Lyme Disease
- Home
- Tick ID
- Overview of Tickborne Diseases
- Lyme Disease
- Tickborne Relapsing Fever (TBRF)
- Hard Tick Relapsing Fever
- Anaplasmosis
- Ehrlichiosis
- Rocky Mountain Spotted Fever
- Rickettsia parkeri Rickettsiosis
- Tularemia
- Babesiosis
- Heartland and Bourbon Virus Diseases
- Colorado Tick Fever
- Powassan Virus Disease
- Tickborne Diseases Abroad
- Tick Bites/Prevention
- Lyme Disease Prophylaxis After Tick Bite
Agents
Borrelia burgdorferi, B. mayonii
Where Found
Lyme disease is most frequently reported from the upper midwestern, northeastern, and mid-Atlantic states where it is spread by Ixodes scapularis ticks. Some cases are also reported from northern California, Oregon, and Washington, where it is spread by Ixodes pacificus ticks. High-incidence states include Connecticut, Delaware, Maine, Maryland, Massachusetts, Minnesota, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, Vermont, Virginia, Washington D.C., West Virginia, and Wisconsin. While these states account for the majority of cases, the geographic area of risk is expanding to include neighboring states.

Incubation Period
3-30 days
Signs and Symptoms
Early Localized (3 to 30 days after a tick bite):
- Erythema migrans (EM)— Red annular or homogeneous rash at the site of tick bite; expands gradually over several days to >5 cm in diameter; central clearing may develop as the rash expands, resulting in a “target” or “bull’s-eye” appearance; may feel warm to the touch but rarely itchy or painful. EM occurs in 70-80% of infected persons. The classic rash is not present in all cases; see examples on the following pages.
- Fever, chills, malaise, fatigue, headache, myalgia, arthralgia
- Lymphadenopathy
Disseminated (days to months after a tick bite):
Untreated or unnoticed early Lyme disease will progress to disseminated disease for about 60% of patients, with diverse clinical manifestations. Most manifestations will appear in the first few weeks to months of infection, though rheumatologic manifestations may be particularly delayed.
Dermatologic manifestations
- Multiple EM rashes, distant from site of tick bite
Neurologic manifestations
- Cranial neuritis, most commonly Bell’s palsy (facial paralysis, can be bilateral)
- Lymphocytic meningitis
- Painful radiculoneuritis involving one or multiple dermatomes
- Painful peripheral motor and sensory neuropathy (mononeuritis multiplex)
- Intracranial hypertension (rare)
Cardiac manifestations
- Lyme carditis resulting in conduction abnormalities (e.g., atrioventricular node block; myopericarditis)
- Rarely, can be fatal
Rheumatologic manifestations
- Oligoarticular arthritis: transient, migratory arthritis and effusion in one or multiple joints, often large joints; may cause Baker’s cyst
- Migratory pain in tendons, bursae, muscle, and bones
LYME DISEASE OR STARI?
An erythema migrans-like rash has also been described in humans following bites of the lone star tick. This condition has been named Southern Tick-Associated Rash Illness (STARI). Although the rash may be accompanied by systemic symptoms, disseminated or severe disease has not been reported. Because the cause of STARI is unknown, diagnostic blood tests are not available. It is not known whether antibiotic treatment is necessary or beneficial for patients with STARI. Nevertheless, because STARI resembles early Lyme disease, physicians often treat patients with the same antibiotics recommended for Lyme disease.
Lone star ticks can be found from central Texas and Oklahoma eastward across the southern states and along the Atlantic Coast as far north as Maine.
General Laboratory Findings for Lyme Disease
- Elevated erythrocyte sedimentation rate
- Mildly elevated hepatic transaminases
- Microscopic hematuria or proteinuria
Laboratory Diagnosis
- For patients who present with an EM rash after being in an area where Lyme disease is common, Lyme disease should be diagnosed clinically (without diagnostic testing), as serologic tests may be negative during the first few weeks of infection before antibodies have developed.
- Serologic tests are highly sensitive in patients with disseminated Lyme disease, and diagnosis relies on signs and symptoms supported by results of testing.
- Two-step serologic testing is recommended using validated first- and second-tier tests according to a standard or modified two-test algorithm. IgM Western immunoblot results should only be considered if signs and symptoms have been present for less than 30 days.
Notes on Serologic Tests for Lyme Disease
- For details, refer to the APHL guide for interpretation of serologic test results [PDF – 17 pages].
- While not necessary, acute and convalescent serologies may be useful for diagnosis in some cases, such as for patients with suspected re-infection.
- Serologic tests cannot be used to measure treatment response.
- Other conditions, including some tickborne infections and autoimmune diseases, can result in false positive test results.
NOTE: Coinfection with Babesia microti or Anaplasma phagocytophilum should be considered in patients who present with initial symptoms that are more severe than are commonly observed with Lyme disease alone, especially in those who have high-grade fever for more than 48 hours despite appropriate antibiotic therapy or who have unexplained leukopenia, thrombocytopenia, or anemia. Coinfection should also be considered in patients whose erythema migrans skin lesion has resolved but who have persistent systemic symptoms.
Treatment of Erythema Migrans Rash
People treated with appropriate antibiotics in the early stages of Lyme disease usually recover rapidly and completely. Early diagnosis and proper antibiotic treatment of Lyme disease can help prevent late Lyme disease. Treatment regimens listed in the following table are for the erythema migrans rash, the most common manifestation of early Lyme disease. These regimens may need to be adjusted depending on a person’s age, medical history, underlying health conditions, pregnancy status, or allergies. Consult an infectious disease specialist regarding individual patient treatment decisions. For treating other manifestations, see www.cdc.gov/Lyme/treatment.
| Age Category | Drug | Dosage | Maximum | Duration, Days* |
|---|---|---|---|---|
| Adults | Doxycycline OR |
100 mg, twice per day orally | N/A | 10-14 |
| Amoxicillin OR |
500 mg, three times per day orally | N/A | 14 | |
| Cefuroxime | 500 mg, twice per day orally | N/A | 14 | |
| Children | Doxycycline OR |
4.4 mg/kg per day orally, divided into 2 doses | 100 mg per dose | 10–14 |
| Amoxicillin OR |
50 mg/kg per day orally, divided into 3 doses | 500 mg per dose | 14 | |
| Cefuroxime | 30 mg/kg per day orally, divided into 2 doses | 500 mg per dose | 14 |
*When different durations of antibiotics are shown to be effective for the treatment of Lyme disease, the shorter duration is preferred to minimize adverse effects, including infectious diarrhea and antimicrobial resistance.
NOTE: For people intolerant of amoxicillin, doxycycline, and cefuroxime, the macrolide azithromycin may be used, although it is less effective. People treated with azithromycin should be closely monitored to ensure that symptoms resolve.
References
Association of Public Health Laboratories. Suggested Reporting Language, Interpretation and Guidance Regarding Lyme Disease Serologic Test Results. 2021. Silver Spring, MD: Association of Public Health Laboratories; 2021.
Centers for Disease Control and Prevention. Updated CDC Recommendation for Serologic Diagnosis of Lyme Disease. MMWR Morb Mortal Wkly Rep. 2019;68(32):703.
Centers for Disease Control and Prevention. Recommendations for test performance and interpretation from the second national conference on serologic diagnosis of Lyme disease. MMWR Morb Mortal Wkly Rep. 1995;44:590–591.
Halperin JJ, Baker P, Wormser GP. Common misconceptions about Lyme disease. Am J Med. 2013;126(3):264.
Hu LT. Lyme Disease. Ann Intern Med. 2016;165(9):677.
Kugeler KJ, Schwartz AM, Delorey MJ, Mead PS, Hinckley AF. Estimating the Frequency of Lyme Disease Diagnoses, United States, 2010-2018. Emerg Infect Dis. 2021;27(2):616-619.
Lantos PM, Rumbaugh J, Bockenstedt LK, et al. Clinical Practice Guidelines by the Infectious Diseases Society of America (IDSA), American Academy of Neurology (AAN), and American College of Rheumatology (ACR): 2020 Guidelines for the Prevention, Diagnosis and Treatment of Lyme Disease. Clin Infect Dis. 2021;72(1):e1-e48.
Sanchez E, Vannier E, Wormser GP, Hu LT. Diagnosis, treatment, and prevention of Lyme disease, human granulocytic anaplasmosis, and babesiosis: A review. JAMA. 2016;315(16):1767-77.
Stanek G, Wormser GP, Gray J, et al. Lyme borreliosis. Lancet. 2012;379(9814):461-73.
Steere AC. Lyme Disease (Lyme Borreliosis) Due to Borrelia burgdorferi. In: Bennett J, Dolin R, Blaser M., editors. Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases. 9th ed. Elsevier Health Sciences; 2020.
Erythema Migrans Rashes
The erythema migrans (EM) rash occurs in 70–80% of patients with Lyme disease. EM rashes may have the classic appearance or may take alternate forms; solid lesions, blue-purple hues, and crusted or blistering lesions have all been documented.
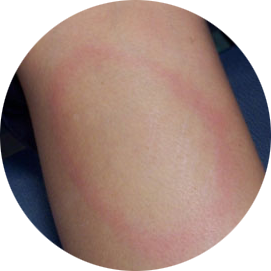
CLASSIC EM—CIRCULAR RED RASH WITH CENTRAL CLEARING THAT SLOWLY EXPANDS
Photo courtesy of Taryn Holman.

BLUISH HUE WITHOUT CENTRAL CLEARING
Photo courtesy of Yevgeniy Balagula.
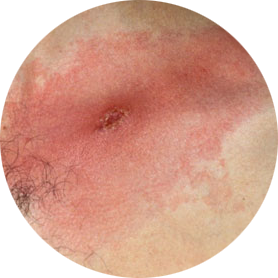
EXPANDING LESION WITH CENTRAL CRUST ON CHEST
Photo courtesy of Bernard Cohen.
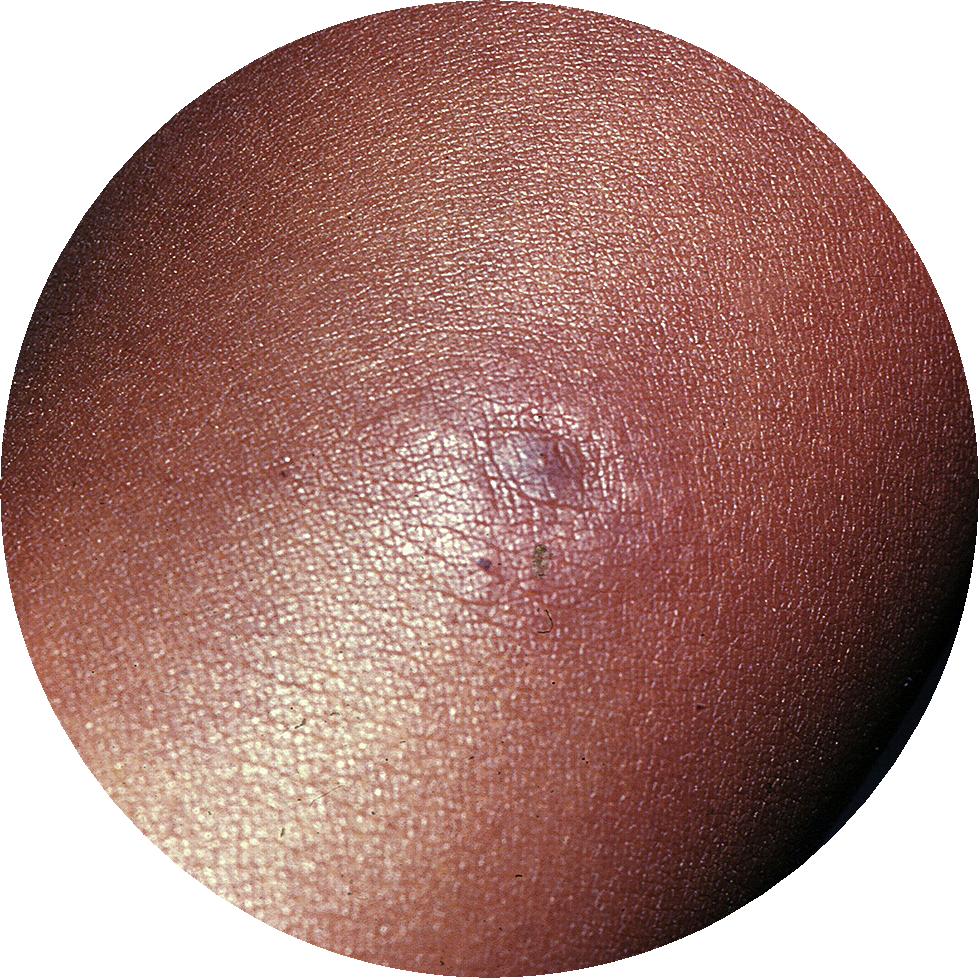
EARLY, EXPANDING ERYTHEMA MIGRANS WITH NODULE
Reprinted from Bhate C, Schwartz RA. Lyme disease: Part I. Advances and perspective. J Am Acad Dermatol. 2011;64:619-36, with permission from Elsevier.
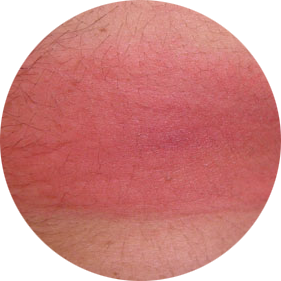
RED, EXPANDING OVAL-SHAPED PLAQUE ON TRUNK
Photo courtesy of Alison Young.
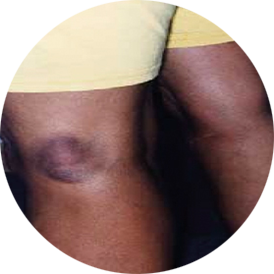
PURPLE LESION ON BACK OF KNEE
Photo courtesy of New York State Department of Health.
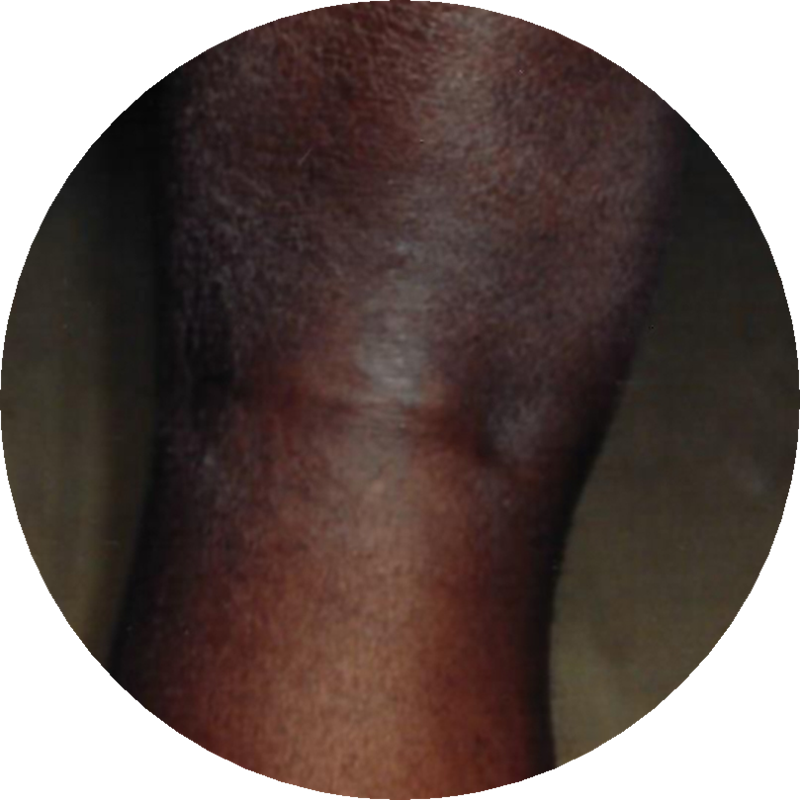
FAINT EM ON BACK OF KNEE
Photo courtesy of Gary Wormser, New York Medical College

EARLY DISSEMINATED LYME DISEASE—MULTIPLE LESIONS WITH DUSKY CENTERS ON TRUNK
Photo courtesy of Bernard Cohen.
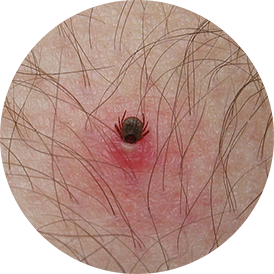
TICK BITE WITH MILD ALLERGIC REACTION
Not erythema migrans. Hypersensitivity reactions typically appear within the first 48 hours of tick attachment, are often itchy and are usually <5 cm in diameter. Localized tick bite reactions can occur following bites from any tick species.
Special thanks to DermAtlas for providing many photographs.