Key points
- Chagas disease is caused by the parasite Trypanosoma cruzi. It usually spreads through contact with triatomine bugs, sometimes called kissing bugs.
- Chagas disease is most common in rural areas of Mexico and Central and South America.
- The early stage, or acute infection, of Chagas disease often has mild symptoms or goes unnoticed. Chronic infection can lead to serious heart and digestive system issues.
- Early diagnosis and treatment can be lifesaving.

Overview
Chagas disease is a condition caused by the parasite Trypanosoma cruzi. This parasite is mainly found in rural areas of Mexico and Central and South America. Triatomine bugs can carry the parasite and infect people and animals. About 8 million people globally, including an estimated 280,000 in the United States, have this disease, often without knowing it. Without treatment, Chagas disease can be life-threatening.
As people living with Chagas disease move from rural areas to cities and other countries, Chagas disease has spread to new areas. In places like the United States, where Chagas disease is present but not regularly spread by triatomine bugs, it is important to recognize infection and prevent its spread through blood transfusion, organ transplants, and from pregnant women to their babies.
Signs and symptoms
Chagas disease has two stages. The first stage, called the acute phase, happens shortly after infection. The second stage, known as the chronic phase, occurs over a long time. In both stages, some people might not feel sick at all, while others can have serious health problems.
This early stage happens in the first weeks or months after getting infected. Symptoms are often mild or not there at all and can include:
- Fever
- Feeling tired
- Body aches
- Headache
- Rash
- Loss of appetite
- Diarrhea
- Vomiting
- Eyelid swelling (Romaña's sign)
Chronic phase
This stage can last many years or even a lifetime. Most people have no symptoms during this time. However, about 20 – 30% of those infected develop serious problems, including:
- Heart issues, such as an enlarged heart, heart failure, altered heart rate or rhythm, or sudden death.
- Digestive problems, such as an enlarged esophagus or colon, leading to trouble eating or going to the bathroom.
Romaña's sign
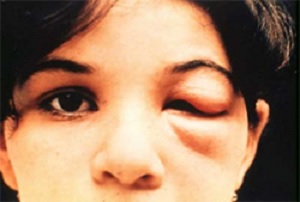
A symptom of Chagas disease is Romaña's sign—when the eyelid swells up. This happens when the Trypanosoma cruzi parasite gets into the eyelid, usually by accidentally rubbing the bug feces (poop) into your eye or into a bug bite near your eye.
Risk factors
If your mother has Chagas disease, she may have unintentionally passed on the infection to you.
If you've lived in Mexico, CA, or SA, you may have gotten CD from triatomines carrying the parasite. In some parts of Latin America, programs targeting triatomine bugs have effectively stopped the disease's spread.
How it spreads
Chagas disease mainly spreads to people from the droppings (poop) of triatomine bugs. Chagas disease does not spread from person-to-person like a cold or the flu. It also does not spread through casual contact with people or animals who are infected.
Prevention
There are no vaccines or drugs that can prevent Chagas disease at this time. The best way to prevent infection is to avoid bites from triatomine bugs.
If traveling to areas with Chagas disease, take steps to prevent infection.
Diagnosis
Only a healthcare provider can diagnose Chagas disease. Lab tests can confirm Chagas disease using a small sample of your blood. If you have symptoms of Chagas disease, talk with your healthcare providers—especially if you have traveled to an area where Chagas disease is widespread.
Treatment
Antiparasitic treatment can kill the parasite that causes Chagas disease and works best when started early.
Your healthcare provider can prescribe medicines to help manage your symptoms. Learn more about treatment of Chagas disease.
