Key points
- Social factors like education and economic status can affect people's risk of vision loss and eye disease.
- Reducing disparities in social determinants of health is essential to reaching vision health equity.

Social determinants and health equity
Social determinants and health equity
Social factors like where someone lives and how much money they earn can affect their health, including risk of vision loss.
Social determinants are key drivers of health inequities—especially among people from racial and ethnic minority groups. Health inequities increase the risk of poor health outcomes. It is essential to reduce and eliminate these disparities to reach health equity.
Social determinants of health and vision loss
Social determinants of health (SDOH) are the nonmedical conditions that shape people's daily lives and influence their health. They include where people live, learn, work, and play.
How social determinants affect vision health
The following social factors play an important role in vision loss:
Income
People with lower incomes are less likely to access preventive care, including an eye exam. They are also less likely to be able to afford eyeglasses and more likely to have vision loss due to diabetic retinopathy.1234
Education
People with less than a high school education are less likely to have had an eye care visit in the last year compared to people with more than a high school education.1
Neighborhood
Neighborhood safety can impact physical activity, weight management, blood sugar levels, and stress. These are all factors that affect someone's risk for diabetes, which can lead to vision loss.5
Health care access
People living with a disability such as vision impairment or blindness report having more problems accessing care. Common issues include cost, insurance coverage, transportation, and refusal of services by providers. People with vision impairment are also more likely to be uninsured compared to people without.6
Addressing these barriers is key to eliminating health disparities and reaching vision health equity.
Who's affected
Vision loss in the United States
Vision loss ranks among the top 10 causes of disability in the United States. About 7 million Americans have vision impairment, including 1 million who are blind.7 These numbers are expected to double by 2050 due to population aging and increases in chronic diseases that can lead to vision loss.8
Populations impacted
The risk for eye disease varies by race/ethnicity, age, and sex. In addition, having a chronic health condition (such as diabetes, high blood pressure, or heart disease) can increase risk. Behavioral factors such as smoking and being physically inactive also increase the risk of vision loss.
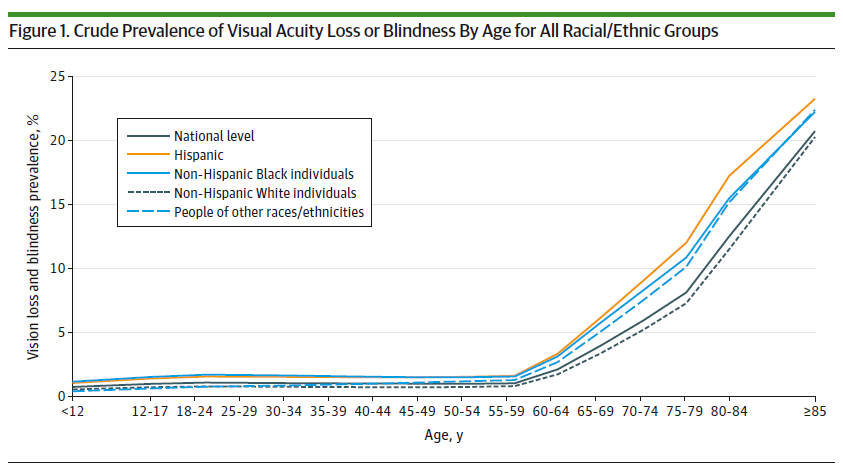
Data spreadsheet for Figure 1.
Research shows that SDOH are also linked to vision loss.9 A recent study found that people who reported having visual difficulty were more likely to:
- Have a lower education level.
- Have health care coverage through Medicaid.
- Have problems paying medical bills.
- Have trouble finding a doctor.
- Skip doses of medicine because of cost.
- Experience food insecurity.
- Identify as a gay male.
What CDC is doing
Learn more about the CDC's Vision Health Initiative and its partnerships to advance vision health equity.
- Zhang X, Cotch MF, Ryskulova A, et al. Vision health disparities in the United States by race/ethnicity, education, and economic status: findings from two nationally representative surveys. Am J Ophthalmol. 2012;154:S53–S62.
- Barsegian A, Kotlyar B, Lee J, Salifu MO, McFarlane SI. Diabetic retinopathy: focus on minority populations. Int J Clin Endocrinol Metab. 2017;3(1):34–45.
- Saydah SH, Gerzoff RB, Saaddine JB, Zhang X, MD, Cotch MF. Eye care among US adults at high risk for vision loss in the United States in 2002 and 2017. JAMA Ophthalmol. 2020;138(5):479–489.
- Gibson DM. Food insecurity, eye care receipt, and diabetic retinopathy among US adults with diabetes: Implications for primary care. J Gen Intern Med. 2019;34:1700–1702.
- Tamayo A, Karter AJ, Mujahid MS, et al. Associations of perceived neighborhood safety and crime with cardiometabolic risk factors among a population with type 2 diabetes. Health Place. 2016;39:116–21.
- Spencer C, Frick K, Gower EW, Kempen JH, Wolff JL. Disparities in Access to Medical Care for Individuals with Vision Impairment. Ophthalmic Epidemiology. 2009;16(5):281–288.
- Flaxman AD, Wittenborn JS, Robalik T, et al. The prevalence of visual acuity loss or blindness in the US: a Bayesian meta-analysis. JAMA Ophthalmol. Published online May 13, 2021. doi:10.1001/jamaophthalmol.2021.0527
- Varma R, Vajaranant TS, Burkemper B, et al. Visual impairment and blindness in adults in the United States: demographic and geographic variations from 2015 to 2050. JAMA Ophthalmol. 2016;134(7):802–809.
- Su NH, Moxona NR, Wang A, French DD. Associations of social determinants of health and self-reported visual difficulty: analysis of the 2016 National Health Interview Survey. Ophthalmic Epidemiology. 2020;27(2):93–97.
