Ehrlichiosis
‹View Table of Contents
Agents
Ehrlichia chaffeensis, Ehrlichia ewingii, Ehrlichia muris eauclairensis
Ehrlichiosis can be severe or, in rare cases, fatal.
Incidence of E. chaffeensis enhrlichiosis generally increases with age, however, case-fatality rates are highest among children aged <10 years and adults aged ≥70 years.
Where Found
Ehrlichiosis is most frequently reported from the southeastern and south-central United States, from the East Coast extending westward to Texas. The areas from which most cases are reported correspond with the known geographic distribution of the lone star tick (Amblyomma americanum), which is associated with transmission of both E. chaffeensis and E. ewingii. In 2019, four states (Missouri, Arkansas, North Carolina, and New York) accounted for nearly half of all reported cases of E. chaffeensis ehrlichiosis. Since 2009, >115 cases of ehrlichiosis caused by E. muris eauclairensis have been identified in patients in the Upper Midwest. The tick responsible for transmitting this new subspecies of Ehrlichia is Ixodes scapularis, and the clinical presentation is generally similar to those associated with infections caused by E. chaffeensis and E. ewingii.
Incubation Period
5–14 days
Signs and Symptoms
- Fever, chills
- Headache
- Malaise
- Muscle pain
- Gastrointestinal symptoms (nausea, vomiting, diarrhea, anorexia)
- Altered mental status
- Rash (more commonly reported among children)
The Signs and Symptoms list presents symptoms commonly seen with ehrlichiosis. However, it is important to note that few people will develop all symptoms, and the number and combination of symptoms varies greatly from person to person.

CONFIRMATION OF THE DIAGNOSIS IS BASED ON LABORATORY TESTING, BUT ANTIBIOTIC THERAPY SHOULD NOT BE DELAYED IN A PATIENT WITH A SUGGESTIVE CLINICAL PRESENTATION.
General Laboratory Findings
Typically observed during the first week of clinical disease:
- Thrombocytopenia
- Leukopenia (absolute)
- Anemia (generally occurs later in illness than thrombocytopenia or leukopenia)
- Mild to moderate elevations in hepatic transaminases
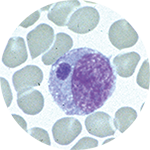
During the acute stage of illness, morulae can be detected in about 20% of patients. E. chaffeensis most commonly infects monocytes, whereas E. ewingii more commonly infects granulocytes. The target cell of E. muris eauclairensis has not yet been identified. Visualization of morulae during examination of blood smears is highly suggestive of a diagnosis; however, blood smear examination is insensitive and should never be relied upon solely to rule ehrlichiosis in or out.
Laboratory Diagnosis
- Detection of DNA by PCR of whole blood. This method is most sensitive during the first week of illness and sensitivity can decrease after administration of tetracycline-class antibiotics.
- Demonstration of a four-fold rise in IgG-specific antibody titer by indirect immunofluorescence antibody (IFA) assay in paired serum samples. The first sample should be taken within the first 2 weeks of illness, and the second should be taken 2 to 4 weeks later.
- Immunohistochemical (IHC) staining of organism from skin, tissue, or bone marrow biopsies.
NOTE: Antibody titers are frequently negative in the first 7–10 days of illness. Acute antibody results cannot independently be relied upon for confirmation.
NOTE: IgM antibodies are less specific than IgG antibodies and are more likely to generate false positives. IgM results alone should not be used for laboratory diagnosis.
Treatment
Anaplasmosis, ehrlichiosis, and spotted fever group rickettsioses are treated with doxycycline. Clinical suspicion of any of these diseases is sufficient to begin treatment. Delay in treatment may result in severe illness and death. These regimens may need to be adjusted depending on a person’s age, medical history, underlying health conditions, pregnancy status, or allergies. Consult an infectious disease specialist in cases of pregnancy or life-threatening allergy to doxycycline.
| Age Category | Drug | Dosage | Maximum | Duration (Days) |
|---|---|---|---|---|
| Adults | Doxycycline | 100 mg twice per day, orally or IV | 100 mg/dose | Patients should be treated for at least 3 days after the fever subsides and until there is evidence of clinical improvement. Minimum course of treatment is 5-7 days. |
| Children weighing <100 lbs. (45.4 kg) | Doxycycline | 2.2 mg/kg per dose twice per day, orally or IV | 100 mg/dose |
NOTE: Use doxycycline as first-line treatment for suspected ehrlichiosis in patients of all ages. The use of doxycycline to treat suspected ehrlichiosis in children is recommended by both the CDC and the American Academy of Pediatrics Committee on Infectious Diseases. Use of antibiotics other than doxycycline increases the risk of patient death. At the recommended dose and duration needed to treat ehrlichiosis, no evidence has been shown to cause staining of permanent teeth, even when multiple courses are given before the age of eight.
References
Centers for Disease Control and Prevention. Diagnosis and management of tickborne rickettsial diseases: Rocky Mountain spotted fever and other spotted fever group rickettsioses, ehrlichioses, and anaplasmosis—United States: a practical guide for health care and public health professionals. MMWR 2016; 65 (No.RR-2).
Dumler JS, Madigan JE, Pusterla N, et al. Ehrlichioses in humans: epidemiology, clinical presentation, diagnosis, and treatment. Clin Infect Dis 2007 Jul 15;45 Suppl 1:S45–51.
Engel J, Bradley K, et al. Revision of the national surveillance case definition for ehrlichiosis. Council of State and Territorial Epidemiologists, Infectious Diseases Committee, 2007 Position Statement [PDF – 7 pages].
Gelfand JA, Vannier E. Ehrlichia chaffeensis (human monocytotropic ehrlichiosis), Anaplasma phagocytophilum (human granulocytotropic anaplasmosis) and other ehrlichiae. In: Mandell GL, Bennett JE, Dolin R, editors. Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases. 6th ed. Philadelphia, PA: Churchill Livingstone; 2005. p. 2310–2318.
Harris, RM, Couturier BA, Sample SC. Expanded Geographic Distribution and Clinical Characteristics of Ehrlichia ewingii Infections, United States. Emerg Infect Dis 2016 May;22(5):862-865.
Johnson DK, Schiffman EK, Davis JP, et al. Human infection with Ehrlichia muris-like pathogen, United States, 2007-2013(1). Emerg Infect Dis 2015 Oct;21(10):1794-1799.
Mowla SJ, Drexler NA, Cherry CC, et al. Ehrlichiosis and anaplasmosis among transfusion and transplant recipients in the United States. Emerg Infect Dis. 2021 Nov;27(11):2768-2775.
Pritt BS, Sloan LM, Johnson DK, et al. Emergence of a new pathogenic Ehrlichia species, Wisconsin and Minnesota, 2009. N Engl J Med 2011; 365:422-429
Saha A, Browning C, Dandamudi R, et al. Donor-derived ehrlichiosis: 2 clusters following solid organ transplantation. Clin Infect Dis. 2022 Mar 9;74(5):918-923.
Todd SR, Dahlgren FS, et al. No visible dental staining in children treated with doxycycline for suspected Rocky Mountain spotted fever. J Pediatr 2015 May;166(5):1246-1251.
Contents
- Home
- Tick ID
- Overview of Tickborne Diseases
- Lyme Disease
- Tickborne Relapsing Fever (TBRF)
- Hard Tick Relapsing Fever
- Anaplasmosis
- ›Ehrlichiosis
- Rocky Mountain Spotted Fever
- Rickettsia parkeri Rickettsiosis
- Tularemia
- Babesiosis
- Heartland and Bourbon Virus Diseases
- Colorado Tick Fever
- Powassan Virus Disease
- Tickborne Diseases Abroad
- Tick Bites/Prevention
- Lyme Disease Prophylaxis After Tick Bite