Pediatric Emergency Department Visits Associated with Mental Health Conditions Before and During the COVID-19 Pandemic — United States, January 2019–January 2022
Weekly / February 25, 2022 / 71(8);319–324
On February 18, 2022, this report was posted online as an MMWR Early Release.
Lakshmi Radhakrishnan, MPH1; Rebecca T. Leeb, PhD2; Rebecca H. Bitsko, PhD2; Kelly Carey, MPH1; Abigail Gates, MSPH1; Kristin M. Holland, PhD3; Kathleen P. Hartnett, PhD1; Aaron Kite-Powell, MS1; Jourdan DeVies, MS4; Amanda R. Smith, PhD1,5; Katharina L. van Santen, MSPH4; Sophia Crossen, MS6; Michael Sheppard, MS1; Samantha Wotiz, MPH7; Rashon I. Lane, PhD8; Rashid Njai, PhD9; Amelia G. Johnson, DrPH10; Amber Winn, MPH10; Hannah L. Kirking, MD10; Loren Rodgers, PhD1; Craig W. Thomas, PhD11; Karl Soetebier, MAPW1; Jennifer Adjemian, PhD1; Kayla N. Anderson, PhD12 (View author affiliations)
View suggested citationSummary
What is already known about this topic?
The proportion of pediatric emergency department (ED) visits for mental health conditions (MHCs) increased during 2020.
What is added by this report?
Weekly ED visits among adolescent females (aged 12–17 years) increased for two MHCs (eating and tic disorders) during 2020, four (depression, eating, tic, and obsessive-compulsive disorders) during 2021, and five (anxiety; trauma and stressor-related; eating; tic; and obsessive-compulsive disorders) and overall MHC visits during January 2022, compared with 2019. The proportion of ED visits with eating disorders doubled among adolescent females; those for tic disorders approximately tripled during the pandemic.
What are the implications for public health practice?
Early identification and expanded evidence-based prevention and intervention strategies are critical to improving pediatric mental health, especially among adolescent females, who might have increased need.
Altmetric:

In 2021, a national emergency* for children’s mental health was declared by several pediatric health organizations, and the U.S. Surgeon General released an advisory† on mental health among youths. These actions resulted from ongoing concerns about children’s mental health in the United States, which was exacerbated by the COVID-19 pandemic (1,2). During March–October 2020, among all emergency department (ED) visits, the proportion of mental health-related visits increased by 24% among U.S. children aged 5–11 years and 31% among adolescents aged 12–17 years, compared with 2019 (2). CDC examined changes in U.S. pediatric ED visits for overall mental health conditions (MHCs) and ED visits associated with specific MHCs (depression; anxiety; disruptive behavioral and impulse-control disorders; attention-deficit/hyperactivity disorder; trauma and stressor-related disorders; bipolar disorders; eating disorders; tic disorders; and obsessive-compulsive disorders [OCD]) during 2019 through January 2022 among children and adolescents aged 0–17 years, overall and by sex and age. After declines in weekly visits associated with MHCs among those aged 0–17 years during 2020, weekly numbers of ED visits for MHCs overall and for specific MHCs varied by age and sex during 2021 and January 2022, when compared with corresponding weeks in 2019. Among adolescent females aged 12–17 years, weekly visits increased for two of nine MHCs during 2020 (eating disorders and tic disorders), for four of nine MHCs during 2021 (depression, eating disorders, tic disorders, and OCD), and for five of nine MHCs during January 2022 (anxiety, trauma and stressor-related disorders, eating disorders, tic disorders, and OCD), and overall MHC visits during January 2022, compared with 2019. Early identification and expanded evidence-based prevention and intervention strategies are critical to improving children’s and adolescents’ mental health (1–3), especially among adolescent females, who might have increased need.
CDC examined data from the National Syndromic Surveillance Program (NSSP)§ using three pandemic surveillance periods following the declaration of a national COVID-19 emergency on March 13, 2020: March 15, 2020–January 2, 2021 (2020); January 3, 2021–January 1, 2022 (2021); and January 2, 2022–January 29, 2022 (January 2022). These periods were compared with corresponding weeks in 2019, from facilities consistently reporting data during 2019–2022.¶ Keyword syndromes** using reported reason for visit (chief complaint) and administrative diagnosis codes were developed and validated by CDC in partnership with state, tribal, local, and territorial health departments (Supplementary Box, https://stacks.cdc.gov/view/cdc/114477). To quantify change over time, CDC calculated the percent change in mean number of weekly ED visits†† for children and adolescents aged 0–17 years, as well as by age group (0–4, 5–11, and 12–17 years) and sex. To describe changes in visit volume reported to NSSP, CDC classified the percent change in visits as decreasing (less than a −10% change), stable (−10% to 10% change), or increasing >10% change). Visit ratios (VRs)§§ with 95% CIs were calculated; CIs that excluded 1 were considered statistically significant. Analyses were conducted using R software (version 4.1.2; R Foundation). This activity was reviewed by CDC and was conducted consistent with applicable federal law and CDC policy.¶¶
Average weekly visits for overall MHCs*** among all children and adolescents (aged 0–17 years) decreased during 2020 (–27%) and were stable during 2021 (–8%) and January 2022 (–5%) compared with 2019, with differences by sex (Figure 1) (Supplementary Table, https://stacks.cdc.gov/view/cdc/114477). However, visits for overall MHCs among all children and adolescents accounted for a larger proportion of all pediatric visits during 2020, 2021, and January 2022 than during 2019, with variation by age group and MHC. By age group and sex, female adolescents aged 12–17 years accounted for the largest increases in the number and proportion of visits for overall MHCs and specific MHCs during all periods compared with 2019 (Supplementary Figure 1, https://stacks.cdc.gov/view/cdc/114477). The number of weekly visits for overall MHCs and specific MHCs mostly decreased for males aged 0–17 years and for children aged 0–4 and 5–11 years across surveillance periods; the proportion of ED visits for males and younger children varied by MHCs and surveillance period (Supplementary Table; https://stacks.cdc.gov/view/cdc/114477) (Supplementary Figure 2, https://stacks.cdc.gov/view/cdc/114477). The volume of visits was low for overall MHCs and for specific MHCs among children aged 0–4 years.
With regard to specific MHCs, weekly visits for tic disorders among girls aged 5–11 years increased during 2020, 2021, and in January 2022, compared with 2019, as did the proportion of visits for tic disorders (VR = 3.04, 2.03, and 2.16, respectively); this pattern was not found among children aged 5–11 years overall or among boys within this age group (Supplementary Table, https://stacks.cdc.gov/view/cdc/114477) (Supplementary Figure 2, https://stacks.cdc.gov/view/cdc/114477).
Among adolescents aged 12–17 years, weekly visits increased among females for two of nine MHCs in 2020 (eating and tic disorders); four of nine MHCs during 2021 (depression, eating and tic disorders, and OCD); and five of nine MHCs during January 2022 (anxiety, trauma and stressor-related, eating and tic disorders, and OCD) and overall MHC visits during January 2022, compared with 2019 (Figure 1) (Figure 2) (Supplementary Table, https://stacks.cdc.gov/view/cdc/114477) (Supplementary Figure 1, https://stacks.cdc.gov/view/cdc/114477). Whereas the proportion of visits varied by MHC and surveillance period compared with 2019, the proportion of visits for eating disorders among adolescent females increased during 2020, 2021, and January 2022 (VR = 1.95, 2.29, and 1.99, respectively) as did those for tic disorders (VR = 3.65, 3.94, and 2.96 respectively).
Discussion
Following declines in weekly visits associated with MHCs among children and adolescents aged 0–17 years, during 2020 compared with 2019, weekly ED visits for MHCs overall and for specific MHCs varied by age and sex during 2021 and in January 2022. The current trends in the number and proportion of MHC-related ED visits, along with previous research (1,2,4–8), indicate that the mental health effects of the pandemic might be particularly high among adolescent girls.
Increases in weekly visits for eating and tic disorders for females, and particularly among adolescent females aged 12–17 years during 2020, 2021, and in January 2022, could represent an overall increase in distress among females during the pandemic. Both eating and tic disorders can co-occur with anxiety, depression, and OCD (1,4–7). Eating disorders can be triggered by pandemic-related risk factors (e.g., lack of structure in daily routine, emotional distress, and changes in food availability) or exacerbated by reduced access to mental health care during the pandemic (4,5). Increases in visits for tic disorders among adolescent females are atypical; tic disorders usually begin earlier in childhood and are more prevalent among males (6,7). Stress of the pandemic or exposure to severe tics, highlighted on social media platforms, might be associated with increases in visits with tics and tic-like behavior among adolescent females (6). In general, the number of MHC-related visits decreased for adolescent males aged 12–17 years during 2020, 2021, and in January 2022, but there was variation in the proportion of MHCs of all ED visits by pandemic year and specific MHC. These sex differences might represent differences in need, recognition, and health care–seeking behavior. Systemic changes, such as increasing access to available tools††† and mental health services can improve emotional well-being during and after crises among children and adolescents (3).
EDs are often the access point of care for pediatric mental health emergencies. Declines in MHC-related visits during 2020 align with previous research (2), and with reported declines in overall volume of pediatric ED visits during the pandemic (8). During 2021 and January 2022, visits for overall MHCs were stable among children and adolescents aged 0–17 years but accounted for a larger proportion of all ED visits compared with 2019. Concerns about ED capacity and potential spread of COVID-19 might have contributed to a delay in seeking health care; thus, ED visits related to MHCs during the pandemic might underestimate the actual need and represent more severe presentations of MHCs than if earlier intervention and treatment were available (5).
The highly complex nature of individual experiences makes it difficult to identify a single reason for changes in MHCs during the pandemic. Although prolonged time at home could have increased familial support and identification of mental health care needs for some youths, it might have amplified adversities and stressors among others.§§§ Exposure to adverse childhood experiences,¶¶¶ such as loss of parents and caregivers, increases in parental mental health challenges and substance use (9), and financial vulnerabilities**** might have been exacerbated by the pandemic and are associated with poor mental health outcomes among children and adolescents. As of June 2021, approximately 140,000 U.S. children and adolescents had lost parents and caregivers to COVID-19 (10). In addition, the pandemic disrupted social and physical activities: many adolescents have experienced substantial disruption to daily and academic routines, faced uncertainty and loneliness, and increased social media use (3–7,9). These factors could have created or exacerbated risk for MHCs among children and adolescents. Promoting policies to improve access to mental health services, including telemental health, and community-based primary prevention strategies to reduce exposure to adverse childhood experiences can help mitigate risk for MHCs before they begin (3,9).
The findings of this study are subject to at least five limitations. First, findings might differ from other studies based on the method of assessing ED visits for health effects. Second, these cross-sectional data cannot be used to make causal inferences for changes in visit trends, draw conclusions about the acute versus chronic presentation of MHC visits within EDs, or distinguish between visits where MHCs are primary reason for visit versus those where MHCs are present but might not be the sole reason for the visit. Third, estimates for the youngest age group (0–4 years) should be interpreted with caution because of small numbers of weekly visits. Fourth, fluctuations in underlying data quality, coding practices, and variations in lengths of surveillance periods, particularly during 2022, might not be reflective of trends from a longer period, potentially over- or underrepresenting visit trends. To account for this, only facilities with more complete data during the period of study were included. Finally, NSSP ED visit data are a convenience sample and should not be considered nationally representative. However, surveillance periods were compared with corresponding weeks in 2019 from facilities consistently reporting data during 2019–January 2022, and numbers of EDs remained relatively constant over time.
Implementing evidence-based primary prevention, early identification, and intervention, and treatment strategies that promote physical and mental health among children and adolescents and that can be rapidly adapted during public health emergencies, can help prevent MHCs and improve pediatric health (1–3). CDC supports efforts to promote the emotional well-being of children and adolescents and provides resources for clinicians,†††† families,§§§§ schools,¶¶¶¶ and communities.*****
Acknowledgments
National Syndromic Surveillance Program Community of Practice (NSSP CoP); NSSP CoP Syndrome Definition Committee and Council of State and Territorial Epidemiologists; Dylan Johns, Zachary Stein, Barbara Lopes-Cardozo, Matthew D. Ritchey, Umed A. Ajani, Paula Yoon.
Corresponding author: Lakshmi Radhakrishnan, LRadhakrishnan@cdc.gov.
1Division of Health Informatics and Surveillance, Center for Surveillance, Epidemiology, and Laboratory Services, CDC; 2Division of Human Development and Disability, National Center on Birth Defects and Developmental Disabilities, CDC; 3Division of Overdose Prevention, National Center for Injury Prevention and Control, CDC; 4ICF International, Fairfax, Virginia; 5Epidemic Intelligence Service, CDC; 6InductiveHealth Informatics, Atlanta, Georgia; 7Deloitte, Atlanta, Georgia; 8Division of STD Prevention, National Center for HIV, Viral Hepatitis, STD, & TB Prevention, CDC; 9Office of Minority Health and Health Equity, Office of the Deputy Director for Public Health Service and Implementation, CDC; 10Division of Viral Diseases, National Center for Immunization and Respiratory Diseases, CDC; 11Division of Population Health, National Center for Chronic Disease Prevention and Health Promotion, CDC; 12Division of Violence Prevention, National Center for Injury Prevention and Control, CDC.
All authors have completed and submitted the International Committee of Medical Journal Editors form for disclosure of potential conflicts of interest. No potential conflicts of interest were disclosed.
† https://www.hhs.gov/sites/default/files/surgeon-general-youth-mental-health-advisory.pdf
§ NSSP is a collaboration among CDC, local, and state health departments, and federal, academic, and private sector partners. https://www.cdc.gov/nssp/index.html
¶ To reduce artifactual impact from changes in reporting patterns, analyses were restricted to facilities with a coefficient of variation ≤40 and average weekly informative discharge diagnosis ≥75% complete during 2019–2022.
** NSSP collects free-text reason for visit (chief complaint), discharge diagnosis, and patient demographic details. Diagnosis information is collected using codes from the International Classification of Diseases, Ninth Revision, Clinical Modification, International Classification of Diseases, Tenth Revision, Clinical Modification, and Systematized Nomenclature of Medicine. Free-text keywords and diagnostic codes combined using Boolean searches were used to create distinct keyword syndromes to identify visits associated with overall MHCs and nine distinct disorders (anxiety; depression; attention-deficit/hyperactivity; bipolar; disruptive behavioral and impulse-control; eating; obsessive-compulsive; tic; trauma and stressor-related). The overall MHC keyword syndrome captures any mental health-related visits, nine individual mental disorders, schizophrenia spectrum disorders, some additional low prevalence mental health conditions (e.g., reactive attachment disorder, delusional disorders, and somatoform disorders), and general mental health terms and codes.
†† Percent change in visits per week during each surveillance period was calculated as ([mean weekly ED visits with health outcome during surveillance period − mean weekly ED visits with health outcome during comparison period] / mean weekly ED visits with health outcome during comparison period) × 100.
§§ VRs = (ED visits with health outcome [surveillance period] / all ED visits [surveillance period]) / (ED visits with health outcome [comparison period] / all ED visits [comparison period]). Ratios >1 indicate a higher proportion of ED visits with the health outcome during the surveillance period than the comparison period; ratios 1 indicate a higher proportion of ED visits with health outcome during the surveillance period for females compared with males.
¶¶ 45 C.F.R. part 46.102(l)(2), 21 C.F.R. part 56; 42 U.S.C. Sect. 241(d); 5 U.S.C. Sect. 552a; 44 U.S.C. Sect. 3501 et seq
*** Overall MHCs keyword syndrome captures any mental health–related visit, nine individual mental disorders, schizophrenia spectrum disorders, some additional low prevalence mental health conditions (e.g., reactive attachment disorder, delusional disorders, and somatoform disorders), and general mental health terms and codes.
††† https://www.nap.edu/resource/other/dbasse/wellbeing-tools/interactive/
§§§ https://www.aap.org/en/patient-care/family-snapshot-during-the-covid-19-pandemic/
¶¶¶ https://www.cdc.gov/violenceprevention/pdf/preventingACES.pdf
†††† https://www.cdc.gov/childrensmentalhealth/documents/access-infographic.html
§§§§ https://www.cdc.gov/mentalhealth/stress-coping/help-children-cope/index.html
¶¶¶¶ https://www.cdc.gov/healthyyouth/whatworks/what-works-safe-and-supportive-environments.htm
***** https://www.cdc.gov/violenceprevention/childabuseandneglect/essentials/
References
- Whitney DG, Peterson MD. US national and state-level prevalence of mental health disorders and disparities of mental health care use in children. JAMA Pediatr 2019;173:389–91. https://doi.org/10.1001/jamapediatrics.2018.5399 PMID:30742204
- Leeb RT, Bitsko RH, Radhakrishnan L, Martinez P, Njai R, Holland KM. Mental health-related emergency department visits among children aged <18 years during the COVID-19 pandemic—United States, January 1–October 17, 2020. MMWR Morb Mortal Wkly Rep 2020;69:1675–80. https://doi.org/10.15585/mmwr.mm6945a3 PMID:33180751
- So M, McCord RF, Kaminski JW. Policy levers to promote access to and utilization of children’s mental health services: a systematic review. Adm Policy Ment Health 2019;46:334–51. https://doi.org/10.1007/s10488-018-00916-9 PMID:30604005
- Castellini G, Cassioli E, Rossi E, et al. The impact of COVID-19 epidemic on eating disorders: a longitudinal observation of pre versus post psychopathological features in a sample of patients with eating disorders and a group of healthy controls. Int J Eat Disord 2020;53:1855–62. https://doi.org/10.1002/eat.23368 PMID:32856333
- Otto AK, Jary JM, Sturza J, et al. Medical admissions among adolescents with eating disorders during the COVID-19 pandemic. Pediatrics 2021;148:e2021052201. https://doi.org/10.1542/peds.2021-052201 PMID:34244452
- Pringsheim T, Ganos C, McGuire JF, et al. Rapid onset functional tic-like behaviors in young females during the COVID-19 pandemic. Mov Disord 2021;36:2707–13. https://doi.org/10.1002/mds.28778 PMID:34387394
- Müller-Vahl KR, Pisarenko A, Jakubovski E, Fremer C. Stop that! It’s not Tourette’s but a new type of mass sociogenic illness. Brain 2021;awab316. https://doi.org/10.1093/brain/awab316 PMID:34424292
- Adjemian J, Hartnett KP, Kite-Powell A, et al. Update: COVID-19 pandemic–associated changes in emergency department visits—United States, December 2020–January 2021. MMWR Morb Mortal Wkly Rep 2021;70:552–6. https://doi.org/10.15585/mmwr.mm7015a3 PMID:33857069
- McKnight-Eily LR, Okoro CA, Strine TW, et al. Racial and ethnic disparities in the prevalence of stress and worry, mental health conditions, and increased substance use among adults during the COVID-19 pandemic—United States, April and May 2020. MMWR Morb Mortal Wkly Rep 2021;70:162–6. https://doi.org/10.15585/mmwr.mm7005a3 PMID:33539336
- Hillis SD, Blenkinsop A, Villaveces A, et al. COVID-19–associated orphanhood and caregiver death in the United States. Pediatrics 2021;148:e2021053760. https://doi.org/10.1542/peds.2021-053760
 FIGURE 1. Weekly number of emergency department visits* for overall mental health conditions† among children and adolescents aged 0–17 years, by sex — National Syndromic Surveillance Program, United States, 2019–2022
FIGURE 1. Weekly number of emergency department visits* for overall mental health conditions† among children and adolescents aged 0–17 years, by sex — National Syndromic Surveillance Program, United States, 2019–2022
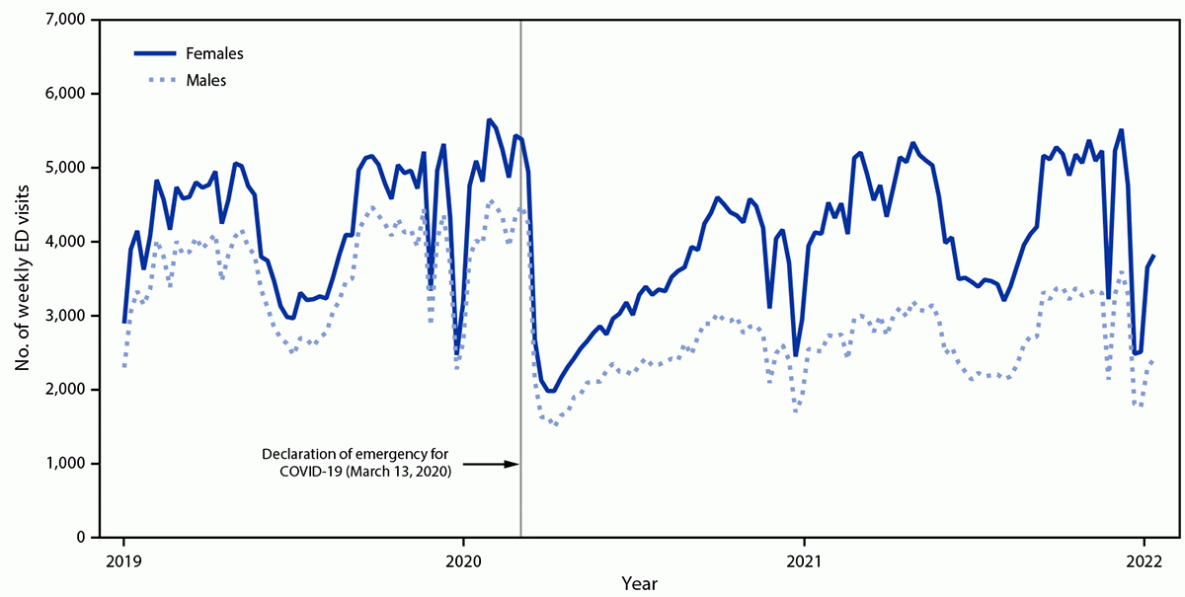
Abbreviations: ED = emergency department; ICD-9-CM = International Classification of Diseases, Ninth Revision, Clinical Modification; ICD-10-CM = International Classification of Diseases, Tenth Revision, Clinical Modification; MHC = mental health condition; NSSP = National Syndromic Surveillance Program; SNOMED = Systematized Nomenclature of Medicine.
* NSSP receives anonymized medical record information from approximately 71% of nonfederal EDs nationwide. To reduce artifactual impact from changes in reporting patterns, analyses were restricted to facilities with more consistent reporting of more complete data (coefficient of variation ≤40 and average weekly informative discharge diagnosis ≥75% complete during 2019–2022).
† NSSP collects free-text reason for visit (chief complaint), discharge diagnosis, and patient demographic details. Diagnosis information is collected using ICD-9-CM, ICD-10-CM, and SNOMED codes. Free-text keywords and diagnostic codes combined using Boolean searches were used to create a keyword syndrome to identify visits associated with overall MHCs. This keyword syndrome includes visits related to nine distinct disorders (anxiety; depression; attention-deficit/hyperactivity; bipolar; disruptive behavioral and impulse-control; eating; obsessive-compulsive; tic; and trauma and stressor-related), schizophrenia spectrum disorders, some additional low prevalence MHCs (e.g., reactive attachment disorder, delusional disorders, or somatoform disorders), and general mental health terms and codes.
 FIGURE 2. Weekly number of emergency department visits* associated with eating disorders† (A) and tic disorders (B)† among adolescents aged 12–17 years, by sex—National Syndromic Surveillance Program, United States, 2019–2022
FIGURE 2. Weekly number of emergency department visits* associated with eating disorders† (A) and tic disorders (B)† among adolescents aged 12–17 years, by sex—National Syndromic Surveillance Program, United States, 2019–2022

Abbreviations: ED = emergency department; ICD-9-CM = International Classification of Diseases, Ninth Revision, Clinical Modification; ICD-10-CM = International Classification of Diseases, Tenth Revision, Clinical Modification; NSSP = National Syndromic Surveillance Program; SNOMED = Systematized Nomenclature of Medicine.
* NSSP receives anonymized medical record information from approximately 71% of nonfederal EDs nationwide. To reduce artifactual impact from changes in reporting patterns, analyses were restricted to facilities with more consistent reporting of more complete data (coefficient of variation ≤40 and average weekly informative discharge diagnosis ≥75% complete during 2019–2022).
† NSSP collects free-text reason for visit (chief complaint), discharge diagnosis, and patient demographic details. Diagnosis information is collected using ICD-9-CM, ICD-10-CM, and SNOMED codes. Free-text keywords and diagnostic codes combined using Boolean searches were used to create a keyword syndrome to identify visits associated with eating and tic disorders.
Suggested citation for this article: Radhakrishnan L, Leeb RT, Bitsko RH, et al. Pediatric Emergency Department Visits Associated with Mental Health Conditions Before and During the COVID-19 Pandemic — United States, January 2019–January 2022. MMWR Morb Mortal Wkly Rep 2022;71:319–324. DOI: http://dx.doi.org/10.15585/mmwr.mm7108e2.
MMWR and Morbidity and Mortality Weekly Report are service marks of the U.S. Department of Health and Human Services.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All HTML versions of MMWR articles are generated from final proofs through an automated process. This conversion might result in character translation or format errors in the HTML version. Users are referred to the electronic PDF version (https://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.