Antimicrobial Resistance Questions and Answers
Antimicrobial resistance is one of the greatest public health challenges of our time—few treatment options exist for people infected with antimicrobial-resistant bacteria.
Visit CDC’s Antimicrobial Resistance website for more information, including fact sheets describing some of these answers and what CDC is doing to combat this threat.
What are bacteria?
Bacteria are germs found inside and outside of our bodies. Most germs are harmless, and some can even be helpful to humans, but some bacteria can cause infections, like strep throat and urinary tract infections.
What is an antibiotic?
Antibiotics are critical tools for preventing and treating infections caused by specific bacteria in people, animals, and crops. In health care, antibiotics are one of our most powerful drugs for fighting life-threatening bacterial infections.
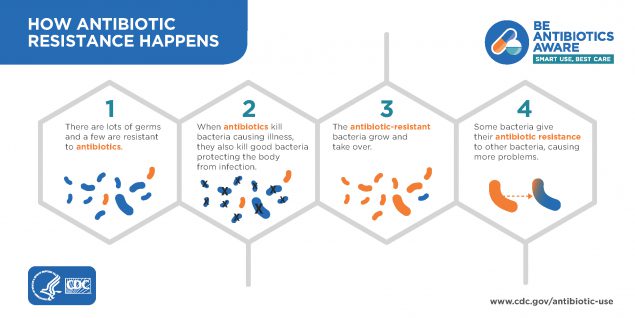
What is antimicrobial resistance?
Antimicrobial resistance happens when germs like bacteria or fungi no longer respond to the drugs designed to kill them. That means these germs are not killed and continue to grow. It does not mean our body is resistant to antibiotics or antifungals.
Antimicrobial resistance is a naturally occurring process. Bacteria and fungi are constantly finding new ways to avoid the effects of the antibiotic and antifungal drugs used to treat the infections they cause.
Infections caused by antimicrobial-resistant germs are difficult, and sometimes impossible, to treat. In many cases, antimicrobial-resistant infections require extended hospital stays, additional follow-up doctor visits, and costly and toxic alternatives.
How can taking antibiotics contribute to antimicrobial resistance?
Anytime antibiotics are used, they can contribute to antimicrobial resistance. This is because increases in antimicrobial resistance are driven by a combination of germs exposed to antibiotics, the spread of those germs, and their mechanisms of resistance. When antibiotics are needed, the benefits usually outweigh the risks of antimicrobial resistance. However, too many antibiotics are being used unnecessarily and misused, which threatens the usefulness of these important drugs.
For example, too many antibiotics are being prescribed unnecessarily to people in the United States. CDC estimates about 47 million antibiotic courses are prescribed for infections that don’t need antibiotics, like colds and the flu, in U.S. doctors’ offices and emergency departments each year. That’s about 28% of all antibiotics prescribed in these settings.
Everyone has a role to play in improving antibiotic use. Appropriate antibiotic use helps fight antimicrobial resistance and ensures these lifesaving drugs will be available for future generations.
More about Antimicrobial Resistance
How to Use Antibiotics

Antimicrobial resistance can affect any person, at any stage of life. People receiving health care or those with weakened immune systems are often at higher risk for getting an infection.
Antimicrobial resistance jeopardizes advancements in modern health care that we have come to rely on, such as joint replacements, organ transplants, and cancer therapy. These procedures have a significant risk of infection, and patients won’t be able to receive them if effective antibiotics are not available.
Aside from healthcare, antimicrobial resistance also impacts veterinary and agriculture industries.
No one can completely avoid getting an infection, but there are additional steps you can take to protect yourself and your family.
Taking antibiotics only when they are needed is an important way you can protect yourself and your family from antimicrobial resistance. Talk to your doctor about the best treatment if you are sick. Never pressure your doctor to prescribe an antibiotic.
When antibiotics aren’t needed, they won’t help you, and their side effects could still cause harm. Ask your doctor or pharmacist about steps you can take to feel better when an antibiotic isn’t needed.
If your doctor decides an antibiotic is the best treatment when you are sick:
- Take the medication exactly as your doctor tells you.
- Do not share your medication with others.
- Do not save them for later. Talk to your pharmacist about safely discarding leftover medicines.
- Do not take antibiotics prescribed for someone else. This may delay the best treatment for you, make you even sicker, or cause side effects.
- Talk with your doctor and pharmacist if you have any questions about your antibiotics prescribed to you.
How can I protect myself and my family from antimicrobial resistance?
Other ways to protect yourself and your family from infections, including resistant infections:
- Doing your best to stay healthy and keep others healthy
- Cleaning hands
- Covering coughs
- Staying home when sick
- Getting recommended vaccines, such as the flu vaccine