CDC Levels of Care Assessment ToolSM (CDC LOCATeSM)
Risk-Appropriate Care
Risk-appropriate care is a strategy to improve health outcomes for pregnant women and infants. States may develop coordinated regional systems to help ensure that pregnant women and infants at high risk of complications receive care at a birth facility that is best prepared to meet their health needs. For example, pregnant women with severe heart conditions need care at facilities that have a full range of specialists available to help care for complex medical conditions. Infants born before 32 weeks gestation should be cared for at facilities with specialized health care providers and equipment to care for infants who are born too early or who are critically ill.
CDC Levels of Care Assessment ToolSM
Definitions and monitoring of levels of care vary widely among states. To address this issue, CDC developed the CDC Levels of Care Assessment ToolSM (LOCATeSM). This web-based tool helps states and other jurisdictions create standardized assessments of levels of maternal and neonatal care. CDC LOCATeSM is based on the most recent guidelines and policy statements issued by the American Academy of Pediatrics, the American College of Obstetricians and Gynecologists, and the Society for Maternal-Fetal Medicine. Review Frequently Asked Questions about CDC LOCATeSM.
If you are interested in participating in or have questions about CDC LOCATeSM, e-mail drhinfo@cdc.gov
Use of CDC LOCATeSM is free.

BUILD SUPPORT
FOR PARTICIPATION
An agency or organization serving as a state champion for CDC LOCATeSM identifies stakeholders to help encourage birth facilities to use the CDC LOCATeSM tool.
The champion builds relationships with facilities to work toward statewide participation.
BEGIN USING TOOL
TO COLLECT DATA
The champion sends the CDC LOCATeSM web link to facilities in the state and follows up with those that don’t respond.
ANALYZE DATA
AND SHARE RESULTS
The champion sends data to CDC to analyze.
CDC assesses levels of maternal and neonatal care and sends back results that can be used and shared as desired.
How CDC LOCATeSM Data Are Used
CDC LOCATeSM produces standardized assessments that allow participating states to see levels of care by facility, and the distribution of staff and services throughout the state. States can combine CDC LOCATeSM data with public health surveillance data, including vital records and hospital discharge data.
These data allow for more detailed analyses that support understanding of:
- Maternal and infant health outcomes by level of care.
- The relationship between the volume of services provided by a facility and maternal and infant health outcomes.
CDC LOCATeSM is designed to be used by public health decision makers. This tool can create opportunities for informed conversations among partners who work in the area of risk-appropriate care. Examples of these partners include state and local public health departments, state perinatal quality collaboratives (PQCs), hospital associations, and health care providers working in maternal and neonatal care. The results from CDC LOCATeSM are a starting point for discussions about how states can improve health outcomes for women and infants.
Learn More about CDC LOCATeSM and Levels of Care
Guidelines and Policy Statements
- Levels of Neonatal Care from the American Academy of Pediatrics
- Levels of Maternal Care from the American College of Obstetricians and Gynecologists and the Society for Maternal-Fetal Medicine
- LoMC Levels of Maternal Care from the American College of Obstetricians and Gynecologists
Publications
- Maternal and neonatal risk-appropriate care: gaps, strategies, and areas for further research
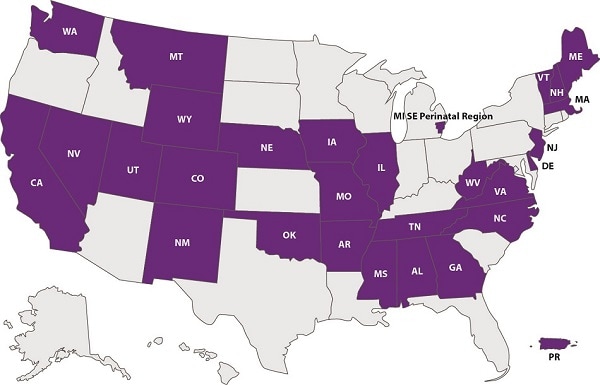
- Levels of neonatal care among birth facilities in 20 states and other jurisdictions: CDC levels of care assessment toolSM(CDC LOCATeSM)
- Seven years later: state neonatal risk-appropriate care policy consistency with the 2012 American Academy of Pediatrics Policy
- CDC LOCATeSM: discrepancies between self-reported level of maternal care and LOCATe-assessed level of maternal care among 463 birth facilities.
- Maternal transport: an opportunity to improve the system of risk-appropriate care
- Levels of Maternal Care Verification Pilot: Translating Guidance Into Practice Obstetrics & Gynecology: December 2018 – Volume 132 – Issue 6 – p 1401–1406
- Implementing CDC’s Level of Care Assessment ToolSM(LOCATeSM): A National Collaboration to Improve Maternal and Child Health
Information for Families
- Levels of Medical Care for Your Newborn from the March of Dimes
CDC LOCATeSM and CDC Levels of Care Assessment ToolSM are service marks of the US Department of Health and Human Services.