Safe and Effective Deployment of Personnel to Support the Ebola Response — West Africa
Supplements / July 8, 2016 / 65(3);90–97
Please note: An erratum has been published for this report. To view the erratum, please click here.
Edward N. Rouse, MPA1; Shauna Mettee Zarecki, MSN, MPH1; Donald Flowers, MS, MSS1; Shawn T. Robinson1; Reed J. Sheridan1; Gary D. Goolsby1; Jeffrey Nemhauser, MD2; Sachiko Kuwabara, PhD1 (View author affiliations)
View suggested citationSummary
From the initial task of getting “50 deployers within 30 days” into the field to support the 2014–2016 Ebola virus disease (Ebola) epidemic response in West Africa to maintaining well over 200 staff per day in the most affected countries (Guinea, Liberia, and Sierra Leone) during the peak of the response, ensuring the safe and effective deployment of international responders was an unprecedented accomplishment by CDC. Response experiences shared by CDC deployed staff returning from West Africa were quickly incorporated into lessons learned and resulted in new activities to better protect the health, safety, security, and resiliency of responding personnel. Enhanced screening of personnel to better match skill sets and experience with deployment needs was developed as a staffing strategy. The mandatory predeployment briefings were periodically updated with these lessons to ensure that staff were aware of what to expect before, during, and after their deployments. Medical clearance, security awareness, and resiliency programs became a standard part of both predeployment and postdeployment activities. Response experience also led to the identification and provision of more appropriate equipment for the environment. Supporting the social and emotional needs of deployed staff and their families also became an agency focus for care and communication. These enhancements set a precedent as a new standard for future CDC responses, regardless of size or complexity.
The activities summarized in this report would not have been possible without collaboration with many U.S and international partners (http://www.cdc.gov/vhf/ebola/outbreaks/2014-west-africa/partners.html).
Background
Because of the size and scope of the 2014–2016 Ebola virus disease (Ebola) epidemic in West Africa, CDC leaders activated the Incident Management System (IMS) and began coordinating its response from CDC’s Emergency Operations Center on July 9, 2014. At CDC, the IMS comprises a staffing structure and standardized operating procedures that are used to coordinate various response components and functions in areas such as surveillance, laboratory testing, operations, and logistics (1). Before the 2014–2016 epidemic, CDC had responded to smaller Ebola outbreaks, usually in remote rural areas in Uganda, the Democratic Republic of the Congo, and other areas of Africa, without the need for an IMS activation. CDC typically deployed multidisciplinary teams of four to 10 staff, for whom CDC’s Division of Emergency Operations (DEO) provided field equipment and travel arrangements. In the field, the deployed team was primarily responsible for arranging logistics, such as lodging, transportation (air and ground), meals, and specimen shipments. In some instances, if available, the team might have received additional logistic support from CDC country offices; U.S. embassies; or international partners, such as the World Health Organization’s Global Outbreak Alert and Response Network or Médecins Sans Frontières. DEO is available 24 hours a day, 7 days a week for field staff to coordinate additional assistance. This logistic support model functioned well for most prior small-scale outbreak responses.
In the early stages of the 2014–2016 Ebola epidemic, CDC used this same model for logistic support. Small teams were deployed to Guinea, Liberia, and Sierra Leone and received limited support from the Global Outbreak Alert and Response Network and the U.S. Embassy or Consulate in-country. As the response mission in-country grew more complex and the teams grew in size, CDC needed to adapt to adequately deploy and support field teams.
By the end of July 2014, as the number of Ebola cases was rapidly increasing, CDC decided to deploy at least 50 staff members to the three countries within 30 days. To do so required a shift in how the agency thought about and managed responses to Ebola outbreaks.
New Environment, New Workforce
CDC has large numbers of experienced staff working across the globe on major public health issues every day. From the start of the Ebola response, the agency had to balance maintenance of ongoing global (and domestic) public health efforts with surge staffing requirements for the response. Maintaining this balance required training and preparing staff from throughout CDC for challenging international assignments, the first international experience for many responders. CDC faced many challenges in identifying and preparing responders for this unique response, including deployments for ≥30 days, austere living conditions, food and water safety, language barriers, harsh climate conditions, coordination with new partners, frequent rotations of staff and leadership into and out of the response, transportation issues, exposures to endemic infectious diseases, and the risk for exposure to the potentially fatal Ebola virus. Each concern factored into CDC’s emergency response in West Africa.
Initially identifying experienced staff to deploy who met travel requirements was not difficult. As the response continued, increasing in size and scope, that was no longer the case. When the CDC director initially called for “50 deployers within 30 days” in July 2014, staff were identified with predeployment preparations well under way within 2 weeks. Those persons reported to West Africa with basic responder preparedness: mission awareness, deployment location, local points of contact, and basic physical health assessment, as well as medical kits (malaria prophylaxis, antibiotics, and first aid supplies), communications equipment (laptops, cell phones, and satellite phones), and field equipment (backpacks, insect repellent, sunscreen, ponchos, flashlights, respirators, and personal protective equipment).
Responding to the Challenge
The CDC IMS is the agency’s implementation of the National Incident Management System, used governmentwide in the United States to manage emergency response operations. At CDC, standard emergency management–based general staff sections support the science-based teams and task forces, which are the mechanisms CDC uses to apply its subject-matter expertise to the public health consequences of an incident. At IMS activation, these specialized teams and task forces are scaled up at CDC headquarters in Atlanta, Georgia, to coordinate the scientific aspects of each unique response. Similarly, IMS logistics, planning, operations, finance, and other general staff sections must grow to effectively manage the day-to-day operations of the response. For instance, the IMS logistics section usually is staffed with two or three persons at the start of an activation. During the Ebola response, 23 staff members from across CDC rotated through the IMS logistics section to meet the growing needs of the response. Contractors, term-limited external hires, and staff from the Federal Emergency Management Agency further augmented the IMS logistics section, a solution likely to be considered in future large-scale responses.
Before this Ebola response, the only occasion for which had CDC deployed 50 persons simultaneously to an international location, let alone to multiple locations, was in 2000 in response to the earthquake in Haiti. Within 2 months of IMS activation for Ebola, approximately 100 staff members were in West Africa every day, and by January 2015, approximately 200 were in the field daily. During the first year of CDC’s activation, from July 2014 through June 2015, approximately 1,400 deployments had occurred to the three West African countries most heavily affected, totaling approximately 53,000 person-days of deployment time. At the time of deactivation on March 31, 2016, there had been 2,292 deployments to Guinea, Liberia, and Sierra Leone (Table); this includes the Public Health Agency of Canada (PHAC), Field Epidemiology Training Program, and others not included in the table.
Whereas CDC’s DEO normally processes approximately 300 emergency international travel requests each year, the Ebola response required processing of this many travel requests each month. In addition to the sheer quantity of deployments, CDC adapted to various travel-related challenges. For example, many airlines cancelled flights to and from Guinea, Liberia, and Sierra Leone for fear of spreading Ebola. By November 2014, only one airline had flights twice a week, which necessitated innovative approaches to travel coordination to get boots on the ground as quickly as possible. Compounding this challenge was severe winter weather in the United States and Europe, which affected departure and transit points, and labor stoppages occurred at European transit points. Because of the limited number of available and willing carriers to and from West Africa, CDC had few options for shipping supplies and equipment. To meet this need, deployed staff often hand-carried critical items in their personal luggage. To ensure the safe transfer of specimens from patients suspected or confirmed to have Ebola to CDC laboratories, CDC contracted special charter flights to transport thousands of specimens to Atlanta.
In the affected countries, deployed staff adapted to a number of logistics-related and other challenges. For example, as international partners expanded their own response operations in West Africa, CDC had to find ways to procure a sufficient quantity of increasingly scarce, safe, long-term lodging in all three highly affected countries. To ensure the effectiveness and safety of responders, CDC equipped them to work in austere conditions with communications and personal equipment, such as satellite phones, global positioning system trackers (to enhance the monitoring of location of staff for safety purposes), portable power supplies, water purifiers, “bug huts” to avoid mosquitoes and other pests, and lightweight sleeping bags. Enhanced coordination between logistics and procurement staff within the IMS became critical in ensuring rapid purchase and shipping of needed equipment and supplies.
Early in the response, agency leaders realized that CDC’s previous model for logistic support of Ebola responses had to adapt to ensure deployed staff were prepared and equipped adequately to respond. Not only was the number of staff in-country beyond the capability of the field teams to self-support but also the absence of CDC country offices in any of the three countries, volume of deployments (Figure 1), and pointed feedback from early deployed staff drove changes in how staff were prepared for deployment and supported. Logistics staff were deployed to each of the three affected countries to coordinate in-country transportation; lodging; inventory management; supply shipments; procurement requests with the IMS Logistics Section in Atlanta; and, with the United Nations, in-country flights. CDC established close partnerships with the U.S. embassies and the U.S. Agency for International Development’s Disaster Assistance Response Team to meet these new mission requirements.
Response operations must rapidly adjust in accordance with lessons learned during any response, for which Ebola has been a prime example. For IMS activations, the IMS Evaluation Team conducts in-progress and after-action reviews to evaluate lessons learned and then tracks implementation of tasks to address identified issues. Because of the size and scope of the Ebola response, beginning in August 2014, the IMS Evaluation Team and CDC’s Worklife Wellness Office implemented Real-Time Evaluation (RTE) approaches to identify health and safety risks to responders to make appropriate course corrections during the response. RTE, increasingly used in international humanitarian emergencies, is defined as “an evaluation in which the primary objective is to provide feedback in a participatory way in real time (i.e., during the evaluation field work) to those executing and managing the humanitarian response” (2,3). The RTE approach included three voluntary opportunities for responders to provide feedback: 1) a structured survey completed online or in person that solicited information about a responder’s predeployment, deployment, and postdeployment experiences, 2) individual comment submissions sent through a CDC intranet-based submission system, and 3) in-person postdeployment group debriefs. The Worklife Wellness Office also implemented a predeployment and postdeployment well-being assessment process comprising three validated instruments (4–6) with confidential follow-up as needed. This new assessment process was integrated into medical history and physical screening processes used by CDC’s Occupational Health Clinic to ensure confidentiality and ease of access by deployed staff.
As the first deployed staff reported back to CDC, they confirmed many of the challenges listed above but, more importantly, provided awareness of new and long-term preparedness needs that, when addressed, would improve the effectiveness of hundreds of future deployments. Among these new challenges were preparation for the constant concern about exposure to Ebola with every personal or surface encounter. Of more impact perhaps was preparation of CDC staff for the death from Ebola of an international colleague who shared an office (or even a computer) with those CDC staff members. One of the most unexpected challenges was preparation of staff and their families for the stigma some deployed staff encountered after returning home, such as a spouse being asked not to come to work or a child denied entry to school. Within the first month after the response began, CDC started reevaluating its preparedness efforts to address these issues and to better provide for the health, safety, security, and resiliency of its most valued resource.
Staffing issues can challenge even small-scale responses. Identifying personnel who have skill sets that match the needs of the response and the ability to handle the rigors of a complex response in austere international settings requires strong coordination between in-country team leadership, staffing recruiters, employee supervisors and emergency coordinators in home centers or programs, and the staff to be deployed. Before a person deploys, the IMS leadership needs to address several key factors: ensuring the role in the field is well defined and the staff member to be deployed has the requisite skills for the job; ensuring he or she is ready mentally and emotionally; ensuring he or she has supervisory approval to leave the “day job” for at least 30 days and often much longer and that other staff can fill the void; and last but by no means least, determining how quickly the staff member can be prepared to deploy. Although hundreds of CDC personnel have deployed domestically over the years and are considered “deployment-ready,” few were prepared (in the early activation period) for international deployments, requirements for which include appropriate medical clearance and vaccinations, security training, and possession of a U.S. government (not personal) passport. Many had never considered volunteering to deploy internationally and therefore often required several weeks to complete vaccination requirements; online and in-person security training; passport and visa processing; and of critical importance, make any necessary personal and family arrangements. To meet new and more rigorous U.S. Department of State requirements for overseas travel, approximately 637 staff completed High-Threat Security Overseas Training, and many others completed the week-long Foreign Affairs Counter-Threat Course during the first year of the response. Although these delays occasionally exacerbated staffing gaps in the Ebola response, one positive long-term outcome of preparedness is a much larger deployment-ready international responder workforce at CDC.
Ideally, international responders would deploy long enough (≥3 months) to become familiar with the local context and environment, acquire tacit knowledge and skills specific to their roles, and establish meaningful and effective relationships with partners. However, work and personal commitments within a volunteer responder workforce limited the ability to recruit persons for such long deployments, which in turn led to the need for higher than optimal numbers of persons to address identified staffing gaps for the response. Although intense staffing efforts resulted in approximately 2,844 persons participating during the first year of the response, either in the field or in the CDC IMS, critical staffing gaps required constant recruitment efforts within CDC and were met through the hiring of additional staff, acquisition of contract assistance, and use of partner agency personnel (e.g., other operating divisions of the U.S. Department of Health and Human Services, U.S. Public Health Service Commissioned Corps, Federal Emergency Management Agency, National Disaster Medical System, PHAC, and academic institutions).
In addition to logistic and staffing support for the international component of the Ebola response during this period, CDC deployed approximately 1,300 staff throughout the United States, including to five CDC quarantine stations at major airports, where enhanced entry risk assessment and management of travelers from Ebola-affected countries was conducted; approximately 63 hospitals to assess Ebola readiness; Anniston, Alabama, for CDC-conducted Ebola treatment unit training (7); and Texas, Ohio, and New York for response activities related to patients with Ebola. Although CDC adapted to the surge and unique needs of internationally deployed staff, it still needed to ensure capacity to provide logistic and resiliency support for the domestic staff.
Establishing the Deployment Risk Mitigation Unit
CDC staff deploying to West Africa during the early months of the outbreak had limited preparation for the environment and conditions they would encounter. No one working in the Ebola response was untouched by the physical and mental toll of the work itself (e.g., long hours, long deployments, changing demands) or by the mental and emotional toll of observing Ebola’s devastating impact on West Africans. In addition, deployed personnel shared concerns about being exposed to, or becoming ill with, Ebola.
By September 2014, returning responders increasingly voiced concerns about health, safety, security, and well-being. Feedback indicated that better training and preparation were required to help responders anticipate on-the-ground needs and do their jobs safely. CDC needed to be able to reassure concerned communities, families, and employers. To accomplish this, the CDC IMS activated a new team, the Deployment Risk Mitigation Unit (DRMU).
Initially a team of four (unit lead, predeployment coordinator, in-country coordinator, and postdeployment coordinator), the DRMU was tasked with supporting the health, safety, security, and well-being of CDC responders and their families throughout the deployment process. The DRMU coordinated predeployment educational activities, developed medical evacuation (medevac) procedures with the U.S. Department of State (for Ebola-related and non–Ebola-related health conditions), provided requisite health and safety supplies for in-country use by deployed staff (e.g., first aid kits, fire extinguishers, door stops to prevent unwanted entry into rooms at night), and recruited and deployed field safety officers to Guinea, Liberia, and Sierra Leone.
The DRMU collaborated with the IMS Deployment Coordination team, U.S. Department of State (for medevacs), CDC’s Occupational Health Clinic, Employee Assistance Program, National Institute for Occupational Safety and Health, IMS Logistics Support Section, and other organizations. The DRMU led, oversaw, supported, or coordinated implementation of several strategies to address concerns about health, safety, security, and well-being, including predeployment assessments, training, and preparedness; placement of safety officers in affected countries; reintegration and acceptance of returning deployed personnel and their families into workplaces, schools, and the community; and postdeployment physical and resiliency monitoring.
The DRMU helped develop, implement, and evaluate more robust and thorough predeployment briefings for staff. These briefings had always been a routine part of emergency deployments, but based on input from returning personnel deployed to the Ebola-affected countries, they were expanded to include sessions on Ebola and infectious disease prevention; cultural awareness; safety precautions in-country; personal protective equipment; mental and emotional resiliency; guidance on team organization; and coordination with partners, such as the U.S. Agency for International Development’s Office of Foreign Disaster Assistance, the lead U.S. government agency in-country. Briefings were held twice a week to share these lessons learned with personnel preparing to deploy for the first time.
Advanced planning for the medevac of deployed CDC personnel proved especially challenging because of the variety of staff possibly affected (CDC civil servants, locally employed staff, non–U.S. citizen employees, U.S. citizen nonemployee) and potential variety of circumstances (exposed, possibly exposed, febrile, or afebrile). Because of the difficulty of distinguishing Ebola from other diseases endemic to the area (e.g., malaria) (8) and because of the global panic surrounding importation of Ebola cases, routine medevac procedures were disrupted. Although U.S. citizens and legal permanent residents were assured of a medevac to the United States, non–U.S. citizens working for CDC were not.
Any U.S. citizen CDC staff member determined to have been exposed to Ebola or to be febrile was required to travel home on an aircraft arranged by the U.S. Department of State, using the Aeromedical Biologic Containment System (ABCS).* The ABCS is an isolation chamber, originally developed by CDC and others after the epidemic of severe acute respiratory syndrome in 2003 and designed to isolate persons having airborne illnesses, but capable of transporting only one person per flight (Figure 2). The ABCS was not otherwise commercially available and could be deployed only with the approval of the U.S. Department of State.
Resolving how to effect a medevac was substantially more complicated for non–U.S. citizen CDC staff. Because of immigration laws, evacuating non-U.S. citizens to the United States was highly problematic. Successfully locating medevac companies agreeable to transporting febrile persons traveling from Guinea, Liberia, or Sierra Leone to another country was a challenge. Then, many countries (even home countries) were themselves initially unwilling to accept an evacuee unless that person had completed a 21-day monitoring period elsewhere. Sorting through the myriad issues and the case-by-case nature of medevacs required substantial time and frequent coordination between CDC, the U.S. Department of State, and other U.S. and international government agencies. Ultimately, none of CDC’s deployed staff required medevac for febrile illness.
While the DRMU addressed predeployment and postdeployment health, safety, security, and well-being concerns from CDC’s Atlanta headquarters, field safety officers extended that support to teams working in-country. Field safety officers reported directly to the DRMU throughout the response, providing situational awareness on the most pressing health and safety issues. Moreover, the field safety officers worked with country leadership to address issues related to accountability (knowing the location of deployed responders, daily); encourage use of the buddy system among staff traveling outside the capitals; decrease generally risky behaviors (e.g., not wearing seat belts); and support overall well-being (e.g., serving as confidantes to deployed personnel, encouraging behaviors that enhanced resiliency).
Field safety officers also served as a conduit for information between the DRMU and the U.S. Embassy Health Units as well as the regional security officers in Guinea, Liberia, and Sierra Leone. These regular interactions with the U.S. Embassy in each country enabled field safety officers to improve working relationships between the Embassy and deployed personnel, especially crucial when services from the U.S. Embassy Health Units or regional security officers were needed. Finally, field safety officers identified on-the-ground health, safety, and well-being issues that had deleteriously affected (or had the potential to deleteriously affect) responders’ ability to conduct their work. Among many of their accomplishments: field safety officers successfully helped identify and stop an outbreak of foodborne illness among deployed personnel by inspecting the suspected kitchen source for the outbreak and by collaborating with management to implement changes to operations and food-handling practices.
The ongoing findings of the RTE, as well as postdeployment physical and resiliency monitoring and outreach, demonstrated that deployed personnel appreciated these interventions and reported improvements in their predeployment process, logistic and resiliency support throughout the deployment, and availability of resources postdeployment to reduce stress or improve well-being. As a result of these efforts, CDC responders experienced remarkably improved conditions while traveling to West Africa later in the 2014–2016 Ebola response compared with conditions experienced during the early phase of the response and those usually experienced in international deployments.
Lessons Learned
To mount a timely and effective response while ensuring the safety and well-being of deployed staff, CDC must be able to identify and prepare a cadre of staff willing and able to deploy internationally on reasonably short notice. Although some preparations, such as international visas and final medical clearance, cannot be completed until the destination is known, most actions can be completed well in advance, such as acquiring and maintaining an official U.S. government passport, completing annual medical and respirator clearance, and completing required safety and security training. Other personal preparations involve taking care of the “home front” (e.g., by providing for family members, pets, and residences).
The size and complexity of the Ebola response highlighted the need for focus on developing processes, plans, and procedures to acquire, access, use, and deploy assets, whether personnel or other resources, before an activation; doing so during a response often is not the most efficient, timely, or safe way to operate. Readiness for the next large response requires CDC to document and institutionalize a variety of procedures, such as returning retirees to the workforce, deploying non-CDC staff, providing safety and resilience training to more staff, and increasing the number of CDC staff who have skills in different languages.
Establishment of the DRMU reflected a change in how CDC views and manages deployment risks. The DRMU significantly improved the preparation of CDC staff for deployment and, equally important, assisted in staff reintegration into the agency and their families upon their return. The employment of deployed safety officers not only eased concerns of other deployed staff but also provided field team leadership with a dedicated resource to ensure staff were operating safely, despite the long hours and austere conditions.
Deployment of dedicated logistics personnel freed CDC scientific staff from the distractions of coordinating lodging, transportation, and other support needs while simultaneously facilitating coordination with embassies and consulates. Furthermore, by providing a single contact to the IMS Logistics Section in Atlanta, field team support requirements were more efficiently identified and fulfilled. Before the 2014–2016 Ebola response, CDC had few logistics staff with the background or skills to operate effectively overseas. Although not every future response will require deployment of logistics staff, the pool of available logisticians is greater now, and a program to maintain and improve their skills is being developed.
Conclusion
The 2014–2016 Ebola epidemic in West Africa required an unprecedented response from CDC. It challenged the agency’s routine operations; logistics; staffing; and responder health, safety, and resiliency programs to rapidly adjust to new geographic environments and increased, ever-changing staffing needs. CDC used new resources, innovative problem-solving, and critical partnerships to support the scientific, public health, and emergency responses of persons deployed and help the affected countries end the Ebola epidemic.
Acknowledgments
IMS Logistics team, IMS Deployment Coordination team, IMS Evaluation team, IMS Deployment Risk Mitigation Unit, CDC Occupational Health Clinic and Workforce Wellness Program, National Institute for Occupational Safety and Health, and Steve Ahrenholtz, Robert (Bob) Allin, Theresa Armstead, James Boiano, Michael Breitenstein, Kate Brett, Scott Brown, Sherrie Bruce, Jacqueline Burkholder, Charmaine Burton, Marion Carter, David Caruso, Joni Charme, Mary Choi, Lisa Clark, Pamela Clark, Gayle DeBord, Lisa Delaney, Patricia Doggett, Brent Doney, Kevin H. Dunn, Kevin L. Dunn, Adrienne Eastlake, Judi Eisenberg, Fred Frondarina, Karen Forbes, Kelli Foster, Stephanie Frink (FEMA), Renee Funk, Kevin Gallagher, John Gibbins, Johanna Gilstrap, Christine Godfrey, Thomasina Greene, Lindsey Gressard, Stephanie Griese, LaTarsha Hall, Nancy Habarta, Mark Hall, Brittani Harmon, Lauri Hicks, Ryan Hill, Steve Holland, Jennifer Hornsby-Myers, Gordon Hughes, Robert (Rob) Hutchinson (FEMA), Allen Hyde, Laura Jackson-Usher, Maria Jolly, David Kelley, David Kennedy, Richard Klomp, John Kools, Keri Lubell, David Maples, Tonya Martin, Larry Mastin, Stephen Miles, William Moore, Brian Morrison, Christopher Mozingo, Latoria Mullins, Jennifer Murphy, John Myers, Mahiyar Nasarwanji, Jeanine Neipert (FEMA), Samara Nelson, Andrea Okun, Alexandra Oster, Lauren Peel, Laura Perrone, Carol Pertowski, Xander Phoenix, Michelle Podgonik, Amanda Powell, Marilyn Radke, Ismaila Ramon, Jenny Raspberry, George Roark, Patricia Robinson, Dale A. Rose, Cecelia Sanders, Raymond Sarmiento, Melissa Seaton, Sharon Shipman, Jill Shugart, Lawrence (Gray) Smithson, Robin Soler, Erica Spies, Renee Stein, Marie Sweeney, Loren Tapp, James Tyson, Katherine Wargo, Holly G. Williams, Mac Williams, and Christine Zerbie. CDC Ebola response staff in Atlanta and in affected countries.
Corresponding author: Edward Rouse, Division of Emergency Operations, Office of Public Health Preparedness and Response, CDC. Telephone: 404-639-3902; E-mail: ERouse@cdc.gov.
1Division of Emergency Operations, Office of Public Health Preparedness and Response, CDC; 2Office of Public Health Preparedness and Response, CDC
References
- Leidel L, Groseclose S, Burney B, et al. CDC’s Emergency Management Program activities—worldwide, 2003–2012. MMWR Morb Mortal Wkly Rep 2013;62:709–13.
- Brusset E, Cosgrave J, MacDonald W. Real‐time evaluation in humanitarian emergencies. In: Ritchie LA, MacDonald W, eds. Enhancing disaster and emergency preparedness, response, and recovery through evaluation. New Directions for Evaluation 2010;126:9–20.
- Cosgrave J, Ramalingam B, Beck T. Real-time evaluations of humanitarian action: an ALNAP guide. London, UK: ALNAP; 2009. http://www.alnap.org/resource/5595
- Connor KM, Davidson JR. Development of a new resilience scale: the Connor-Davidson resilience scale (CD-RISC). Depress Anxiety 2003;18:76–82. CrossRef
- Kessler RC, Andrews G, Colpe LJ, et al. Short screening scales to monitor population prevalences and trends in non-specific psychological distress. Psychol Med 2002;32:959–76. CrossRef
- Prins A, Ouimette P, Kimerling R, et al. The primary care PTSD screen (PC-PTSD): development and operating characteristics. Prim Care Psychiatry 2004;9:9–14. CrossRef
- CDC. Preparing healthcare workers to work in Ebola treatment units (ETUs) in Africa. Atlanta, GA: US Department of Health and Human Services, CDC; 2015. http://www.cdc.gov/vhf/ebola/hcp/safety-training-course
- CDC. Recommendations for managing and preventing cases of malaria in areas with Ebola. Atlanta, GA: US Department of Health and Human Services, CDC; 2015. http://www.cdc.gov/vhf/ebola/outbreaks/malaria-cases.html
* Names of specific vendors, manufacturers, or products are included for public health and informational purposes; inclusion does not imply endorsement of the vendors, manufacturers, or products by CDC or the U.S. Department of Health and Human Services.
 TABLE. Number of CDC-supported international deployments and number of days deployed, by country or region — July 1, 2014–March 31, 2016*
TABLE. Number of CDC-supported international deployments and number of days deployed, by country or region — July 1, 2014–March 31, 2016*
| Country/Region | No. deployments† | No. days deployed | |||
|---|---|---|---|---|---|
| Mean | Maximum | Minimum | Total no. person-days deployed†,§ | ||
| Sierra Leone | 1,099 | 36 | 276 | 2 | 39,791 |
| Liberia | 619 | 32 | 135 | 2 | 20,112 |
| Guinea | 442 | 36 | 131 | 2 | 15,872 |
| All other Africa deployments¶ | 222 | 19 | 62 | 1 | 4,190 |
| All other international deployments** | 79 | 7 | 49 | 2 | 592 |
| Total | 2,461 | 33 | 276 | 1 | 80,557 |
* Deployment dates on or after July 1, 2014, and return dates on or before March 31, 2016, entered into Preparedness Workforce Management System as of April 24, 2016, 1 pm Eastern daylight time. Deployments include staff from other agencies and partners supported through the CDC Emergency Operations Center (i.e., U.S. Department of Health and Human Services, 43 deployments; Council of State and Territorial Epidemiologists, 35 deployments; and other partners) but do not include some deployments of Public Health Agency of Canada (PHAC), Field Epidemiology Training Program (FETP), and other staff not processed by the CDC Emergency Operations Center. At the time of deactivation on March 31, 2016, there had been 2,292 total deployments to Guinea, Liberia, and Sierra Leone (this includes the PHAC, FETP, and others not included in the table).
† One person can be deployed multiple times.
§ Number of days CDC-supported responders were deployed using deployment start date and end date. Numbers might differ slightly from those provided in previous reports.
¶ Benin, Burkina Faso, Cameroon, Côte d’Ivoire, Democratic Republic of the Congo, Egypt, Equatorial Guinea, Ethiopia, Ghana, Guinea-Bissau, Mali, Mauritania, Niger, Nigeria, People’s Republic of the Congo, Senegal, The Gambia, and Togo.
** Belgium, Canada, France, Germany, Italy, Luxembourg, Singapore, Switzerland, and United Kingdom.
 FIGURE 1. Approximate number of staff deployed internationally who were managed by the CDC Emergency Operations Center, by week — July 2014–June 2015
FIGURE 1. Approximate number of staff deployed internationally who were managed by the CDC Emergency Operations Center, by week — July 2014–June 2015
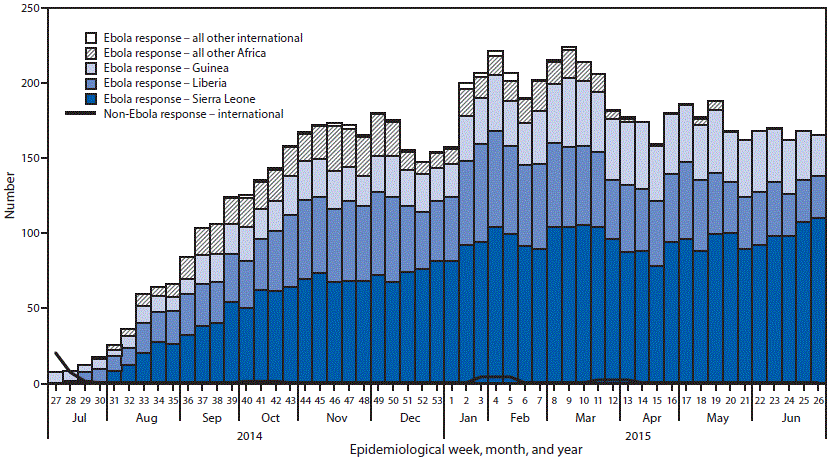
Abbreviations: Ebola = Ebola virus disease; EOC = Emergency Operations Center.
 FIGURE 2. The Aeromedical Biologic Containment System installed in a Gulfstream III aircraft*
FIGURE 2. The Aeromedical Biologic Containment System installed in a Gulfstream III aircraft*

*Names of specific vendors, manufacturers, or products are included for public health and informational purposes; inclusion does not imply endorsement of the vendors, manufacturers, or products by CDC or the U.S. Department of Health and Human Services.
Suggested citation for this article: Rouse EN, Zarecki SM, Flowers D, et al. Safe and Effective Deployment of Personnel to Support the Ebola Response — West Africa. MMWR Suppl 2016;65(Suppl-3):90–97. DOI: http://dx.doi.org/10.15585/mmwr.su6503a13.
MMWR and Morbidity and Mortality Weekly Report are service marks of the U.S. Department of Health and Human Services.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All HTML versions of MMWR articles are generated from final proofs through an automated process. This conversion might result in character translation or format errors in the HTML version. Users are referred to the electronic PDF version (https://www.cdc.gov/mmwr) and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.