Possible Exposures Among Mpox Patients Without Reported Male-to-Male Sexual Contact — Six U.S. Jurisdictions, November 1–December 14, 2022
Weekly / September 1, 2023 / 72(35);944–948
J. Danielle Sharpe, PhD1,2,*; Kelly Charniga, PhD1,*; Katrina M. Byrd, MD1,2; Ruth Stefanos, MD1,2; Linda Lewis, DVM3; Jessica Watson, MD3; Amanda Feldpausch, DVM4; Jessica Pavlick, DrPH4; Julie Hand, MSPH5; Theresa Sokol, MPH5; Emma Ortega, MPHTM5; Preeti Pathela, DrPH6; Robin R. Hennessy, MPH6,7; Melissa Dulcey, DVM, PhD2,8; Lisa McHugh, PhD8; Michael Pietrowski, MPH9; Dana Perella, MPH9; Seema Shah, MD10; Azarnoush Maroufi, MPH10; Melanie Taylor, MD1; Anna Cope, PhD1; Ermias D. Belay, MD1; Sascha Ellington, PhD1; Andrea M. McCollum, PhD1; Leah Zilversmit Pao, PhD1; Sarah Anne J. Guagliardo, PhD1; Patrick Dawson, PhD1 (View author affiliations)
View suggested citationSummary
What is already known about this topic?
During the 2022 U.S. mpox outbreak, approximately 30% of mpox patients had missing exposure data or no reported male-to-male sexual contact (MMSC).
What is added by this report?
Among 52 mpox patients who did not report MMSC from six jurisdictions, 14 (27%) had a known exposure to a person with mpox; these exposures included sexual activity (eight) and household contact (six). Among 38 (73%) patients with no known exposure to a person with mpox, behaviors preceding illness included sexual activity (17; 45%), close face-to-face contact (14; 37%), attending large social gatherings (11; 29%), and being in occupational settings (10; 26%).
What are the implications for public health practice?
Although a small proportion of mpox patients did not report MMSC, possible mpox exposures among these patients involved exposures or other behaviors known to potentially transmit Monkeypox virus, including sexual activity (other than MMSC) or other close skin-to-skin contact.
Altmetric:
Abstract
The extent to which the 2022 mpox outbreak has affected persons without a recent history of male-to-male sexual contact (MMSC) is not well understood. During November 1–December 14, 2022, CDC partnered with six jurisdictional health departments to characterize possible exposures among mpox patients aged ≥18 years who did not report MMSC during the 3 weeks preceding symptom onset. Among 52 patients included in the analysis, 14 (27%) had a known exposure to a person with mpox, including sexual activity and other close intimate contact (eight) and household contact (six). Among 38 (73%) patients with no known exposure to a person with mpox, self-reported activities before illness onset included sexual activity and other close intimate contact (17; 45%), close face-to-face contact (14; 37%), attending large social gatherings (11; 29%), and being in occupational settings involving close skin-to-skin contact (10; 26%). These findings suggest that sexual activity remains an important route of mpox exposure among patients who do not report MMSC.
Introduction
During infectious disease outbreaks, there are often cases for which a source of infection cannot be identified. The 2022 mpox outbreak disproportionately affected adult gay, bisexual, and other men who have sex with men; however, approximately 30% of U.S. mpox patients did not report male-to-male sexual contact (MMSC)† (1,2). During May–October 2022, increases in mpox cases among persons with missing exposure data or no reported MMSC highlighted a need to understand the extent to which the outbreak has affected other populations, as well as additional potential routes of Monkeypox virus (MPXV) transmission, to aid in the development and implementation of public health prevention guidance (1).
Methods
Data on confirmed and probable mpox cases are electronically reported to CDC by U.S. jurisdictional health departments as part of national mpox surveillance, using a standardized case report form§ or through the National Notifiable Diseases Surveillance System.¶ CDC analyzed data on confirmed and probable mpox cases among persons aged ≥18 years reported by six jurisdictional health departments** during November 1–December 14, 2022, for whom MMSC during the 3 weeks preceding symptom onset was unknown, not reported, or not applicable. A desk review was conducted using jurisdiction-level mpox, HIV, and sexually transmitted infection surveillance data not previously reported to CDC to obtain information on demographic and clinical characteristics and possible exposures during the 3 weeks before symptom onset, including sexual activity and close intimate contact,†† caregiving,§§ household contact,¶¶ attendance at small*** and large††† social gatherings, shared transportation,§§§ close face-to-face contact,¶¶¶ occupational settings,**** and recreational drug use.†††† After the desk review, a subset of patients was contacted up to three times for an in-depth reinterview guided by a standardized questionnaire; those who were unable to be reinterviewed were retained in the analysis if sufficient data from the desk review were available. Patients without a known exposure to a person with mpox were interviewed about activities and interactions during the 3 weeks preceding symptom onset to identify possible sources of infection. Disease intervention specialists or epidemiologists at the local or federal level conducted the desk reviews and reinterviews. Data were analyzed using R statistical software (version 4.1.1; R Foundation). This activity was reviewed by CDC and was conducted consistent with applicable federal law and CDC policy.§§§§
Results
During November 1–December 14, 2022, a total of 932 mpox cases were reported to CDC; among these, 122 (13%) were reported from the six jurisdictions participating in the investigation and met the initial inclusion criteria. Upon desk review or reinterview, patients 1) who did not have mpox (one), 2) for whom MMSC was reported or could not be ruled out (65), or 3) who were missing all exposure data (four) were excluded from further analysis (Supplementary Figure, https://stacks.cdc.gov/view/cdc/132208). Among the remaining 52 (6%) patients, the median age was 36 years (range = 18–70 years) (Table). Among 48 patients reporting race and ethnicity, 24 (50%) were non-Hispanic Black or African American (Black), 16 (33%) were Hispanic or Latino (Hispanic), and five (10%) were non-Hispanic White. Thirty-two (62%) patients were cisgender men, 15 (29%) were cisgender women, and three (6%) were transgender women. Among 45 patients reporting sexual orientation, 30 (67%) were heterosexual, seven (16%) were gay or lesbian, and six (13%) were bisexual. Among 42 patients reporting occupation, 26 (62%) were employed, 10 (24%) were unemployed, and six (14%) were categorized as other (e.g., student). Among 32 patients reporting housing information, four (13%) were not securely housed or were living in a congregate setting.
Overall, 48 (98%) of 49 patients with available information reported rash during their illness; the most frequently reported first rash location was the genitals (48%), followed by the legs (34%), arms (32%), and trunk (30%). Among 32 patients reporting HIV status, eight (25%) had HIV infection. Information on receipt of JYNNEOS vaccine was available for 30 patients, three (10%) of whom had received ≥1 dose.¶¶¶¶
Patients with Known MPXV Exposures
Fourteen (27%) patients reported a known exposure to a person with suspected or confirmed mpox; among these, eight***** reported sexual activity and other close intimate contact, and six††††† reported household contact (Figure) (Supplementary Table 1, https://stacks.cdc.gov/view/cdc/132206).
One household cluster involving three transmission events was identified. The index patient (patient A), a cisgender man, was exposed after being arrested and detained in a jail cell with up to seven other persons, including one who reportedly had characteristic mpox lesions on the arms and who shared a cell with patient A for >10 hours. This person shared a water fountain, bench, and toilet facilities with patient A, who was detained for 5 days and experienced the onset of symptoms the day after his release. After returning home, patient A had sex with his female partner (patient B), whose symptoms commenced 1 week later. Patients A and B share a residence with an adult woman (patient C) and a preschool-aged child,§§§§§ both of whom acquired mpox. Patient C’s symptom onset occurred 2 weeks after that in patient B; the child’s illness began 1 week after that in patient C (the child’s primary caregiver).
Other reported exposures among patients with a known exposure to a person with mpox included shared transportation (three), close face-to-face contact (two), caregiving (two), occupational setting (one), and attendance at a large social gathering where an mpox patient was present (one). In the suspected caregiving exposure, patient D reported cleaning her son’s¶¶¶¶¶ home while he was in the hospital after receiving an mpox diagnosis. Patient D lived in a separate residence and reported having no direct contact with her son at his home. Patient D reported inconsistently wearing gloves after learning of her son’s diagnosis and later developed mpox lesions on her hand.
In the suspected occupational setting exposure, patient E, a property manager, was exposed to a client with mpox. Patient E reported skin-to-skin contact, close face-to-face interactions within 6 ft (1.8 m), and handling objects shared with or potentially contaminated by the client. Neither used personal protective equipment (PPE); patient E was informed of the client’s diagnosis by a person with direct knowledge about it.
In another case, close face-to-face contact was suspected as a source of exposure: patient F met a friend with a diagnosis of mpox at an indoor bar or restaurant (i.e., large social gathering). Whether the friend was acutely ill during the meeting is unclear. They had close face-to-face contact within 6 ft (1.8 m) for 1.5 hours without the use of face masks or other PPE. Patient F did not report skin-to-skin contact with the friend, nor did they share food or drinks.
Patients Without Known MPXV Exposures
Thirty-eight (73%) patients had no known exposure to a person with suspected or confirmed mpox, among whom 17 (45%) reported recent sexual activity or other close intimate contact (Figure) (Supplementary Table 2, https://stacks.cdc.gov/view/cdc/132207). Six of 17 patients reported sex only with a partner or spouse who did not have mpox, suggesting sexual activity might not have been their source of infection. In addition to sexual activity, patients with unknown exposures reported close face-to-face contact (14; 37%), attending large social gatherings (11; 29%) (including gyms, restaurants, bars, and clubs), and being in occupational settings involving close skin-to-skin contact (10; 26%) during the 3 weeks before symptom onset. Only one patient reported potential exposure through casual contact or fomites (i.e., large social gathering, occupational setting, or shared transportation) without also reporting sexual activity or close face-to-face contact. This patient lived alone and reported going to a bar, using a rideshare service, and having no close contact with anyone during the 3 weeks before the onset of illness.
Discussion
Among 52 mpox patients without MMSC in this study, possible mpox exposures in a range of settings were identified. Sexual or other intimate contact was the most common exposure. This finding is consistent with findings from other studies (1–4), suggesting that during the current U.S. mpox outbreak, sexual transmission or close skin-to-skin contact with a person with suspected or confirmed mpox is the predominant mode of transmission. However, other transmission modes, including household transmission, were reported.
The household mpox cluster described in this report involving three transmission events and possible transmission via contaminated household objects and surfaces (5,6) underscores the need for public health agencies to consider outreach and mpox transmission prevention education for patients in household settings (7,8). Messaging for uninfected persons sharing or visiting a living space where a person with mpox resides should consider emphasizing maintenance of adequate hand hygiene; adhering to home cleaning and disinfection guidelines; and avoiding touching potentially contaminated surfaces or sharing personal items including bedding, clothing, towels, or utensils. Vaccination against mpox is also recommended for persons who have been exposed to mpox or those who are at increased risk for MPXV infection (9).
For patients without a known exposure to a person with mpox, a variety of activities and interactions with others was reported; however, it was not possible to determine the likely source of infection for most of them. Several of these patients reported close contact with one or more persons who might have had an unrecognized or undisclosed case of mpox at the time of the contact. Mpox can be transmitted before symptoms become apparent (10). Persons who have had close contact with a person with mpox should monitor themselves for symptoms for 21 days from the date of their last exposure, be vaccinated against mpox as soon as possible after the exposure, and seek immediate attention from a health care provider if they develop a new or unexplained rash or other symptoms of mpox (9).
Similar to patients identified in other studies (1–4), patients in this study were disproportionately Black and Hispanic. In addition, approximately one quarter of patients were unemployed, and more than one in 10 were not securely housed. Deploying JYNNEOS vaccine and focusing outreach and education to communities disproportionately affected by mpox should be prioritized to minimize health disparities. Coordinating with health departments, community-based organizations, and other partners can help achieve health equity in the current mpox outbreak.
Limitations
The findings in this report are subject to at least three limitations. First, all exposure data are self-reported and might be subject to recall and social desirability biases. Second, data included in this analysis are from six jurisdictions and might not be representative of other jurisdictions. Finally, the small sample size and high level of missingness for some variables might limit generalizability and highlight the need for further investigation of possible exposures among mpox patients who did not report recent sexual activity or close intimate contact.
Implications for Public Health Practice
Although a small proportion of mpox patients did not report MMSC, possible mpox exposures among these patients involved exposures or other behaviors known to potentially transmit MPXV, including sexual activity (other than MMSC) or other close skin-to-skin contact.
Acknowledgments
Mpox response teams from state and local health departments; Kayla Saadeh, Robert Snyder, California Department of Public Health; Okwudiri Nlemadin, Amanda Shinall, New York City Department of Health and Mental Hygiene.
Corresponding author: J. Danielle Sharpe, oyv7@cdc.gov.
1CDC Mpox Emergency Response Team; 2Epidemic Intelligence Service, CDC; 3California Department of Public Health; 4Georgia Department of Public Health; 5Louisiana Department of Health; 6New York City Department of Health and Mental Hygiene, New York, New York; 7Division of STD Prevention, National Center for HIV, Viral Hepatitis, STD, and TB Prevention, CDC; 8Pennsylvania Department of Health; 9Philadelphia Department of Public Health, Philadelphia, Pennsylvania; 10County of San Diego Health and Human Services Agency, San Diego, California.
All authors have completed and submitted the International Committee of Medical Journal Editors form for disclosure of potential conflicts of interest. No potential conflicts of interest were disclosed.
* These authors contributed equally to this report.
† MMSC is defined as cisgender male-to-cisgender male sexual (e.g., oral or anal sex) or intimate contact (e.g., cuddling, kissing, touching partner’s genitals or anus, or sharing sex toys) within 3 weeks of symptom onset.
§ https://www.cdc.gov/poxvirus/mpox/health-departments/case-reporting.html
¶ https://www.cdc.gov/nndss/index.html
** Health departments in California (excluding Los Angeles County), Georgia, Louisiana, New York City, Pennsylvania (excluding Philadelphia), and Philadelphia.
†† Sexual activity includes vaginal, oral, or anal sex, and close intimate contact includes cuddling, kissing, touching a partner’s genitals or anus, or sharing sex toys.
§§ Caregiving is assistance with routine everyday tasks and the social and health needs of another person provided by unpaid family members or friends or paid caregivers and can include touching skin or skin-to-skin contact; handling food, utensils, cups, or dishes; handling clothing, bedding, bed linens, or towels; handling personal care items; handling, dispensing, or administering medication or medical equipment; taking care of other family members, children, or dependents; and taking care of pets or related activities.
¶¶ Household contact includes living together in the same dwelling (e.g., household or shared dormitory room).
*** Small social settings include spending time indoors or outdoors either with one other person or in a small group of nine or fewer persons, including oneself.
††† Large social settings include spending time indoors or outdoors at large events or celebrations, in food or entertainment venues, or in a large group of 10 or more persons, including oneself.
§§§ Shared transportation includes carpooling; sharing a personally owned car, taxi, or rideshare service; using a bus, subway or light rail, railroad or train, airplane; or other transportation modalities.
¶¶¶ Close face-to-face contact includes interactions with another person within a 6 ft (1.8 m) radius, excluding physical contact.
**** Occupational settings include one’s workplace or where contact occurs during the course of one’s job, including health care facilities and sex work.
†††† Recreational drug use includes using or sharing bubblers, vapes, bongs, pipes, other smoking devices, needles or syringes, injection equipment or “works,” or other related items.
§§§§ 45 C.F.R. part 46.102(l)(2), 21 C.F.R. part 56; 42 U.S.C. Sect. 241(d); 5 U.S.C. Sect. 552a; 44 U.S.C. Sect. 3501 et seq.
¶¶¶¶ Receipt of ≥1 dose of JYNNEOS vaccine could have occurred before or after rash onset.
***** Seven of eight patients had available data on where rash first appeared on their body. Among those seven, only one patient reported that their rash did not start on their genitals or perianal area. The locations of first rash appearance reported by patients included genitals (four), perianal area (one), and both genitals and perianal area (one).
††††† Four of six patients had available data on where rash first appeared on their body. Only one had a rash that started on their genitals.
§§§§§ Because of age, the child did not meet the initial inclusion criteria and was not included in this investigation.
¶¶¶¶¶ The son of patient D was not included in the investigation, likely because his symptom onset date occurred before November 1, 2022, or because MMSC was reported.
References
- Kava CM, Rohraff DM, Wallace B, et al. Epidemiologic features of the monkeypox outbreak and the public health response—United States, May 17–October 6, 2022. MMWR Morb Mortal Wkly Rep 2022;71:1449–56. https://doi.org/10.15585/mmwr.mm7145a4 PMID:36355615
- Philpott D, Hughes CM, Alroy KA, et al.; CDC Multinational Monkeypox Response Team. Epidemiologic and clinical characteristics of monkeypox cases—United States, May 17–July 22, 2022. MMWR Morb Mortal Wkly Rep 2022;71:1018–22. https://doi.org/10.15585/mmwr.mm7132e3 PMID:35951487
- Oakley LP, Hufstetler K, O’Shea J, et al.; CDC Mpox Analytics Team. Mpox cases among cisgender women and pregnant persons—United States, May 11–November 7, 2022. MMWR Morb Mortal Wkly Rep 2023;72:9–14. https://doi.org/10.15585/mmwr.mm7201a2 PMID:36602932
- Blackburn D, Roth NM, Gold JAW, et al. Epidemiologic and clinical features of mpox in transgender and gender-diverse adults—United States, May–November 2022. MMWR Morb Mortal Wkly Rep 2022;71:1605–9. https://doi.org/10.15585/mmwr.mm715152a1 PMID:36580418
- Pfeiffer JA, Collingwood A, Rider LE, et al. High-contact object and surface contamination in a household of persons with Monkeypox virus infection—Utah, June 2022. MMWR Morb Mortal Wkly Rep 2022;71:1092–4. https://doi.org/10.15585/mmwr.mm7134e1 PMID:36006842
- Morgan CN, Whitehill F, Doty JB, et al. Environmental persistence of Monkeypox virus on surfaces in household of person who had travel-associated infection, Dallas, Texas, USA, 2021. Emerg Infect Dis 2022;28:1982–9. https://doi.org/10.3201/eid2810.221047 PMID:35951009
- CDC. Mpox: isolation and infection control at home. Atlanta, GA: US Department of Health and Human Services, CDC; 2022. https://www.cdc.gov/poxvirus/mpox/clinicians/infection-control-home.html
- CDC. Mpox: cleaning and disinfecting your home, workplace, and other community settings. Atlanta, GA: US Department of Health and Human Services, CDC; 2023. https://www.cdc.gov/poxvirus/mpox/if-sick/cleaning-disinfecting.html
- CDC. Mpox: if you’re a close contact. Atlanta, GA: US Department of Health and Human Services, CDC; 2023. https://www.cdc.gov/poxvirus/mpox/prevention/close-contact.html
- CDC. Mpox: science brief: detection and transmission of mpox (formerly monkeypox) virus during the 2022 Clade IIb outbreak. Atlanta, GA: US Department of Health and Human Services, CDC; 2022. https://www.cdc.gov/poxvirus/mpox/about/science-behind-transmission.html#asymptomatic
* Percentages calculated using nonmissing data.
† All racial groups listed are non-Hispanic; Hispanic or Latino persons could be of any race.
§ Housing insecurity was defined as being unhoused or living in a congregate setting (e.g., dormitory, shelter, or hotel or motel).
¶ First locations of rash are not mutually exclusive.
 FIGURE. Self-reported activities* of mpox patients aged ≥18 years who did not report male-to-male sexual contact, by known† or unknown§ exposure to a person with suspected or confirmed mpox — United States, November 1–December 14, 2022
FIGURE. Self-reported activities* of mpox patients aged ≥18 years who did not report male-to-male sexual contact, by known† or unknown§ exposure to a person with suspected or confirmed mpox — United States, November 1–December 14, 2022
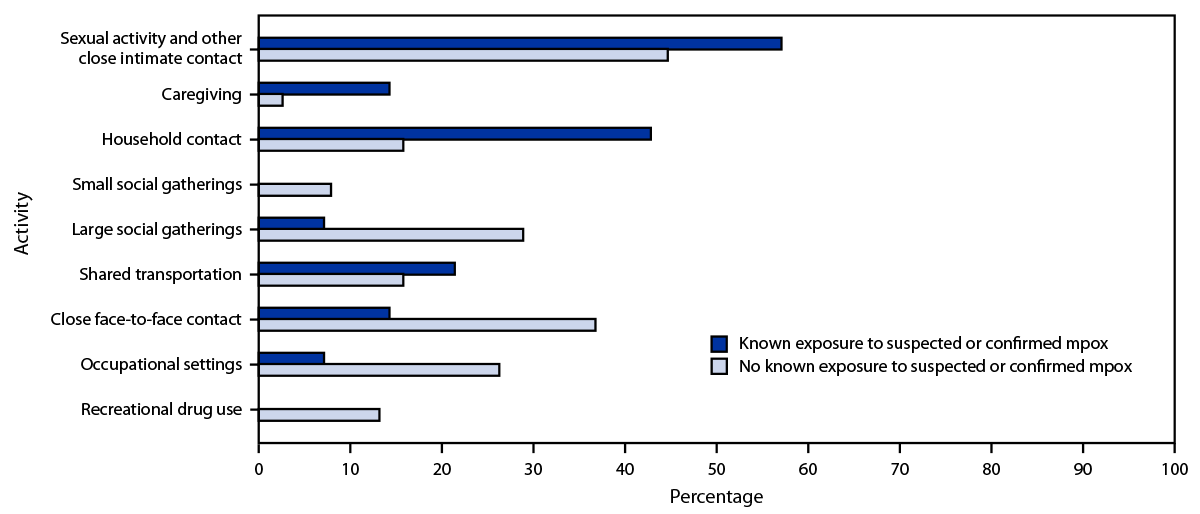
* Activities during the 3 weeks preceding symptom onset are not mutually exclusive.
† Percentages calculated out of 14.
§ Percentages calculated out of 38.
Suggested citation for this article: Sharpe JD, Charniga K, Byrd KM, et al. Possible Exposures Among Mpox Patients Without Reported Male-to-Male Sexual Contact — Six U.S. Jurisdictions, November 1–December 14, 2022. MMWR Morb Mortal Wkly Rep 2023;72:944–948. DOI: http://dx.doi.org/10.15585/mmwr.mm7235a2.
MMWR and Morbidity and Mortality Weekly Report are service marks of the U.S. Department of Health and Human Services.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All HTML versions of MMWR articles are generated from final proofs through an automated process. This conversion might result in character translation or format errors in the HTML version. Users are referred to the electronic PDF version (https://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.