COVID-19 Cases and Hospitalizations Among Medicare Beneficiaries With and Without Disabilities — United States, January 1, 2020–November 20, 2021
Weekly / June 17, 2022 / 71(24);791–796
Yan Yuan, MS1; JoAnn M. Thierry, PhD2; Lara Bull-Otterson, PhD1,3; Marshalyn Yeargin-Allsopp, MD2; Kristie E.N. Clark, MD3; Catherine Rice, PhD2; Matthew Ritchey, DPT1,3; A. Blythe Ryerson, PhD2 (View author affiliations)
View suggested citationSummary
What is already known about this topic?
Persons with disabilities are at high risk for severe outcomes from COVID-19, including death.
What is added by this report?
COVID-19–associated hospitalization rates among disability-eligible Medicare beneficiaries (3,148 per 100,000) were approximately 50% higher than rates among age-eligible (i.e., ≥65 years) beneficiaries (2,129 per 100,000), and hospitalization rates increased by age in both groups. Among persons with disabilities, American Indian or Alaska Native persons experienced the highest rate of COVID-19–associated hospitalization (4,962 per 100,000).
What are the implications for public health practice?
Efforts to increase access to and implementation of COVID-19 prevention and treatment strategies, including vaccination, are critical to reducing severe COVID-19–associated outcomes among persons with disabilities.
Altmetric:
Approximately 27% of adults in the United States live with a disability,* some of whom qualify for Medicare benefits. Persons with disabilities are at increased risk for severe COVID-19–associated outcomes compared with the general population (1); however, existing studies have limited generalizability† or only pertain to a specific disability (e.g., intellectual) (2). Older age is also associated with COVID-19–associated hospitalization and death, but the extent to which age might contribute to increased risk for severe COVID-19–associated outcomes among persons with disabilities is unknown (3). To describe the impact of COVID-19 on persons with disabilities and whether and how age contributes to disease rates, CDC assessed COVID-19 cases and hospitalizations during January 2020–November 2021, among Centers for Medicare & Medicaid Services (CMS) Medicare beneficiaries aged ≥18 years who were either eligible because of a disability (disability-eligible§) or only eligible because of age ≥65 years (age-eligible). COVID-19 incidence and hospitalization rates were higher in the disability-eligible group (10,978 and 3,148 per 100,000 population, respectively) throughout the study period compared with the age-eligible group (8,102 and 2,129 per 100,000 population, respectively). Both COVID-19 incidence and hospitalization rates increased with age in both disability- and age-eligible beneficiaries. American Indian or Alaska Native (AI/AN) persons had the highest disability-eligible (4,962 per 100,000) and age-eligible (5,024 per 100,000) hospitalization rates. Among all other racial and ethnic groups, hospitalization rates were higher among disability-eligible than among age-eligible patients. COVID-19 incidence and hospitalization rates among disability-eligible Medicare beneficiaries were disproportionally higher than rates among age-eligible beneficiaries. Collection of disability status as a core demographic variable in public health surveillance data and identification, as well as the addition of disability questions in other existing data sources can guide research and development of interventions for persons with disabilities. Efforts to increase access to and use of COVID-19 prevention and treatment strategies, including activities that support equitable vaccine access regardless of the substantial challenges that older adults and persons with disability face, are critical to reducing severe COVID-19–associated outcomes among these groups.
Medicare fee-for-service claims data, Medicare Advantage Plans encounter data, and Medicare enrollment information were used to identify the first diagnosis or hospitalization¶ for CMS Medicare beneficiaries with COVID-19 during January 2020–November 2021. International Classification of Diseases, Tenth Revision, Clinical Modification (ICD-10-CM) codes B97.29 or U07.1 (starting in April 2020) were used to identify COVID-19 on a claim or encounter record from any health care setting (e.g., outpatient and inpatient hospital). To better evaluate the contribution of age to disease and hospitalization rates, COVID-19 cases and hospitalizations were stratified into two mutually exclusive groups: aged ≥65 years without disability (age-eligible) and aged ≥18 years with disability (disability-eligible); all disability-eligible adults were grouped together, irrespective of age. Approximately 44% of disability-eligible beneficiaries were also aged ≥65 years; these included persons with developmental, sensory, and mobility disabilities, as well as persons with other or uncategorized disabilities.
Monthly COVID-19 incidence and hospitalization rates were calculated using numbers of COVID-19 cases and hospitalizations among Medicare beneficiaries, divided by the Medicare population, or the population having hospital coverage for each month. Median length of hospital stay, underlying medical conditions, which were defined using measures of Chronic Condition Warehouse chronic disease indicators,** and hospitalization discharge status were compared by eligibility group. Deaths were defined as the number of patients listed as having died on the discharge date (in an inpatient or outpatient setting) or cases for which the inpatient discharge code indicated death. Because previous research suggests that vaccination coverage might differ between disability- and age-eligible groups, with persons with disabilities being less likely to be vaccinated (4), CMS guidance around analyzing and interpreting COVID-19 vaccine data was considered.†† In keeping with this guidance, COVID-19 vaccination was not included in the analysis, as vaccination records were incomplete or not reflective of vaccine doses administered. Rate differences between groups were tested using two-tailed t-tests for continuous variables and Pearson’s chi-square tests for categorical variables; p-values <0.05 were considered statistically significant. Statistical analyses were performed using SAS Enterprise Guide (version 7.1; SAS Institute). This activity was reviewed by CDC and was conducted consistent with applicable federal law and CDC policy.§§
The study population comprised 68,911,412 Medicare beneficiaries, including 53,814,118 (78%) who were age-eligible and 15,097,294 (22%) who were disability-eligible. Compared with age-eligible beneficiaries, among whom overall cumulative COVID-19 incidence was 8,102 per 100,000 population, incidence was higher among disability-eligible beneficiaries (10,978 per 100,000) (p<0.001) (Table). The overall COVID-19–associated hospitalization rate was also significantly higher among disability-eligible beneficiaries (3,148 per 100,000) than among age-eligible beneficiaries (2,129 per 100,000) (p<0.001). COVID-19 incidence and hospitalization rates were higher among disability-eligible beneficiaries throughout the study period (Figure 1). Among disability-eligible beneficiaries, hospitalization rates among females and males (3,175 and 3,121 per 100,000, respectively) were significantly higher than those among age-eligible beneficiaries (1,951 and 2,350 per 100,000, respectively) (p<0.001) (Table). Hospitalization rates increased with increasing age in both groups and were also significantly higher among disability-eligible beneficiaries of all age groups (p<0.001). Among disability-eligible beneficiaries aged <65 years, the COVID-19–associated hospitalization rate (2,423 per 100,000) was significantly higher than the overall hospitalization rate in the age-eligible group (2,129 per 100,000) (p<0.001).
By race and ethnicity, hospitalization rates were highest among AI/AN persons (both disability-eligible [4,962 per 100,000] and age-eligible [5,024 per 100,000]), followed by Black or African American (Black) persons, (disability-eligible = 4,323; age-eligible = 3,318). Hospitalization rates among disability-eligible beneficiaries were significantly higher than were those among age-eligible beneficiaries for all racial and ethnic groups other than AI/AN.
The median length of hospital stay for COVID-19 hospitalizations was 7 days for both disability- and age-eligible beneficiaries. Although place of residence before hospitalization was not identified, the largest proportion of patients were discharged to their home in both groups (58.0% of disability-eligible and 54.4% of age-eligible), followed by discharge to a skilled nursing facility (16.9% of disability-eligible and 17.6% of age-eligible) (Supplementary Table, https://stacks.cdc.gov/view/cdc/118094). Overall, the in-hospital mortality rate was lower among disability-eligible patients (16.5%) than among age-eligible patients (19.0%). However, the mortality rate among disability-eligible beneficiaries aged ≥65 years was 19.1%, similar to that among age-eligible beneficiaries (19.0%).
Among 18 underlying medical conditions¶¶ assessed among Medicare beneficiaries hospitalized with COVID-19, 91.4% of disability-eligible and 90.6% of age-eligible beneficiaries had two or more conditions (p<0.001). The prevalence of 16 of these conditions (including obesity, depression, chronic obstructive pulmonary disease, chronic kidney disease, heart failure, and anemia) were significantly higher in disability-eligible beneficiaries aged ≥65 years than in age-eligible beneficiaries (Figure 2).
Discussion
This study found that COVID-19 incidence and hospitalization rates were disproportionately higher among disability-eligible Medicare beneficiaries aged ≥18 years than among age-eligible beneficiaries (i.e., aged ≥65 years). COVID-19 incidence and hospitalization rates also increased with age among both disability- and age-eligible beneficiaries, consistent with previous findings that age is an important risk factor for COVID-19–associated hospitalization (5). These finding suggest that the observed disparity among persons with disabilities is being driven, in part, by age; however, other factors, including lower vaccination access and coverage among persons with disabilities, and the high prevalence of underlying conditions that increase risk for severe outcomes likely also contribute to this disparity (4). Taken together, these findings reinforce the importance of increasing access to and implementing COVID-19 prevention and treatment strategies, including vaccination, among persons with disabilities.
AI/AN beneficiaries accounted for the smallest racial and ethnic group (0.7% of disability-eligible and 0.3% of age-eligible beneficiaries); however, this group experienced the highest rates of COVID-19 cases and hospitalizations among both age- and disability-eligible beneficiaries. Rates among Black and Hispanic adults with disabilities were also consistently higher than those among non-Hispanic White, non-Hispanic Asian adults, and adults of other or unknown race and ethnicity with disabilities. Previous studies have also identified higher COVID-19–associated risks among certain minority racial and ethnic groups (6,7). Additional intersectional research might help to better elucidate the factors that contribute to these racial and ethnic differences. CMS and CDC have fostered an interagency partnership to share administrative claims data for public health analyses during the COVID-19 pandemic; these data-sharing efforts augment the ability to examine the incidence and severity of disease faced by persons with disabilities. Primary prevention through continued COVID-19 vaccination efforts that focus on racial and ethnic subgroups with disabilities might further public health efforts to minimize mortality and morbidity (5) and reduce disparities.
CDC has also developed guidance and tools to help persons with disabilities and those who serve or care for them make decisions and protect their health.*** Several accessible materials and culturally competent COVID-19 resources have been developed for persons with disabilities and for health care providers who support them. To improve available support to persons with disabilities, CDC has funded partners such as the Administration for Community Living, which manages the Disability Information and Access Line,††† and regularly reviews the literature on the impact of COVID-19 on persons with disabilities; associated clinical evidence reviews are periodically updated and posted online.§§§
The findings in this report are subject to at least four limitations. First, claims submitted to Medicare are not representative of all persons with a disability or older adults, and as with all claims data, there is some delay in reporting data. Disability-eligible Medicare beneficiaries might be more likely to have more severe disabilities than persons without Medicare because eligibility requires both a time component and disease documentation.¶¶¶ These requirements might differentially select for persons with a higher inherent risk for infection with SARS-CoV-2, the virus that causes COVID-19, or less access to medical treatment for COVID-19 than age-eligible beneficiaries. Second, vaccination coverage was not considered in this analysis because of limitations in administrative reporting and data; persons with disabilities are less likely to receive COVID-19 vaccination than are persons without disabilities (3). Third, SARS-CoV-2 genomic variants were not considered in this analysis, nor were rates compared by time; however, trends followed similar peaks identified in national incidence data (8). Finally, the ICD-10-CM codes used to identify COVID-19 diagnosis and associated hospitalization might include incidental COVID-19 cases that were identified during a care visit for another purpose. However, the misclassification bias was likely systematic and equally distributed between the groups, and thus unlikely to affect the observed findings.
Continuing COVID-19 prevention efforts and focused messaging to persons with disabilities remain high-impact public health priorities. Although progress has been made, more work remains to be done to prioritize persons with disabilities in public health programs, data systems, and preparedness and response activities at the federal, state, and local levels. Collection of disability status as a core demographic variable in public health surveillance data and identification, as well as the addition of disability questions in other existing data sources can guide research and development of interventions for persons with disabilities. Efforts to increase access to and use of COVID-19 prevention and treatment strategies, including activities that support equitable vaccine access in the face of the substantial challenges that older adults and those with disabilities face, are critical to reducing severe COVID-19–associated outcomes among these groups.****
Corresponding author: A. Blythe Ryerson, ztq6@cdc.gov.
1Division of Health Informatics and Surveillance, Center for Surveillance, Epidemiology, and Laboratory Services, CDC; 2Division of Human Development and Disability, National Center on Birth Defects and Developmental Disabilities, CDC; 3CDC COVID-19 Emergency Response Team.
All authors have completed and submitted the International Committee of Medical Journal Editors form for disclosure of potential conflicts of interest. No potential conflicts of interest were disclosed.
* https://dhds.cdc.gov (Accessed May 5, 2022).
† https://www.medrxiv.org/content/10.1101/2021.06.10.21258693v1
§ Because Medicare eligibilities can change over time, two mutually exclusive groups were defined based on reasons for initial Medicare enrollment. https://www.cms.gov/Medicare/Eligibility-and-Enrollment/OrigMedicarePartABEligEnrol
¶ CMS released the Medicare data sets on December 17, 2021. COVID-19 hospitalizations were restricted to those among beneficiaries with an inpatient hospitalization claim or encounter record with a primary or secondary diagnosis code indicating COVID-19.
** https://www2.ccwdata.org/web/guest/condition-categories (Accessed April 20, 2022).
†† https://www.cms.gov/medicare-covid-19-vaccine-analysis (Accessed April 20, 2022).
§§ 45 C.F.R. part 46, 21 C.F.R. part 56; 42 U.S.C. Sect. 241(d); 5 U.S.C. Sect. 552a; 44 U.S.C. Sect. 3501 et seq
¶¶ Eighteen underlying medical conditions: Alzheimer disease and dementia, anemia, asthma, atrial fibrillation, cancer (breast, colorectal, leukemia and lymphoma, lung, and prostate), chronic kidney disease, COPD and bronchiectasis, depression, heart failure, hyperlipidemia, hypertension, ischemic heart disease, obesity, osteoporosis, peripheral vascular disease, rheumatoid and osteoarthritis, schizophrenia, and stroke. Underlying medical conditions data are only available in full fee-for-service beneficiaries who had 12 months of Medicare Part A and B (or coverage until time of death) and had no Medicare Advantage coverage during 2020.
††† Persons with a disability seeking assistance in getting a COVID-19 vaccine can call 888-677-1199, Monday–Friday from 9:00 a.m. to 8:00 p.m. EST or can email DIAL@n4a.org
§§§ https://www.cdc.gov/coronavirus/2019-ncov/downloads/clinical-care/C-Disability-Review.pdf
¶¶¶ To be eligible for Social Security disability benefits, persons have to show an inability to engage in any substantial gainful activity by reason of any medically determinable physical or mental impairments, that can be expected to result in death or that have lasted or can be expected to last for a continuous period of not <12 months. https://www.ssa.gov/ (Accessed April 20, 2022).
References
- Henderson A, Fleming M, Cooper SA, et al. COVID-19 infection and outcomes in a population-based cohort of 17 203 adults with intellectual disabilities compared with the general population. J Epidemiol Community Health 2022;76:550–5. https://doi.org/10.1136/jech-2021-218192 PMID:35232778
- Landes SD, Turk MA, Formica MK, McDonald KE, Stevens JD. COVID-19 outcomes among people with intellectual and developmental disability living in residential group homes in New York State. Disabil Health J 2020;13:100969. https://doi.org/10.1016/j.dhjo.2020.100969 PMID:32600948
- Panagiotou OA, Kosar CM, White EM, et al. Risk factors associated with all-cause 30-day mortality in nursing home residents with COVID-19. JAMA Intern Med 2021;181:439–48. https://doi.org/10.1001/jamainternmed.2020.7968 PMID:33394006
- Ryerson AB, Rice CE, Hung MC, et al. Disparities in COVID-19 vaccination status, intent, and perceived access for noninstitutionalized adults, by disability status—National Immunization Survey Adult COVID Module, United States, May 30–June 26, 2021. MMWR Morb Mortal Wkly Rep 2021;70:1365–71. https://doi.org/10.15585/mmwr.mm7039a2 PMID:34591826
- Romero Starke K, Petereit-Haack G, Schubert M, et al. The age-related risk of severe outcomes due to COVID-19 infection: a rapid review, meta-analysis, and meta-regression. Int J Environ Res Public Health 2020;17:5974. https://doi.org/10.3390/ijerph17165974 PMID:32824596
- Killerby ME, Link-Gelles R, Haight SC, et al.; CDC COVID-19 Response Clinical Team. Characteristics associated with hospitalization among patients with COVID-19—metropolitan Atlanta, Georgia, March–April 2020. MMWR Morb Mortal Wkly Rep 2020;69:790–4. https://doi.org/10.15585/mmwr.mm6925e1 PMID:32584797
- Stokes EK, Zambrano LD, Anderson KN, et al. Coronavirus disease 2019 case surveillance—United States, January 22–May 30, 2020. MMWR Morb Mortal Wkly Rep 2020;69:759–65. https://doi.org/10.15585/mmwr.mm6924e2 PMID:32555134
- Iuliano AD, Brunkard JM, Boehmer TK, et al. Trends in disease severity and health care utilization during the early Omicron variant period compared with previous SARS-CoV-2 high transmission periods—United States, December 2020–January 2022. MMWR Morb Mortal Wkly Rep 2022;71:146–52. https://doi.org/10.15585/mmwr.mm7104e4 PMID:35085225
Abbreviations: AI/AN = American Indian or Alaska Native; NA = not applicable.
* Age-eligible beneficiaries were aged ≥65 years and had no disability; disability-eligible beneficiaries were aged ≥18 years and had one or more disabilities.
† COVID-19 cases 100,000 population.
§ COVID-19–associated hospitalizations per 100,000 population.
¶ Rate differences between age- and disability-eligible groups were tested with two-tailed Pearson’s chi-square test; p-values <0.05 were considered statistically significant.
** Dashes indicate not applicable because the values are presented as rates per 100,000 persons,
 FIGURE 1. Monthly COVID-19 incidence (A)* and hospitalization rate (B)†,§ among age- and disability-eligible¶ Medicare beneficiaries — United States, January 1, 2020–November 20, 2021
FIGURE 1. Monthly COVID-19 incidence (A)* and hospitalization rate (B)†,§ among age- and disability-eligible¶ Medicare beneficiaries — United States, January 1, 2020–November 20, 2021
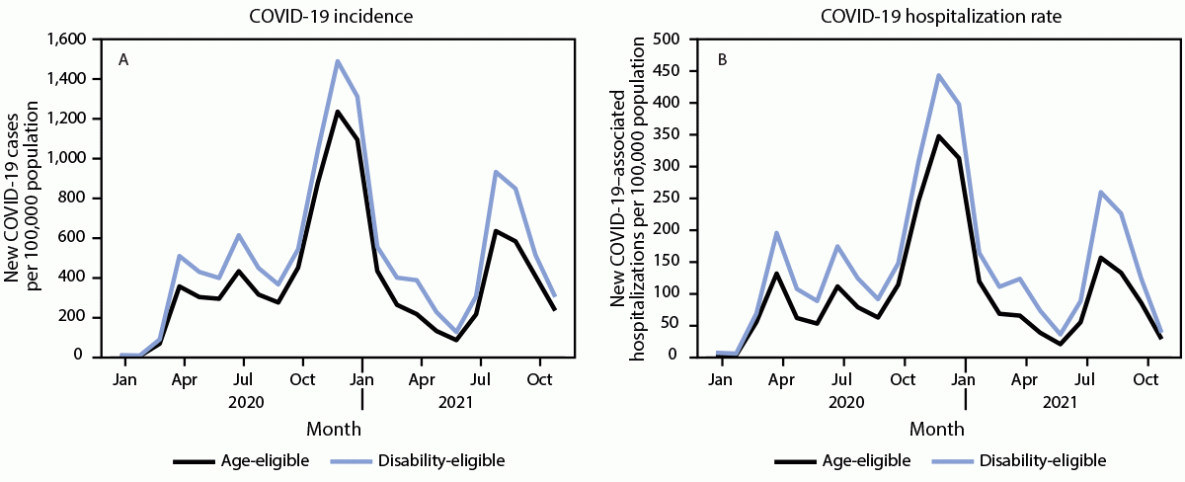
* COVID-19 cases per 100,000 population.
† COVID-19–associated hospitalizations per 100,000 population.
§ The y-axis scales for panels A and B are different.
¶ Age-eligible beneficiaries were aged ≥65 years and had no disability; disability-eligible beneficiaries were aged ≥18 years and had one or more disabilities.
 FIGURE 2. Percentage of Medicare beneficiaries hospitalized with COVID-19 with 18* selected underlying medical conditions,† by age and disability eligibility§ — United States, January 1, 2020–November 20, 2021
FIGURE 2. Percentage of Medicare beneficiaries hospitalized with COVID-19 with 18* selected underlying medical conditions,† by age and disability eligibility§ — United States, January 1, 2020–November 20, 2021
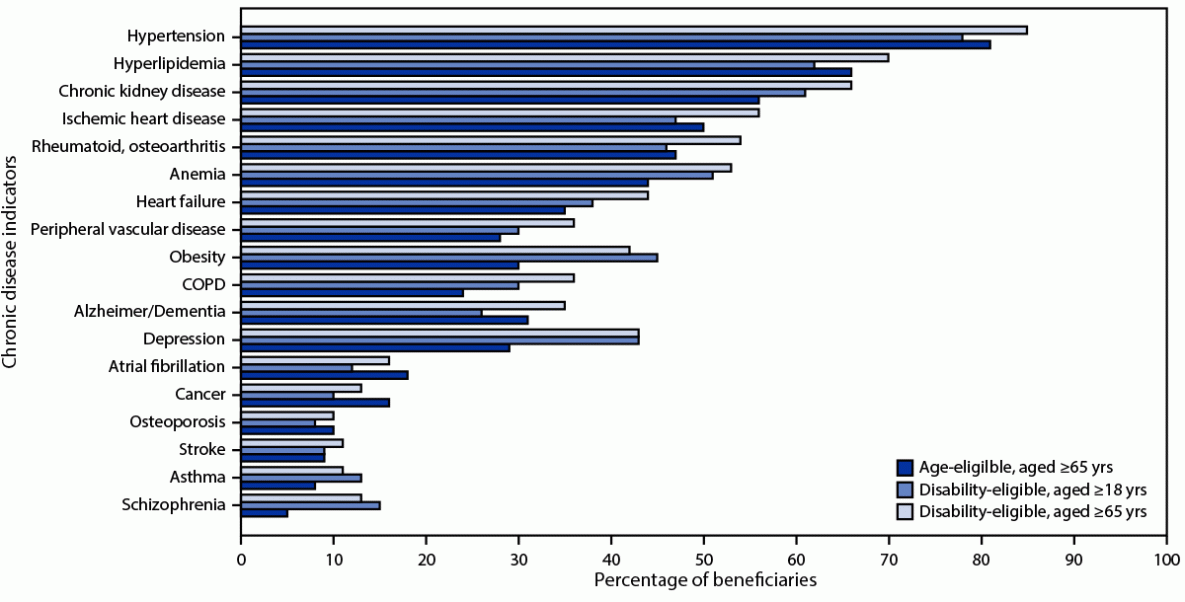
Abbreviation: COPD = chronic obstructive pulmonary disease.
* Eighteen underlying medical conditions: Alzheimer disease and dementia, anemia, asthma, atrial fibrillation, cancer (breast, colorectal, leukemia and lymphoma, lung, and prostate), chronic kidney disease, COPD and bronchiectasis, depression, heart failure, hyperlipidemia, hypertension, ischemic heart disease, obesity, osteoporosis, peripheral vascular disease, rheumatoid and osteoarthritis, schizophrenia, and stroke.
† Data on underlying medical conditions were only available for full fee-for-service beneficiaries who had 12 months of Medicare Part A and B coverage (or coverage until time of death) and no Medicare Advantage Plans coverage during 2020. The chronic disease indicators presented in the figure are a subset of the conditions from the Chronic Conditions Data Warehouse. https://www2.ccwdata.org/web/guest/home/
§ Age-eligible beneficiaries were aged ≥65 years and had no disability; disability-eligible beneficiaries were aged ≥18 years and had one or more disabilities.
Suggested citation for this article: Yuan Y, Thierry JM, Bull-Otterson L, et al. COVID-19 Cases and Hospitalizations Among Medicare Beneficiaries With and Without Disabilities — United States, January 1, 2020–November 20, 2021. MMWR Morb Mortal Wkly Rep 2022;71:791–796. DOI: http://dx.doi.org/10.15585/mmwr.mm7124a3.
MMWR and Morbidity and Mortality Weekly Report are service marks of the U.S. Department of Health and Human Services.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All HTML versions of MMWR articles are generated from final proofs through an automated process. This conversion might result in character translation or format errors in the HTML version. Users are referred to the electronic PDF version (https://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.