak of Ebola Virus Disease Caused by Sudan ebolavirus — Uganda, August–October 2022. MMWR Morb Mortal Wkly Rep 2022;71:1457–1459. DOI: http://dx.doi.org/10.15585/mmwr.mm7145a5.
MMWR and Morbidity and Mortality Weekly Report are service marks of the U.S. Department of Health and Human Services.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All HTML versions of MMWR articles are generated from final proofs through an automated process. This conversion might result in character translation or format errors in the HTML version. Users are referred to the electronic PDF version (https://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.