Study Syllabus for Classification of Radiographs of Pneumoconioses
Radiograph Classification
Subset 1
Section 2: Parenchymal Abnormalities (Continued)
Note: It is customary when referring to the primary and secondary types of opacities in a radiograph to separate the primary and secondary notations by a forward slash (/) with the primary type of opacity occurring before the slash and the secondary type after the slash. Thus, for example, among the Standard ILO Film Radiographs, one was identified as s/t (the primary type of opacity is s; the secondary type, is t) or t/t (nearly all of the opacities are of the t type). It should be noted that in any single radiograph there may be only rounded opacities (p, q, r), only irregular opacities (s, t, u) or there may be both rounded and irregular.
b. Zones
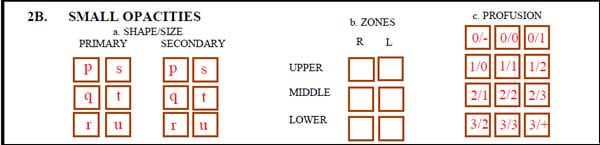
Once the size and shape of the small opacities have been determined, the areas of involvement are indicated. For this purpose, the lungs are divided into an upper, middle and lower zone on each side by imaginary horizontal lines traversing the lungs at levels one-third and two-thirds of the vertical distance between the apices and the hemidiaphragmatic domes. Thus, on the report form, zones of involvement are represented by six boxes arranged in two vertical columns representing the right and left lungs.
Within each vertical column, the boxes from top to bottom represent the upper, middle and lower zones, respectively.
Check each box in the Zones block that represents a zone in which small opacities are thought to be present.
c. Profusion (Radiographs #4 to #10)
Having defined the character (size and shape) of any pneumoconiotic small opacities that may be present, and having indicated their distribution in terms of lung zones, it is next necessary to determine their profusion (concentration, number per unit area). Profusion is expressed in terms of four major categories: 0, 1, 2 and 3. These span the range from no small opacities present (0) to a maximal number present (3), successively higher numbers representing progressively greater numbers of small opacities per unit area.
The profusion of small opacities is determined by visual comparison of the subject radiograph with ILO Standards representing the mid ranges of the four major categories. Profusion is in fact a continuum, and clinical radiographs, therefore, often do not match any one ILO Standard. Rather, they may appear to fall somewhere between two Standards. In recognition of this, each major category is divided into three “minor categories” creating a 12 point scale.
