Hydroxychloroquine and Chloroquine Prescribing Patterns by Provider Specialty Following Initial Reports of Potential Benefit for COVID-19 Treatment — United States, January–June 2020
Weekly / September 4, 2020 / 69(35);1210–1215
Lara Bull-Otterson, PhD1,2; Elizabeth B. Gray, MPH2; Daniel S. Budnitz, MD3,4; Heather M. Strosnider, PhD1,5; Lyna Z. Schieber, MD, DPhil1,6; Joseph Courtney, PhD1,5; Macarena C. García, DrPH1,7; John T. Brooks, MD8; William R. Mac Kenzie, MD1,7; Adi V. Gundlapalli, MD, PhD1,9 (View author affiliations)
View suggested citationSummary
What is already known about this topic?
Hydroxychloroquine and chloroquine are approved to treat autoimmune diseases and to prevent and treat malaria. Earlier this year, they were widely reported to be of potential benefit in the prevention and treatment of COVID-19; however, current data indicate that the potential benefits of these drugs do not outweigh their risks.
What is added by the report?
New prescriptions by specialists who did not typically prescribe these medications (defined as specialties accounting for ≤2% of new prescriptions before 2020) increased from 1,143 prescriptions in February 2020 to 75,569 in March 2020, an 80-fold increase from March 2019.
What are the implications for public health practice?
Attention to updated clinical guidance, especially by nonroutine prescribers, will help safeguard supplies and ensure safe use of hydroxychloroquine and chloroquine for patients with approved indications.
Hydroxychloroquine and chloroquine, primarily used to treat autoimmune diseases and to prevent and treat malaria, received national attention in early March 2020, as potential treatment and prophylaxis for coronavirus disease 2019 (COVID-19) (1). On March 20, the Food and Drug Administration (FDA) issued an emergency use authorization (EUA) for chloroquine phosphate and hydroxychloroquine sulfate in the Strategic National Stockpile to be used by licensed health care providers to treat patients hospitalized with COVID-19 when the providers determine the potential benefit outweighs the potential risk to the patient.* Following reports of cardiac and other adverse events in patients receiving hydroxychloroquine for COVID-19 (2), on April 24, 2020, FDA issued a caution against its use† and on June 15, rescinded its EUA for hydroxychloroquine from the Strategic National Stockpile.§ Following the FDA’s issuance of caution and EUA rescindment, on May 12 and June 16, the federal COVID-19 Treatment Guidelines Panel issued recommendations against the use of hydroxychloroquine or chloroquine to treat COVID-19; the panel also noted that at that time no medication could be recommended for COVID-19 pre- or postexposure prophylaxis outside the setting of a clinical trial (3). However, public discussion concerning the effectiveness of these drugs on outcomes of COVID-19 (4,5), and clinical trials of hydroxychloroquine for prophylaxis of COVID-19 continue.¶ In response to recent reports of notable increases in prescriptions for hydroxychloroquine or chloroquine (6), CDC analyzed outpatient retail pharmacy transaction data to identify potential differences in prescriptions dispensed by provider type during January–June 2020 compared with the same period in 2019. Before 2020, primary care providers and specialists who routinely prescribed hydroxychloroquine, such as rheumatologists and dermatologists, accounted for approximately 97% of new prescriptions. New prescriptions by specialists who did not typically prescribe these medications (defined as specialties accounting for ≤2% of new prescriptions before 2020) increased from 1,143 prescriptions in February 2020 to 75,569 in March 2020, an 80-fold increase from March 2019. Although dispensing trends are returning to prepandemic levels, continued adherence to current clinical guidelines for the indicated use of these medications will ensure their availability and benefit to patients for whom their use is indicated (3,4), because current data on treatment and pre- or postexposure prophylaxis for COVID-19 indicate that the potential benefits of these drugs do not appear to outweigh their risks.
Hydroxychloroquine and chloroquine prescriptions dispensed through outpatient retail pharmacies in the United States during January–June 2019 and January–June 2020 were examined using deidentified pharmacy transactions from the IQVIA National Prescription Audit database.** This database includes 92% of all outpatient retail prescriptions dispensed in the United States; prescription estimates were projected by IQVIA to represent all retail outpatient medication dispensing at the state and national levels.
New prescriptions for hydroxychloroquine and chloroquine were defined as those dispensed to a patient without a history of prescription for these medications in the preceding 12 months. Hydroxychloroquine accounted for approximately 99% of prescriptions dispensed during the study period. Refill/switch prescriptions were defined as those dispensed either as a refill of a previous prescription or as a new prescription with a change in medication strength or brand or switches between medications within the same therapeutic category (i.e., bidirectional switches of hydroxychloroquine and chloroquine). New and refill/switch prescriptions dispensed before reports of potential benefit on medication use for COVID-19 (during January–June 2019) were compared with new and refill/switch prescriptions during January–June 2020. Fold changes in the numbers of new prescriptions were calculated and defined as the ratio between the estimated number of prescriptions in March, April, May, and June 2020, with respect to the same months in 2019. The percentage of total dispensed prescriptions by specialty group was calculated using the total number of dispensed prescriptions by specialty group, divided by the overall total number of dispensed prescriptions for the month; the percentage of new prescriptions by a specialty group was calculated by dividing the new prescriptions dispensed for the specialty group by the total prescriptions for the specialty group. The percentage of new prescriptions dispensed to males was calculated as the number of new prescriptions for males divided by the total number of new prescriptions.
Prescriptions were not included if they were dispensed by mail order; mail-dispensed prescriptions accounted for <7.5% of dispensed hydroxychloroquine and chloroquine. Prescriptions by veterinarians were also excluded.
Prescriptions included information on the prescriber’s medical specialty, as defined by the American Medical Association (AMA) self-designated practice specialties.†† For this study, clinicians prescribing hydroxychloroquine or chloroquine were categorized based on the frequency of prescribing of hydroxychloroquine or chloroquine before the COVID-19 pandemic. Specialists from rheumatology, dermatology, allergy, and nephrology, who might have had experience using these drugs for indicated medical conditions within their specialty before the pandemic (collectively termed routine prescribers) were responsible for 62% of new hydroxychloroquine or chloroquine prescriptions in 2019. Allopathic and osteopathic physicians, who included internal medicine, family practice, general practice, and pediatrics, and nurse practitioners, physician assistants, and prescribers with unspecified specialty (per AMA classification) were grouped for this study into primary care prescribers; this group provided 35% of the new prescriptions in 2019. Other specialists were considered nonroutine prescribers§§ if, in 2019, their specialty prescribed ≤2% of hydroxychloroquine or chloroquine prescriptions. Nonroutine prescribing specialties are less likely under normal circumstances to directly manage patients with autoimmune disorders or provide prescriptions for malaria prophylaxis.
The overall estimated number of hydroxychloroquine or chloroquine prescriptions dispensed in March and April 2020 increased from 819,906 in 2019 to 1,312,859 in 2020 (Table). In 2019, 92% of prescriptions were refill/switch prescriptions. Refill/switch prescriptions increased 1.4-fold, from 377,222 in March 2019 to 536,804 in March 2020, and remained elevated in April (456,489; 1.2-fold higher than in April 2019) (Figure 1). New prescriptions for hydroxychloroquine or chloroquine in March 2020 (222,382) were 7.2-fold higher than the 30,737 prescriptions in March 2019; in April, the number of new prescriptions (106,184) was 3.3-fold higher than the 31,748 in April 2019 (Table).
Overall, 54% of new prescriptions in March and April 2020 were written by primary care prescribers. In March 2020, primary care prescribers wrote more new prescriptions than did routine prescribers, writing 10,350 dispensed prescriptions in 2019 compared with 108,705 in 2020, a 10.5-fold increase (Figure 2). Primary care prescribers continued to be the largest source of new prescriptions in April 2020, writing 67,055 prescriptions (63% of total new prescriptions).
During March and April 2020, nonroutine prescribers accounted for the largest percentage increase in new prescriptions compared with the same period in 2019 (81.3-fold and 18.1-fold increases in March and April, respectively). The nonroutine prescribing specialties with the highest prescribing volume and growth in March 2020 were ophthalmology, anesthesiology, and cardiology.
During March and April 2019, most new prescriptions were dispensed to females (81%). In 2020, the estimated number of total new prescriptions for males was 93,776 in March (16.1-fold higher than March 2019), and 40,055 in April (6.8-fold higher than April 2019), accounting for 42% and 38% of all new prescriptions in March and April, respectively.
In May and June 2020, refill/switch prescriptions declined but remained elevated: 436,823 in May (1.1-fold higher than May 2019) and 461,670 in June (1.3-fold higher than June 2019). New prescriptions in May 2020 declined to 37,537 (7.9%) of all dispensed hydroxychloroquine or chloroquine prescriptions, with a similar number of dispensed prescriptions (38,803; 7.8%) in June 2020. In May 2020, the percentage of new prescriptions by those in nonroutine prescribing specialties declined to 18.5% from 82.5% in March and 54.2% in April.
Discussion
In the United States, during March and April 2020, monthly hydroxychloroquine and chloroquine outpatient prescribing was higher than it was during the previous year. These medications are routinely prescribed for lupus and rheumatoid arthritis (hydroxychloroquine) and for antimalarial prophylaxis malaria treatment (chloroquine), and the annual rate of prescribing has not varied substantially from year to year (6). In contrast, new prescriptions written by primary care prescribers and nonroutine prescribing specialists increased significantly in 2020. Primary care prescribers provided 54% of new prescriptions dispensed at outpatient retail pharmacies during March–April 2020; the largest percentage increase in new prescriptions compared with the same period in 2019 was among nonroutine prescribers.
A large increase in new prescriptions occurred for adult males (16.1-fold increase in March 2020 compared with March 2019). This increase in hydroxychloroquine prescribing for males is notable given that females are historically more likely to receive a new hydroxychloroquine prescription for autoimmune disease, consistent with described prevalence of autoimmune disorders among females (78%) (7). By May and June 2020, the numbers of new prescriptions and the number of new prescriptions from nonroutine prescribing specialties had declined and were approaching those of 2019. These declines might have been influenced by publication of additional studies indicating that the medications were not found to be effective for treatment of COVID-19 and by FDA safety warning (8).
The findings in this report are subject to at least four limitations. First, mail-order prescriptions were not included in the study, nor were prescriptions given in inpatient settings, so data do not indicate total medication use nationwide. However, the data are weighted to be nationally representative, although they are based on a sample of 92% of outpatient prescriptions. Second, because specialty information was lacking for nurse practitioners, physician assistants, and unspecified specialties, these prescribers were categorized as primary care; however, it is possible that these providers were working in routine or nonroutine prescriber practices. In addition, allopathic and osteopathic physicians with internal medicine and subspecialty training potentially were not classified by subspecialty. Third, among patients receiving prescriptions, clinical indications, patients’ underlying medical conditions, and concurrent medications were unknown. Finally, no information was available to confirm whether the medication was taken or stored for future use or if any adverse events occurred.
If prescribing or prescribed these drugs, providers and patients should be familiar with the potential for drug interactions and adverse events associated with hydroxychloroquine or chloroquine use (8,9). The importance of obtaining a patient’s complete medical and medication history to evaluate risks should be emphasized to nonroutine prescribers of hydroxychloroquine or chloroquine. In the setting of polypharmacy and comorbid conditions, such as preexisting heart conditions, performing an electrocardiogram to evaluate the QT interval before starting these medications is advisable, because hydroxychloroquine or chloroquine can prolong the QT interval, leading to malignant arrhythmias such as torsade de pointes or ventricular fibrillation (9). Because of the long-terminal half-life of hydroxychloroquine (>40 days) (10), patients could continue to be at risk for drug interactions and adverse cardiac events after the course of therapy is completed.
Although federal guidelines now recommend against using hydroxychloroquine or chloroquine for the treatment or prevention of COVID-19, dispensing policies and restrictions vary significantly by state (8). Policies by boards of pharmacy in some states, such as New Jersey, require hydroxychloroquine prescriptions to include a diagnosis, documentation of a positive diagnostic test, and be limited to a 14-day supply.¶¶ In Texas, similar restrictions instituted in May expired in July.*** Several other states advise caution in prescribing hydroxychloroquine or chloroquine for COVID-19, while allowing for clinical judgement without policy limitations. Although dispensing of hydroxychloroquine or chloroquine prescriptions has been declining since March 2020, continued attention to updated clinical guidance (3,4), especially by nonroutine prescribers, will help safeguard supplies and ensure safe use of these medications for patients with approved indications.†††
Corresponding author: Lara Bull-Otterson, lbull@cdc.gov.
1Innovation, Technology, and Analytics Task Force, CDC COVID-19 Emergency Response Team; 2Division of Health Informatics and Surveillance, Center for Surveillance, Epidemiology, and Laboratory Services, CDC; 3Division of Healthcare Quality Promotion, National Center for Emerging and Zoonotic Infectious Diseases, CDC; 4Health System and Worker Safety Task Force, CDC COVID-19 Emergency Response Team; 5Division of Environmental Health Science and Practice, National Center for Environmental Health, CDC; 6Division of Overdose Prevention, National Center for Injury Prevention and Control, CDC; 7Office of the Director, Center for Surveillance, Epidemiology, and Laboratory Services, CDC; 8Chief Medical Officer, CDC COVID-19 Response Team; 9Public Health Informatics Office, Center for Surveillance, Epidemiology, and Laboratory Services, CDC.
All authors have completed and submitted the International Committee of Medical Journal Editors form for disclosure of potential conflicts of interest. No potential conflicts of interest were disclosed.
* https://www.fda.gov/media/136534/download.
§ https://www.fda.gov/media/138945/download.
¶ https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7330261/.
** IQVIA projected prescription estimates using proprietary methods and information internal to the company. https://www.iqvia.com/locations/united-states/solutions/commercial-operations/essential-information/prescription-information.
†† http://www.dmddata.com/2009_05_sdps.pdf.
§§ Nonroutine specialties included addiction medicine, allergy/immunology, anesthesiology, cardiology, cardiothoracic surgery, cardiovascular surgery, clinical neurophysiology, clinical pharmacology, colon and rectal surgery, critical care, critical care medicine, dentistry, dermatopathology, diagnostic laboratory, diagnostic laboratory immunology, emergency medicine, endocrinology, gastroenterology, general preventive medicine, general surgery, genetics, geriatric psychiatry, geriatrics, hematology, hepatology, hospice and palliative medicine, infectious disease, medical microbiology, naturopathic doctor, neurologic surgery, neurology, neurosurgery-critical care, nuclear medicine, nutrition, obstetrics/gynecology, obstetrics/gynecology-critical care, occupational medicine, oncology, ophthalmology, optometry, orthopedic surgery, orthopedic surgery of spine, other, other surgery, otolaryngology, otology, pain medicine, pathology, pediatric critical care, pediatric neurosurgery, pharmacist, physical medicine and rehab, plastic surgery, podiatry, psychiatry, psychology, pulmonary critical care, pulmonary diseases, radiology, sleep medicine, sports medicine, surgery, thoracic surgery, and urology.
¶¶ https://www.nj.gov/oag/newsreleases20/DCA_AO_2020-01.pdf.
*** https://www.pharmacy.texas.gov/files_pdf/291.30.pdf.
††† https://www.accessdata.fda.gov/scripts/drugshortages/default.cfm.
References
- Gautret P, Lagier JC, Parola P, et al. Hydroxychloroquine and azithromycin as a treatment of COVID-19: results of an open-label non-randomized clinical trial. Int J Antimicrob Agents 2020;56:105949. CrossRef PubMed
- Rosenberg ES, Dufort EM, Udo T, et al. Association of treatment with hydroxychloroquine or azithromycin with in-hospital mortality in patients with COVID-19 in New York State. JAMA 2020;323:2493–502. CrossRef PubMed
- National Institutes of Health. Coronavirus disease 2019 (COVID-19) treatment guidelines. Rockville, MD: US Department of Health and Human Services, National Institutes of Health; 2020. https://www.covid19treatmentguidelines.nih.gov/
- Arshad S, Kilgore P, Chaudhry ZS, et al.; Henry Ford COVID-19 Task Force. Treatment with hydroxychloroquine, azithromycin, and combination in patients hospitalized with COVID-19. Int J Infect Dis 2020;97:396–403. CrossRef PubMed
- Cavalcanti AB, Zampieri FG, Rosa RG, et al. Coalition Covid-19 Brazil I Investigators. Hydroxychloroquine with or without azithromycin in mild-to-moderate Covid-19. N Engl J Med 2020. Epub July 23, 2020. CrossRef
- Shehab N, Lovegrove M, Budnitz DS. US hydroxychloroquine, chloroquine, and azithromycin outpatient prescription trends, United States, October 2019–March 2020. JAMA Intern Med 2020. Epub July 6, 2020. CrossRef
- Jacobson DL, Gange SJ, Rose NR, Graham NMH. Epidemiology and estimated population burden of selected autoimmune diseases in the United States. Clin Immunol Immunopathol 1997;84:223–43. CrossRef PubMed
- Food and Drug Administration. FDA cautions against use of hydroxychloroquine or chloroquine for COVID-19 outside of the hospital setting or a clinical trial due to risk of heart rhythm problems. Silver Spring, MD: US Department of Health and Human Services, Food and Drug Administration; 2020. https://www.fda.gov/drugs/drug-safety-and-availability/fda-cautions-against-use-hydroxychloroquine-or-chloroquine-covid-19-outside-hospital-setting-or
- Asensio E, Acunzo R, Uribe W, Saad EB, Sáenz LC. Recommendations for the measurement of the QT interval during the use of drugs for COVID-19 infection treatment. Updatable in accordance with the availability of new evidence. J Interv Card Electrophysiol 2020. Epub May 16, 2020. CrossRef PubMed
- Furst DE. Pharmacokinetics of hydroxychloroquine and chloroquine during treatment of rheumatic diseases. Lupus 1996;5(Suppl 1):S11–5. CrossRef PubMed
* Prescription data for 2017 and 2018 were also examined but found consistent with 2019, without remarkable month to month variation.
† Refill/switch prescriptions include dispensed prescriptions that were either a refill or a new prescription for a different dose or a switch in brand.
§ Nonroutine = addiction medicine, allergy/immunology, anesthesiology, cardiology, cardiothoracic surgery, cardiovascular surgery, clinical neurophysiology, clinical pharmacology, colon and rectal surgery, critical care, critical care medicine, dentistry, dermatopathology, diagnostic laboratory, diagnostic laboratory immunology, emergency medicine, endocrinology, gastroenterology, general preventive medicine, general surgery, genetics, geriatric psychiatry, geriatrics, hematology, hepatology, hospice and palliative medicine, infectious disease, medical microbiology, naturopathic doctor, neurologic surgery, neurology, neurosurgery-critical care, nuclear medicine, nutrition, obstetrics/gynecology, obstetrics/gynecology-critical care, occupational medicine, oncology, ophthalmology, optometry, orthopedic surgery, orthopedic surgery of spine, other, other surgery, otolaryngology, otology, pain medicine, pathology, pediatric critical care, pediatric neurosurgery, pharmacist, physical medicine and rehab, plastic surgery, podiatry, psychiatry, psychology, pulmonary critical care, pulmonary diseases, radiology, sleep medicine, sports medicine, surgery, thoracic surgery, and urology.
¶ Primary care/unspecified = family practice, general practice, internal medicine, internal medicine/pediatrics, nurse practitioner, osteopathic medicine, pediatrics, physician assistant, and specialty unspecified.
** Routine = allergy, dermatology, nephrology, and rheumatology.
 FIGURE 1. Estimated refill/switch* and new retail prescriptions for hydroxychloroquine or chloroquine dispensed in the United States — January–June, 2019–2020
FIGURE 1. Estimated refill/switch* and new retail prescriptions for hydroxychloroquine or chloroquine dispensed in the United States — January–June, 2019–2020
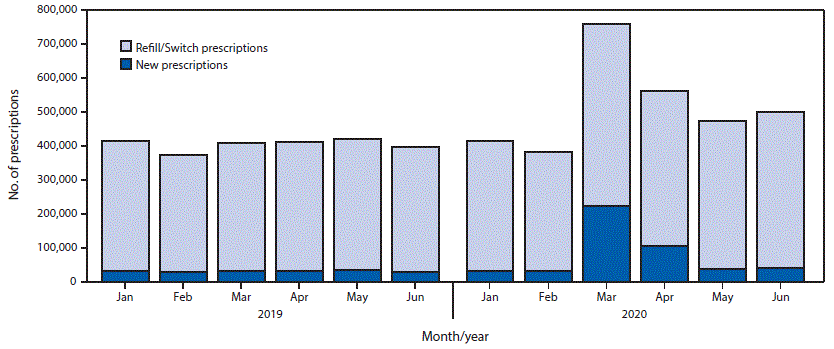
* Refill/switch prescriptions include dispensed prescriptions that were either a refill of an existing prescription or a new prescription for a different dose or a brand switch.
 FIGURE 2. Estimated new retail prescriptions of hydroxychloroquine or chloroquine dispensed, by prescriber category* — United States, January–June, 2019–2020
FIGURE 2. Estimated new retail prescriptions of hydroxychloroquine or chloroquine dispensed, by prescriber category* — United States, January–June, 2019–2020

* Nonroutine prescribers = addiction medicine, allergy/immunology, anesthesiology, cardiology, cardiothoracic surgery, cardiovascular surgery, clinical neurophysiology, clinical pharmacology, colon and rectal surgery, critical care, critical care medicine, dentistry, dermatopathology, diagnostic laboratory, diagnostic laboratory immunology, emergency medicine, endocrinology, gastroenterology, general preventive medicine, general surgery, genetics, geriatric psychiatry, geriatrics, hematology, hepatology, hospice and palliative medicine, infectious disease, medical microbiology, naturopathic doctor, neurological surgery, neurology, neurosurgery-critical care, nuclear medicine, nutrition, obstetrics/gynecology, obstetrics/gynecology-critical care, occupational medicine, oncology, ophthalmology, optometry, orthopedic surgery, orthopedic surgery of spine, other, other surgery, otolaryngology, otology, pain medicine, pathology, pediatric critical care, pediatric neurosurgery, pharmacist, physical medicine and rehab, plastic surgery, podiatry, psychiatry, psychology, pulmonary critical care, pulmonary diseases, radiology, sleep medicine, sports medicine, surgery, thoracic surgery, and urology. Primary care/unspecified prescribers = family practice, general practice, internal medicine, internal medicine/pediatrics, nurse practitioner, osteopathic medicine, pediatrics, physician assistant, and specialty unspecified. Routine prescribers = allergy, dermatology, nephrology, and rheumatology.
Suggested citation for this article: Bull-Otterson L, Gray EB, Budnitz DS, et al. Hydroxychloroquine and Chloroquine Prescribing Patterns by Provider Specialty Following Initial Reports of Potential Benefit for COVID-19 Treatment — United States, January–June 2020. MMWR Morb Mortal Wkly Rep 2020;69:1210–1215. DOI: http://dx.doi.org/10.15585/mmwr.mm6935a4.
MMWR and Morbidity and Mortality Weekly Report are service marks of the U.S. Department of Health and Human Services.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All HTML versions of MMWR articles are generated from final proofs through an automated process. This conversion might result in character translation or format errors in the HTML version. Users are referred to the electronic PDF version (https://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.