Key points
- Zoonotic hookworm infection causes inflammation and skin lesions.
- Diagnosis is based on characteristic signs and symptoms and exposure history.
- Most cases resolve without treatment.
- Medications may be required for severe cases.
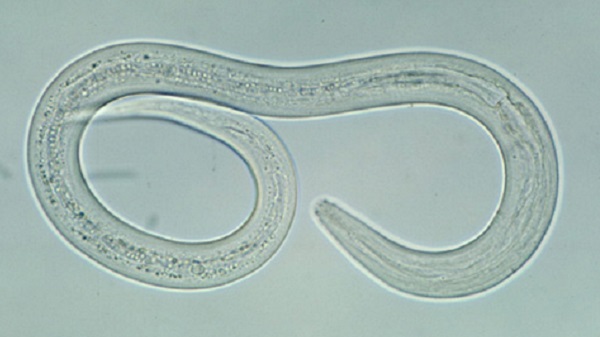
Clinical Presentation
Zoonotic hookworm infection produces an inflammatory reaction known as cutaneous larva migrans (CLM). The parasite's larvae penetrate exposed skin and migrate through the skin or, rarely, into deeper tissues such as the lungs, intestinal tract, or possibly the eye.
- In humans, the larvae of most animal hookworm species cannot penetrate beyond the dermis.
- The larvae of Ancylostoma braziliense will migrate in the epidermis and cause CLM for several weeks before dying. The resulting lesions in the skin resolve spontaneously.
- A. caninum and A. ceylanicum larvae can penetrate more deeply and migrate beyond the dermis. They have been associated with other clinical syndromes, including eosinophilic enteritis.
- Eosinophilic pneumonitis has been reported to occur in patients with CLM, possibly due to larval migration to the lungs.
- Allergic reactions may occur in people who have multiple exposures to the parasite, with an extreme inflammatory response around the exposed area of the skin.
The incubation period for CLM is typically short. Signs and symptoms develop several days after larval penetration of the skin.
- The median time to symptom development in reported outbreaks of CLM ranged from 10 to 15 days.
- However, in some cases, onset of disease may be delayed for weeks to months.
Common symptoms
CLM usually appears in parts of the body that have had unprotected contact with contaminated soil or sand, often bare feet or skin not covered by clothing.
- The most common symptom is intense pruritis, which usually develops first.
- Afterward, an irregular erythematous raised track appears, presumably marking the progress of the larva from the site of penetration.
- The track may move in the skin over time. However, the location of the track may not relate to the location of the larva, which is randomly moving ahead of the track formation.
- Typically, the track moves several millimeters per day and is about 3 mm wide.
- Single tracks or multiple tracks may be present, depending on the severity of infection.
- Complications such as vesiculobullous lesions and edema or, rarely, folliculitis, may develop.
Eosinophilia may or may be present and is more likely when deeper tissue penetration occurs.
Less common disease manifestations include:
- Eosinophilic enteritis
- Ocular larva migrans
- Diffuse unilateral subacute retinitis (DUSN).
Rarely, eosinophilic enteritis has been associated with A. caninum infections, probably due to deeper migration of larvae or possibly inadvertent consumption of infective larvae.
Cases of ocular larva migrans have been attributed to zoonotic hookworm larvae migration to the eye. This is based on the smaller size of these larvae relative to Toxocara or Baylisascaris larvae.
Zoonotic hookworm larvae migration has been suggested as a cause of DUSN, largely based on epidemiological features.
Diagnosis
CLM is a clinical diagnosis based on the presence of the characteristic signs and symptoms and exposure history. For example, the diagnosis can be made based on presence of raised erythematous tracks with pruritis on the feet or lower extremities of a patient with recent travel history to tropical areas.
There is no serological testing for zoonotic hookworm infection. Skin biopsy is not sufficiently sensitive to diagnose CLM, since the location of the migrating larva cannot be predicted by the track.
Differential diagnoses include:
Consider other conditions, such as cutaneous pili migrans, myiasis, and scabies.
