Staph infections can kill
Free Continuing Education (CE) on Vital Signs: Epidemiology and Recent Trends in Methicillin-Resistant and in Methicillin-Susceptible Staphylococcus aureus Bloodstream Infections — United States (MMWR/Medscape) – available until May 23, 2020. Register for free on Medscape to access.



Nearly 1 in 10 serious staph infections in 2016 occurred in people who inject drugs such as opioids.
Overview
Staphylococcus aureus (staph) is a germ found on people’s skin. Staph can cause serious infections if it gets into the blood and can lead to sepsis or death.
- Staph is either methicillin-resistant staph (MRSA) or methicillin-susceptible staph (MSSA).
- Staph can spread in and between hospitals and other healthcare facilities, and in communities.
- People are at higher risk for staph infection when they have surgery or stay in healthcare facilities, have medical devices in their body, inject drugs, or when they come in close contact with someone who has staph.
- Additional tactics in healthcare—such as decolonization (reducing germs people may carry and spread) before surgery—along with current CDC recommendations could prevent more staph infections.
Take action against all staph.
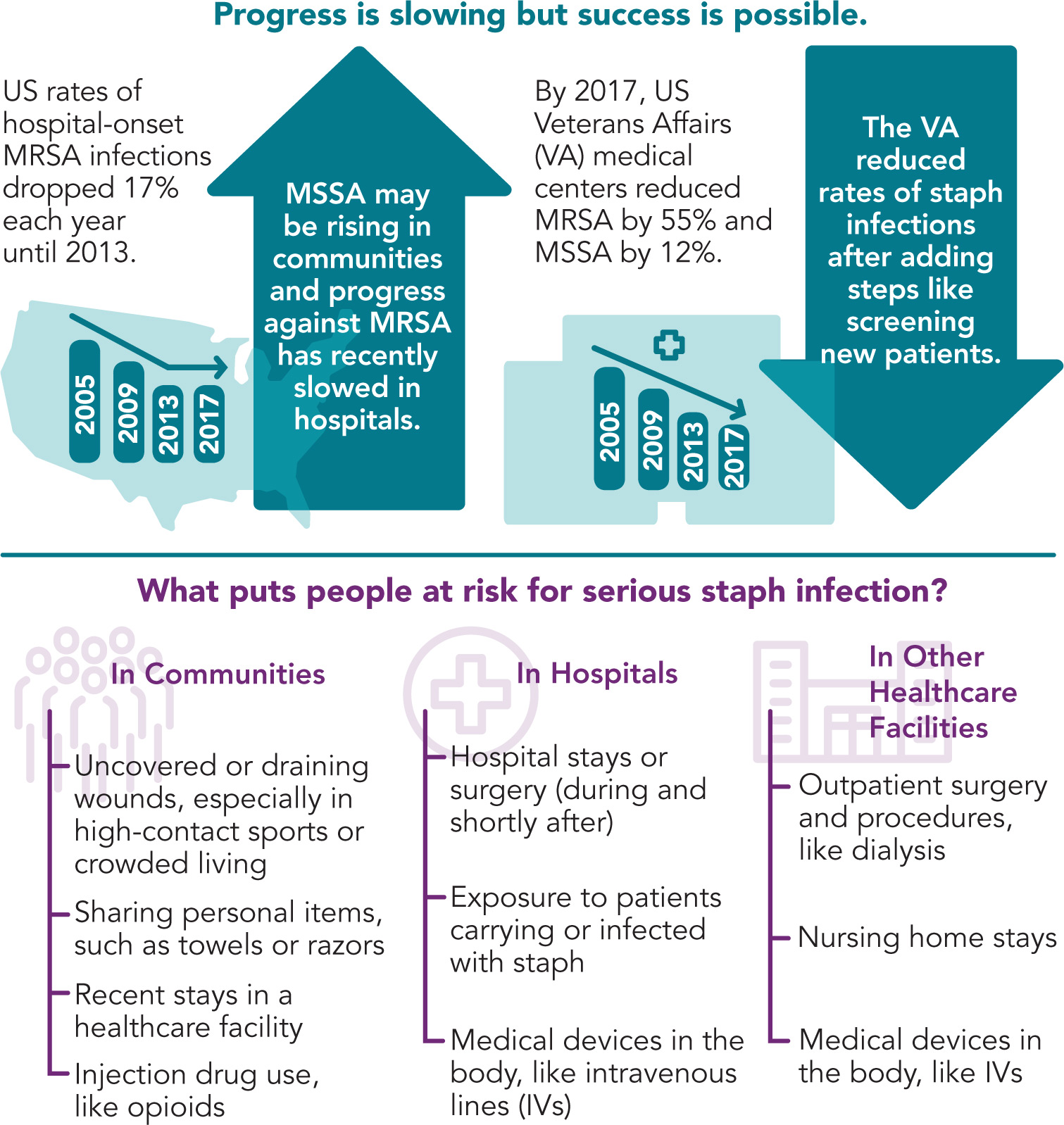
MRSA is well known but any staph can be deadly.
- Staph is a leading cause of infections in US healthcare facilities.
- Current recommendations have reduced MRSA in healthcare, but progress has slowed. Recent data suggest MSSA rates are not declining.
- The rise of staph infections in communities may be connected to the opioid crisis. In 2016, 9% of all serious staph infections happened in people who inject drugs—rising from 4% in 2011.
Healthcare Providers Can:
- Follow current recommendations for preventing device- and procedure-related infections.
- Prevent spread of staph, including use of Contact Precautions (gloves and gowns) for resistant infections. Consider actions including screening high-risk patients and decolonization of germs during high-risk periods, such as intensive care unit (ICU) stays, surgery, or device use.
- Treat infections appropriately and rapidly if they do occur.
- Educate patients about ways to avoid infection and spread, and about early signs of sepsis.
Everyone Can:
- Keep hands clean and cover wounds.
- Avoid sharing items that contact skin, such as towels, razors, and needles.
- Watch for signs of infection and its complications, like sepsis.
- Tell your future healthcare providers if diagnosed with a resistant staph infection.

- Healthcare facilities can make MRSA and MSSA prevention a priority by assessing the facility’s staph infection data, implementing prevention actions, and evaluating progress.
- Many hospitals have successfully prevented infections and spread. Ongoing assessment of facility data and implementation of prevention strategies are critical to this success.
Related Pages and Resources
- Vital Signs: Press Release – Deadly Staph Infections Still Threaten the U.S. [English]
- Vital Signs: Press Release – Las infecciones mortales por estafilococo siguen siendo una amenaza en los EE. UU. [Spanish]
- Vital Signs: Epidemiology and Recent Trends in Methicillin-Resistant and in Methicillin-Susceptible Staphylococcus aureus Bloodstream Infections — United States, Morbidity and Mortality Weekly Report (MMWR)
- Vital Signs: Trends in Staphylococcus aureus Infections in Veterans Affairs Medical Centers — United States, 2005–2017, Morbidity and Mortality Weekly Report (MMWR)
- Invasive Methicillin-Resistant Staphylococcus aureus Infections Among Persons Who Inject Drugs — Six Sites, 2005–2016
- Methicillin-resistant Staphylococcus aureus (MRSA)
- Strategies to Prevent Hospital-onset Staphylococcus aureus Bloodstream Infections in Acute Care Facilities
- Staphylococcus aureus in healthcare settings
- Factsheet: How to Avoid Infections – For Providers Who Treat Patients Who Inject Drugs [88 KB, 2 pages, 508]
- Factsheet: How to Avoid Infections – For Patients Who Inject Drugs [2 MB, 2 pages, 508]
Other Sites
Science Behind the Issue
For More Information
1-800-CDC-INFO (232-4636)
TTY: 1-888-232-6348
Web: www.cdc.gov
Centers for Disease Control and Prevention
1600 Clifton Road NE
Atlanta, GA 30333
Publication date: March 5, 2019