Notes from the Field: Phenibut Exposures Reported to Poison Centers — United States, 2009–2019
Weekly / September 4, 2020 / 69(35);1227–1228
Janessa M. Graves, PhD1; Julia Dilley, PhD2; Sanjay Kubsad3; Erica Liebelt, MD4 (View author affiliations)
View suggested citationPhenibut (β-phenyl-γ-aminobutyric acid) is an unregulated* drug developed in Russia in the 1960s for use as an antianxiety medication with cognitive enhancement properties (1). Online retailers recently have contributed to a growing U.S. market for phenibut, which is advertised for anxiety, relaxation, and sleep (1,2). Phenibut use and misuse can result in sedation, respiratory depression, and reduced levels of consciousness, as well as withdrawal symptoms including anxiety, agitation, and acute psychosis (3). Regional poison center data suggest that phenibut exposures have increased in recent years (3). To characterize the frequency of phenibut-related exposures in the United States, data on human exposure calls to U.S. poison centers during January 2009–December 2019 were extracted from the national database maintained by the American Association of Poison Control Centers.†
Phenibut exposures were identified as poison center calls involving human exposure to phenibut; searches included synonyms (i.e., phenygam or 4-amino-3-phenylbutyric acid)§ (4). Exposures do not necessarily represent a poisoning or overdose. All exposure calls involving single or multiple substances were included¶; calls requesting information on phenibut were not included. The analysis summarized the demographic characteristics, caller location (e.g., health care facility or residence), exposure routes, clinical health effects, and outcomes.
For each poison center call, a case record for a single exposure event (case) is generated, delineating the patient’s history, physical examination, clinical assessment, and recommendations provided. Health care providers (e.g., nurses, pharmacists, and physicians) provide ongoing case management through follow-up calls until the acute toxicologic condition has resolved; therefore, each case might involve more than one call. Multiple data elements are recorded (e.g., reason for poisoning, patient age, substances, clinical effects, therapies, and medical outcomes), as determined by the providers managing the exposures at each poison center. Health care providers managing cases identify the exposure agents by manufacturer name or synonym. Providers use standard National Poison Data System definitions to enable consistent reporting among poison centers and across years of data.
During 2009–2019, U.S. poison centers reported calls for 1,320 phenibut exposures from all 50 U.S. states and the District of Columbia. For most (1,122; 85.0%) cases, calls originated from health care facilities. Most exposures (58.4%) occurred among adults aged 18–34 years (mean = 31.7 years, standard deviation = 13.1 years, interquartile range = 22–38 years). The majority of reported exposures were in men (75.5%).
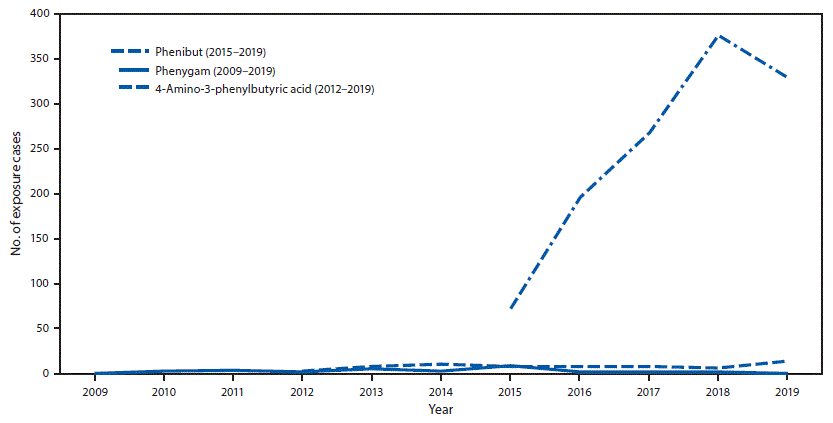
The number of cases increased sharply over the study period, particularly since 2015, when regional poison centers became able to use “phenibut” as a relevant term to capture exposures (Figure). Phenibut exposures with known formulations most often involved solids (e.g., tablets) (65.1%) or powder (24.8%). Reported exposures were predominantly ingestions (93.2%), although 2.8% involved inhalation, and 4.0% involved other routes of exposure, including dermal. Unintentional exposures were more common among persons aged <18 years (21.9%). A significantly higher percentage of exposures among children aged <10 years (93.3%) was unintentional, compared with 6.3% of those among adults (p<0.001). Coingested substances (i.e., exposure to more than one drug or agent) were reported in 29.6% of cases in persons aged <18 years and in 40.2% of all adult cases (p = 0.04).
Commonly reported adverse health effects included drowsiness or lethargy (29.0%), agitation (30.4%), tachycardia (21.9%), and confusion (21.3%). Coma was reported in 80 (6.2%) cases, including one involving an adolescent. In one half (49.6%) of cases, the exposure resulted in moderate effects (i.e., no long-term impairment). Major effects (i.e., life-threatening or resulting in significant disability or disfigurement) occurred in one in eight (12.6%) reported exposures, and three deaths were reported. Among exposures in which phenibut was the only drug or agent involved, 10.2% were associated with major effects, including one death.
The reason for the increase in phenibut-related exposures during 2009–2019 is not known; growing popularity and availability of the product through online retailers might be contributing factors. The increase in phenibut exposures underscores the need for heightened awareness of phenibut as an emerging substance of use and misuse in the United States. Adverse health effects reported to poison centers, such as drowsiness or lethargy, agitation, and confusion, are consistent with those described in previous reports (3). Exposures were associated with long-term health effects, including death. Easy online access to phenibut (2) and the potential for dependence (5) are additional reasons for concern. Phenibut is uncontrolled and legal to possess in the United States. Educational efforts to increase awareness among the public and clinicians regarding the emerging popularity and dangers of phenibut might help prevent adverse health effects and outcomes, including death.
Acknowledgments
Nathaniel Pham, American Association of Poison Control Centers; Washington State University Alcohol and Drug Abuse Program.
Corresponding author: Janessa Graves, janessa.graves@wsu.edu, 509-324-7257.
1Washington State University, College of Nursing, Spokane, Washington; 2Oregon Health Authority Public Health Division & Multnomah County Health Department, Portland, Oregon; 3University of Washington, School of Medicine, Seattle, Washington; 4Washington State Poison Center, Seattle, Washington.
All authors have completed and submitted the International Committee of Medical Journal Editors form for disclosure of potential conflicts of interest. No potential conflicts of interest were disclosed.
* In the United States, phenibut is legal to possess, but not approved as a licensed pharmaceutical drug by the Food and Drug Administration (FDA). Although it is available for purchase online as a nutritional supplement, FDA has ruled that phenibut does not meet the definition of a dietary ingredient and cannot be listed as an ingredient in dietary supplements marketed in the United States (https://www.fda.gov/food/dietary-supplement-products-ingredients/phenibut-dietary-supplements). FDA does analyze the content of phenibut-containing products, including the strength and purity of ingredients; few studies have been published describing the purity of phenibut-containing products.
† Data reflect information provided when an actual or potential exposure to a substance is reported. The American Association of Poison Control Centers is not able to verify the accuracy of every report made to member centers. Additional exposures might not be reported, and these data might not represent the complete incidence of national exposures to any substance.
§ Phenibut has been reported as “phenygam” in the National Poison Data System database since before the study timeline; “4-amino-3-phenylbutyric acid” and “phenibut” were added in 2012 and 2015, respectively.
¶ Phenibut exposures are not confirmed by laboratory testing; no commercially available test is available and phenibut is not detected on routine urine drug screens.
References
- Owen DR, Wood DM, Archer JR, Dargan PI. Phenibut (4-amino-3-phenyl-butyric acid): availability, prevalence of use, desired effects and acute toxicity. Drug Alcohol Rev 2016;35:591–6. CrossRef PubMed
- Wong A, Little M, Caldicott D, Easton C, Andres D, Greene SL. Analytically confirmed recreational use of phenibut (β-phenyl-γ-aminobutyric acid) bought over the internet. Clin Toxicol (Phila) 2015;53:783–4. CrossRef PubMed
- McCabe DJ, Bangh SA, Arens AM, Cole JB. Phenibut exposures and clinical effects reported to a regional poison center. Am J Emerg Med 2019;37:2066–71. CrossRef PubMed
- National Library of Medicine. 4-Amino-3-phenylbutyric acid. Bethesda, MD: National Library of Medicine; 2020. https://druginfo.nlm.nih.gov/drugportal/rn/1078-21-3
- Jouney EA. Phenibut (β-phenyl-γ-aminobutyric acid): an easily obtainable “dietary supplement” with propensities for physical dependence and addiction. Curr Psychiatry Rep 2019;21:23. CrossRef PubMed
 FIGURE. Number of human exposure cases related to phenibut use reported to poison centers, by year — National Poison Data System, United States, January 2009–December 2019
FIGURE. Number of human exposure cases related to phenibut use reported to poison centers, by year — National Poison Data System, United States, January 2009–December 2019
Suggested citation for this article: Graves JM, Dilley J, Kubsad S, Liebelt E. Notes from the Field: Phenibut Exposures Reported to Poison Centers — United States, 2009–2019. MMWR Morb Mortal Wkly Rep 2020;69:1227–1228. DOI: http://dx.doi.org/10.15585/mmwr.mm6935a5.
MMWR and Morbidity and Mortality Weekly Report are service marks of the U.S. Department of Health and Human Services.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All HTML versions of MMWR articles are generated from final proofs through an automated process. This conversion might result in character translation or format errors in the HTML version. Users are referred to the electronic PDF version (https://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.