Notes from the Field: Community Outbreak of Measles — Clark County, Washington, 2018–2019
Weekly / May 17, 2019 / 68(19);446–447
Alyssa Carlson, MPH1; Madison Riethman, MPH1; Paul Gastañaduy, MD2; Adria Lee, MSPH2; Jessica Leung, MPH2; Michelle Holshue, MPH3; Chas DeBolt, MPH4; Alan Melnick, MD1 (View author affiliations)
View suggested citationAltmetric:
On December 31, 2018, Clark County Public Health (CCPH) in Washington was notified of a suspected case of measles in an unvaccinated child, aged 10 years, who had recently arrived from Ukraine. The patient was evaluated at an urgent care clinic for fever, cough, and a maculopapular rash. CCPH launched a case investigation, conducted contact tracing, and facilitated specimen collection and shipment to the Washington State Department of Health Public Health Laboratories. On January 3, 2019, measles virus was detected in the patient’s urine and nasopharyngeal specimens by reverse transcription–polymerase chain reaction (RT-PCR). By January 16, among 12 patients with suspected measles reported to CCPH during January 11–14, all had laboratory-confirmed measles by RT-PCR. In response to these confirmed cases and additional suspected cases, CCPH’s Incident Management Team was activated on January 15. Approximately 200 persons participated in the multiagency response, which included CCPH, the Washington State Department of Health, and CDC. As of March 28, 2019, measles had been confirmed among 71 Clark County residents, with rash onsets from December 30, 2018, to March 13, 2019.
Persons with suspected measles were investigated through patient interviews, electronic medical records review, and consultation with health care providers; specimens were collected in accordance with recommendations (1). To increase awareness of measles circulation, regional provider advisories were issued, and press releases were distributed to notify citizens of exposures in large settings. Outbreak control measures included identifying exposed persons and assessment of their presumptive immunity to measles,* recommending vaccination of persons lacking presumptive evidence of immunity, administering postexposure prophylaxis with measles, mumps, rubella vaccine or immunoglobulin for eligible persons, and implementing social distancing strategies (e.g., isolation of patients and home quarantine of exposed persons without presumptive evidence of immunity) (2).
Among the 71 patients with confirmed measles, all of whom met the clinical case definition for measles,† 41 cases were laboratory-confirmed and 30 were epidemiologically linked to confirmed cases (3). Patients were aged 1–39 years (median = 8 years); 52 (73%) were children aged ≤10 years. Sixty-one (86%) were unvaccinated, three (4%) had received 1 dose of measles, mumps, rubella vaccine before measles exposure, and vaccination status was unknown for seven (10%). Genotype D8, which is currently circulating in Eastern Europe, was identified in all 18 specimens tested (4). No new confirmed cases have been identified since March 13, 2019.
Approximately 3,800 named contacts of the 71 patients were identified from 46 known exposures at Clark County health care facilities, workplaces, churches, schools, and child care centers, as well as social gatherings and home settings. Among these contacts, 22% lacked acceptable presumptive evidence of measles immunity.
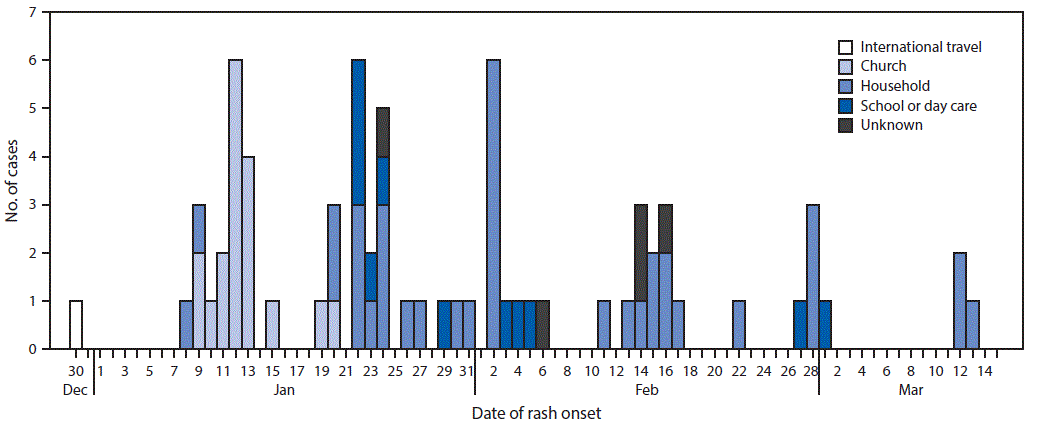
Households and churches were the predominant settings for transmission, associated with 36 (51%) and 18 (25%) of the 71 patients, respectively (Figure). Public exposures (i.e., church, school, and child care centers) most commonly occurred during the first 4 weeks of the outbreak, and decreased following communitywide implementation of CCPH-recommended outbreak control measures. Among the 30 patients identified after February 1, 26 (87%) were known contacts in quarantine and under active surveillance, decreasing public exposures by implementing effective social distancing strategies.
Clark County had not experienced a measles outbreak since 2011, when three cases were confirmed (5). Since 2013, county vaccination rates have remained 10%–14% lower than the statewide average (88%) (6). Additional U.S. jurisdictions are experiencing concurrent, unrelated measles outbreaks (7). As of May 10, 2019, the 839 measles cases identified in 23 states nationwide had surpassed the case counts observed during the same period every year since 2000, when measles was declared eliminated in the United States (range = 6–164; CDC, unpublished data). The current U.S. outbreaks underscore the importance of maintaining 2-dose measles vaccination coverage of ≥95% and of rapid public health responses in an era of increasing measles exposure threat, both in the United States and around the world.
Acknowledgments
Clark County and Washington State Measles Response Incident Management Teams; Monica Czapla, Clark County Public Health; Washington State Public Health Laboratory; Oregon State Public Health Laboratory; Washington State Department of Health; Manisha Patel, Rebecca McNall, Carole Hickman, Paul Rota, Mary Ann Hall, CDC.
Corresponding author: Alyssa Carlson, alyssa.carlson@clark.wa.gov.
1Clark County Public Health, Vancouver, Washington; 2Division of Viral Diseases, National Center for Immunization and Respiratory Diseases, CDC; 3Epidemic Intelligence Service, CDC; 4Office of Communicable Disease Epidemiology, Washington State Department of Health.
All authors have completed and submitted the ICMJE form for disclosure of potential conflicts of interest. No potential conflicts of interest were disclosed.
* Acceptable presumptive evidence of immunity to measles includes written documentation of age-appropriate vaccination, laboratory evidence of immunity, laboratory confirmation of disease, or birth before 1957.
† Fever; maculopapular rash; and cough, coryza, or conjunctivitis.
References
- CDC. Manual for the surveillance of vaccine-preventable diseases: chapter 22: laboratory support for the surveillance of vaccine-preventable diseases. Atlanta, GA: US Department of Health and Human Services, CDC; 2014. https://www.cdc.gov/vaccines/pubs/surv-manual/chpt22-lab-support.pdf
- McLean HQ, Fiebelkorn AP, Temte JL, Wallace GS; CDC. Prevention of measles, rubella, congenital rubella syndrome, and mumps, 2013: summary recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR Recomm Rep 2013;62(No. RR-04). PubMed
- CDC. National Notifiable Diseases Surveillance System. Measles/rubeola 2013 case definition. Atlanta, GA: US Department of Health and Human Services, CDC; 2019. https://wwwn.cdc.gov/nndss/conditions/measles/case-definition/2013/
- Regional Office for Europe, World Health Organization. Measles in the WHO European Region January–June 2018. WHO Epi-Brief 2018;2:1–10. Copenhagen, Denmark: World Health Organization, Regional Office for Europe; 2018. http://www.euro.who.int/__data/assets/pdf_file/0004/386707/epibrief2-eng.pdf
- Washington State Department of Health, Office of Communicable Disease Epidemiology. Communicable disease report 2011. Publication no. DOH 420–004. Shoreline, WA: Washington State Department of Health; 2011. https://www.doh.wa.gov/Portals/1/Documents/5100/420-004-CDAnnualReport2011.pdf
- Washington State Department of Health, Office of Immunization and Child Profile. Historical immunization coverage, Washington state: school years 1998–99 to 2017–18. Publication no. DOH 348–686. Shoreline, WA: Washington State Department of Health; 2018. https://www.doh.wa.gov/Portals/1/Documents/Pubs/348-686-Historical-ImmStateCounty.xlsx
- CDC. Measles cases and outbreaks. Atlanta, GA: US Department of Health and Human Services, CDC; 2019. https://www.cdc.gov/measles/cases-outbreaks.html
 FIGURE. Number of measles cases, by transmission setting and date of rash onset (N = 71) — Clark County, Washington, December 30, 2018–March 13, 2019
FIGURE. Number of measles cases, by transmission setting and date of rash onset (N = 71) — Clark County, Washington, December 30, 2018–March 13, 2019
Suggested citation for this article: Carlson A, Riethman M, Gastañaduy P, et al. Notes from the Field: Community Outbreak of Measles — Clark County, Washington, 2018–2019. MMWR Morb Mortal Wkly Rep 2019;68:446–447. DOI: http://dx.doi.org/10.15585/mmwr.mm6819a5.
MMWR and Morbidity and Mortality Weekly Report are service marks of the U.S. Department of Health and Human Services.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All HTML versions of MMWR articles are generated from final proofs through an automated process. This conversion might result in character translation or format errors in the HTML version. Users are referred to the electronic PDF version (https://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.