Notes from the Field: Varicella Outbreak Associated with Riding on a School Bus — Muskegon County, Michigan, 2015
Weekly / September 9, 2016 / 65(35);941–942
Douglas E. Hoch, MD1; Linda Scott1; Jean Chang, PhD1 (View author affiliations)
View suggested citationOn December 3, 2015, Public Health–Muskegon County (PHMC) in Michigan was notified by a local kindergarten–grade 2 school that a student aged 8 years (the index patient) had been sent home because of a rash suspected to be varicella (chickenpox); the rash had not been observed the previous day. Investigation by PHMC revealed that the student was one of five siblings in household A, none of whom had a history of having received any immunizations. During the preceding month the index patient’s two older siblings (aged 12 years and 25 years) and two younger siblings (twins, aged 4 years) had been excluded from other schools in this rural district because of rashes that also were suspected to be varicella. Investigators also learned that a parent in household A had received a physician diagnosis of herpes zoster (shingles) nearly 7 weeks earlier, on October 20, after having been evaluated for a painful, unilateral trunk rash that had begun 3 days earlier, and for which acyclovir was prescribed. PHMC could not confirm whether any advice regarding prevention of possible transmission of varicella zoster virus to susceptible contacts was provided. The other children in household A had rash onsets on November 3, November 18 (two children), and November 22. The index patient rode a school bus and was the first student on and the last off each day; none of the index patient’s four siblings attended the same school or rode on the same school bus as the index patient. Public health investigators subsequently linked three more cases in children to sharing the same school bus as the index patient.
Three children from two additional households (household B and household C) who routinely rode the same school bus as the index patient also received diagnoses of varicella. The first case was diagnosed in a fully immunized student aged 7 years who resided in household B, and had rash onset on December 15 (Figure). That diagnosis was subsequently confirmed from a cutaneous lesion swab by polymerase chain reaction (PCR). This student rode on the same bus as the index patient for approximately 40 minutes in each direction each day. The next two cases occurred in siblings from household C, aged 7 years and 5 years, who had rash onset on December 17 and December 23, respectively. On December 28, a rash suspected to represent varicella was noted in a younger sibling (aged 17 months) of the two patients from household C. None of the three children in household C had been vaccinated against varicella. The diagnosis in the second sibling (aged 5 years) was also confirmed by PCR testing from a cutaneous lesion swab. None of the four children in households B and C were related to or interacted socially with members of household A; nor did the child in household B share any classes, lunchrooms, or recess with children in household C. It is not known whether the three students from households B and C sat next to or otherwise interacted with the index patient during the bus ride. No other cases of varicella had been reported in that school district during that school year. The reported coverage with at least 1 dose of varicella vaccine in the school was 96% and for coverage with 2 doses was 95%.* The overall coverage rate with all required immunizations for the school was 95%; 2% of children had waivers, and immunizations for 3% of children were incomplete.
This outbreak of varicella appears to have begun with an adult case of herpes zoster and resulted in nine cases of varicella in children residing in three households. The timeline of rash onsets is consistent with the 10–21 day incubation period for varicella (Figure). With continued 2-dose childhood varicella vaccination and declining incidence of varicella among children (1), transmission of varicella initiated by adults with herpes zoster might become increasingly more likely (2). This investigation also strongly suggests that transmission of varicella to children residing in households B and C occurred while riding the same school bus as the index patient. Varicella transmission on school buses is plausible and was implicated previously as a risk factor for transmission in a large varicella outbreak reported in China (3). Public health investigators who see similar findings might consider the close proximity of students in a relatively small, enclosed space, such as a school bus, as a risk factor for airborne transmission of diseases such as varicella.
This investigation underscores the importance of maintaining high 2-dose varicella immunization levels to reduce risk for disease transmission. The high immunization rates achieved in this school likely limited the scope of the varicella outbreak. Two doses of varicella vaccine are routinely recommended for children at age 12–15 months and age 4–6 years (4). In addition, contacts of patients with varicella or herpes zoster should immediately be evaluated for evidence of varicella immunity to determine need for postexposure varicella vaccination. Early vaccination of exposed susceptible persons can prevent disease and transmission.
Corresponding author: Douglas E. Hoch, dehochmd@comcast.net, 231-724-6246.
References
- Lopez AS, Zhang J, Marin M. Epidemiology of varicella during the 2-dose varicella vaccination program—United States, 2005–2014. MMWR Morb Mortal Wkly Rep 2016;65:902–5. CrossRef PubMed
- Viner K, Perella D, Lopez A, et al. Transmission of varicella zoster virus from individuals with herpes zoster or varicella in school and day care settings. J Infect Dis 2012;205:1336–41. CrossRef PubMed
- Ma H, Fontaine R. Varicella outbreak among primary school students—Beijing, China, 2004. In: CDC. Global epidemiology: proceedings of the Third TEPHINET Conference—Beijing, China, November 8–12, 2004. MMWR Suppl 2006;55(No. Suppl 1).
- Marin M, Güris D, Chaves SS, Schmid S, Seward JF; Advisory Committee on Immunization Practices. Prevention of varicella: recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR Recomm Rep 2007;56(No. RR-4). PubMed
* Michigan IP100 Report, February 2016 Reporting Period, 6124008057. Michigan schools and licensed childcare centers are required to report Immunization Program (IP) compliance on students aged ≤18 years to their local health department (https://www.mcir.org/school-childcare/reporting-immunization-program-status-to-the-health-department/).
 FIGURE. Dates of varicella (chickenpox) rash onset among children in outbreak,* and date of diagnosis of herpes zoster (shingles) in the initiating parent in household A — Michigan, October–December, 2015
FIGURE. Dates of varicella (chickenpox) rash onset among children in outbreak,* and date of diagnosis of herpes zoster (shingles) in the initiating parent in household A — Michigan, October–December, 2015
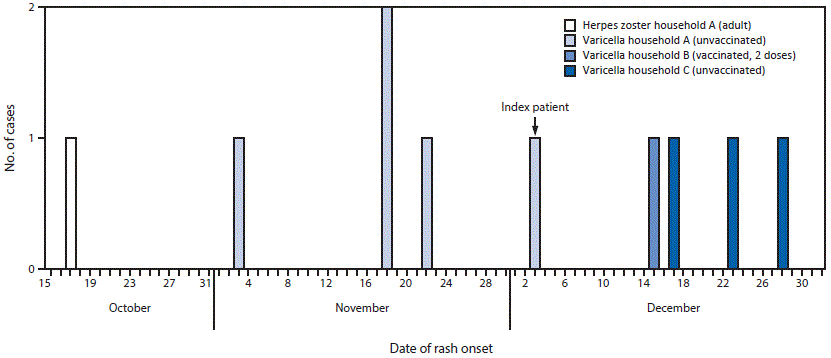
* The patient with rash onset December 28 was aged 17 months and did not attend school.
Suggested citation for this article: Hoch DE. Notes from the Field. Varicella Outbreak Associated with Riding on a School Bus — Muskegon County, Michigan, 2015. MMWR Morb Mortal Wkly Rep 2016;65:941–942. DOI: http://dx.doi.org/10.15585/mmwr.mm6535a4.
MMWR and Morbidity and Mortality Weekly Report are service marks of the U.S. Department of Health and Human Services.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All HTML versions of MMWR articles are generated from final proofs through an automated process. This conversion might result in character translation or format errors in the HTML version. Users are referred to the electronic PDF version (https://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.