FIGURE 1. Number* and percentage of respiratory specimens testing positive for influenza, by type, surveillance week, and year — U.S. World Health Organization and National Respiratory and Enteric Virus Surveillance System collaborating laboratories, United States, October 2–November 26, 2011†
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail.
Update: Influenza Activity — United States, October 2–November 26, 2011
During October 2–November 26, 2011, influenza activity remained low in the United States. Thus far, influenza A viruses have predominated, and the majority are antigenically related to the 2011–12 influenza vaccine strains for the Northern Hemisphere. This report summarizes U.S. influenza activity* since October 2 and updates the previous summary (1).
Viral Surveillance
During October 2–November 26,† the World Health Organization (WHO) and National Respiratory and Enteric Virus Surveillance System collaborating laboratories in the United States tested 24,027 respiratory specimens for influenza viruses; 266 (1.1%) were positive (Figure 1). Of these, 191 (71.8%) were influenza A viruses, and 75 (28.2%) were influenza B viruses. Of the 191 influenza A viruses, 87 (45.5%) were subtyped; 79 (90.8%) were influenza A (H3) viruses, and eight (9.1%) were 2009 influenza A (H1) viruses. Influenza viruses have been reported from 30 states in all 10 U.S. Department of Health and Human Services (HHS) regions. Of the 266 influenza-positive specimens reported to CDC so far this season, most (131 of 266 [49.2%]) have been reported from the southeastern United States (Region 4 [Alabama, Florida, Georgia, Kentucky, Mississippi, North Carolina, South Carolina, and Tennessee]).
Antigenic Characterization
WHO collaborating laboratories in the United States are requested to submit a subset of their influenza-positive specimens to CDC for further antigenic characterization. CDC has antigenically characterized 21 influenza viruses collected and submitted by U.S. laboratories since October 1, 2011, including one 2009 influenza A (H1N1), 16 influenza A (H3N2) and four influenza B viruses. The one 2009 influenza A (H1N1) virus was characterized as A/California/7/2009-like, the influenza A (H1N1) component of the 2011–12 influenza vaccine for the Northern Hemisphere. All 16 influenza A (H3N2) viruses were antigenically related to the A/Perth/16/2009, the influenza A (H3N2) component included in the 2011–12 influenza vaccine for the Northern Hemisphere. Three of the four influenza B viruses tested belong to the B/Victoria lineage and were characterized as B/Brisbane/60/2008-like, the influenza B component of the 2011–12 influenza vaccine for the Northern Hemisphere; one of the four B viruses tested belongs to the B/Yamagata lineage of viruses.
Antiviral Resistance of Influenza Virus Isolates
CDC conducts surveillance for resistance of circulating influenza viruses to influenza antiviral medications. Since October 1, 2011, a total of 31 influenza viruses (five 2009 influenza A (H1N1), 24 influenza A (H3N2), and two influenza B viruses) have been tested for antiviral resistance. None of the tested viruses were found to be resistant to either oseltamivir or zanamivir.
Novel Influenza A Viruses
Since the last influenza activity update (1), six cases of human infection with a novel influenza A virus§ were reported: two from Maine and one from Indiana in October (2), as well as three from Iowa in November. All six patients were infected with novel influenza A (H3N2) viruses with genes from swine, human, and avian lineages. The two cases in Maine occurred in children, and the case in Indiana occurred in an adult male; all patients had exposure to swine in the period immediately preceding their illness. All three cases in Iowa occurred in children with no known recent exposure to swine. The investigation in Iowa revealed evidence of limited human-to human transmission (2). All patients recovered fully.
State-Specific Activity Levels
For the week ending November 26, the geographic spread of influenza¶ was reported as local by one state (Massachusetts). Sporadic influenza activity was reported by the District of Columbia (DC), Guam, and 28 states. The U.S. Virgin Islands and 21 states reported no influenza activity. Puerto Rico did not report. No states have reported geographically regional or widespread influenza activity to date for the 2011–12 influenza season.
Outpatient Influenza-Like Illness
Since October 2, the weekly percentage of outpatient visits for influenza-like illness (ILI)** reported each week by the approximately 1,500 U.S. Outpatient Influenza-Like Illness Surveillance Network (ILINet) reporters in 50 states, New York City, Chicago, and DC, has remained below the national baseline†† of 2.4% (Figure 2). None of the regions have been above their region-specific baselines. Data collected in ILINet also are used to produce a measure of ILI activity by state. During the week ending November 26, all 50 states and New York City experienced minimal ILI activity. Data were insufficient to calculate an ILI activity level from DC.§§
Pneumonia- and Influenza-Related Mortality
For the week ending November 26, pneumonia and influenza (P&I) was reported as an underlying or contributing cause of death for 6.4% of all deaths reported to the 122 Cities Mortality Reporting System. This percentage is below the epidemic threshold¶¶ of 7.1% for that week. Since October 2, 2011, the weekly percentage of deaths attributed to pneumonia and influenza ranged from 5.9% to 6.4%, remaining below the epidemic threshold.
Influenza-Related Pediatric Mortality
No influenza-related pediatric deaths have been reported through the Influenza Associated Pediatric Mortality Surveillance System for the 2011–12 influenza season.
Reported by
World Health Organization Collaborating Center for Surveillance, Epidemiology, and Control of Influenza. Lynnette Brammer, MPH, Scott Epperson, MPH, Krista Kniss, MPH, Desiree Mustaquim, MPH, Amber Bishop, MPH, Rosaline Dhara, MPH, Michael Jhung, MD, Lenee Blanton, MPH, Teresa Wallis, MS, Lyn Finelli, DrPH, Larisa Gubareva, PhD, Joseph Bresee, MD, Alexander Klimov, PhD, Nancy Cox, PhD, Influenza Div, National Center for Immunization and Respiratory Diseases; Grace Chen, MD, EIS Officer, CDC. Corresponding contributor: Grace Chen, glchen@cdc.gov, 404-718-4585.
Editorial Note
Since October 2, surveillance data have indicated that influenza is circulating at low levels in the United States; low activity typically is noted in this early portion of the influenza season. Antigenic characterization of the viral isolates that have been submitted demonstrated that the majority of these isolates are antigenically similar to the influenza virus strains in the Northern Hemisphere 2011–12 vaccine.
Influenza vaccination is the best method for preventing influenza and its associated complications. Influenza vaccination currently is recommended for all persons aged ≥6 months (3). Vaccine manufacturers had distributed approximately 129.2 million doses of influenza vaccine in the United States as of November 25 (4). Influenza vaccination should continue to be offered by health-care providers throughout the influenza season for all persons without contraindications to vaccination to provide protection for as many persons as possible. Multiple influenza vaccines are approved for use and are being distributed during the 2011–12 season, including trivalent inactivated vaccine (TIV) for persons aged ≥6 months; live, attenuated influenza vaccine (LAIV) for nonpregnant, otherwise healthy persons aged 2–49 years; a high-dose inactivated vaccine for persons aged ≥65 years; and a new, intradermally administered vaccine, which was licensed by the Food and Drug Administration on May 10, 2011, for adults aged 18–64 years (3). Children aged 6 months–8 years who did not receive 2 doses of the 2010–11 seasonal influenza vaccine should receive 2 doses (administered at least 4 weeks apart) of the 2011–12 seasonal influenza vaccine (3).
Although annual vaccination is the best method for preventing and reducing the impact of influenza, influenza antiviral medications are an important adjunct, particularly under circumstances and in groups where vaccine might be less efficacious (5). The benefits of influenza antiviral treatment are likely to be greatest if treatment is started as soon as possible after illness onset, and evidence for benefit is strongest in studies in which treatment was started within 48 hours of illness onset (5). Antiviral treatment is recommended as early as possible for patients with confirmed or suspected influenza who have severe, complicated, or progressive illness; who require hospitalization; or who are at greater risk for influenza-related complications (5).*** However, substantial observational data and one study in pregnant women (6) have indicated that antiviral treatment still can be beneficial in patients with severe, complicated, or progressive illness and in hospitalized patients even when administered more than 48 hours after illness onset (5,7). In such cases, decisions on starting antiviral treatment should not wait for laboratory confirmation of influenza. Antiviral treatment also may be considered for outpatients with confirmed or suspected influenza who do not have known risk factors for severe illness if treatment can be initiated within 48 hours of illness onset. Recommended antiviral medications include oseltamivir and zanamivir.
Transmission of swine-origin influenza A viruses to humans is rare and usually occurs among persons in direct contact with swine or among persons who have visited places where swine are present (e.g., agricultural fairs, farms, and petting zoos). Clinicians should consider swine-origin influenza A virus infection as well as seasonal influenza virus infections in the differential diagnosis of patients with febrile respiratory illness who have been near swine (8). Clinicians who suspect influenza virus infection in patients with recent exposure to swine should obtain a nasopharyngeal swab from the patient, place the swab in a viral transport medium, and contact their state or local health department to facilitate transport and timely diagnosis at a state public health laboratory. Public health laboratories are requested to submit any suspected swine-origin influenza A samples to CDC for further testing. Early identification and prompt investigation of novel influenza A cases is critical to evaluating the extent of outbreaks and possible human-to-human transmission.
Influenza surveillance reports for the United States are posted online weekly and are available at http://www.cdc.gov/flu/weekly. Additional information regarding influenza viruses, influenza surveillance, influenza vaccine, influenza antiviral medications, and novel influenza A infections in humans is available at http://www.cdc.gov/flu.
Acknowledgments
State and territorial health departments and public health laboratories. U.S. World Health Organization collaborating laboratories. National Respiratory and Enteric Virus Surveillance System collaborating laboratories. U.S. Outpatient Influenza-Like Illness Surveillance Network. Influenza-Associated Pediatric Mortality Surveillance System. 122 Cities Mortality Reporting System.
References
- CDC. Update: influenza activity—United States, May 22–September 3, 2011. MMWR 2011;60:1239–42.
- CDC. Limited human-to-human transmission of novel influenza A (H3N2) virus—Iowa, November 2011. MMWR 60:1615–7.
- CDC. Prevention and control of influenza with vaccines: recommendations of the Advisory Committee on Immunization Practices (ACIP), 2011. MMWR 2011;60:1128–32.
- CDC. Seasonal influenza vaccine—total doses distributed. Atlanta, GA: US Department of Health and Human Services, CDC; 2011. Available at http://www.cdc.gov/flu/professionals/vaccination/vaccinesupply.htm. Accessed December 2, 2011.
- CDC. Antiviral agents for the treatment and chemoprophylaxis of influenza—recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR 2011;60(No.RR-1).
- Siston AM, Rasmussen SA, Honein MA, et al. Pandemic 2009 influenza A (H1N1) virus illness among pregnant women in the United States. JAMA 2010;303:1517–25.
- Yu H, Feng Z, Uyeki T, et al. Risk factors for severe illness with 2009 pandemic influenza A (H1N1) virus infection in China. Clin Infect Dis 2011; 52:457–65.
- CDC. Swine-origin influenza A (H3N2) virus infection in two children—Indiana and Pennsylvania, July–August 2011. MMWR 2011;60:1213–5.
* The CDC influenza surveillance system collects five categories of information from eight data sources: 1) viral surveillance (World Health Organization collaborating U.S. laboratories, the National Respiratory and Enteric Virus Surveillance System, and novel influenza A virus case reporting); 2) outpatient illness surveillance (U.S. Outpatient Influenza-Like Illness Surveillance Network); 3) mortality (122 Cities Mortality Reporting System and influenza-associated pediatric mortality reports); 4) hospitalizations (FluSurvNet, which includes the Emerging Infections Program and surveillance in four additional states); and 5) summary of geographic spread of influenza (state and territorial epidemiologist reports).
† Data as of December 3, 2011.
§ Discussions concerning virus nomenclature related to these novel H3N2 viruses, also referred to as swine-origin triple reassortant influenza A (H3N2) viruses, identified in this report are ongoing.
¶ Levels of geographic spread are 1) no activity; 2) sporadic: isolated laboratory-confirmed influenza cases or a laboratory-confirmed outbreak in one institution, with no increase in activity; 3) local: increased ILI, or at least two institutional outbreaks (ILI or laboratory-confirmed influenza) in one region with recent laboratory evidence of influenza in that region; virus activity no greater than sporadic in other regions; 4) regional: increased ILI activity or institutional outbreaks (ILI or laboratory-confirmed influenza) in at least two but less than half of the regions in the state with recent laboratory evidence of influenza in those regions; and 5) widespread: increased ILI activity or institutional outbreaks (ILI or laboratory-confirmed influenza) in at least half the regions in the state, with recent laboratory evidence of influenza in the state.
** Defined as a temperature of ≥100.0°F (≥37.8°C), oral or equivalent, and cough and/or sore throat, in the absence of a known cause other than influenza.
†† The national and regional baselines are the mean percentage of visits for ILI during noninfluenza weeks for the previous three seasons plus two standard deviations. A noninfluenza week is a week during which <10% of specimens tested positive for influenza. National and regional percentages of patient visits for ILI are weighted on the basis of state population. Use of the national baseline for regional data is not appropriate.
§§ Activity levels are based on the percentage of outpatient visits in a state for ILI and are compared with the average percentage of ILI visits that occur during weeks with little or no influenza virus circulation . Activity levels range from minimal, which would correspond to ILI activity from outpatient clinics being at or below the average, to high, which would correspond to ILI activity from outpatient clinics being much higher than the average. Because the clinical definition of ILI is very general, not all ILI is caused by influenza; however, when combined with laboratory data, the information on ILI activity provides a clear picture of influenza activity in the United States.
¶¶ The seasonal baseline proportion of pneumonia and influenza deaths is projected using a robust regression procedure in which a periodic regression model is applied to the observed percentage of deaths from pneumonia and influenza that were reported by the 122 Cities Mortality Reporting System during the preceding 5 years. The epidemic threshold is 1.645 standard deviations above the seasonal baseline.
*** Persons at greater risk include children aged <5 years (especially those aged <2 years); adults aged ≥65 years; persons with chronic pulmonary (including asthma), cardiovascular (except hypertension alone), renal, hepatic, hematologic (including sickle cell disease), metabolic (including diabetes mellitus), or neurologic and neurodevelopmental conditions (including disorders of the brain, spinal cord, peripheral nerve, and muscle, such as cerebral palsy, epilepsy [seizure disorders], stroke, intellectual disability [mental retardation], moderate to severe developmental delay, muscular dystrophy, or spinal cord injury); persons with immunosuppression, including that caused by medications or by human immunodeficiency virus infection; women who are pregnant or postpartum (within 2 weeks after delivery); persons aged ≤18 years who are receiving long-term aspirin therapy; American Indians/Alaska Natives; persons who are morbidly obese (i.e., body mass index ≥40); and residents of nursing homes and other chronic-care facilities.
What is already known on this topic?
CDC collects, compiles, and analyzes data on influenza activity year-round in the United States. Although influenza activity this season has been low, the influenza season continues through the winter and spring months.
What is added by this report?
The United States has continued to experience low levels of influenza activity from October 2 to November 26, 2011, and influenza A (H3N2), 2009 influenza A (H1N1), and influenza B viruses have been identified sporadically. The majority of viral isolates that have been submitted to CDC for testing are antigenically similar to the influenza vaccine strains in the Northern Hemisphere 2011–12 vaccine.
What are the implications for public health practice?
Influenza currently is circulating at low levels at this early point in the season. The influenza viruses currently circulating are a good match with the influenza vaccine. Vaccination remains the best method for preventing influenza and its associated complications and, influenza vaccination is recommended in all persons aged ≥6 months. Antiviral medications are an important adjunct in reducing the impact of influenza, and the benefits are likely to be greatest if antiviral treatment is started as soon as possible after illness onset.
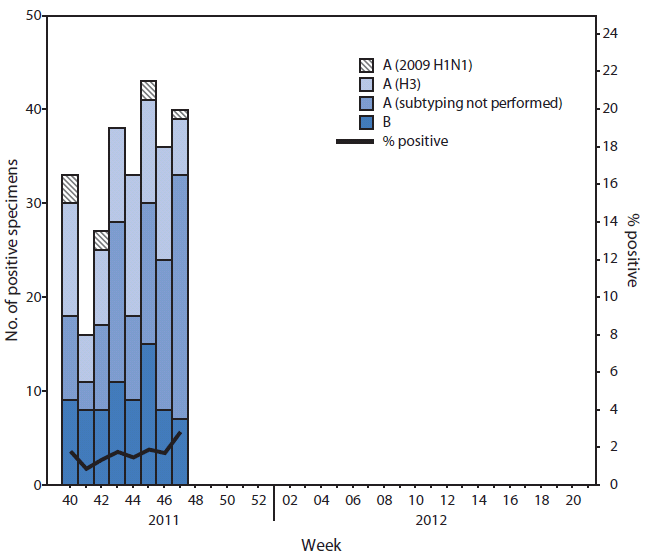
* Total tested = 24,027; total positive = 266.
† As of November 26, 2011.
Alternate Text: The figure above shows the number and percentage of respiratory specimens testing positive for influenza, by type, surveillance week, and year, in the United States during October 2-November 26, 2011, based on data from U.S. World Health Organization (WHO) and National Respiratory and Enteric Virus Surveillance System collaborating laboratories. During October 2-November 26, these laboratories tested 24,027 respiratory specimens for influenza viruses; 266 (1.1%) were positive.
FIGURE 2. Percentage of visits for influenza-like illness (ILI) reported by the U.S. Outpatient Influenza-Like Illness Surveillance Network (ILINet), by surveillance week — United States, September 28, 2008, through November 26, 2011*
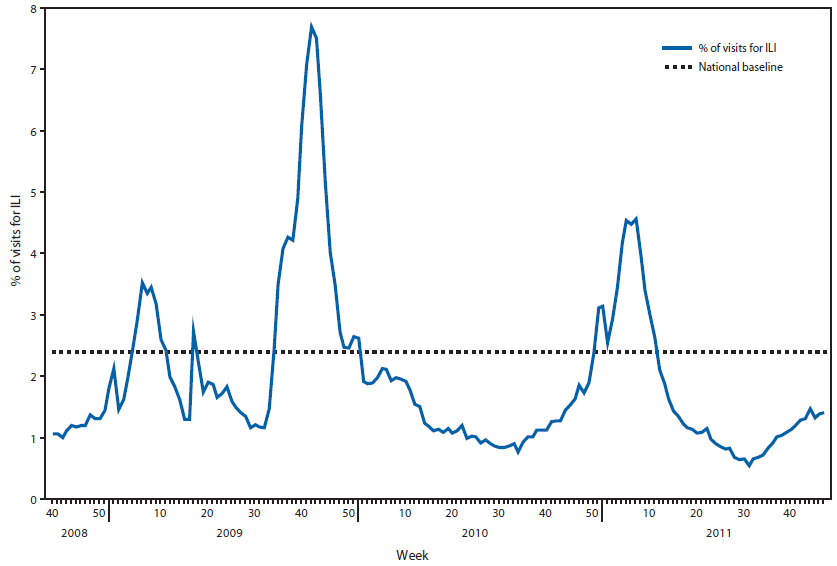
* The national baseline is the mean percentage of visits for ILI during noninfluenza weeks for the previous three seasons plus two standard deviations. A noninfluenza week is a week during which <10% of specimens tested positive for influenza. Use of the national baseline for regional data is not appropriate.
Alternate Text: The figure above shows the percentage of visits for influenza-like illness (ILI) reported by the U.S. Outpatient Influenza-Like Illness Surveillance Network (ILINet), by surveillance week, in the United States from September 28, 2008, through November 26, 2011. Since October 2, the weekly percentage of outpatient visits for ILI reported each week by the approximately 1,500 ILINet reporters in 50 states, New York City, Chicago, and the District of Columbia has remained below the national base¬line of 2.4%.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All MMWR HTML versions of articles are electronic conversions from typeset documents.
This conversion might result in character translation or format errors in the HTML version.
Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr)
and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S.
Government Printing Office (GPO), Washington, DC 20402-9371;
telephone: (202) 512-1800. Contact GPO for current prices.
**Questions or messages regarding errors in formatting should be addressed to
mmwrq@cdc.gov.


