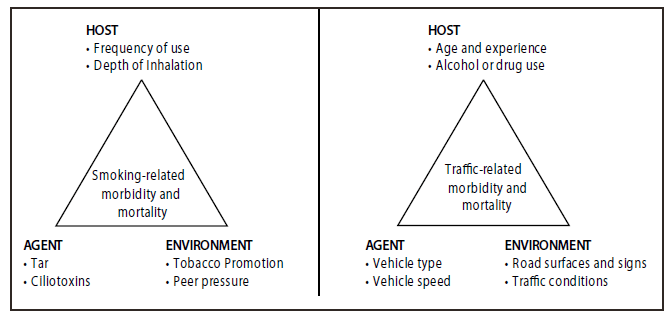
FIGURE 1. Parallels in the epidemiologic triad related to smoking harm and traffic injury
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail.
Injury Prevention, Violence Prevention, and Trauma Care: Building the Scientific Base
Corresponding author: David A. Sleet, PhD, Division of Unintentional Injury Prevention, National Center for Injury Prevention and Control, CDC, 4770 Buford Highway, MS F62, Atlanta, GA 30341; Telephone: 770-488-4699; Fax: 770-488-1317; E-mail: dds6@cdc.gov.
Introduction
Injuries and violence are widespread in society. Unintentional injuries and injuries caused by acts of violence are among the top 10 killers of U.S. residents of all ages. Injuries are the leading cause of death of persons aged 1--44 years and a leading cause of disability among persons of all ages, regardless of sex, race/ethnicity, or socioeconomic status. Nearly 180,000 persons die each year from unintentional injuries or from acts of violence, and one in 10 sustains a nonfatal injury serious enough to require treatment in a hospital emergency department (1). In addition, injuries and violence have a major effect on the well-being of Americans by contributing to premature death, disability, poor mental and physical health, chronic disease, and other health conditions, as well as high medical costs and lost productivity.
The science of injury prevention and control encompasses activities from primary prevention through treatment and rehabilitation. Since 1961, when MMWR was first published by CDC, progress has been made in developing the science of injury prevention and control, creating surveillance systems to capture injury mechanisms and intent, and establishing a scientific framework to address injury prevention and treatment.
Perspectives on Unintentional Injuries and Public Health
Many consider the first 50 years of the 20th century as the prescientific era of injury control because of the prevalent perception at the time that injuries resulted from inevitable, random, or unavoidable events, termed accidents. Many public health officials believed that injury prevention was outside the realm of scientific inquiry because it could not be predicted or controlled. Epidemiologic data were difficult to obtain, and patterns in injuries had not been systematically reviewed.
History of Injury before 1961
The National Safety Council was founded in 1913 as a clearinghouse for safety data and information, which previously had been lacking. Injury or accident prevention progressed largely by trial and error. In 1923, Julian Harvey introduced the three Es (education, engineering, and enforcement) to control the causes of accidents (2). However, an epidemiologic framework for the ways these approaches work to reduce injuries was not available for another 40 years.
The scientific approach to injuries developed during 1940--1950 laid the groundwork for a public health understanding and response (3). Hugh De Haven studied cases in which persons fell 50--150 feet without sustaining serious injury. He observed that the type of force and its distribution across the body contributed to injury (4). This discovery later allowed for engineering designs that prevented or modified energy exchange, such as seat belts, dashboard padding, automobile crush zones, and bicycle helmets.
In 1949, John E. Gordon suggested that injuries, like classic diseases, were characterized by epidemic episodes, seasonal variation, long-term trends, and demographic distribution (5). He further explained how injury, like disease, was the product of at least three sources: the host, the agent, and the environment.
Ten years later, in 1959, James Gibson, an experimental psychologist who applied traditional epidemiologic methods to the study of injuries, concluded that injuries to a living organism can be produced only by some form of energy exchange (6). This energy (the agent of injury) may be kinetic, chemical, thermal, radiatory, or electrical and, when released, can cause tissue damage or functional impairment. In an automobile crash, for example, the agent of injury is kinetic energy released on the host in amounts beyond human tolerance. This discovery helped clarify the energy transfer theory of injury causation as the missing component in understanding the epidemiology of traffic injuries (Figure 1). The next step would be to design interventions to break the causal chain.
Key Developments in Unintentional Injury Prevention since 1961
The 1960s brought new attention to injury prevention research and new scientific approaches. One of the most noteworthy advances came in the work of William Haddon, Jr., an engineer, public health physician, and director of the New York State Department of Health, who is often considered the father of modern injury epidemiology. Haddon's suggestion (7) that injury prevention depended on controlling the agent---energy---led him to develop strategies later applied to preventing motor vehicle--related injuries (8). In 1966, Haddon became the first Administrator of the U.S. government's National Highway Safety Bureau (renamed the National Highway Traffic Safety Administration [NHTSA] in 1970).
Haddon Matrix
Haddon developed a two-dimensional phase-factor matrix (The Haddon Matrix) to help conceptualize an injury event (9). The first dimension comprised the three factors influencing injury: host, agent (or vector), and environment; the second dimension was injury phase divided into preevent, event, and postevent. The Haddon Matrix can be applied readily to a motor vehicle crash (Table).
This framework for analysis makes possible identification of factors related to the host, agent, and environment within the three phases before, during, and after the crash that might be explanatory and contribute to injury prevention strategies. A guiding principle of injury control that emerged from Haddon's work was that effective injury control relied on a combination of intervention strategies. Estimates suggest that federal motor vehicle safety standards resulting from application of Haddon's energy exchange management approach saved an estimated 328,551 lives during 1960--2002 (10).
Federal Leadership
Adding to the impetus for a more disciplined approach to injury control was the 1966 National Research Council's landmark report, Accidental Death and Disability: The Neglected Disease of Modern Society (11). This report documented how little scientific progress had been made in understanding injury causation or in applying what was already known to reduce injuries and improve trauma outcomes.
Early federal programs in the 1960s and 1970s were centered in the Division of Accident Prevention within the U.S. Public Health Service. At the same time, traffic safety and consumer safety were being addressed by NHTSA and the Consumer Product Safety Commission, respectively. The Highway Safety Act of 1966 and the Consumer Product Safety Act of 1972 ushered in new regulatory authority and launched an era of engineering and product regulation as bedrocks of modern injury control (12).
CDC
In the early 1970s, CDC began to investigate injuries, particularly in the home and recreational environment. However, not until the Institute of Medicine's landmark publication, Injury in America (13), did CDC's role in injury prevention become firmly established. That report recommended the establishment of a Center for Injury Control within CDC and in 1986, Congress responded by appropriating $10 million to initiate a 3-year pilot program for the study of injury control at CDC.
The Injury Prevention Act of 1986 amended the Public Health Service Act, officially placing the injury control program at CDC. Subsequently, the Injury Control Act of 1990 (Public Law 101-558) reauthorized CDC's injury funding, and the National Center for Injury Prevention and Control was inaugurated in 1992 as the lead federal agency for nonoccupational injury prevention and control.
Through this locus in public health, the National Center for Injury Prevention and Control has developed a strong scientific base through intramural research and an extramural investigator-initiated grant program and has put prevention to work by supporting state and community injury control programs. Under CDC leadership, the field has grown, research has flourished, and effective programs have been identified and delivered to communities. Injury rates have fallen substantially in the United States since 1961; however, although effective strategies to prevent unintentional injuries are now widely recognized (14), they remain inadequately adopted.
Perspectives on Violence and Public Health
Thirty years ago, the words "violence" and "health" were rarely used in the same sentence. Today, violence is recognized as a major public health problem. Violence is defined as the intentional use of physical force or power, threatened or actual, against oneself, another person, or a group or community that either results in, or has a high likelihood of resulting in, injury, death, psychological harm, maldevelopment, or deprivation (15). This definition encompasses three broad types of violence: interpersonal violence (e.g., intimate partner violence, sexual violence, child maltreatment, elder maltreatment, and youth violence), self-directed violence (e.g., suicidal behavior), and collective violence (e.g., war, armed conflict, terrorism, and state-sponsored violence).
Several trends contributed to increased recognition and acceptance that violence could be addressed from a public health perspective:
- Homicide and suicide rose in the rankings of causes of death as the United States became more successful in preventing and treating infectious diseases. Since 1965, homicide and suicide have consistently been among the 15 leading causes of death in the United States (16,17).
- The risk for homicide and suicide reached epidemic proportions during the 1980s. Suicide rates among persons aged 15--24 years almost tripled during 1950--1990 (18). Similarly, during 1985--1991, homicide rates among 15- to 19-year-old males increased 154% (19). This increase was particularly acute among young African-American males.
- The importance of behavioral factors was recognized in the etiology and prevention of disease. Successes in applying behavioral strategies to changing other health risks encouraged public health professionals to apply these strategies to prevent interpersonal violence and suicidal behavior (20).
- Child maltreatment and intimate partner violence were recognized as social problems in the 1960s and 1970s, demonstrating the need to move beyond sole reliance on the criminal justice sector in solving these problems (20).
Public Health Call for Action
Several landmark reports highlighted the public health significance of violence. In 1979, the Surgeon General's report, Healthy People, identified 15 priority areas in which, with appropriate action, further gains could be expected during the next decade (21). Among the priorities was the control of stress and violent behavior. The goals for violence prevention established in this report were translated into measurable objectives in Promoting Health/Preventing Disease: Objectives for the Nation (22). These objectives called for substantial reductions by 1990 in the number of child-abuse injuries and deaths, reduction in the rates of homicide and suicide among persons 15--24 years of age, and improvements in the reliability of data on child abuse and family violence. In 1985, the Report of the Secretary's Task Force on Black and Minority Health identified homicide as a major cause of the disparity in death rate and illness by African Americans and other minorities relative to non-Hispanic whites (23). These themes were carried forward in subsequent versions of Healthy People 1990 and 2010 and, now, 2020.
Response to Healthy People Initiatives
The emergence of violence as a legitimate issue on the national health agenda spurred a variety of responses from the public health sector during the 1980s. In 1983, CDC established the Violence Epidemiology Branch, which was integrated into the Division of Injury Epidemiology and Control (DIEC) 3 years later. The creation of DIEC resulted directly from the Institute of Medicine report (13).
In 1985, the Surgeon General convened a workshop on violence and public health (24). This workshop marked the first time that the Surgeon General encouraged all health professionals to respond to the problem. One recommendation from the workshop was an explicit call to include education about domestic violence in the curricula of medical schools and other relevant professional schools across the nation. Findings from the first survey to determine the prevalence of medical school instruction on domestic and other forms of family violence were summarized in MMWR in 1989 (25). In the same year, the Report of the Secretary's Task Force on Youth Suicide provided a comprehensive synthesis of the state of knowledge about youth suicide and recommended a course of action for stemming the substantial increases that had occurred during the previous 3 decades (18).
Applying the Tools of Epidemiology in Violence Prevention
During the same period, CDC undertook a number of epidemiologic investigations of a series of child murders in Atlanta and suicide clusters in Texas and New Jersey (26--28). These investigations helped to demonstrate that epidemiologic research methods could be successfully applied to incidents of violence. The suicide investigations also informed the first recommendations for preventing and containing suicide clusters issued by CDC and subsequent media guidelines for reporting on suicide (27,29).
Beginning in the early 1990s, the public health approach to violence shifted from describing the problem to understanding what worked in preventing it and increasingly began drawing on methods from the social and behavioral sciences (Box). CDC evaluation studies in the 1990s were among the first randomized controlled trials to specifically assess the effect of prevention programs on violence-related behaviors and injury outcomes among youth. These studies helped demonstrate that substantial reductions in aggressive and violent behavior were possible with applied, skill-based violence-prevention programs that address social, emotional, and behavioral competencies, as well as family and community environments. The achievements in the prevention of youth violence throughout the 1980s and 1990s were published in Youth Violence: A Report of the Surgeon General (30). The report also highlighted the cost-effectiveness of prevention over incarceration and set forth a vision for the 21st century.
The early successes in youth violence prevention paved the way for a public health approach to other violence problems, such as intimate partner violence, sexual violence, and child maltreatment. In 1994, CDC and the National Institute of Justice began collaborating on the first national violence-against-women survey, which produced the first national data on the incidence, prevalence, and economic costs of intimate partner violence, sexual violence, and stalking (31). In 1994, Congress also passed the Violence Against Women Act---landmark legislation that established rape prevention and education programs across the nation and called for local demonstration projects to coordinate the intervention and prevention of domestic violence. These programs were instrumental in building local- and state-level infrastructure and capacity for preventing intimate partner violence and sexual violence (Box).
Global Focus
As public health efforts to understand and prevent violence gained momentum in the United States, they garnered attention abroad. Violence was placed on the international agenda in 1996 when the World Health Assembly adopted Resolution WHA49.25, which declared violence "a leading worldwide public health problem." The resolution requested that the World Health Organization (WHO) initiate public health activities to document and respond to the problem. In 2000, WHO created the Department of Injuries and Violence Prevention to increase the global visibility of unintentional injury and violence and to facilitate public health action. A framework for approaching violence as a public health problem was presented in the 2002 World Report on Violence and Health (15)---the first comprehensive examination of violence as a preventable global public health problem---and has been elucidated and expanded in subsequent reports, including the United Nations Secretary-General's World Report on Violence Against Children (32).
Perspectives on Trauma-Related Public Health
Care of the traumatically injured patient, with the explicit goal of reducing injury-related disability and death, is a clearly recognized public health priority. Access to health services, such as systems created for injury-related care, ranging from prehospital and acute care to rehabilitation, is among the most important strategies to reduce the consequences of injuries when prevention fails.
State of Trauma Care Before 1961
Until 1961, major clinical advancements in the care of acutely injured patients had resulted primarily from novel medical and scientific advancements. Wilhelm Rontgen and Alexander Fleming's discoveries of x-rays and penicillin, respectively, introduced into clinical practice radiography in injury diagnosis and antibiotics in the treatment of wound infections (33,34). Hemorrhagic shock experiments by Carl Wiggers led to acceptance of intravenous fluid resuscitation of the acutely injured patient (35). Although certain clinical management principles were recognized, nationally accepted guidelines addressing care for the injured patient were lacking, resulting in an absence of standardized practices or a systematic approach to improve survival. Since 1961, acute injury care in the United States has rapidly evolved, resulting in decreased disability and death. This success can be attributed, not to a single advancement in technology, but rather to a comprehensive, systems-based public health approach incorporating federal, state, and local governments and nongovernment stakeholders.
Key Developments in Trauma-Related Injury Since 1961
Development of Trauma Centers and Standardized Care
A major milestone in trauma-related public health was establishment of the first two U.S. trauma centers in 1966---one in San Francisco and the other in Chicago (36). These centers were developed to address increasing urban violence and marked recognition of the importance of systematic care for injured patients (36). This concept was furthered by R Adams Cowley, a U.S. Army trauma surgeon who established a Clinical Shock Trauma Research Unit in 1961 (37). In 1969, this unit developed into the Shock Trauma Center, the nation's first comprehensive health-care facility dedicated to trauma care. The Shock Trauma Center later became an autonomous clinical and research trauma institute. Cowley and colleagues subsequently developed a patient transportation and field communication system that became the first integrated, statewide trauma-response and emergency medical services (EMS) system in the United States (37).
Another milestone followed a plane crash in 1976, where orthopedic surgeon James Styner and his children were evacuated to a rural Nebraska hospital where they were treated by emergency department staff without specialized trauma training (38). Styner and his colleagues, motivated by the desire to standardize trauma care, produced the nation's first course in Advanced Trauma Life Support (ATLS), held in Nebraska in 1978 (38). Two years later, the American College of Surgeons (ACS) Committee on Trauma (COT) adopted ATLS and began national and international dissemination (38). After establishment of the nation's first two trauma centers and widespread ATLS adoption, ACS and several state and local agencies initiated a trauma center verification process for validating appropriate resources for optimal trauma care. In 1994, ACS-COT piloted a consultation process facilitating regional trauma system development. These consultations, modeled on a comprehensive public health approach, were highly effective in facilitating trauma system development, primarily in areas related to planning and system design (39).
The Effect of Military and Federal, State, and Local Government Involvement
The combat experiences of the U.S. military have played a substantial role in the development of trauma systems. The use of organized field medics during the Vietnam War served as a precursor for paramedics in civilian areas (40). Air medical transport of injured patients, first developed during World War I, became routine during the Korean and Vietnam wars (40). Lessons from routine air medical transport of soldiers in Vietnam fueled the rapid increase of civilian air transport of trauma patients in the United States during the 1980s (41). The conflicts in Iraq and Afghanistan led to further advances in military trauma care, which offer great promise for use in civilian settings. These include management of traumatic brain injury, use of hemostatic dressings and tourniquets, phased surgical approaches for complex injuries, and new approaches to resuscitation (42).
Legislation has been critical to the advancement of trauma care--related public health since 1961. The 1966 Federal Highway Safety Act mandated uniform guidelines improving EMS related to highway crashes (43). In 1973, the landmark Emergency Medical Services Systems Act established a program providing resources to state and local governments for implementing comprehensive EMS systems.
EMS providers and their medical directors use field triage decision schemes to assist with expeditious and appropriate transport decisions to regional trauma centers. These are a combination of physiologic, anatomic, and mechanistic criteria intended to identify patients with, or at risk for, a severe injury. The first ACS-COT decision scheme was published in 1986 and revised three times (44). In 2005, CDC and its partners established the National Expert Panel on Field Triage to guide the 2006 revision of the field triage scheme. The 2006 Field Triage Decision Scheme, published by ACS-COT, was endorsed by 17 national organizations. CDC subsequently published these guidelines in MMWR in 2009 (44). Other federal agencies, including the Health Resources and Services Administration (HRSA) and NHTSA, have played a substantial role in developing public health interventions for trauma care. Trauma care and EMS resources directed at children were outlined in the 1984 HRSA Emergency Medical Services for Children Program (43). Additionally, in 1992, HRSA released the draft Model Trauma Care System Plan as a template for states in designing comprehensive trauma care delivery (43). In 1989, NHTSA developed a program to assist in coordinating state- and regional-level trauma-care resources.
The Need for Standardized Data Collection and Registries
Responding to the need for establishing a data coding, collection, and analysis system to guide clinical and public health practice, in 1967 the International Classification of Diseases (ICD) employed three- or four-digit codes to specify injury (45). Although potentially useful in recognizing injury incidence, ICD codes were not reliable for comparing injuries or describing severity. Recognizing the need for a comprehensive coding system to capture type, location, and severity of injury, a joint Committee on Injury Scaling, comprising members from the Society of Automotive Engineers, the American Association for Automotive Medicine, and the American Medical Association, published the General Motors Collision Performance and Injury Report in 1971 (45). This report described the Abbreviated Injury Severity (AIS) scale, which was the first widely adopted anatomical scoring system describing the threat to life associated with an injury (45). In 1974, the AIS scoring system was incorporated into the Injury Severity Score (ISS) to predict comprehensive injury mortality (46). In 1997, CDC guidelines on external mechanisms of injury were integrated and standardized with AIS to improve data quality, recording, and reporting (47). Both AIS and ISS marked a key step in the public health approach to trauma that allowed for public health practitioners to systematically approach and evaluate trauma prevention interventions, and outcomes.
Trauma registries have been important for the care performance improvement process. These registries serve as repositories for data that can be evaluated, associated with outcomes, and used for quality control (48). In 1969, the first computerized trauma registry in the United States began in Chicago at Cook County Hospital. This system later evolved into the Illinois Trauma Registry and aggregated data from all trauma centers in the state. A milestone in the development of U.S. trauma registries came in 1989 with establishment of the National Trauma Data Bank (NTDB) by ACS (48). Since its inception, the National Trauma Data Bank has grown into the largest trauma data registry assembled with a large sample of trauma centers from across the nation.
The Next 50 Years in Injury Prevention, Violence Prevention, and Trauma Care
Substantial progress has been made since 1961 in recognizing unintentional injury and violence; developing trauma-care systems; developing a scientific base for the field; and discovering successful prevention measures. The tremendous growth in the field can be measured by number of publications by decade from <25 during 1940-1949 to approximately 750 during 2000--2005 (Figure 2). By end of 2011, the number of publications may well exceed 3,000. MMWR has been a critical partner in these efforts by providing a credible vehicle to share this scientific knowledge and its implications for practice with the media and the profession (49,50).
In the global arena, the World Report on Violence and Health (15), and the World Report on Road Traffic Injury Prevention (51) are now used throughout the world as platforms for prevention. The Guidelines For Field Triage of Injured Patients (44) has become a widely adopted national tool and is increasingly being implemented in other parts of the world.
As the 21st century unfolds, public health is increasing its emphasis on the dissemination and implementation of effective injury and violence prevention programs and policies and tackling problems such as child maltreatment, youth violence, sexual violence, elder maltreatment, prescription drug overdose, alcohol-impaired and distracted driving, and falls among the elderly. Expanded use of treatment guidelines and effective trauma-care coverage will need to expand into rural and underserved areas and globally to enhance trauma-care systems in low- and middle-income countries (52).
One of the greatest challenges in the next 50 years will be to further change public attitudes and behaviors about the preventability of violence and unintentional injuries, just as public health has changed public attitudes to prevent tobacco use, sedentary lifestyle, and sexual risk-taking behavior. Unintentional injuries can no longer be considered "accidents." Violence can no longer be viewed as just a problem for the police or criminal justice sector. Evidence-based strategies uncovered in the last 50 years need to be disseminated and widely adopted in the next half century, and new strategies must be discovered to stem the tide of escalating injuries caused by prescription drug overdose, motorcycle crashes, falls by older adults, and the increasing popularity of motor-vehicle travel in low- and middle-income countries that lack appropriate safety systems.
Because most injuries are now considered preventable, the challenges lie in identifying those injury and violence winnable battles and in developing effective policies and delivering effective programs that can save many more lives. Achievements in injury and violence prevention and trauma care during the past 50 years have involved difficult professional and political struggles, and these struggles will continue during the next half century. The need for credible science, strong leadership, and strong partnerships will be more important than ever.
References
- National Center for Injury Prevention and Control, CDC. Web-based Injury Statistics Query and Reporting System (WISQARS). Available at www.cdc.gov/ncipc/wisqars.
- Nichols J. Driver education and improvement programs [Chapter 3]. In: Heimstra NW, ed. Injury control in traffic safety. Springfield, IL: Charles C. Thomas; 1970:49.
- National Committee for Injury Prevention and Control. Injury prevention: meeting the challenge. New York, NY: Oxford University Press; 1989.
- De Haven H. Mechanical analysis of survival in falls from heights of fifty to one hundred and fifty feet. War Med 1942;2:586--96.
- Gordon JE. The epidemiology of accidents. Am J Public Health 1949;39:504--15.
- Gibson JJ. The contribution of experimental psychology to the formulation of the problem of safety: a brief for basic research. In: Behavioral approaches to accident research. New York, NY: Association for the Aid of Crippled Children; 1961:77--89.
- Haddon W Jr. A note concerning accident theory and research with special reference to motor vehicle accidents. Ann N Y Acad Sci 1963;107: 635--46.
- Haddon W, Goddard J. An analysis of highway safety strategies. In: Passenger car design and highway safety. New York, NY: Association for the Aid of Crippled Children and Consumers Union of New York; 1962;6--11.
- Haddon W. A logical framework for categorizing highway safety phenomena and activity, J Trauma 1972;12:193--207.
- Kahane CJ. Lives saved by the federal motor vehicle safety standards and other vehicle safety technologies, 1960--2002. Passenger cars and light trucks. With a review of 19 FMVSS and their effectiveness in reducing fatalities, injuries and crashes. Washington, DC: US Department of Transportation, National Highway Traffic Safety Administration; 2004. NHTSA technical report no. DOT HS 809 833. Available at http://www.nhtsa.gov/cars/rules/regrev/evaluate/809833.html.
- National Research Council. Accidental death and disability: the neglected disease of modern society. Washington, DC: National Academy of Sciences; 1966.
- Fisher L. Childhood injuries---causes, preventive theories and case studies. J Environ Health 1988;50:355--60.
- Institute of Medicine. Injury in America: a continuing public health problem. Washington, DC: National Research Council; 1985.
- Doll L, Bonzo S, Mercy JA, Sleet DA, eds. Handbook of injury and violence prevention. New York, NY: Springer; 2007.
- Krug EG, Dahlberg LL, Mercy JA, Zwi AB, Lozano R, eds. World report on violence and health. Geneva, Switzerland: World Health Organization; 2002.
- CDC. Leading Causes of Death, 1900-1998 [online]. Retrieved July 27, 2008. Available from URL: http://www.cdc.gov/nchs/data/dvs/lead1900_98.pdf.
- CDC. Web-based Injury Statistics Query and Reporting System (WISQARS) [online]. Retrieved July 27, 2011. Available from URL: www.cdc.gov/ncipc/wisqars
- Alcohol, Drug Abuse, and Mental Health Administration. Report of the Secretary's Task Force on Youth Suicide. Vol. 1. Rockville, MD: US Department of Health and Human Services, Alcohol, Drug Abuse, and Mental Health Administration; 1989.
- CDC. Homicides among 15--19-year-old males---United States, 1963--1991. MMWR 1994; 43:725--7.
- Dahlberg LL, Mercy JA. History of violence as a public health problem. American Medical Association's Virtual Mentor February 2009; Vol 11(2):167-172.
- US Department of Health, Education, and Welfare. Healthy people: The Surgeon General's report on health promotion and disease prevention. Rockville, MD: US Department of Health, Education, and Welfare; 1979.
- US Department of Health and Human Services. Promoting health/preventing disease; objectives for the nation. Rockville, MD: US Department of Health and Human Services; 1980.
- US Department of Health and Human Services. Report of the Secretary's Task Force on Black and Minority Health. Rockville, MD: US Department of Health and Human Services; 1985.
- US Department of Health and Human Services. US Department of Justice. Surgeon General's Workshop on Violence and Public Health report. Washington, DC: Health Resources and Service Administration; 1986.
- CDC. Education about adult domestic violence in U.S. and Canadian medical schools, 1987--88. MMWR 1989;38:17--9.
- Blaser MJ, Jason JM, Weniger BG, et al. Epidemiologic analysis of a cluster of homicides of children in Atlanta. JAMA 1984;251:3255--8.
- CDC. CDC recommendations for a community plan for the prevention and containment of suicide clusters. MMWR 1988;37(No. SS-6).
- Davidson LE, Rosenberg ML, Mercy JA, Franklin J, Simmons JT. An epidemiologic study of risk factors in two teen suicide clusters. JAMA 1989;262:2687--92.
- CDC. Suicide contagion and the reporting of suicide: recommendations from a national workshop. MMWR 1994;43(No. RR-6).
- US Department of Health and Human Services. Youth violence: a report of the Surgeon General. Rockville, MD: US Department of Health and Human Services, CDC, Substance Abuse and Mental Health Services Administration, National Institutes of Health for the National Institute of Mental Health; 2001.
- Tjaden P, Thoennes N. Full report of the prevalence, incidence, and consequences of violence against women: findings from the National Violence Against Women Survey. Washington, DC: National Institute of Justice, Office of Justice Programs, US Department of Justice; US Department of Health and Human Services, CDC; 2000.
- Pinheiro PS. World report on violence against children. Geneva, Switzerland: United Nations; 2006.
- Waksman SA. Contribution of a simple bacteriologist to humanity. Science 1955;121:580--1.
- Toledo-Pereyra LH. X-rays surgical revolution. J Invest Surg 2009;22:327--32.
- Manji RA, Wood KE, Kumar A. The history and evolution of circulatory shock. Crit Care Clin 2009;25:1--29, vii.
- Trunkey DD. The emerging crisis in trauma care: a history and definition of the problem. Clin Neurosurg 2007;54:200--5.
- Edlich RF. Three giant steps toward the development of a modern emergency medical service system. J Emerg Med 1991;9:61--6.
- Styner JK. The birth of advanced trauma life support. J Trauma Nurs 2006;13:41--4.
- Winchell RJ, Ball JW, Cooper GF, et al. An assessment of the effect of trauma systems consultation on the level of trauma system development. J Am Coll Surg 2008;207:623--9.
- Stephenson JC. Echelons of care and aeromedical evacuation from the Middle East area of operations. ADF Health 2008;9:9--14.
- Meier DR, Samper ER. Evolution of civil aeromedical helicopter aviation. South Med J 1989;82:885--91.
- Bell RS, Mossop CM, Dirks MS, et al. Early decompressive craniectomy for severe penetrating and closed head injury during wartime. Neurosurg Focus 2010;28:E1.
- Cooper G, Laskowski-Jones L. Development of trauma care systems. Prehosp Emerg Care 2006;10:328--31.
- CDC. Guidelines for field triage of injured patients. Recommendations of the National Expert Panel on Field Triage. MMWR 2009;58(No. RR-1).
- Petrucelli E, States JD, Hames LN. The abbreviated injury scale: evolution, usage, and future adaptability. Accid Anal Prev 1981;13:29--35.
- Baker SP, O'Neill B, Haddon W, et al. The injury severity score: a method for describing patients with multiple injuries and evaluating emergency care. J Trauma 1974;14:187--96.
- CDC. Recommended framework for presenting injury mortality data. MMWR 1997;46(No. RR-14).
- Nwomeh BC, Lowell W, Kable R, et al. History and development of trauma registry: lessons from developed to developing countries. World J Emerg Surg 2006;1:32.
- CDC. Prevention of motor vehicle--related injuries: a compendium of articles from the Morbidity and Mortality Weekly Report---1985--1996. Atlanta, GA: CDC, National Center for Injury Prevention and Control; 1997.
- CDC. Home and leisure injuries in the United States: a compendium of articles from the Morbidity and Mortality Weekly Report---1985--1995. Atlanta, GA: National Center for Injury Prevention and Control, CDC; 1996.
- Peden M, Scurfield R, Sleet DA, et al, eds. World report on road traffic injury prevention. Geneva, Switzerland: World Health Organization; 2004.
- World Health Organization. Strengthening care for the injured: success stories and lessons learned from around the world. Geneva, Switzerland, World Health Organization; 2010. Available at http://whqlibdoc.who.int/publications/2010/9789241563963_eng.pdf.
Source: Sleet DA, Gielen A. Injury prevention. In: Health promotion handbook. Arnold J, Gorin SS, eds. St. Louis, MO: Mosby; 1998.
Alternate Text: The figure is a graphic that presents parallels in the epidemiologic triad between smoking harm and traffic injury.
|
Type |
Host |
Agent |
Environment |
|---|---|---|---|
|
Preevent |
Alcohol use |
Brake condition |
Road curvature |
|
Fatigue |
Load weight |
Weather |
|
|
Driving experience |
Vehicle visibility |
Speed limit |
|
|
Defensive driving skill |
|||
|
Event |
Seat belt use |
Speed at impact |
Guard rails |
|
Bone density |
Vehicle size |
Median barriers |
|
|
Stature |
Vehicle safety features |
Recovery zones |
|
|
Postevent |
Age |
Fuel tank integrity |
911 access |
|
Sex |
Triage protocols |
||
|
Frailty |
Emergency medical services training |
||

Source: Pless IB. A brief history of injury and accident prevention publications. Inj Prev 2006;12:65--6. Reprinted with permission from BMJ Publishing Group Ltd.
Alternate Text: The figure is a bar graph that presents the number of publications in the field of injury prevention during 1940-2005.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All MMWR HTML versions of articles are electronic conversions from typeset documents.
This conversion might result in character translation or format errors in the HTML version.
Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr)
and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S.
Government Printing Office (GPO), Washington, DC 20402-9371;
telephone: (202) 512-1800. Contact GPO for current prices.
**Questions or messages regarding errors in formatting should be addressed to
mmwrq@cdc.gov.


