For Healthcare Providers
From the Merck Manual Consumer Version, edited by Robert Porter. Copyright 2015 by Merck Sharp & Dohme Corp., a subsidiary of Merck & Co, Inc, Kenilworth, NJ. Available at merckmanuals.com. Accessed June 2015.
The Virus
Mumps is a viral illness caused by a paramyxovirus, a member of the Rubulavirus family. The average incubation period for mumps is 16 to 18 days, with a range of 12 to 25 days.
Clinical Features
To learn more about how to promptly recognize and diagnose mumps, check out this Mumps Clinical Diagnosis Fact Sheet [2 pages].
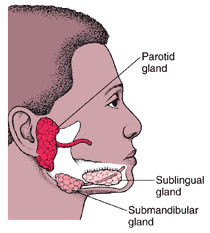
Mumps usually involves pain, tenderness, and swelling in one or both parotid salivary glands (cheek and jaw area). Swelling usually peaks in 1 to 3 days and then subsides during the next week. The swollen tissue pushes the angle of the ear up and out. As swelling worsens, the angle of the jawbone below the ear is no longer visible. Often, the jawbone cannot be felt because of swelling of the parotid. One parotid may swell before the other, and in 25% of patients, only one side swells. Other salivary glands (submandibular and sublingual) under the floor of the mouth also may swell but do so less frequently (10%).
Nonspecific prodromal symptoms may precede parotitis by several days, including low-grade fever which may last 3 to 4 days, myalgia, anorexia, malaise, and headache. Parotitis usually lasts on average 5 days and most cases resolve after 10 days. Mumps infection may also present only with nonspecific or primarily respiratory symptoms, or may be asymptomatic. Reinfection after natural infection and recurrent parotitis, when parotitis on one side resolves but is followed weeks to months later by parotitis on the other side, can also occur in mumps patients.
Mumps can occur in a person who is fully vaccinated, but vaccinated patients are less likely to present severe symptoms or complications than under- or unvaccinated cases. Mumps should be suspected in all patients with parotitis or mumps complications, regardless of age, vaccination status, and travel history.
Mumps infection is most often confused with swelling of the lymph nodes of the neck. Lymph node swelling can be differentiated by the well-defined borders of the lymph nodes, their location behind the angle of the jawbone, and lack of the ear protrusion or obscuring of the angle of the jaw, which are characteristics of mumps.
While not a common symptom of flu, swelling of their salivary glands (parotitis) has been reported in persons with laboratory-confirmed influenza infections. To learn more, see 2016-2017 Influenza Update for Health Care Providers: Parotitis and Influenza.
Background
Before the U.S. mumps vaccination program started in 1967, about 186,000 cases were reported each year, and many more unreported cases occurred. The disease caused complications, such as permanent deafness in children, and occasionally, encephalitis, which could rarely result in death. Following the implementation of the routine two dose MMR vaccination policy, there was a 99% decrease in mumps cases in the United States, with just a few hundred cases reported each year by the early 2000s. However, starting in 2006 there has been an increase in mumps cases with several peak years. From year to year, the number of mumps cases can range from roughly a couple hundred to a several thousand, with majority of cases and outbreaks occurring among people who are fully vaccinated and in close-contact or congregate settings.
Transmission
The mumps virus replicates in the upper respiratory tract and is transmitted person to person through direct contact with saliva or respiratory droplets of a person infected with mumps. The risk of spreading the virus increases the longer and the closer the contact a person has with someone who has mumps. The infectious period is considered from 2 days before to 5 days after parotitis onset, although virus has been isolated from saliva as early as 7 days prior to and up to 9 days after parotitis onset. Mumps virus has also been isolated up to 14 days in urine and semen.
When a person is ill with mumps, they should avoid contact with others from the time of diagnosis until 5 days after the onset of parotitis by staying home from work or school and staying in a separate room if possible.
Complications
Mumps complications include orchitis, oophoritis, mastitis, meningitis, encephalitis, pancreatitis, and hearing loss. Complications can occur in the absence of parotitis and occur less frequently in vaccinated patients. Some complications of mumps are known to occur more frequently among adults than children.
Orchitis occurs in approximately 30% of unvaccinated and 6% of vaccinated post-pubertal male mumps patients. In 60% to 83% of males with mumps orchitis, only one testis is affected. Mumps orchitis has not been linked to infertility, but may result in testicular atrophy and hypofertility. Among adolescent and adult female mumps patients in the United States in the post-vaccine era, rates of oophoritis and mastitis have been ≤1%. However, these complications may be more difficult to recognize and are likely underreported. Pancreatitis, deafness, meningitis, and encephalitis have been reported in less than 1% of cases in recent U.S. outbreaks. Cases of nephritis and myocarditis and other sequelae, including paralysis, seizures, cranial nerve palsies, and hydrocephalus, in mumps patients have been reported but are very rare. Death from mumps is exceedingly rare. There have been no mumps-related deaths reported in the United States during recent mumps outbreaks.
Mumps during Pregnancy
Mumps that occurs in pregnant women is generally benign and not more severe than in women who are not pregnant. Like other infections, there is a theoretical risk that mumps during the early months of pregnancy may cause complications. Most studies on the effects of gestational mumps on the fetus were conducted in the 1950s–60s when the disease was more common before mumps vaccine was available. One study from 1966 reported an association between mumps infection during the first trimester of pregnancy and an increase in the rate of spontaneous abortion or intrauterine fetal death1, but this result has not been observed in other studies2. One study of low birth weight in relation to mumps during pregnancy found no significant association1. While there are case reports of congenital malformations in infants born to mothers who had mumps during pregnancy, the only prospective, controlled study found rates of malformations were similar between mothers who had mumps and those who did not have mumps during pregnancy3.
Learn more about preventing infections during pregnancy.
Mumps in Vaccinated People
People who previously had one or two doses of MMR vaccine can still get mumps and transmit the disease. During mumps outbreaks in highly vaccinated communities, the proportion of cases that occur among people who have been vaccinated may be high. This does not mean that the vaccine is ineffective. The effectiveness of the vaccine is assessed by comparing the attack rate in people who are vaccinated with the attack rate in those who have not been vaccinated. In outbreaks of highly vaccinated populations, people who have not been vaccinated against mumps usually have a much greater mumps attack rate than those who have been fully vaccinated. Disease symptoms are generally milder and complications are less frequent in vaccinated people.
Vaccination
Vaccination is the best way to prevent mumps and mumps complications. This vaccine is included in the combination measles-mumps-rubella (MMR) and measles-mumps-rubella-varicella (MMRV) vaccines. Two doses of mumps vaccine are 88% (range 32% to 95%) effective at preventing the disease; one dose is 78% (range 49% to 91%) effective.
In October 2017, the Advisory Committee on Immunization Practices (ACIP) recommended that people identified by public health authorities as being part of a group at increased risk for acquiring mumps because of a mumps outbreak should receive a third dose of MMR vaccine. The purpose of the recommendation is to improve protection of people in outbreak settings against mumps disease and mumps-related complications.
- Your health department will provide information on groups at increased risk who should receive a dose. If you suspect an outbreak, or are unsure if your patient belongs to a group at increased risk, contact your local health department for more information.
- You should not give a third dose unless your patient is part of a group at increased risk as determined by your local public health authorities.
- MMR vaccine has not been shown to prevent illness in persons already infected with mumps and should not be used as post-exposure prophylaxis in immediate close contacts. However, close contacts should still be offered a dose to help protect them against future exposures in the event their prior exposures did not result in infection.
See Mumps Vaccination for vaccination recommendations.
Case Classification
For information about how to classify mumps cases, visit the Laboratory Testing Section of the Manual for the Surveillance of Vaccine-Preventable Diseases (2018), Chapter 9: Mumps.
Laboratory Tests to Diagnose Mumps
RT-PCR and viral culture are used to confirm mumps infection. Buccal swabs are most commonly used for RT-PCR testing, but urine and CSF may also be used in specific situations. IgM serology can also be used to aid in diagnosing mumps infection. A patient’s vaccination status and timing of specimen collection are important for interpreting laboratory results. A negative test result does not rule out mumps infection.
Reporting Mumps Cases
Mumps is a nationally notifiable disease, and all cases should be reported to the state or local health department. Contact your state health department for more information on how to report mumps in your state.
Mumps Prevention and Control in Healthcare Settings
Mumps transmission in healthcare settings, while not common, has occurred in past outbreaks, involving hospitals and long-term care facilities housing adolescents and adults. Information about what measures to take to prevent and control mumps in healthcare settings can be found under the Healthcare Setting section of the Manual for the Surveillance of Vaccine-Preventable Diseases (2018), Chapter 9: Mumps
Footnotes
- Siegel M, Fuerst HT, Peress NS. Comparative fetal mortality in maternal virus diseases. A prospective study on rubella, measles, mumps, chicken pox and hepatitis. N Engl J Med 1966;274(14):768-71.
- Wilson CB, Nizet V, Maldonado YA, Remington JS, Klein JO. Remington and Klein’s infectious diseases of the fetus and newborn infant. 8th Edition, Elsevier Health Sciences, 2016.
- Siegel M. Congenital malformations following chickenpox, measles, mumps, and hepatitis. Results of a cohort study. JAMA 1973;226(13):1521-4.