FIGURE. Confirmed cholera cases (N = 59), by province --- Dominican Republic, 2010*
Persons using assistive technology might not be able to fully access information in this file. For assistance, please send e-mail to: mmwrq@cdc.gov. Type 508 Accommodation and the title of the report in the subject line of e-mail.
Update on Cholera --- Haiti, Dominican Republic, and Florida, 2010
On October 21, 2010, a cholera outbreak was confirmed by the Haitian National Public Health Laboratory (1). By November 19, the outbreak had reached every department of the country, and by December 17, a total of 121,518 cases of cholera, resulting in 63,711 hospitalizations and 2,591 deaths, had been reported. By November 16, additional cases of cholera had been confirmed in the neighboring Dominican Republic and in Florida. Several confirmed cases in the Dominican Republic and all confirmed U.S. cases were among travelers from Haiti. This report describes cases of cholera identified in the Dominican Republic and United States and provides recommendations to physicians regarding management of travel-related cases. Travelers who develop watery diarrhea within 5 days after returning from cholera-affected areas should seek health care and report their travel histories. Clinicians should enquire about recent travel when evaluating patients with diarrhea. When cholera is suspected, rehydration should be initiated immediately, a stool specimen should be collected for culture of Vibrio cholerae, and public health authorities should be notified.
Dominican Republic
In the Dominican Republic, intensive surveillance for cholera-like illness and laboratory testing to confirm cases were initiated by the Ministry of Public Health on October 24, 2010. Suspected cases were defined as profuse watery diarrhea among persons aged ≥5 years, death in a person with acute watery diarrhea, or diarrhea among persons with an epidemiologic link to a laboratory-confirmed case. Suspected cases were reported to the Ministry's Division of Epidemiology. When possible, rectal swabs were collected from suspected cases, transported in Cary Blair media, and sent to the National Reference Laboratory for confirmation by isolation of V. cholerae and agglutination with V. cholerae O1 antiserum.
Through December 18, a total of 399 suspected cases were reported; laboratory testing was performed for at least 327 of these cases. V. cholerae O1 serotype Ogawa was identified in 59 cases; the majority of negative test results were attributed to other enteric pathogens for which testing is not performed routinely. Three confirmed cases were attributed to importation from Haiti, one each in the provinces of La Altagracia, Independencia and Monte Cristi. The remaining 56 confirmed cases occurred in the provinces of Santiago (19), San Juan (11), Elías Piña (10), Santo Domingo (10), Dajabón (two), Valverde (two), Independencia (one), and Monte Cristi (one). These 56 cases, with no known association with travel from Haiti, were attributed to local transmission (Figure). Of the 59 confirmed cases, 46 (78%) resulted in hospitalization; no fatalities have been confirmed.
Three separate outbreaks of cholera, involving 19 of the 59 confirmed cases, were identified and investigated in the Dominican Republic. In El Dique, a resource-poor neighborhood in the capital city of Santo Domingo, eight cases of cholera-like illness, including six confirmed cholera cases, were identified in two households; investigation suggested household transmission, although the vehicle of transmission was not determined. In a second outbreak in Navarrete, Santiago Province, preliminary investigation suggested that contaminated canal water was the source of infection for 29 cases of cholera-like illness (six confirmed). A third outbreak in Bánica, Elías Piña Province, occurred in a community along the banks of the Artibonite River near the Haitian border and resulted in nine cases (seven confirmed); drinking untreated river water was considered the most likely source of infection.
United States
In the United States, cholera is a nationally notifiable disease. A confirmed case of cholera is defined by the Council of State and Territorial Epidemiologists as a clinically compatible illness in a person from whom toxigenic V. cholerae O1 or O139 has been isolated from stool or vomitus, or who has serologic evidence of recent infection.* After the outbreak was confirmed in Haiti, to encourage early reporting of suspected cholera cases without waiting for laboratory confirmation, the Florida Department of Health created two working case classifications for surveillance purposes.† A probable case was defined as a clinically compatible illness in a person with a stool culture that yielded Vibrio species and who recently traveled to Haiti or another affected area or who was linked epidemiologically to a confirmed case. A suspected case was defined as a clinically compatible illness in a person who recently traveled to Haiti or another affected area or who was linked epidemiologically to a confirmed case, but whose stool culture or serology results were pending. Case reporting guidelines were distributed to county health departments, and clinician advisories were developed and distributed.
As of December 18, a total of 13 cases had been investigated by the Florida Department of Health. V. cholerae O1 serotype Ogawa was isolated from stool specimens of five patients at Florida laboratories. All five developed symptoms during October 23--November 29, either while in Haiti or on the day of arrival in Florida from Haiti. The five patients with confirmed cases ranged in age from 9 to 84 years; four were female. One patient reported using community well water in Haiti for drinking and bathing, one had eaten several meals in family homes in Haiti, and one was a physician who had treated cholera patients in Haiti but might have had other exposures. In addition to diarrhea, reported symptoms included abdominal pain or cramping, vomiting, and lethargy or weakness.
Four of the five patients were hospitalized, including two who had been evaluated in an emergency department, discharged the same day, and readmitted 2--3 days later. A history of recent travel from Haiti had not been elicited on the first emergency department visit for one of those patients. All five patients with confirmed cholera received intravenous rehydration and oral antibiotics, including single doses of doxycycline or ciprofloxacin or multiday courses of doxycycline, tetracycline, azithromycin, or ciprofloxacin; three patients received two different antibiotics. Some treatment regimens were not consistent with recommendations. No secondary transmission was identified.
Characterization of Isolates
Isolates from four confirmed cases in the Dominican Republic and all five Florida cases were sent to CDC for confirmation and additional characterization. All were confirmed as toxigenic V. cholerae O1, serotype Ogawa, biotype El Tor, and matched the Haiti outbreak strain by pulsed-field gel electrophoresis (2). Those isolates from Florida cases had the same antimicrobial susceptibility pattern as the Haiti outbreak strain (pending for Dominican Republic isolates). CDC's laboratory assessment of 380 cholera isolates subtyped since 2005 has indicated that isolates from the cases in Haiti, the Dominican Republic, and Florida are most similar to a strain previously characterized from South Asia and elsewhere.
Reported by
PH Jenkins, MPH, HJ Montejano, MS, Broward County Health Dept; MJ Abbasi, MD, MS Crowley, MS, MG O'Brien, Collier County Health Dept; V Conte, MD, M Etienne, MPH, E Rico, MPH, Miami-Dade County Health Dept; DG Rea, MPH, Orange County Health Dept; RM Baker, MS, EA Burden, LD Gillis, PhD, JJ Hamilton, MPH, RS Hopkins, MD, AC Kite-Powell, MS, E Merlo, Florida Dept of Health. Ministry of Public Health, Dominican Republic. Ministry of Public Health and Population, Haiti. Pan American Health Organization. CDC.
Editorial Note
Less than 4 weeks after the Haitian National Public Health Laboratory first confirmed cholera in Haiti and before cholera had been identified in all 10 Haitian departments, confirmed cases were reported in the neighboring Dominican Republic and in a resident of Florida who had traveled to Haiti. Transnational spread of cholera is not uncommon. In late January 1991, an outbreak of cholera began in Peru and, by 1992, had spread to most other countries in Central and South America and to the United States (3). During 2000--2008, of 51 cholera cases in the United States reported to CDC, 29 (57%) were associated with international travel.§
Although transnational spread of cholera is caused most commonly by importation by travelers, it also has been associated with contaminated food that was imported commercially (4) or transported by travelers (5). Toxigenic V. cholerae also can be transported by ships' ballast water (6).
Travel between Haiti and other countries predominantly involves those countries where most expatriate Haitians reside (7). In November, of approximately 60,000 airline passenger seats available on direct flights from Haiti, 76% were on flights to the United States and U.S. territories, 17% to the Dominican Republic and other Caribbean islands, 4% to France, 2% to Canada, and 2% to Panama.¶ Substantial travel also occurs across the border between Haiti and the Dominican Republic.
More cholera cases associated with the current outbreak in Haiti are expected. In preparation for an anticipated increase in holiday travel, public health authorities in countries receiving travelers from Haiti should consider the need to heighten surveillance for cholera and educate clinicians to be vigilant for cholera-like illness in patients who have traveled from cholera-affected areas. CDC is distributing Travel Health Alert Notices to travelers from Haiti to the United States, advising them to seek health care promptly if they develop diarrhea within 5 days after arrival.
Although the risk for acquiring cholera during travel is low (8), travelers can reduce their risk for cholera and other enteric infections by drinking and using water that has been boiled or treated or is supplied in cans or bottles, eating only food that has been cooked and served hot, paying vigorous attention to handwashing with soap, and avoiding swimming or bathing in rivers. Health-care providers and persons traveling to Haiti or other cholera-affected countries should consult CDC,** World Health Organization (WHO),†† or Pan American Health Organization (PAHO)§§ websites for general information about international travel and for specific information related to cholera. Neither cholera vaccine nor chemoprophylaxis is indicated for U.S. travelers to Haiti. CDC, the Haitian Ministry of Public Health and Population, PAHO, and other organizations are evaluating the potential role of cholera vaccines for populations in Haiti and other countries.
Physicians evaluating patients with diarrhea should obtain a travel history. If cholera is suspected, clinicians should initiate rehydration, treat hospitalized patients with antibiotics, obtain a stool specimen for culture before starting antibiotic treatment (if indicated), and report the case to public health authorities. The risk for person-to-person transmission is low, and isolation of cholera patients or quarantine of asymptomatic travelers from affected areas is not warranted. However, persons in sensitive occupations, such as food preparation, child care or health care, should not work while they have diarrhea.
The mainstay of cholera treatment is vigorous oral or intravenous rehydration. Antibiotics can reduce the volume and duration of diarrhea and should be given to hospitalized patients. A single dose of doxycycline by mouth (300 mg for nonpregnant adults; 2--4 mg/kg for children, not to exceed 300 mg) is the preferred regimen. A single dose of azithromycin (1 g by mouth) is recommended for pregnant women. Alternative therapies and additional guidance for clinicians are available from CDC¶¶ and PAHO.
The Florida Department of Health provided advisories to clinicians, prompting correct referral of specimens to clinical laboratories. Because Vibrio species require special media for isolation, the laboratory should be notified to suspect cholera. Specific information on V. cholerae culture methods and specimen transport can be found at CDC's cholera website.*** In the United States, all suspected cholera isolates should be sent to state public health laboratories and from there to CDC for confirmation and additional characterization.
The potential for secondary transmission of cholera is low in countries where sanitation, water, and food production systems minimize the risk for fecal contamination. Only two instances of secondary transmission in the United States have been reported since 1965 (8,9). Spread within the Dominican Republic has been limited to date, as is typical in countries with improved water and sanitation infrastructure.††† Nonetheless, the risk for secondary and ongoing transmission of cholera remains high in populations with limited access to improved water sources and sanitation.
An increase in reported cases of cholera associated with holiday travel to cholera-affected areas is anticipated in the United States and other countries. Travelers are encouraged to take precautions, and providers should suspect cholera in patients with diarrhea and recent travel to cholera-affected areas. All suspected cases should be reported to public health authorities, and stool samples should be collected under appropriate conditions to increase the yield of V. cholerae. In 2009, 45 countries reported 221,226 cases of cholera to WHO (10). The persistence of cholera in any country puts other countries at risk. Until cholera is controlled around the world, importations to other countries probably will continue, and areas with poor water and sanitation infrastructure will be at risk for transmission. Public health authorities in unaffected countries should be vigilant in monitoring for cholera introductions and take public health actions to prevent its spread.
References
- CDC. Update: outbreak of cholera---Haiti, 2010. MMWR 2010;59:1586--90.
- CDC. Update: cholera outbreak---Haiti, 2010. MMWR 2010;59;1473--9.
- CDC. Update: Vibrio cholerae O1---Western Hemisphere, 1991--1994, and V. cholerae O139---Asia, 1994. MMWR 1995;44:215--9.
- Taylor JL, Tuttle J, Pramukul T, et al. An outbreak of cholera in Maryland associated with imported commercial frozen fresh coconut milk. J Infect Dis 1993;167:1330--5.
- Finelli L, Swerdlow D, Mertz K, Ragazzoni H, Spitalny K. Outbreak of cholera associated with crab brought from an area with epidemic disease. J Infect Dis 1992;166:1433--5.
- McCarthy SA, Khambaty FM. International dissemination of epidemic Vibrio cholerae by cargo ship ballast and other nonpotable waters. Appl Environ Microbiol 1994;60:2597--601.
- Pan American Health Organization. Haiti. In: Health in the Americas. Volume II-countries. Pan American Health Organization; 2007:412--29. Available at http://www.paho.org/hia/archivosvol2/paisesing/haiti%20english.pdf.
- Weber JT, Levine WC, Hopkins DP, Tauxe RV. Cholera in the United States, 1965--1991. Risks at home and abroad. Arch Intern Med 1994;154:551--6.
- Ackers M, Pagaduan R, Hart G, et al. Cholera and sliced fruit: probable secondary transmission from an asymptomatic carrier in the United States. Int J Infect Dis 1997;1:212--4.
- World Health Organization. Cholera, 2009. Wkly Epidemiol Rec 2010;85:293--308.
* Case definition available at http://www.cdc.gov/ncphi/disss/nndss/casedef/cholera_current.htm.
† Available at http://www.doh.state.fl.us/disease_ctrl/epi/acute/haiti_cholera_impact_surv_guidance_chds_v1.1.pdf.
§ Information available at http://www.cdc.gov/nationalsurveillance/cholera_vibrio_surveillance.html.
¶ Information obtained December 3, 2010, from https://www.airlineplanning.com.
** Available at http://wwwnc.cdc.gov/travel.
†† Available at http://www.who.int/ith/en.
§§ Available at http://new.paho.org/hq/index.php?option=com_content&task=view&id=4500&Itemid=3527&lang=en.
¶¶ Available at http://www.cdc.gov/haiticholera/consider-cholera.htm.
*** Available at http://www.cdc.gov/cholera/laboratory.html.
††† Improved water and sanitation as defined by the World Health Organization and the United Nations Children's Fund Joint Monitoring Programme for Water Supply and Sanitation. Information available at http://www.wssinfo.org/definitions-methods/watsan-categories.
What is already known on this topic?
A cholera outbreak has spread rapidly through Haiti since October 2010. Transnational spread of cholera is not uncommon.
What is added by this report?
Cholera has now been confirmed in the Dominican Republic and Florida, and the strains are indistinguishable from the strain causing the outbreak in Haiti. Secondary spread in the Dominican Republic has been limited to date; in the United States, no transmission to household contacts has been reported.
What are the implications for public health practice?
Additional cases of cholera in travelers from Haiti are likely to occur in the United States, the Dominican Republic, and elsewhere. Clinicians should ask patients with diarrhea about their travel history. If cholera is suspected, clinicians should initiate rehydration, treat hospitalized patients with antibiotics, obtain a stool specimen for culture before starting antibiotic treatment (if indicated), and report the case to public health authorities.
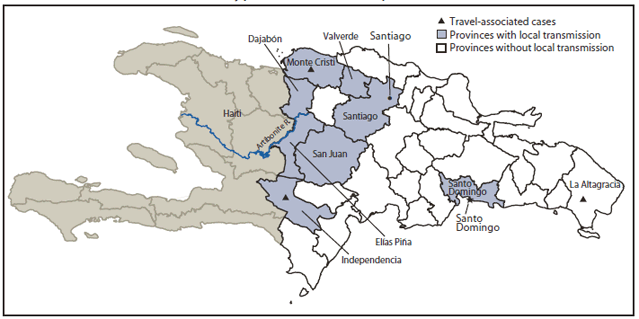
* Through December 18, 2010.
Alternate Text: The figure above shows confirmed cholera cases (N = 59), by province in the Dominican Republic in 2010. Three confirmed cases were attributed to importation from Haiti, one each in the provinces of La Altagracia, Independencia and Monte Cristi. The remaining 56 confirmed cases, with no known association with travel from Haiti, have been attributed to local transmission.
Use of trade names and commercial sources is for identification only and does not imply endorsement by the U.S. Department of
Health and Human Services.
References to non-CDC sites on the Internet are
provided as a service to MMWR readers and do not constitute or imply
endorsement of these organizations or their programs by CDC or the U.S.
Department of Health and Human Services. CDC is not responsible for the content
of pages found at these sites. URL addresses listed in MMWR were current as of
the date of publication.
All MMWR HTML versions of articles are electronic conversions from typeset documents.
This conversion might result in character translation or format errors in the HTML version.
Users are referred to the electronic PDF version (http://www.cdc.gov/mmwr)
and/or the original MMWR paper copy for printable versions of official text, figures, and tables.
An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S.
Government Printing Office (GPO), Washington, DC 20402-9371;
telephone: (202) 512-1800. Contact GPO for current prices.
**Questions or messages regarding errors in formatting should be addressed to
mmwrq@cdc.gov.


