At a glance
CDC recommends testing blood for lead exposure. A patient’s blood lead level (BLL) is measured in micrograms of lead per deciliter of blood (μg/dL). Healthcare providers should follow recommendations based on initial screening capillary and confirmed venous BLLs. Learn more about the recommended actions after a blood lead level test.

Testing
Two types of blood collection tests may be used:
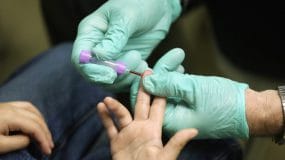
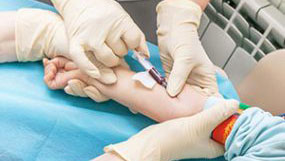
Initial screening blood lead level
Healthcare providers may use a capillary or venous sample for initial BLL screening. If capillary results are equal to or greater than CDC's Blood Lead Reference Value (BLRV), providers should collect a venous sample. If a venous sample was taken during the initial screening test, skip to Confirmed Venous Blood Lead Level.
If the patient's BLL is ≥ 3.5 micrograms per deciliter
- Provide education about common sources of lead exposure and information on how to prevent further lead exposure.
- Common sources of exposure include paint in homes built before 1978, contaminated soil, and contaminated drinking water. In addition to these sources of lead, there are several other sources that exist and can be harmful to children.
- Adults can help reduce children's lead exposure by frequently washing children's hands, especially before meals and frequently wiping and cleaning children's toys.
Children in homes built before 1978
For children living in or visiting homes or structures built before 1978, adults can reduce lead exposure from lead-based paint by:
- Regularly wet-wiping windows and windowsills and wet-mopping floors.
- Avoiding repairs and construction projects that may create lead-based paint dust.
- Covering chipping or peeling paint to keep lead from spreading to surrounding areas.
- Using approved methods for removing lead hazards from the home and using contractors certified by the Environmental Protection Agency (EPA) when repairs or renovations are needed. Visit EPA's webpage to locate a certified contractor.
- Obtaining a confirmatory venous sample for blood lead testing. Use the schedule shown in Table 1.
Confirmed venous blood lead level
CDC recommends that healthcare providers use a venous draw for confirmatory BLL screening. If the initial screening test used a venous sample, the patient does not need another venous draw.
If the patient's BLL is < 3.5 micrograms per deciliter
- Provide education about common sources of lead exposure and information on how to further prevent exposure.
- During well-child visits, check development to make sure age-appropriate milestones are being met.
- During well-child visits, discuss diet and nutrition with a focus on iron and calcium intake.
- Conduct follow-up blood lead testing at recommended intervals based on the child's age.
- Centers for Medicare and Medicaid Services requires all children enrolled in Medicaid to get tested for lead at ages 12 and 24 months, or age 24–72 months if they have never been screened.
- For children not enrolled in Medicaid, CDC recommends focusing screening efforts on high-risk neighborhoods and children. Identify risk for lead poisoning based on the age of housing and social and demographic risk factors.
- Public health personnel and healthcare workers should use local data to develop screening plans that are responsive to local conditions. In the absence of such plans, CDC recommends universal blood lead testing.
If the patient's BLL is 3.5-19 micrograms per deciliter
- Follow the recommendations above for BLL < 3.5 μg/dL.
- Report the test result to your state or local health department.
- Obtain an environmental exposure history to identify potential sources of lead.
- Arrange for an environmental investigation of the home to identify potential sources of lead, as required.
- During an environmental investigation, professionals check the child's environment for possible causes of lead exposure and recommend ways to prevent further lead exposure.
- BLLs < 5 μg/dL may not trigger a Department of Housing and Urban Development (HUD) environmental investigation when the housing is covered by the HUD's Lead Safe Housing Rule. Additionally, environmental investigations for BLLs that are 3.5–19 μg/dL vary based on jurisdictional requirements and available resources.
- Ensure the child does not have iron deficiency using testing and treatment. Follow testing and treatment guidelines from the American Academy of Pediatrics (AAP).
- Discuss the child's diet and nutrition with a focus on calcium and iron intake. Refer caregivers to supportive services, as needed (e.g., Special Supplemental Nutrition Program for Women, Infants and Children).
- Check the child's development to ensure appropriate milestones are being met per AAP guidelines. Refer caregivers to supportive services, as needed (e.g., developmental specialists, Early Intervention Program).
- Provide follow-up BLL testing at recommended intervals. See schedule shown in Table 2.
If the patient's BLL is 20-44 micrograms per deciliter
- Follow the recommendations above for BLL is 3.5–19 μg/dL.
- Perform a complete history and physical exam, assessing the child for signs and symptoms related to lead exposure.
- Arrange for or refer the family for an environmental investigation of the home and a lead hazard reduction program.
- Consider performing an abdominal X-ray to check for lead-based paint chips and other radiopaque foreign bodies. This is important for young children who tend to swallow or eat non-food items. Children may also put their mouths on surfaces that could be covered with lead dust. Initiate bowel decontamination if indicated.
- Contact a Pediatric Environmental Health Specialty Unit (PEHSU) or the Poison Control Center (1-800-222-1222) for guidance. PEHSUs provide information on protecting children and reproductive-age adults from environmental hazards. PEHSUs work with healthcare professionals, parents, schools, and community groups.
If the patient's BLL is ≥ 45 micrograms per deciliter
- Follow recommendations for BLL 20–44 μg/dL.
- Perform a complete history and physical exam including a detailed neurological exam.
- Perform an abdominal X-ray and, if needed, initiate bowel decontamination.
- If the patient exhibits signs or symptoms of lead poisoning, including, confusion, weakness, seizures, coma, nausea, vomiting, and abdominal pain, admit them to a hospital as soon as possible.
- Consider admitting the patient to a hospital if one of these conditions exists:
- The patient's home is not lead-safe, and they are unable to find a lead-free living space.
- The source of lead exposure has not been identified, and the potential for further lead exposure is still possible.
- The healthcare provider is consulting with a medical toxicologist or pediatrician with experience in treating lead poisoning to initiate:
- Gastrointestinal decontamination (removal of swallowed lead using laxatives) or
- Chelation therapy (a treatment that uses a medication to remove lead from the body when BLLs are very high).
- Contact a PEHSU or Poison Control Center (1-800-222-1222) for assistance.
Table 1
Recommended schedule for obtaining a confirmatory venous sample
Blood Lead Level (μg/dL)
Time to Confirmation Testing**
≥3.5–9
Within 3 months
10–19
Within 1 month
20–44
Within 2 weeks
≥45
Within 48 hours
**The higher the BLL is on the initial screening capillary test, the more urgent it is to get a venous sample for confirmatory testing.
Table 2
Schedule for follow-up blood lead testing
Venous blood lead levels (µg/dL)
Early follow up testing (2–4 tests after initial test above specific venous BLLs)
Later follow up testing after BLL declining
≥3.5–9
3 months*
6–9 months
10–19
1–3 months*
3–6 months
20–44
2 weeks–1 month
1–3 months
≥45
As soon as possible
As soon as possible
Note: changes in BLLs due to seasonal weather changes may be more apparent in colder climate areas. Greater exposure in the summer months may necessitate more frequent follow ups.
*Some case managers or healthcare providers may choose to repeat blood lead tests on all new patients within a month. Repeated testing may confirm that the child's BLL is decreasing.
Additional resources
- Blood Lead Levels in Children – information on blood lead testing in children
- Testing Children for Lead Poisoning – information about testing children for lead poisoning.
- Blood Lead Reference Value – CDC recommendations on children's blood lead levels.
- American Academy of Pediatrics (AAP) information on lead exposure – information and resources for physicians on prevention and medical management.
- Find a Pediatric Environmental Health Specialty Unit (PEHSU) in Your Region – information about protecting children from environmental hazards.
- Learn more about the causes, symptoms, and prevention of childhood lead exposure with these videos in English and en Español.
- CDC's recommended terminology when discussing children's blood lead levels
- American Academy of Pediatrics Council on Environmental Health. Chapter 32: Lead. In: Etzel RA, ed. Pediatric Environmental Health, 4thEdition; Itasca, IL: American Academy of Pediatrics; 2019:557–584.
- Hauptman M, Bruccoleri R, Woolf AD. An Update on Childhood Lead Poisoning. Clinical Pediatric Emergency Medicine. 2017 September; 18(3): 181–192.
- Advisory Committee for Childhood Lead Poisoning Prevention, 2012. Low Level Lead Exposure Harms Children: A Renewed Call for Primary Prevention
- The Clinical & Laboratory Standards Institute (CLSI) Guidelines #C40: Measurement Procedures for the Determination of Lead Concentrations in Blood and Urine, 2nd Edition (October 2013).
