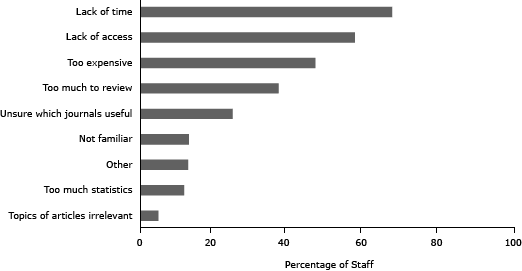Volume 11 — August 14, 2014
BRIEF
Information–Seeking Among Chronic Disease Prevention Staff in State Health Departments: Use of Academic Journals
Navigate This Article
Jenine K. Harris, PhD; Peg Allen, PhD, MPH; Rebekah R. Jacob, MPH, MSW; Lindsay Elliott; Ross C. Brownson, PhD
Suggested citation for this article: Harris JK, Allen P, Jacob RR, Elliott L, Brownson RC. Information–Seeking Among Chronic Disease Prevention Staff in State Health Departments: Use of Academic Journals. Prev Chronic Dis 2014;11:140201. DOI: http://dx.doi.org/10.5888/pcd11.140201.
PEER REVIEWED
Abstract
Use of scientific evidence aids in ensuring that public health interventions have the best possible health and economic return on investment. We describe use of academic journals by state health department chronic disease prevention staff to find public health evidence. We surveyed more than 900 state health department staff from all states and the District of Columbia. Participants identified top journals or barriers to journal use. We used descriptive statistics to examine individual and aggregate state health department responses. On average, 45.7% of staff per state health department use journals. Common barriers to use included lack of time, lack of access, and expense. Strategies for increasing journal use are provided.
Objective
State health departments are key to adoption of evidence-based public health strategies across the public health system (1). Identifying and implementing evidence-based approaches requires access to scientific evidence (2) available through academic journals, conferences, policy briefs, seminars, and elsewhere. The quality of scientific evidence is important; systematic reviews and articles in scientific journals are considered the most objective evidence available (3). We explore state health department staff use of academic journals and barriers to use.
Methods
All identified state health department professional staff working in chronic disease prevention (ie, tobacco, physical activity, nutrition, obesity prevention, comprehensive cancer, cancer screening, diabetes, heart health) from all 50 states and the District of Columbia (DC) were invited by e-mail to complete an online survey in spring 2013. We identified participants through state health department websites and lists from the Centers for Disease Control and Prevention and National Association of Chronic Disease Directors. After follow-up, 77.3% (904 of 1169 current eligible employees) completed the survey. Test–retest reliability with 75 participants was adequate (Cronbach’s α ≥ .70). Additional survey details are published elsewhere (4); the Washington University in St Louis Institutional Review Board approved this study.
Participants were asked “what methods allow you to learn about the current findings in public health research? (Using the list below please rank the top 3, where 1 is the most important.)” If journals were selected, participants were asked “which journals do you most often read to stay up-to-date on current findings in public health? (Please rank the top 3, with 1 being the journal you most often read.)” If journals were not selected, participants were asked to check all barriers to journal use that applied. Test–retest results showed 62.5% and 91.7% selected 2 or 3 of the same methods and journals, respectively. The barriers question was used in previous research (4).
State health department characteristics were obtained from the Association of State and Territorial Health Officers 2010 survey. We examined the percentage of state health department staff reporting journal use and state health department participation in research activities, staffing levels, mean employee age, mean years at state health department, number of people served, and revenue.
Results
The 904 respondents were from each of the 50 state health departments and DC. There were 6 to 45 participants per state health department (mean = 31; median = 30). Response rates from state health departments varied from 58.6% to 96.0%. Participants self-identified as program managers or coordinators (57.3%), health educators (12.1%), epidemiologists (8.6%), bureau or division chiefs or directors of chronic disease units (4.5%), and 17.5% other (eg, program evaluators). An average of 45.7% of staff per state health department reported using journals as a top method for finding evidence. State health departments where at least 50% of staff identified journals as a top source participated in more research activities compared with state health departments where fewer than 50% of staff used journals (6.5 activities vs 5.0). There were no other notable differences in journal use for staffing levels, mean employee age, mean years of service, number of people served, or revenue.
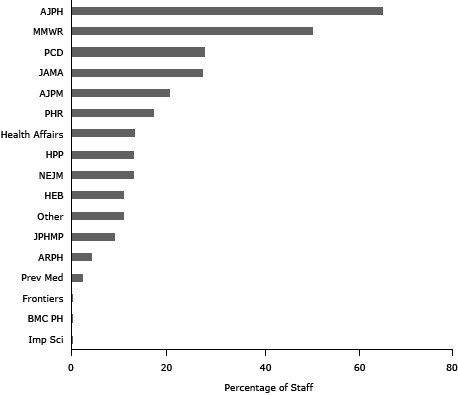
The American Journal of Public Health was used by the highest mean percentage of state health department staff (m = 65.4%; Figure 1), followed by Morbidity and Mortality Weekly Report (MMWR) (m = 50.8%) and Preventing Chronic Disease (PCD) (m = 28.0%). MMWR and PCD are both open-access with a long publication history and affiliation with a national governmental organization.
Figure 1. Mean percentage of journal-using staff per health department selecting each journal as 1 of the top 3 they use. [A tabular version of this figure is also available.]
The most common barriers to journal use included lack of time (m = 66.8% per state health department), lack of access (m = 56.9%), and expense (m = 46.4%) (Figure 2).
Figure 2. Percentage of non-journal using participants per health department who indicated each barrier to journal use as 1 of their top 3 barriers. [A tabular version of this figure is also available.]
At the individual level (not aggregated), of those who selected journals as a top source, seminars or workshops were the most highly concurrent method (46.7%) of finding research, followed by policy briefs (32.5%), and e-mail alerts (31.6%). Common methods of finding research for those not selecting journals were seminars or workshops (64.5%), e-mail alerts (57.4%), and newsletters (32.8%).
Discussion
On average, less than half of staff members per state health department selected journals as a top source of research evidence. Consistent with findings from previous studies (5), common barriers were lack of time, lack of access, expense, and too much to review. Staff members not using journals used seminars or workshops, e-mail, and newsletters. Seminars and workshops address lack of time by providing protected time (6,7), while e-mail and newsletters address too much to review by summarizing information (5). Addressing access is necessary, although likely not sufficient, for increasing journal use. One approach to increasing access, and reducing expense, is developing stronger practice–academia linkages (8,9), which could facilitate formal exchanges of staff (eg, state health department staff as adjunct faculty). The National Network of Libraries of Medicine (NNLM) plans to expand public health digital libraries nationwide (10). Digital libraries can facilitate time savings and promote evidence-based practice for health department staff (10), thus addressing access, expense, and other barriers. Access and expense may also be addressed by increasing availability of open-access journals (11).
Relevance of journal content for state health department practice may also influence use, although relevance was not a top barrier selected. Previous studies of public health agencies found staff wanted access to journals and gray literature for evidence directly related to public health practice (12). Unfortunately, there is limited literature focused on practice; instead, scientific evidence in journals focuses heavily on discovery research (3), which identifies existence of and relationships between health risks and health conditions (eg, smoking and lung cancer) (6,10).
Our main limitation is the use of close-ended measures from previous studies, which may not have captured all existing methods people use to access evidence. Also, “lack of access to journals” was not defined for participants.
State health departments play an important role in protecting and improving public health (1); the use of scientific evidence aids in ensuring public health interventions have the best possible health and economic return on investment (3). Addressing barriers to journal use may increase use of scientific evidence.
Acknowledgments
This study is funded by the National Cancer Institute of the National Institutes of Health under award no. R01CA160327. This article is a product of a Prevention Research Center and was also supported by cooperative agreement no. U48/DP001903 from the Centers for Disease Control and Prevention. The findings and conclusions in this article are those of the authors and do not necessarily represent the official positions of the National Institutes of Health or the Centers for Disease Control and Prevention. We appreciate the collaboration on this study with Ellen Jones and John Robitscher at the National Association of Chronic Disease Directors, and Vicki Benard and Marcus Plescia at the Division of Cancer Prevention and Control, Centers for Disease Control and Prevention. We are grateful for the survey development contributions of Jon Kerner at Canadian Partnership Against Cancer; Elizabeth A. Baker and Katherine A. Stamatakis at the College of Public Health and Social Justice, St Louis University; and Maureen Dobbins at McMaster University in Ontario, Canada. We also thank Sonia Sequeira for survey development and data collection while a graduate research scholar at Washington University in St Louis. We also appreciate the administrative support of Linda Dix and Mary Adams at the Prevention Research Center in St Louis, Brown School, Washington University in St Louis.
Author Information
Corresponding Author: Jenine K. Harris, PhD, Brown School, Washington University in St Louis, One Brookings Dr, Campus Box 1196, St Louis, MO 63130. Telephone: 314-935-3522. E-mail: harrisj@wustl.edu.
Author Affiliations: Peg Allen, Rebekah R. Jacob, Lindsay Elliott, Ross C. Brownson, Prevention Research Center in St Louis. Dr Brownson is also affiliated with the Division of Public Health Sciences and Alvin J. Siteman Cancer Center, Washington University School of Medicine, Washington University in St Louis, St Louis, Missouri.
References
- Brownson RC, Ballew P, Dieffenderfer B, Haire-Joshu D, Heath GW, Kreuter MW, et al. Evidence-based interventions to promote physical activity: what contributes to dissemination by state health departments. Am J Prev Med 2007;33(1):S66–S73. CrossRef PubMed
- Steele CB, Rose JM, Chovnick G, Townsend JS, Stockmyer CK, Fonseka J, et al. Use of evidence-based practices and resources among comprehensive cancer control programs. J Public Health Manag Pract 2014. CrossRef PubMed
- Brownson RC, Fielding JE, Maylahn CM. Evidence-based public health: a fundamental concept for public health practice. Annu Rev Public Health 2009;30:175–201. CrossRef PubMed
- Allen P, Sequeira S, Jacob RR, Hino AA, Stamatakis KA, Harris JK, et al. Promoting state health department evidence-based cancer and chronic disease prevention: a multi-phase dissemination study with a cluster randomized trial component. Implement Sci 2013;8(141). PubMed
- Robeson P, Dobbins M, DeCorby K, Tirilis D. Facilitating access to pre-processed research evidence in public health. BMC Public Health 2010;10(1):95. CrossRef PubMed
- Dilley JA, Bekemeier B, Harris JR. Quality improvement interventions in public health systems: a systematic review. Am J Prev Med 2012;42(5):S58–71. CrossRef PubMed
- Linzer M. The journal club and medical education: over one hundred years of unrecorded history. Postgrad Med J 1987;63(740):475–8. CrossRef PubMed
- Cilenti D, Brownson RC, Umble K, Erwin PC, Summers R. Information-seeking behaviors and other factors contributing to successful implementation of evidence-based practices in local health departments. J Public Health Manag Pract 2012;18(6):571–6. CrossRef PubMed
- Erwin PC, Keck CW. The academic health department: the process of maturation. J Public Health Manag Pract 2014;20(3):270–7. CrossRef PubMed
- LaPelle NR, Dahlen K, Gabella BA, Juhl AL, Martin E. Overcoming inertia: increasing public health departments’ access to evidence-based information and promoting usage to inform practice. Am J Public Health 2014;104(1):77–80. CrossRef PubMed
- Laakso M, Welling P, Bukvova H, Nyman L, Björk B, Hedlund T. The development of open access journal publishing from 1993 to 2009. PLoS ONE 2011;6(6):e20961. CrossRef PubMed
- LaPelle NR, Luckmann R, Simpson EH, Martin ER. Identifying strategies to improve access to credible and relevant information for public health professionals: a qualitative study. BMC Public Health 2006;6(1):89. CrossRef PubMed
The opinions expressed by authors contributing to this journal do not necessarily reflect the opinions of the U.S. Department of Health and Human Services, the Public Health Service, the Centers for Disease Control and Prevention, or the authors' affiliated institutions.