State and Local Comprehensive Smoke-Free Laws for Worksites, Restaurants, and Bars — United States, 2015
Weekly / June 24, 2016 / 65(24);623–626
Michael A. Tynan1; Carissa Baker Holmes, MPH1; Gabbi Promoff, MA1; Cynthia Hallett, MPH2; Maggie Hopkins2; Bronson Frick2 (View author affiliations)
View suggested citationSummary
What is already known about this topic?
In 2006, the Surgeon General reported that there is no level of risk-free exposure to secondhand smoke. The only effective way to eliminate involuntary exposure to secondhand smoke is to eliminate smoking completely in all indoor areas.
What is added by this report?
The number of states that enacted statewide comprehensive smoke-free policies (i.e., no smoking allowed in worksites, restaurants, and bars) increased from zero in 2000 to 27 in 2015. Overall, nearly 50% of the U.S. population is protected by smoke-free laws. Although regional disparities remain, such as in the southeastern United States, substantive progress has been made adopting comprehensive smoke-free laws at the local level in some states in those areas.
What are the implications for public health practice?
Continued efforts to promote implementation of statewide and local comprehensive smoke-free laws are critical to protect nonsmokers from this preventable health hazard in the places they live, work, and gather.
Exposure to secondhand smoke from burning tobacco products causes stroke, lung cancer, and coronary heart disease in adults (1,2). Children who are exposed to secondhand smoke are at increased risk for sudden infant death syndrome, acute respiratory infections, middle ear disease, more severe asthma, respiratory symptoms, and slowed lung growth (1,2). Secondhand smoke exposure contributes to approximately 41,000 deaths among nonsmoking adults and 400 deaths in infants each year (2). This report updates a previous CDC report that evaluated state smoke-free laws in effect from 2000–2010 (3), and estimates the proportion of the population protected by comprehensive smoke-free laws. The number of states, including the District of Columbia (DC), with comprehensive smoke-free laws (statutes that prohibit smoking in indoor areas of worksites, restaurants, and bars) increased from zero in 2000 to 26 in 2010 and 27 in 2015. The percentage of the U.S. population that is protected increased from 2.72% in 2000 to 47.8% in 2010 and 49.6% in 2015. Regional disparities remain in the proportions of state populations covered by state or local comprehensive smoke-free policies, as no state in the southeast has a state comprehensive law. In addition, nine of the 24 states that lack state comprehensive smoke-free laws also lack any local comprehensive smoke-free laws. Opportunities exist to accelerate the adoption of smoke-free laws in states that lack local comprehensive smoke-free laws, including those in the south, to protect nonsmokers from the harmful effects of secondhand smoke exposure.
CDC assessed laws that completely prohibit smoking in all indoor areas of private-sector worksites, restaurants, and bars. These three venues were selected because they are a major source of secondhand smoke exposure for nonsmoking employees and the public (1–3). CDC considers a smoke-free law to be comprehensive if it prohibits smoking in indoor areas of all of these three venues. Some states and communities have enacted laws with less stringent smoking restrictions (e.g., provisions restricting smoking to designated areas or to separately ventilated areas); however, these laws do not eliminate secondhand smoke exposure (1).
Data on state smoke-free policies were obtained from CDC’s State Tobacco Activities Tracking and Evaluation (STATE) System database.* State legislation is collected quarterly from an online legal research database of state laws and is analyzed, coded, and entered into the STATE System. Data on local smoking restrictions and the percentage of the population covered were obtained from the American Nonsmokers’ Rights Foundation (ANRF) U.S. Tobacco Control Laws Database.† This database categorizes various types of U.S. municipal and county laws relating to tobacco, including smoking restrictions. Laws included in the database are identified through various means, including systematic scanning of tobacco control publications, websites, and e-mail discussion lists and through partnerships with the National Association of County and City Health Officials and the National Association of Local Boards of Health. The number of states with comprehensive smoke-free laws during 2000–2015 was assessed. The percentage of state populations with local comprehensive smoke-free laws and the percentage of the U.S. population that lives in a state or community with a comprehensive smoke-free law was calculated using 2007 U.S. Census data.
The number of states (including DC) with comprehensive smoke-free laws in effect increased from zero on December 31, 2000 to 26 on December 31, 2010 and 27 on December 31, 2015 (Figure). During 2011–2015, only North Dakota implemented a comprehensive smoke-free law. Among the 24 states that lack a comprehensive smoke-free law, five prohibit smoking in two of three venues; five prohibit smoking in one venue; eight allow smoking in ventilated or designated smoking areas; and six lack any statewide smoking restrictions (Table 1).
In some states without statewide comprehensive smoke-free laws, substantial progress has been made in adopting comprehensive smoke-free laws at the local level (Table 2). For example, although West Virginia has no statewide smoke-free law, local laws that prohibit smoking in worksites, restaurants, and bars provide protection for 60.1% of West Virginia’s population. Between one fourth and one third of a state’s population is protected through local comprehensive smoke-free laws in other states, such as Texas (36.6%), South Carolina (31.8%), Kentucky (31.4%), and Mississippi (24.2%). Overall, 49.6% of the U.S. population was protected by state or local comprehensive smoke-free laws as of December 31, 2015.
Nine of 24 states without comprehensive statewide smoke-free laws also lack any local comprehensive smoke-free laws; eight of the nine (Connecticut, Florida, New Hampshire, North Carolina, Oklahoma, Pennsylvania, Tennessee, and Virginia) have preemption statutes that prohibit adoption of local smoke-free laws (Table 2) (4).§ Nevada is the only one of these nine states where local comprehensive smoke-free laws are allowed, yet none have been adopted. Although local smoke-free laws are permitted in Georgia, Arkansas, and Wyoming, relatively few local comprehensive laws exist in those states.
Discussion
This report marks the 10-year anniversary of the 2006 U.S. Surgeon General’s report, The Health Consequences of Involuntary Exposure to Tobacco Smoke, which concluded that there is no risk-free level of secondhand smoke exposure (1). The report also found that completely eliminating smoking indoors was the only way to protect persons from involuntary exposure to secondhand smoke, and that separating smokers from nonsmokers, cleaning the air, and ventilating buildings cannot eliminate secondhand smoke exposure (1). Smoke-free laws have been shown to substantially improve indoor air quality, reduce secondhand smoke exposure, change social norms regarding the acceptability of smoking, prevent youth and young adult smoking initiation, and reduce heart attack and asthma hospitalizations among nonsmokers (1,2). Smoke-free laws aid smokers as well; for example, smoke-free laws increase smokers’ efforts to quit smoking (1,2). Although considerable progress has been made in adopting comprehensive smoke-free laws during the past two decades (3), as of December 31, 2015, half the U.S. population remained unprotected by a comprehensive smoke-free law at the state or local level.
In May 2016, California adopted a law eliminating exemptions in the state smoke-free law.¶ Those exemptions previously precluded CDC from considering California’s law as comprehensive. When California’s law became effective on June 9, 2016, the number of states that have a comprehensive smoke-free law increased to 28. With this change in California’s smoke-free status, it is estimated the proportion of the U.S. population protected by a comprehensive state or local law increased from 49.6% in December 2015 to nearly 60% in June 2016.
Exposure to secondhand smoke is not limited to private-sector worksites, restaurants, and bars. For example, casino workers are heavily exposed to secondhand smoke at work (5). Casinos are also not categorized as a private workplace in smoke-free tracking systems because they are sometimes excluded from laws and tracked as their own category (similar to restaurants and bars). In casinos where smoking is permitted, studies have consistently found substantial levels of secondhand smoke including in designated no-smoking areas of such casinos (5). CDC conducted a health hazard evaluation in three Las Vegas, Nevada, casinos, found nicotine and chemicals from secondhand smoke in the air, and determined that carcinogens from secondhand smoke were absorbed into workers’ bodies (6,7). Evidence from that evaluation led to a recommendation that smoking should be prohibited in these casinos (7). Further policy surveillance should be conducted to evaluate which states and communities prohibit smoking in casinos and other state-regulated gaming facilities, such as racetracks and card rooms.
Smoke-free laws can also be extended to other types of tobacco products, such as electronic nicotine delivery systems (ENDS), which include e-cigarettes (8). It is important for ENDS to be included in state and local smoke-free laws because indoor use of ENDS can expose nonusers to aerosolized nicotine and other harmful constituents, complicate smoke-free enforcement, and impact the social acceptability of tobacco use (2,8). Currently, approximately 350 communities and seven states (California,** Delaware, Hawaii, New Jersey, North Dakota, Oregon, and Utah) prohibit the use of ENDS in private worksites, restaurants, and bars.††
The findings in this report are subject to at least two limitations. First, the STATE System and ANRF only capture information on certain types of smoking restrictions, primarily laws and executive orders; therefore, this report does not include information on state or local administrative laws, regulations, or implementation guidelines. As a result, the manner in which a smoking statute is implemented or enforced in practice might differ from the way it is coded by CDC or ANRF. Second, because statewide smoke-free law information was based on data collected by CDC, and local smoke-free information is based on data collected by ANRF, differences in how laws are interpreted might occur, which could alter state and national population coverage estimates and could increase the total population covered by state comprehensive smoke-free laws. Therefore, national population estimates can be considered conservative.§§
Considerable progress has been made at state and local levels in the adoption of comprehensive smoke-free laws in indoor public places over the past two decades. However, even after considering the recent change in smoke-free status in California, state comprehensive smoke-free adoption progress has stalled in recent years (9), and no states in the southeast have a statewide comprehensive smoke-free law. Further, some states without comprehensive smoke-free laws legally prohibit local communities from adopting such laws to protect persons from secondhand smoke exposure. Persisting gaps in smoke-free protections leave large numbers of vulnerable populations exposed to secondhand smoke and could contribute to health disparities (10). Continued efforts to promote implementation of statewide and local comprehensive smoke-free laws are critical to protect nonsmokers from this preventable health hazard in the places they live, work, and gather.
Corresponding author: Michael A. Tynan, mtynan@cdc.gov, 404-498-1202.
1Office on Smoking and Health, National Center for Chronic Disease Prevention and Health Promotion, CDC; 2American Nonsmokers’ Rights Foundation, Berkeley, California.
References
- US Department of Health and Human Services. The health consequences of involuntary exposure to tobacco smoke: a report of the Surgeon General. Atlanta, GA: US Department of Health and Human Services, CDC; 2006. http://www.surgeongeneral.gov/library/secondhandsmoke/report
- US Department of Health and Human Services. The health consequences of smoking—50 years of progress. Atlanta, GA: US Department of Health and Human Services, CDC; 2014. http://www.cdc.gov/tobacco/data_statistics/sgr/50th-anniversary/index.htm
- CDC. State smoke-free laws for worksites, restaurants, and bars—United States, 2000–2010. MMWR Morb Mortal Wkly Rep 2010;60:472–5.
- CDC. State preemption of local tobacco control policies restricting smoking, advertising, and youth access—United States, 2000–2010. MMWR Morb Mortal Wkly Rep 2011;60:1124–7. PubMed
- Babb S, McNeil C, Kruger J, Tynan MA. Secondhand smoke and smoking restrictions in casinos: a review of the evidence. Tob Control 2015;24:11–7. CrossRef PubMed
- CDC. Health hazard evaluation report: environmental and biological assessment of environmental tobacco smoke exposure among casino dealers, Las Vegas, Nevada. Cincinnati, OH: US Department of Health and Human Services, CDC, National Institute for Occupational Safety and Health; 2009.
- Achutan C, West C, Mueller C, Bernert JT, Bernard B. Environmental tobacco smoke exposure among casino dealers. J Occup Environ Med 2011;53:346–51. CrossRef PubMed
- Marynak K, Holmes CB, King BA, Promoff G, Bunnell R, McAfee T. State laws prohibiting sales to minors and indoor use of electronic nicotine delivery systems—United States, November 2014. MMWR Morb Mortal Wkly Rep 2014;63:1145–50. PubMed
- Holmes CB, King BA, Babb SD. Stuck in neutral: stalled progress in statewide comprehensive smoke-free laws and cigarette excise taxes, United States, 2000–2014. Prev Chronic Dis 2016;13:E80. CrossRef PubMed
- Huang J, King BA, Babb SD, Xu X, Hallett C, Hopkins M. Sociodemographic disparities in local smoke-free law coverage in 10 states. Am J Public Health 2015;105:1806–13. CrossRef PubMed
* http://www.cdc.gov/tobacco/statesystem.
† http://www.no-smoke.org/pdf/SummaryUSPopList.pdf and http://www.no-smoke.org/pdf/percentstatepops.pdf.
§ In addition, although they lack any local smoke-free ordinances, the following states have statewide comprehensive smoke-free laws in effect, which could impact local enforcement of smoke-free provisions: Maine, Michigan, South Dakota, and Vermont.
¶ California enacted a law eliminating exemptions in the state smoke-free law, effective June 9, 2016. http://www.leginfo.ca.gov/pub/15-16/bill/asm/ab_0001-0050/abx2_7_bill_20160504_chaptered.pdf.
** California enacted a law that prohibits ENDS use, effective June 9, 2016. http://www.leginfo.ca.gov/pub/15-16/bill/sen/sb_0001-0050/sbx2_5_bill_20160504_chaptered.pdf.
†† http://www.no-smoke.org/pdf/ecigslaws.pdf.
§§ For example, CDC considered Colorado or New Mexico to have comprehensive smoke-free laws, although ANRF does not because of certain workplace exemptions for small employers. Therefore, population coverage estimates only account for 10.1% of Colorado and 36.6% of New Mexico populations. If these states were considered to have state comprehensive smoke-free laws, it is expected that the total population covered by smoke-free laws in the United States would increase.
 FIGURE. Statewide comprehensive* smoke-free air laws — United States,† December 31, 2015§
FIGURE. Statewide comprehensive* smoke-free air laws — United States,† December 31, 2015§
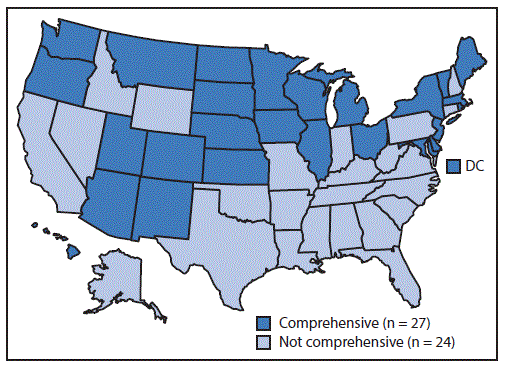
Source: CDC’s State Tobacco Activities Tracking and Evaluation System (http://www.cdc.gov/statesystem).
Abbreviation: DC = District of Columbia.
* Comprehensive = prohibited in worksites, restaurants, and bars.
† Includes District of Columbia.
§ California law became effective June 9, 2016.
 TABLE 1. State smoking restrictions* for worksites, restaurants, and bars in 24 states that do not have a comprehensive smoke-free law† – United States, December 31, 2015
TABLE 1. State smoking restrictions* for worksites, restaurants, and bars in 24 states that do not have a comprehensive smoke-free law† – United States, December 31, 2015
| State | Locations of smoking restrictions | ||
|---|---|---|---|
| Worksites | Restaurants | Bars | |
| Smoke-free in two locations (n = 5) | |||
| Florida | Smoke-free | Smoke-free | — |
| Indiana | Smoke-free | Smoke-free | — |
| Louisiana | Smoke-free | Smoke-free | — |
| Nevada | Smoke-free | Smoke-free | — |
| North Carolina | — | Smoke-free | Smoke-free |
| Smoke-free in one location (n = 5) | |||
| Arkansas | Smoke-free | Designated§ | — |
| Idaho | Designated | Smoke-free | — |
| New Hampshire | Designated | Smoke-free | — |
| Pennsylvania | Smoke-free | Ventilated | — |
| Tennessee | Smoke-free | Designated§ | — |
| Other restrictions (n = 8) | |||
| Alabama | Designated | — | — |
| Alaska | — | Designated | — |
| California¶ | Ventilated | Ventilated | Ventilated |
| Connecticut | Ventilated | Ventilated | Ventilated |
| Georgia | Designated | Designated§ | Designated§ |
| Missouri | Designated | Designated | Designated |
| Oklahoma | Designated | Ventilated | — |
| Virginia | — | Ventilated | Ventilated |
| No smoking restrictions (n = 6) | |||
| Kentucky | — | — | — |
| Mississippi | — | — | — |
| South Carolina | — | — | — |
| Texas | — | — | — |
| West Virginia | — | — | — |
| Wyoming | — | — | — |
Source: State Tobacco Activities Tracking and Evaluation System, Office on Smoking and Health, CDC.
*Smoke-free = no smoking allowed; designated = designated smoking areas required or allowed; ventilated = designated smoking areas allowed if separately ventilated.
† States with comprehensive smoke-free laws are those that require worksites, restaurants, and bars to be smoke-free.
§ State law allows smoking in venues that prohibit minors.
¶ Data reported as of December 31, 2015. However, California adopted a smoke-free law in May 2016, that became effective June 9, 2016, and eliminates exemptions that allow smoking in certain ventilated areas of locations; therefore, as of June 9, 2016, California is considered to have a comprehensive smoke-free law.
 TABLE 2. Percentage of state population with local comprehensive smoke-free laws* for 24 states that do not have a statewide comprehensive smoke-free law — United States, December 31, 2015
TABLE 2. Percentage of state population with local comprehensive smoke-free laws* for 24 states that do not have a statewide comprehensive smoke-free law — United States, December 31, 2015
| State | State population with local comprehensive smoke-free laws (%) |
|---|---|
| West Virginia | 60.1 |
| Alaska | 43.9 |
| Texas | 36.6 |
| South Carolina | 31.8 |
| Kentucky | 31.4 |
| California | 28.1 |
| Indiana | 26.8 |
| Mississippi | 24.2 |
| Missouri | 21.9 |
| Idaho | 13.6 |
| Alabama | 12.7 |
| Louisiana | 11.2 |
| Georgia | 2.4 |
| Arkansas | 0.5 |
| Wyoming | 0.3 |
| Connecticut† | 0.0 |
| Florida† | 0.0 |
| Nevada | 0.0 |
| New Hampshire† | 0.0 |
| North Carolina† | 0.0 |
| Oklahoma† | 0.0 |
| Pennsylvania† | 0.0 |
| Tennessee† | 0.0 |
| Virginia† | 0.0 |
Sources: CDC and American Nonsmokers’ Rights Foundation.
* Comprehensive smoke-free laws are those that require worksites, restaurants, and bars to be smoke-free.
† State law preempts local communities from enacting smoke-free laws.
Suggested citation for this article: Tynan MA, Holmes CB, Promoff G, Hallett C, Hopkins M, Frick B. State and Local Comprehensive Smoke-Free Laws for Worksites, Restaurants, and Bars — United States, 2015. MMWR Morb Mortal Wkly Rep 2016;65:623–626. DOI: http://dx.doi.org/10.15585/mmwr.mm6524a4.
MMWR and Morbidity and Mortality Weekly Report are service marks of the U.S. Department of Health and Human Services.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All HTML versions of MMWR articles are generated from final proofs through an automated process. This conversion might result in character translation or format errors in the HTML version. Users are referred to the electronic PDF version (https://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.