Ebola Surveillance — Guinea, Liberia, and Sierra Leone
Supplements / July 8, 2016 / 65(3);35–43
Lucy A. McNamara, PhD1; Ilana J. Schafer, DVM2; Leisha D. Nolen, MD, PhD3; Yelena Gorina, MPH, MS4; John T. Redd, MD5; Terrence Lo, PhD3; Elizabeth Ervin, MPH6; Olga Henao, PhD7; Benjamin A. Dahl, PhD8; Oliver Morgan, PhD9; Sara Hersey, MPH3; Barbara Knust, DVM6 (View author affiliations)
View suggested citationSummary
Developing a surveillance system during a public health emergency is always challenging but is especially so in countries with limited public health infrastructure. Surveillance for Ebola virus disease (Ebola) in the West African countries heavily affected by Ebola (Guinea, Liberia, and Sierra Leone) faced numerous impediments, including insufficient numbers of trained staff, community reticence to report cases and contacts, limited information technology resources, limited telephone and Internet service, and overwhelming numbers of infected persons. Through the work of CDC and numerous partners, including the countries’ ministries of health, the World Health Organization, and other government and nongovernment organizations, functional Ebola surveillance was established and maintained in these countries. CDC staff were heavily involved in implementing case-based surveillance systems, sustaining case surveillance and contact tracing, and interpreting surveillance data. In addition to helping the ministries of health and other partners understand and manage the epidemic, CDC’s activities strengthened epidemiologic and data management capacity to improve routine surveillance in the countries affected, even after the Ebola epidemic ended, and enhanced local capacity to respond quickly to future public health emergencies. However, the many obstacles overcome during development of these Ebola surveillance systems highlight the need to have strong public health, surveillance, and information technology infrastructure in place before a public health emergency occurs. Intense, long-term focus on strengthening public health surveillance systems in developing countries, as described in the Global Health Security Agenda, is needed.
The activities summarized in this report would not have been possible without collaboration with many U.S and international partners (http://www.cdc.gov/vhf/ebola/outbreaks/2014-west-africa/partners.html).
Introduction
Accurate, timely surveillance data are critical during public health emergencies because these data can provide the information needed for appropriate resource allocation, assessment of the success of response, and planning for staffing and resource needs. This was especially true during the 2014–2016 Ebola virus disease (Ebola) epidemic in West Africa. During the epidemic, CDC, along with many other organizations, overcame challenges to conducting effective surveillance in the three countries that were heavily affected (Guinea, Liberia, and Sierra Leone) and had limited public health infrastructure.
Establishing, Maintaining, and Improving Ebola Surveillance
Ebola surveillance in Guinea, Liberia, and Sierra Leone had two primary components: 1) case investigation and reporting and 2) contact tracing. Although other components of Ebola surveillance, such as community event-based surveillance, were important in these countries, case reporting and contact tracing made up the core of Ebola surveillance and are the focus of this report. Effective case reporting requires timely collection, reporting, and integration of epidemiologic, clinical, laboratory, and outcome data on all suspected, probable, and confirmed Ebola cases. These data help response staff understand the current impact and distribution of Ebola in the country and provide insight into whether the response is succeeding and where future response efforts should be targeted. Meanwhile, contact tracing promotes rapid identification of new cases and referral of those case-patients to isolation units, thereby improving clinical outcomes and reducing opportunities for transmission. Contact tracing requires individual tracking of each contact for 21 days after exposure and constant, effective community engagement (1).
By the end of the epidemic, the overall components of Ebola surveillance were similar in all three countries. Cases initially were identified through contact tracing; case-finding; or additional surveillance mechanisms, such as calls to the national alert system (2) and walk-ins to Ebola treatment units (ETUs), holding centers, and hospitals (Figure 1). Once a possible case was identified, surveillance staff gathered additional information about the possible case-patient and his or her contacts (Figure 1). Case data were then compiled at the prefecture, county, or district level in a local database or line list and transmitted to ministry of health staff working at the national level. Meanwhile, local staff initiated contact tracing to observe each contact’s health for 21 days after exposure. Contact lists were sometimes shared with the national level, but detailed contact tracing information usually was retained and used only locally. However, despite these broad similarities, surveillance system structure and information flow varied widely among areas.
Challenges to obtaining case-level information in Guinea, Liberia, and Sierra Leone included reluctance of some communities to report cases; few and often inadequately trained outbreak response staff to collect, enter, synthesize, and analyze surveillance data; and difficulties in coordinating the many groups involved with surveillance and the response. Compounding these difficulties, particularly in Liberia and Sierra Leone, was the exponential increase in the number of cases reported during summer and fall 2014, which made timely collection and compilation of case information by surveillance staff increasingly difficult.
Despite these issues, Ebola surveillance was continuously maintained in each of the three countries heavily affected by Ebola. Data gathered through these surveillance systems are not complete or perfectly accurate, but they enabled analyses of case characteristics, risk factors for infection, and changes in case distribution over time (3–5). The data also were used to inform the indicators by which specific components of the Ebola response in the three countries were assessed. CDC’s process indicators (Box) enabled identification of gaps in surveillance data and communicated progress toward ending the epidemic to U.S. government leaders.
Guinea
The first CDC team deployed to Guinea soon after the outbreak was identified in March 2014. This team, along with the Guinean Ministry of Health and Public Hygiene (MoH) and the World Health Organization (WHO), immediately began work on an Ebola surveillance system. The CDC team set up a national database using CDC’s Epi Info Viral Hemorrhagic Fever (VHF) application (http://epiinfovhf.codeplex.com/releases/), development of which began in early 2013. CDC provided on-site programming assistance to continue development and modify the application to suit local needs and trained partner organization staff to use this database. Within 2 weeks after outbreak identification, the database was being used daily to compile up-to-date case information from the initially affected prefectures (Gueckedou, Macenta, and Kissidougou and the capital city of Conakry) and to produce national situation reports. These data were also shared with WHO, which produced international situation reports that were then shared with CDC and other partners. WHO and the MoH continued to use this database throughout the emergency response.
Along with the MoH, Médecins Sans Frontières, and numerous other partners, CDC facilitated development and implementation of case identification and contact tracing procedures in Conakry and Gueckedou. The CDC team played a particularly critical role in starting contact tracing in Conakry by training contact tracers, organizing the contact tracing system, and implementing an initial system for contact data management using the Epi Info VHF application (transitioned to Microsoft Excel in August 2014). In rural areas, CDC staff supported contact tracing through data management, training, and quality control through direct supervision of local contact tracers. The CDC team also introduced a standardized case investigation form and trained partners to use the form. Finally, CDC staff helped coordinate transfer of Ebola case information from ETUs to data entry staff and helped verify and clean data entered into the national database.
Beginning in September 2014, the growing number of CDC response staff in Guinea enabled CDC to expand its support to the MoH and WHO through more intense field-based case finding, contact listing and tracing, and case and contact investigations. CDC staff focused on improving rigor and oversight of these activities with the goal of improving documentation of each chain of transmission, which in turn improved investigation of cross-prefecture and cross-border movement of contacts.
Still, full implementation of strong case identification and contact tracing procedures sometimes lagged substantially behind the appearance of cases in affected prefectures (e.g., 6), in part because of limited numbers of trained staff and reliance on insufficiently supervised community agents (community members who each day check on contacts within their own or neighboring villages). To overcome this difficulty, CDC worked with the MoH and other partners to strengthen case investigations and contact tracing and to supplement passive case reporting with active case finding, including house-to-house visits in affected areas (6,7). However, some persons and communities resisted surveillance efforts by not disclosing the status of contacts or cases or refusing to allow outbreak response staff into villages, which resulted in missed cases and increased transmission (8) (CDC, unpublished data, 2014–2015). Nevertheless, as of May 13, 2016, Guinea had not reported any Ebola cases since the last Ebola patient twice tested negative on April 19, 2016.
Liberia
Liberia’s Ministry of Health and Social Welfare (renamed Ministry of Health [MoH] in October 2014) began surveillance when the first Ebola cases appeared in Liberia in March 2014 (9); however, when no new cases were reported during late April–early June, surveillance was discontinued. When Ebola resurged in mid-June 2014, the MoH reestablished surveillance and began obtaining aggregate case counts from each county daily by telephone or e-mail. The CDC team that arrived in July 2014 immediately began collaborating with the MoH, WHO, and other partners on a case-based surveillance system, in which detailed information about each case is reported individually, to obtain more comprehensive and accurate information about the epidemic.
Initially, case-based surveillance data from throughout the country were transmitted by Excel line lists and paper forms to the MoH in Monrovia, where they were entered into an Epi Info VHF database. Lofa County started a second database in mid-August 2014 to compile data for that county; this database was then transmitted to the MoH (daily when possible) to maintain a complete national database. During this period, however, Ebola incidence in Liberia increased much faster than data management capacity. The rapid increase in cases led to a quickly growing backlog of information to enter into the case-based surveillance database. To address this backlog, CDC staff performed data entry, trained new data entry and management staff, and fixed numerous software and hardware issues that hindered data entry.
CDC staff also initiated key improvements to the case-based surveillance system. In late August 2014, CDC and MoH staff implemented preprinted unique identification (ID) stickers that could be used on, for example, case report forms and laboratory samples to facilitate linking of multiple pieces of information pertaining to the same case-patient. In early September, CDC staff collaborated with the MoH to introduce a shorter case report form to make form completion and data entry easier. CDC staff also helped organize the surveillance and laboratory data flow, which faced logistical obstacles because of the outbreak’s broad geographic scale and the large number of partners involved in surveillance (Figure 2). Finally, CDC helped the MoH design and run surveillance training sessions for county public health staff to improve case finding, contact tracing, and case reporting throughout the country.
As the case-based surveillance system developed, comparisons with the aggregate case data received from telephone calls and e-mails demonstrated that the latter were inaccurate. Therefore, in October 2014 Liberia’s national situation reports transitioned reporting from aggregate case data to case-based data from laboratory and ETU line lists. This change resulted in an increase of 1,870 reported* cases during October 25–29, 2014 (Figure 3). Meanwhile, each county began to manage and enter data into its own case database rather than sending case identification forms to the MoH for entry. The initial plan was for each county to send an updated Epi Info VHF database to the MoH daily to maintain the national database. However, limited Internet connectivity, lags in data entry, and problems combining databases made this system unsustainable. Liberia switched to the District Health Information Software system (https://www.dhis2.org) (Health Information Systems Programme) for data transmission and management beginning in December 2014; even after this change, however, substantial lags in data entry meant that these detailed data were inaccurate for current case counts and difficult to directly apply to outbreak control.
As the incidence rate of Ebola in Liberia declined in October–December 2014, renewed emphasis was placed on controlling outbreaks in remote communities through active case finding, contact tracing, and community education (10,11). The MoH, CDC, and numerous partners conducted rapid response investigations in outlying areas of Liberia during October–November 2014 to establish patient care strategies and enhance contact tracing, active surveillance, and other response activities (12). In Montserrado County, CDC worked with county staff and partner agencies, especially Action Contre la Faim, to implement decentralized, sector-based contact tracing in January 2015; this approach resulted in more complete contact tracing and helped eliminate transmission in this area (13). Cases in Liberia subsequently dropped to zero from late May until early July 2015 and have remained at zero except for small clusters of illness in July and November 2015 and March–April 2016.
After initially reaching zero cases, Liberia maintained surveillance through Ebola testing of dead bodies and health facility patients with symptoms consistent with suspected Ebola; community event–based surveillance to trigger alerts for events (e.g., suspicious deaths) associated with Ebola transmission in communities bordering neighboring countries; and establishment of isolation, infection control, and triage protocols at health facilities nationwide. Along with strengthening integrated disease surveillance and response for hemorrhagic fevers and priority diseases with symptoms that overlap with those of Ebola, these measures promoted rapid detection and control of new Ebola clusters.
Sierra Leone
When the CDC team arrived in Sierra Leone in early August 2014, the country already had reported approximately 550 Ebola cases. The team found that, because of Sierra Leone’s decentralized health system, districts were taking different approaches to control the epidemic, including using differing case definitions. CDC, WHO, the Sierra Leone Ministry of Health and Sanitation (MoHS), and other partners quickly began creation of a consistent national surveillance system. The CDC team helped develop and train local staff on standardized procedures for case notification, investigation, and reporting, as well as on standardized definitions of Ebola infection, transmission, and control, leading to standardization of case investigation protocols throughout the country.
Although Sierra Leone’s surveillance system is similar in many ways to those in Guinea and Liberia, it has several unique features. For example, beginning in October 2014, Sierra Leone’s policy was that all deaths, not just those of persons whose illness met the Ebola case definition, would be tested for Ebola, a unique approach that enabled Ebola laboratory result records to double as a short-term death registry. Sierra Leone also used multidisciplinary field teams to conduct periodic “surges” of house-to-house active case finding beginning with Western Area (Freetown and surrounding region) in December 2014.
The initial CDC teams also implemented Epi Info VHF databases that could be controlled and maintained at the district level but combined and analyzed nationally. The national Epi Info VHF database was maintained through the end of the epidemic and is often used for national-level and international-level data analyses because it provides the most comprehensive epidemiologic and laboratory data on Ebola cases available in Sierra Leone. However, a major challenge to Sierra Leone’s surveillance early in the epidemic was difficulty getting information from ETUs to district surveillance officers. As a result, patients’ families often lacked information about the status or location of their loved ones, and patient outcome data collected in the surveillance system were highly incomplete. An analysis conducted in September 2014 demonstrated that although Sierra Leone’s Ebola case-fatality rate appeared to be 31.6% when all reported confirmed and probable cases were included, the rate actually was 69.0% when only those with definitive outcome data available were included (5).
Throughout the epidemic,† CDC helped strengthen Ebola surveillance and contact tracing in Sierra Leone. CDC staff provided daily contact tracing support to the district surveillance officers and helped develop consistent messaging to counteract the fear and mistrust that lead to community resistance to case investigation and contact tracing. In October 2014, CDC worked with the International Rescue Committee and the Bo District Health Management Team to develop and implement community event–based surveillance to supplement case finding and contact tracing, an initiative piloted in Bo and then adopted as part of the national surveillance strategy (14). CDC helped train local contact tracing staff beginning with Bo district in November 2014 and January 2015; CDC also helped support the “Western Area surge” strategy (15) implemented in December 2014, in which many additional district surveillance officers, contact tracers, and community mobilizers were recruited and trained across Western Area. The surge greatly improved contact tracing capacity in this region.
In January 2015, CDC staff helped distribute and train local and partner staff to use an updated case identification form with water-resistant unique ID stickers that enabled use of a universal ID by the laboratory, ETU, and district surveillance officers. CDC staff also were pivotal in identifying laboratory performance and coordination issues and, for some districts, distributing laboratory results to surveillance staff to help with contact tracing and patient management.
Key Challenges to Ebola Surveillance
Case Definitions
Lack of a consistent Ebola case definition was an early impediment in the response. In Guinea and Liberia, involvement of CDC teams and their partners early in the response led to rapid adoption of a case definition similar to the one used by WHO and CDC (16). In contrast, in Sierra Leone, many districts initially adopted a narrower case definition requiring fever, vomiting, diarrhea, and one additional symptom. Use of this narrower case definition probably resulted in many missed cases early in the epidemic. After the CDC team arrived in Sierra Leone, CDC and Sierra Leone MoHS staff aligned the case definition with those in the neighboring countries, resulting in adoption of a broader case definition in mid-August 2014. However, even after central adoption of the new case definition, ensuring nationwide application of this definition was difficult. Only after several months did all the rural districts adopt the new version. Earlier nationwide standardization would have improved and unified the response in Sierra Leone.
Case Data Collection
Throughout the epidemic, missing case data and underreporting of cases were serious obstacles to obtaining accurate surveillance data. Many factors contributed to the often substantial amount of missing data on each reported case, including insufficient training of case investigation staff, logistical difficulties in getting case investigation forms to all parties who identified cases, and inadequate time to find and complete the initial case investigation form, which proved too long given the often overwhelming number of cases identified. CDC staff helped resolve these issues by training case investigation staff at the national and local levels and developing a shorter case investigation form. Meanwhile, underreporting of cases also was substantial; published estimates suggest that the true number of cases in some areas might have been 17%–250% higher than the number reported (17,18). Underreporting and missing data substantially impaired the ability of surveillance staff to understand the true magnitude and distribution of the epidemic and highlighted the need for streamlined, standardized, and flexible case reporting tools that could be easily adapted to accommodate infectious disease outbreaks, especially outbreaks of new or uncommon diseases.
Laboratory Testing
When the number of infected persons dramatically increased in Liberia and Sierra Leone in July 2014, few laboratories in-country were equipped to test samples from Ebola patients, resulting in substantial delays in sample transport, testing, and reporting. Difficulties linking laboratory results with epidemiologic data exacerbated reporting delays. In some instances, sample testing and reporting were delayed a week or longer, which hindered use of test results for patient management. To improve in-country laboratory capacity, CDC and the National Institutes of Health established an additional laboratory in Monrovia, Liberia, in August 2014; CDC also established a laboratory in Kenema, Sierra Leone (later moved to Bo), that tested up to 180 samples each day at the peak of the epidemic. Expanding laboratory capacity improved patient management and the overall function of the surveillance system and resulted in a shift toward reporting primarily confirmed cases (rather than suspected or probable cases) from all three countries by December 2014. The difficulties encountered in providing timely laboratory testing during this epidemic highlight the need to expand public health laboratory capacity in these countries.
Contact Tracing
Contact tracing teams in Guinea, Liberia, and Sierra Leone often were hindered by inadequate staffing to follow the sometimes enormous number of contacts, difficulties reaching remote villages, inadequate pay, and insufficient training. However, one of the greatest difficulties in contact tracing was community mistrust of contact tracers and other outbreak response staff. For example, this mistrust motivated individual contacts to deny their exposures and/or hide or flee from contact tracers and communities to bar outbreak response staff from entering or even erupt into violence (7,8,19) (CDC, unpublished data, 2014–2015). CDC staff in many areas of Guinea, Liberia, and Sierra Leone were physically threatened by local communities and forced to evacuate; other outbreak staff were injured and even killed by angry community members (7). Creating a strong network of trusted local health care workers to provide information and assistance during a public health crisis is critical to preventing such resistance during future public health emergencies.
Information Technology
Information technology (IT) is essential during a public health emergency for data to be rapidly collected, synthesized, and used to provide information for the response. Guinea, Liberia, and Sierra Leone had limited IT and communications infrastructure. Internet and cell phone service are inadequate in many areas, especially in rural areas; power outages occur frequently; and availability of servers, routers, and other IT equipment is limited. In addition, in-country IT expertise is limited: only a tiny proportion of the population has the basic computer skills needed for data entry tasks, let alone the training to set up or troubleshoot IT systems.
To support Ebola surveillance, CDC has, by necessity, supported IT needs in the three countries through both on-site and remote assistance. This support included assistance setting up servers and other equipment, technical support and development of the Epi Info VHF application, and IT and computer training for local staff. In Sierra Leone, for instance, beginning in November 2014, CDC and WHO trained MoHS staff on data management, Microsoft Excel, the Epi Info VHF application, and computer security. Development of improved IT and communications infrastructure (especially increasing Internet access nationwide) and extensive IT training for local staff is needed to resolve the limitations in IT capacity in these and other countries before the next public health emergency.
Case Data Management
In Guinea, Liberia, and Sierra Leone, CDC staff were key to establishing and maintaining data management systems for case-based surveillance. Staff working on these systems faced numerous obstacles, including limited communications infrastructure, software and hardware issues, limited computer expertise among local staff, insufficient funding to pay local data entry and management staff, and often systemic problems with the surveillance system (Figure 2) that resulted in low-quality incoming data. In addition, the huge volume of cases during summer and fall 2014 made obtaining, entering, cleaning, and verifying data on all cases particularly difficult and led to a high frequency of missing or erroneous data. These problems made using case-based surveillance strategies for timely case reporting difficult and highlight the need for robust surveillance and data management systems and extensive training and support to in-country users on the use of these systems before a public health emergency occurs.
Contact Data Management
Managing contact tracing data is complex and time-consuming at the best of times because of the difficulty of maintaining an accurate contact list and the need to record each contact’s follow-up information daily. Because of the complexity of contact data management and limited numbers of local data management staff, CDC frequently assisted with contact data management in the countries heavily affected by Ebola, especially in rural areas.
Software for contact data management was limited. Excel was often used for this purpose in the three countries, but it lacks automated functions suitable for managing contact data. The frequent manipulations needed to update contact lists often resulted in substantial errors in the data. Paper-based systems have similar flaws and make analyzing contact data or sharing data among partners more difficult. Other software systems were implemented only occasionally. For instance, the mobile Sense Follow-up application (https://play.google.com/store/apps/details?id=com.ehealthafrica.lrsenseebola) was used in Montserrado and Margibi counties in Liberia to manage contact tracing around a small cluster of cases in mid-2015. CDC developed the Epi Info VHF application specifically to facilitate and link case and contact tracing data management for outbreaks of Ebola and other viral hemorrhagic fevers; however, limited flexibility in the application, difficulties changing contact tracing systems, limited familiarity with the contact tracing features of the application, and ongoing application development during the epidemic led to use of this tool as the primary contact data management tool in only a few areas, notably Kambia District, Sierra Leone. To prepare for future viral hemorrhagic fever outbreaks, it would be beneficial for CDC, WHO, and their partners to agree on and pilot a single contact data management software tool that can be quickly and easily implemented when needed.
Conclusion
Developing Ebola surveillance in Guinea, Liberia, and Sierra Leone was difficult because of the need to implement timely, accurate surveillance under emergency conditions over a wide area. The Ebola responders conducted impressive and meaningful work supporting Ebola surveillance in these three countries; however, the many challenges faced during surveillance implementation highlight the need to be prepared for public health emergencies before they occur. CDC and its partners can facilitate the public health response by developing and agreeing on standardized response systems with clear protocols and objectives before outbreaks occur and rapidly implementing these systems during an outbreak. In addition, CDC and other public health partners need to continue to support development of strong, sustainable public health surveillance, data management, and IT infrastructure and training in developing countries, as described in the Global Health Security Agenda (20), to frame the response to future public health emergencies. With the establishment of CDC offices in Guinea, Liberia, and Sierra Leone, CDC is well-positioned to continue supporting the expansion of public health and surveillance capacity infrastructure to improve the response to future epidemics.
Acknowledgments
Sheree Boulet and Hannah Gould provided information about CDC’s process indicators. Candice Robinson provided the initial draft of Figure 1.
Corresponding author: Lucy A. McNamara, Division of Bacterial Diseases, National Center for Immunization and Respiratory Diseases, CDC. Telephone: 404-639-8743; E-mail: LMcNamara@cdc.gov.
1Division of Bacterial Diseases, National Center for Immunization and Respiratory Diseases, CDC; 2Division of Health Informatics and Surveillance, Center for Surveillance, Epidemiology, and Laboratory Services, CDC; 3Division of Global Health Protection, Center for Global Health, CDC; 4Office of Analysis and Epidemiology, National Center for Health Statistics, CDC; 5Ebola-Affected Countries Office, Center for Global Health, CDC; 6Division of High-Consequence Pathogens and Pathology, National Center for Emerging and Zoonotic Infectious Diseases, CDC; 7Division of Foodborne, Waterborne, and Environmental Diseases, National Center for Emerging and Zoonotic Infectious Diseases, CDC; 8Global Immunization Division, Center for Global Health, CDC; 9Division of Preparedness and Emerging Infections, National Center for Emerging and Zoonotic Infectious Diseases, CDC
References
- CDC. CDC methods for implementing and managing contact tracing for Ebola virus disease in less-affected countries. Atlanta, GA: US Department of Health and Human Services, CDC; 2015. http://www.cdc.gov/vhf/ebola/pdf/contact-tracing-guidelines.pdf
- Miller LA, Stanger E, Senesi RG, et al. Use of a nationwide call center for Ebola response and monitoring during a 3-day house-to-house campaign—Sierra Leone, September 2014. MMWR Morb Mortal Wkly Rep 2015;64:28–9. PubMed
- Dietz PM, Jambai A, Paweska JT, Yoti Z, Ksaizek TG. Epidemiology and risk factors for Ebola virus disease in Sierra Leone—23 May 2014 to 31 January 2015. Clin Infect Dis 2015;61:1648–54. PubMed
- Faye O, Boëlle PY, Heleze E, et al. Chains of transmission and control of Ebola virus disease in Conakry, Guinea, in 2014: an observational study. Lancet Infect Dis 2015;15:320–6. CrossRef PubMed
- WHO Ebola Response Team. Ebola virus disease in West Africa—the first 9 months of the epidemic and forward projections. N Engl J Med 2014;371:1481–95. CrossRef PubMed
- Victory KR, Coronado F, Ifono SO, Soropogui T, Dahl BA. Ebola transmission linked to a single traditional funeral ceremony—Kissidougou, Guinea, December, 2014–January 2015. MMWR Morb Mortal Wkly Rep 2015;64:386–8. PubMed
- Enserink M. Infectious diseases. In Guinea, a long, difficult road to zero Ebola cases. Science 2015;348:485–6. CrossRef PubMed
- Dixon MG, Taylor MM, Dee J, et al. Contact tracing activities during the Ebola virus disease epidemic in Kindia and Faranah, Guinea, 2014. Emerg Infect Dis 2015;21:2022–8. CrossRef PubMed
- Sharma A, Heijenberg N, Peter C, et al. Evidence for a decrease in transmission of Ebola virus—Lofa County, Liberia, June 8–November 1, 2014. MMWR Morb Mortal Wkly Rep 2014;63:1067–71. PubMed
- Blackley DJ, Lindblade KA, Kateh F, et al. Rapid intervention to reduce Ebola transmission in a remote village—Gbarpolu County, Liberia, 2014. MMWR Morb Mortal Wkly Rep 2015;64:175–8. PubMed
- Hagan JE, Smith W, Pillai SK, et al. Implementation of Ebola case-finding using a village chieftaincy taskforce in a remote outbreak—Liberia, 2014. MMWR Morb Mortal Wkly Rep 2015;64:183–5. PubMed
- Nyenswah T, Fahnbulleh M, Massaquoi M, et al. Ebola epidemic—Liberia, March–October 2014. MMWR Morb Mortal Wkly Rep 2014;63:1082–6. PubMed
- Nyenswah T, Fallah M, Sieh S, et al. Controlling the last known cluster of Ebola virus disease—Liberia, January–February 2015. MMWR Morb Mortal Wkly Rep 2015;64:500–4. Erratum in MMWR Morb Mortal Wkly Rep 2015;64:806. PubMed
- Crowe S, Hertz D, Maenner M, et al. A plan for community event-based surveillance to reduce Ebola transmission—Sierra Leone, 2014–2015. MMWR Morb Mortal Wkly Rep 2015;64:70–3. PubMed
- World Health Organization. Sierra Leone: Western Area surge combats Ebola proactively. Geneva, Switzerland: World Health Organization; 2014. http://www.who.int/features/2014/ebola-western-area-surge/en/
- World Health Organization. Case definition recommendations for Ebola or Marburg virus diseases. Geneva, Switzerland: World Health Organization; 2014. http://www.who.int/csr/resources/publications/ebola/ebola-case-definition-contact-en.pdf
- Meltzer MI, Atkins CY, Santibanez S, et al. Estimating the future number of cases in the Ebola epidemic—Liberia and Sierra Leone, 2014–2015. MMWR Suppl 2014;63(No. Suppl 3).
- Scarpino SV, Iamarino A, Wells C, et al. Epidemiological and viral genomic sequence analysis of the 2014 Ebola outbreak reveals clustered transmission. Clin Infect Dis 2015;60:1079–82. PubMed
- Cohn S, Kutalek R. Historical parallels, Ebola virus disease and cholera: understanding community distrust and social violence with epidemics. PLoS Curr 2016;8:pii. PubMed
- CDC. The Global Health Security Agenda. Atlanta, GA: US Department of Health and Human Services, CDC; 2016. http://www.cdc.gov/globalhealth/security/ghsagenda.htm
* Suspected, probable, or confirmed cases reported to the MoH.
† As of May 13, 2016, Sierra Leone had not identified any Ebola cases since the last Ebola patient was discharged on February 5, 2016.
 FIGURE 1. Ebola surveillance network — Bo District, Sierra Leone, late November 2014
FIGURE 1. Ebola surveillance network — Bo District, Sierra Leone, late November 2014
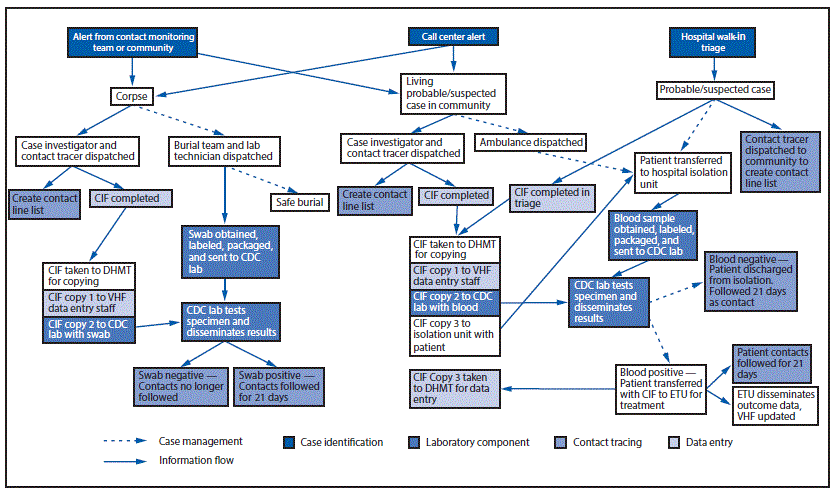
Abbreviations: CIF = case investigation form; DHMT = District Health Management team; Ebola = Ebola virus disease; ETU = Ebola treatment unit; VHF = Epi Info Viral Hemorrhagic Fever application.
 BOX. Process indicators of CDC’s response to the 2014–2016 Ebola virus disease epidemic — West Africa, 2015*
BOX. Process indicators of CDC’s response to the 2014–2016 Ebola virus disease epidemic — West Africa, 2015*
-
National emergency management program established, functional, and intraconnected (yes/no)
-
Percentage of affected subnational units with access to adequate bed capacity
-
Percentage of new laboratory tests that are positive for Ebola
-
Percentage of suspected community deaths of persons testing positive for Ebola
-
Percentage of calls to burial teams responded to within 24 hours after request
-
Percentage of cases that occur among known and monitored contacts
-
Percentage of new infections among health care workers
-
Percentage of respondents who report willingness to visit a health care facility if symptoms appear
* Indicators were updated periodically during the epidemic to reflect current information needs.
 FIGURE 2. National surveillance data flow for reporting Ebola — Liberia, late August 2014
FIGURE 2. National surveillance data flow for reporting Ebola — Liberia, late August 2014
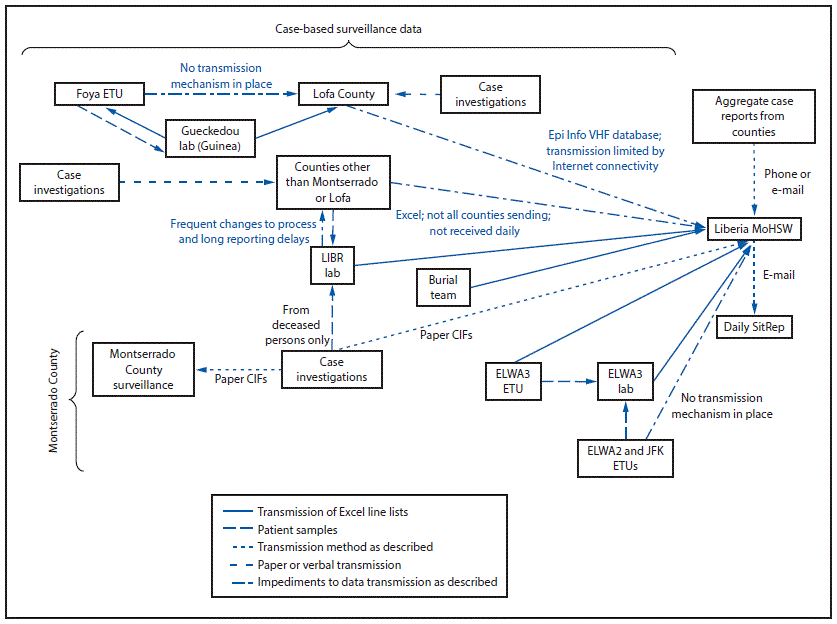
Abbreviations: CIF = case investigation form; Ebola = Ebola virus disease; ELWA = Eternal Love Winning Africa; ETU = Ebola treatment unit; Excel = Microsoft Excel; JFK = John F. Kennedy; LIBR = Liberia Institute for Biomedical Research; MoHSW = Ministry of Health and Social Welfare; SitRep = situation report; VHF = Viral Hemorrhagic Fever application.
 FIGURE 3. Total number of reported* suspected, probable, and confirmed cases of Ebola as reported through World Health Organization situation reports — Guinea, Liberia, and Sierra Leone, March 2014–July 29, 2015†
FIGURE 3. Total number of reported* suspected, probable, and confirmed cases of Ebola as reported through World Health Organization situation reports — Guinea, Liberia, and Sierra Leone, March 2014–July 29, 2015†
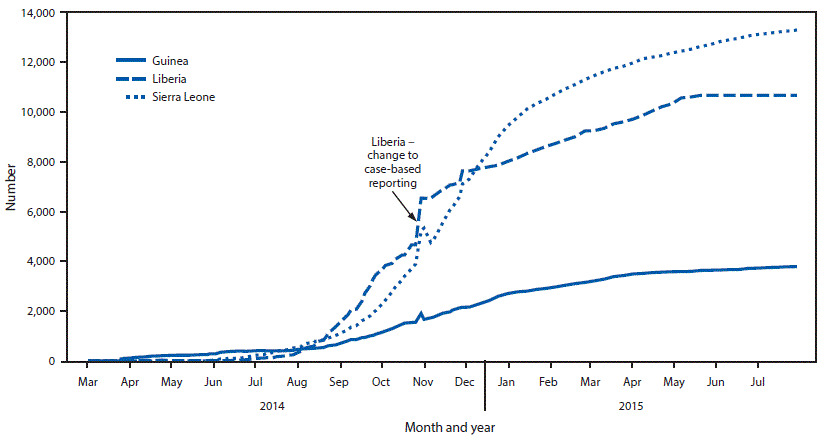
Abbreviation: Ebola = Ebola virus disease.
* Suspected, probable, or confirmed cases reported to ministries of health.
† Figure highlights increase in reported cases from Liberia due to transition from aggregate to case-based reporting in October 2014. Reported case counts temporarily increased in Guinea and Sierra Leone during the same period. Shortly thereafter, reported case counts for Guinea decreased again as several hundred cases initially reported as suspected were reclassified. Meanwhile, reported case counts from Sierra Leone also decreased because the World Health Organization shifted data sources from a combination of patient databases and country situation reports to national reports only.
Suggested citation for this article: McNamara LA, Schafer IJ, Nolen LD, et al. Ebola Surveillance — Guinea, Liberia, and Sierra Leone. MMWR Suppl 2016;65(Suppl-3):35–43. DOI: http://dx.doi.org/10.15585/mmwr.su6503a6.
MMWR and Morbidity and Mortality Weekly Report are service marks of the U.S. Department of Health and Human Services.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All HTML versions of MMWR articles are generated from final proofs through an automated process. This conversion might result in character translation or format errors in the HTML version. Users are referred to the electronic PDF version (https://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.